Ordering Tests - A Strategic Approach
- Pre-test Probability: Start with clinical assessment. High suspicion warrants different tests than low suspicion.
- Test Characteristics:
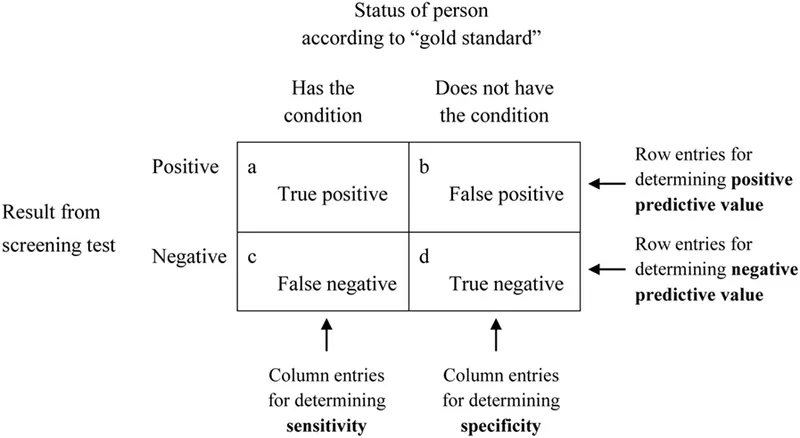
- Screening: High sensitivity (Sn) to rule out (SNOUT).
- Confirmatory: High specificity (Sp) to rule in (SPIN).
- Avoid Cascades: Order tests sequentially, not all at once. Re-evaluate after each result.
⭐ Likelihood Ratios (LRs): A key tool for evidence-based testing.
- LR+ > 10 and LR- < 0.1 provide strong evidence to rule in or rule out a disease, respectively.
Incidentalomas - The Unexpected Discovery

An unexpected finding on imaging ordered for an unrelated reason. The core challenge is balancing the risk of malignancy against the risks and costs of over-investigation.
- General Approach: Assess for symptoms, high-risk features (e.g., patient history of malignancy), and compare with prior imaging if available.
- Key Factors: Focus on lesion size, morphology (shape, density, enhancement), and stability over time.
- Common Thresholds:
- Adrenal: >1 cm needs biochemical workup. Consider surgery if >4 cm or functional.
- Thyroid: >1 cm may require FNA based on sonographic features.
- Renal: Use Bosniak classification for cysts. III/IV warrant urology referral.
⭐ Most adrenal incidentalomas are non-functioning benign adenomas. The primary goal is to exclude pheochromocytoma, Cushing's syndrome, and malignancy. A biopsy is contraindicated until pheochromocytoma is ruled out.
Management Pathways - Charting The Course
- Initial step: Characterize the finding based on size, morphology, density, and enhancement patterns.
- Assess patient context: Consider age, comorbidities, life expectancy, and personal history of malignancy.
- Utilize established guidelines (e.g., Fleischner for pulmonary nodules, Bosniak for renal cysts, ACR TI-RADS for thyroid nodules).
- 💡 Principle of primum non nocere: Balance the risk of invasive workup (anxiety, cost, complications) against the risk of missing a significant pathology.
- Involve the patient in shared decision-making, especially for surveillance plans.
⭐ For adrenal incidentalomas, a key threshold is size. Lesions >4 cm or those with suspicious imaging features (e.g., high attenuation on non-contrast CT >10 HU, low washout) warrant further workup for malignancy or hormonal activity.

High‑Yield Points - ⚡ Biggest Takeaways
- The primary principle for incidental findings is "first, do no harm."
- Always correlate clinically; an incidentaloma in an asymptomatic patient is often benign.
- Adhere to standardized guidelines like Fleischner criteria (for lung nodules) or Bosniak classification (for renal cysts).
- Informed consent and shared decision-making are crucial before further investigation.
- Active surveillance is frequently preferred over immediate intervention for low-risk findings.
- Decision-making must consider patient age, life expectancy, and comorbidities.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

