Sensitivity & Specificity - Test True Tellers
-
Sensitivity (True Positive Rate): Probability of a positive test in a patient with the disease.
- Formula: $TP / (TP + FN)$
- 📌 SNOUT: a highly SeNsitive test, when Negative, rules OUT the disease.
- Ideal for screening tests.
-
Specificity (True Negative Rate): Probability of a negative test in a patient without the disease.
- Formula: $TN / (TN + FP)$
- 📌 SPIN: a highly SPecific test, when Positive, rules IN the disease.
- Ideal for confirmatory tests.
ROC Curve Analysis
- Plots Sensitivity (y-axis) vs. 1-Specificity (x-axis) at all cut-off points.
- Area Under the Curve (AUC) reflects test accuracy:
- AUC = 1.0: Perfect test.
- AUC = 0.5: Useless (random chance).
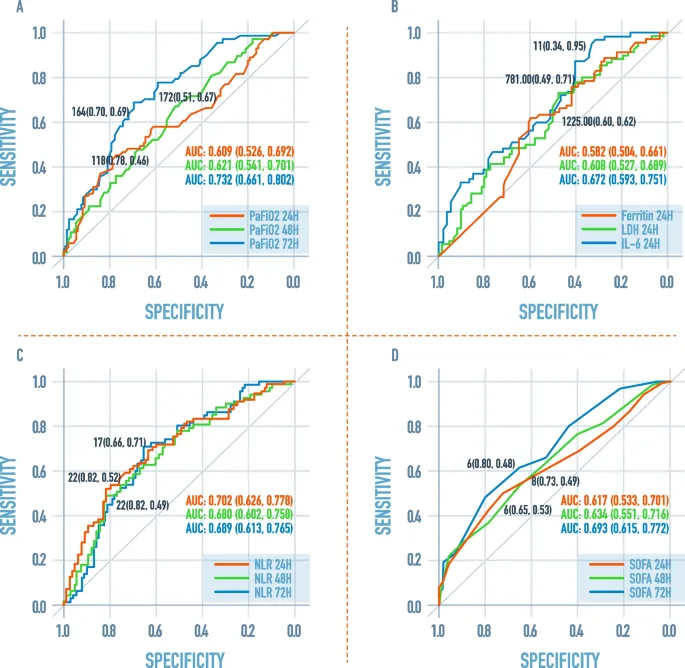
⭐ The optimal cut-off point on an ROC curve is typically the one closest to the top-left corner, maximizing both sensitivity and specificity.
ROC Curve Construction - Dot-to-Dot Diagnosis
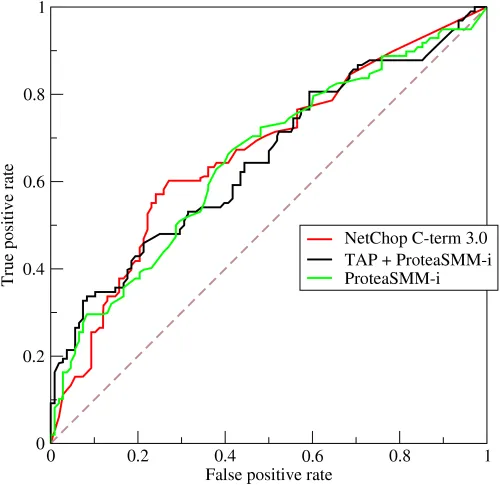 curve showing sensitivity vs. 1-specificity)
curve showing sensitivity vs. 1-specificity)
- Plotting the Curve: An ROC curve graphs a test's performance across all possible cut-off points.
- Y-axis: Sensitivity (True Positive Rate, TPR)
- $Sensitivity = TP / (TP + FN)$
- X-axis: 1 - Specificity (False Positive Rate, FPR)
- $1 - Specificity = FP / (TN + FP)$
- Y-axis: Sensitivity (True Positive Rate, TPR)
- Interpretation: Each point on the curve represents a sensitivity/specificity pair for a specific diagnostic threshold.
⭐ The ideal cut-off point is often the one closest to the top-left corner (100% sensitivity, 100% specificity). The overall test accuracy is measured by the Area Under the Curve (AUC). An AUC of 0.5 is random chance; 1.0 is a perfect test.
AUC & Interpretation - The Curve's Clues
- Area Under the Curve (AUC): Represents the overall diagnostic accuracy of a test. It's the probability that the test will correctly rank a random positive patient higher than a random negative one.
- AUC Scale: Ranges from 0.5 (no discrimination) to 1.0 (perfect discrimination).
Interpreting AUC Values:
- AUC = 1.0: Perfect test.
- AUC > 0.9: Excellent.
- AUC 0.8-0.9: Good.
- AUC 0.7-0.8: Fair.
- AUC < 0.7: Poor/Fail.
- AUC = 0.5: No better than chance (the diagonal line).
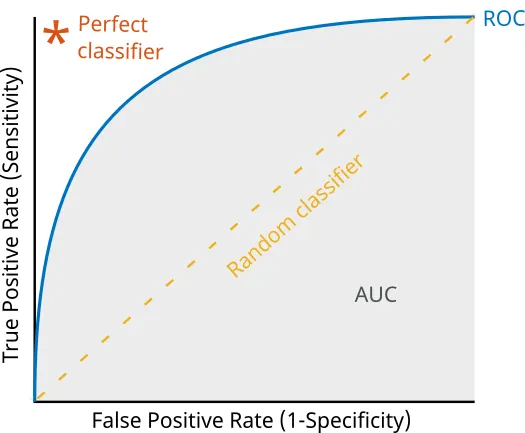
- Test Comparison: The test with the ↑ AUC is generally the more accurate diagnostic tool.
⭐ Key Pearl: The AUC is a measure of a test's intrinsic accuracy and is independent of the prevalence of the disease in the population being tested.
High‑Yield Points - ⚡ Biggest Takeaways
- ROC curves plot Sensitivity (TPR) vs. 1-Specificity (FPR) across multiple cut-off thresholds.
- The Area Under the Curve (AUC) is a measure of the overall accuracy of a diagnostic test.
- An AUC of 1.0 represents a perfect test; an AUC of 0.5 represents a test with no discriminatory capacity (i.e., chance).
- The optimal cut-off point on the curve is typically closest to the top-left corner (high sensitivity and specificity).
- When comparing two diagnostic tests, the test with the higher AUC is generally more accurate.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

