Core Metrics - The Diagnostic Foundation

-
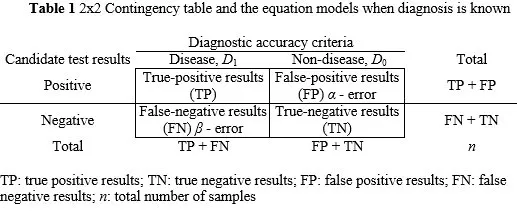
Sensitivity (Sn): The ability of a test to correctly identify individuals with the disease.
- Formula: $Sn = TP / (TP + FN)$
- Use: High sensitivity is crucial for screening tests to avoid missing cases (low false negatives).
- 📌 SNOUT: A highly SeNsitive test, when Negative, helps to rule OUT disease.
-
Specificity (Sp): The ability of a test to correctly identify individuals without the disease.
- Formula: $Sp = TN / (TN + FP)$
- Use: High specificity is vital for confirmatory tests to avoid false alarms (low false positives).
- 📌 SPIN: A highly SPecific test, when Positive, helps to rule IN disease.
⭐ Sensitivity and Specificity are intrinsic to the test and are not affected by disease prevalence.
Predictive Values - Prevalence's Impact
- Predictive values depend heavily on disease prevalence in the target population.
- Sensitivity and Specificity are intrinsic test properties and do not change with prevalence.
-
Positive Predictive Value (PPV):
- Probability of having the disease with a positive test.
- Directly proportional to prevalence: As prevalence ↑, PPV ↑.
-
Negative Predictive Value (NPV):
- Probability of being disease-free with a negative test.
- Inversely proportional to prevalence: As prevalence ↑, NPV ↓.
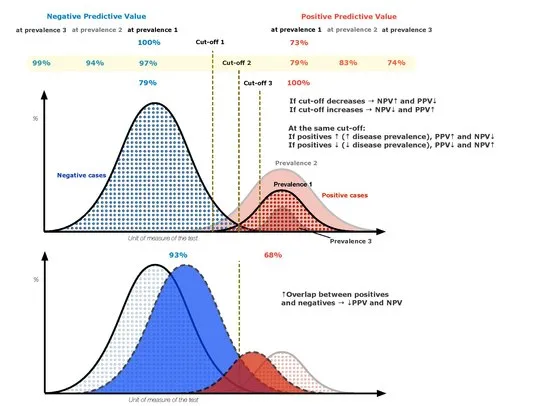
⭐ In low-prevalence settings, even tests with high specificity have a low PPV. A positive result in a general population screen for a rare disease is more likely to be a false positive.
ROC Curves - Finding the Sweet Spot
- Function: Plots test performance across all cut-off points. Compares $Sensitivity (TPR)$ vs. $1 - Specificity (FPR)$.
- Axes:
- Y-axis: Sensitivity (True Positive Rate)
- X-axis: 1 - Specificity (False Positive Rate)
- Area Under the Curve (AUC):
- Represents overall accuracy.
- AUC = 1.0: Perfect test.
- AUC = 0.5: Useless test (the diagonal "line of chance").
- Optimal Cut-off Point:
- Typically the point on the curve nearest the top-left corner (0,1).
- This point maximizes the Youden Index: $(Sensitivity + Specificity) - 1$.
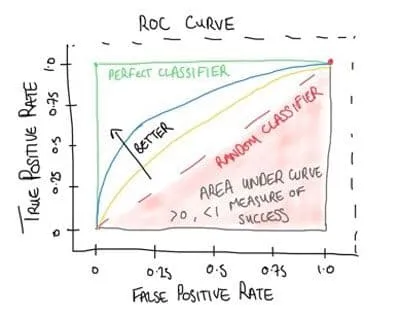 curve showing multiple cut-off points and the area under the curve)
curve showing multiple cut-off points and the area under the curve)
⭐ An AUC >0.8 suggests a good test; 0.7-0.8 is acceptable. An AUC <0.7 has poor diagnostic ability.
Screening Biases - The Hidden Traps
- Lead-time bias: Early detection artificially inflates survival time, even if mortality is unchanged. The "survival clock" simply starts earlier.
- Length-time bias: Screening tends to detect more slow-growing, indolent cases with a better prognosis, while missing rapidly progressive, aggressive diseases.
- Selection (Volunteer) bias: Health-conscious individuals are more likely to participate in screening, leading to better outcomes unrelated to the screening itself.
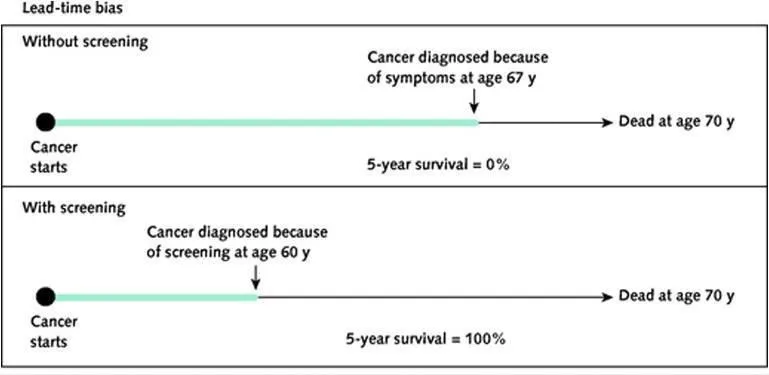
⭐ A randomized controlled trial is the gold standard to mitigate these biases and prove a screening test reduces mortality.
High‑Yield Points - ⚡ Biggest Takeaways
- Screening tests require high sensitivity to rule out disease (S-N-OUT) and avoid false negatives.
- Confirmatory tests demand high specificity to rule in disease (S-P-IN) and minimize false positives.
- Sensitivity and specificity are intrinsic to the test and unaffected by prevalence.
- Predictive values (PPV & NPV), however, are heavily dependent on disease prevalence.
- PPV is the most important measure for a positive screening test result's clinical utility.
- Adjusting a test's cut-off point creates an inverse relationship between sensitivity and specificity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

