BCAA Metabolism - The VIP Amino Acids
- The three essential branched-chain amino acids (BCAAs) are Valine, Isoleucine, and Leucine. They are primarily metabolized in muscle, not the liver.
- 📌 Mnemonic: I Love Vermont.
- Their catabolism provides energy during fasting states.
- Metabolic Fates:
- Leucine: Exclusively ketogenic → forms acetyl-CoA.
- Isoleucine: Both ketogenic and glucogenic → forms acetyl-CoA & succinyl-CoA.
- Valine: Exclusively glucogenic → forms succinyl-CoA.
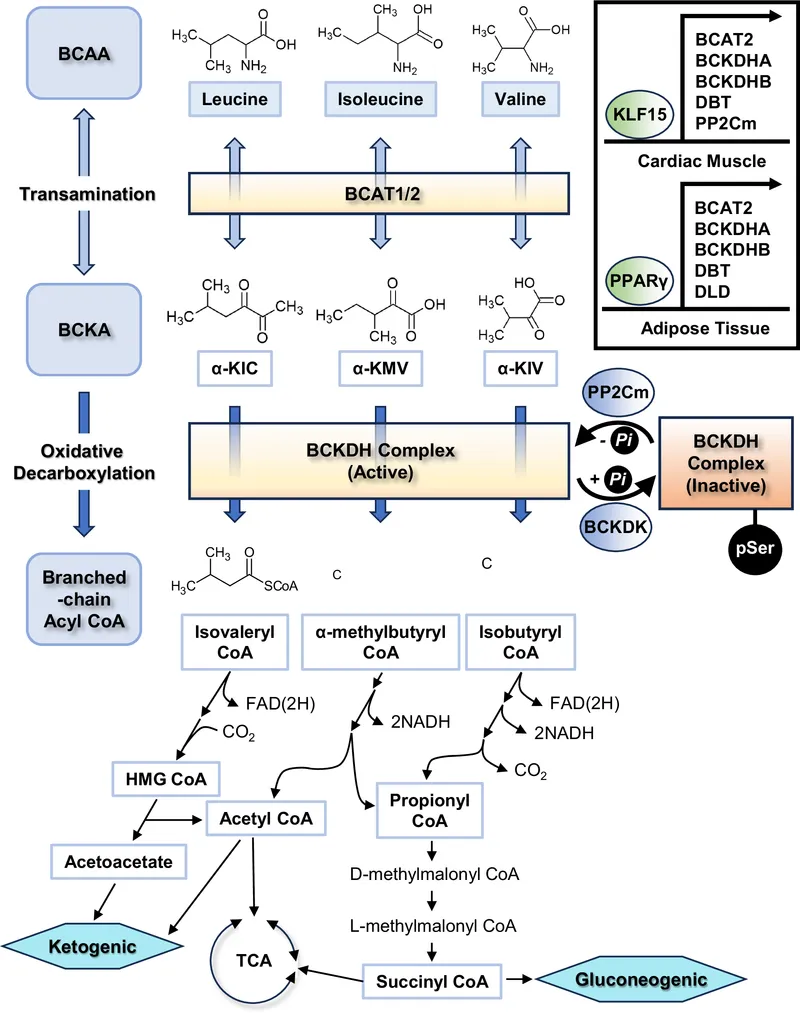
⭐ A deficiency in the key enzyme, Branched-Chain α-Ketoacid Dehydrogenase (BCKDH), leads to Maple Syrup Urine Disease (MSUD), characterized by the sweet smell of urine.
Catabolic Pathway - Breaking Down the Branches
-
Step 1: Transamination
- Enzyme: Branched-chain aminotransferase (BCAT).
- Action: Reversibly transfers the amino group from BCAAs to α-ketoglutarate, forming branched-chain α-ketoacids (BCKAs).
-
Step 2: Oxidative Decarboxylation
- Enzyme: Branched-chain α-ketoacid dehydrogenase (BCKDH) complex.
- Action: Irreversibly decarboxylates BCKAs to form branched-chain acyl-CoA derivatives.
- 📌 Mnemonic (Cofactors): Tender Loving Care For Nancy - Thiamine (B1), Lipoate, CoA (B5), FAD (B2), NAD (B3).
⭐ The BCKDH complex is structurally and functionally analogous to the pyruvate dehydrogenase (PDH) and α-ketoglutarate dehydrogenase complexes.
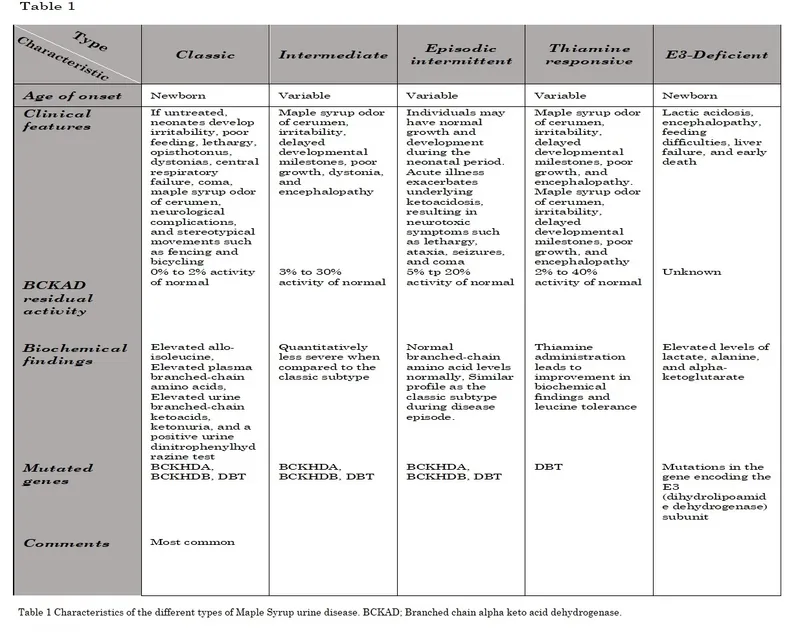
Maple Syrup Urine Disease - Sweet-Smelling Danger
- Pathophysiology: Deficiency of the Branched-chain α-ketoacid dehydrogenase (BCKDH) complex, leading to the accumulation of branched-chain amino acids.
- Inheritance: Autosomal Recessive.
- Classic Presentation: Onset in the first few days of life with poor feeding, vomiting, lethargy, and progressive encephalopathy.
- Key Sign: A characteristic sweet odor of urine and cerumen, similar to maple syrup or burnt sugar.
- Diagnosis:
- ↑ Plasma and urine levels of BCAAs (Leucine, Isoleucine, Valine).
- Presence of allo-isoleucine is pathognomonic.
- Management:
- Lifelong dietary restriction of BCAAs.
- Thiamine (Vitamin B1) supplementation, as it is a necessary cofactor for the BCKDH complex.
⭐ Leucine is the most neurotoxic of the BCAAs; its accumulation is primarily responsible for the severe neurological damage (e.g., encephalopathy, seizures) seen in MSUD crises.
High‑Yield Points - ⚡ Biggest Takeaways
- Maple Syrup Urine Disease (MSUD) is caused by deficient branched-chain α-ketoacid dehydrogenase (BCKDH).
- This leads to toxic accumulation of BCAAs (leucine, isoleucine, valine) and their corresponding α-ketoacids.
- Classic presentation includes urine smelling like burnt sugar, neurotoxicity, and poor feeding.
- Leucine is the primary neurotoxic metabolite.
- Diagnosis is confirmed by ↑ plasma BCAAs and allo-isoleucine.
- Management requires lifelong dietary restriction of BCAAs and thiamine (B1) supplementation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

