Withdrawal Principles - The Opt-Out Clause
- Core Principle: Rooted in patient autonomy, the right to refuse or withdraw is absolute.
- Timing & Method: Can be revoked at any time, through verbal or non-verbal cues. No formal process is needed.
- No Prejudice: Withdrawal must not result in penalty, loss of benefits, or compromised future care. The physician-patient relationship should remain intact.
- Capacity: A patient with decision-making capacity can withdraw consent previously given.

⭐ High-Yield Fact: A patient withdrawing from a clinical trial does not forfeit their right to standard medical care. They must be offered the best available alternative treatment outside of the trial protocol.
📌 Mnemonic: Remember A.C.T.
- Any time withdrawal
- Capacity required
- Treatment alternatives offered
Clinical Workflow - Hitting the Brakes
A patient with decision-making capacity can withdraw consent at any time. This right persists even if withdrawal may result in death.
- Process Initiation: Patient communicates desire to stop treatment or leave.
- Capacity Assessment: Re-evaluate the patient's capacity to make informed decisions.
- Informed Refusal: Discuss risks of leaving and benefits of staying. Explore alternatives and answer questions.
- Documentation: If the patient still refuses, document the discussion, their understanding of the risks, and the plan for leaving. This is often done via an "Against Medical Advice" (AMA) form.
- Safe Discharge: Do not abandon the patient. Provide necessary prescriptions, arrange follow-up, and ensure a safe transition from the hospital.
⭐ A patient with capacity refusing life-saving treatment is NOT a reason to involve the ethics committee or seek a court order. The patient's autonomy is paramount.
Special Populations - Gray Area Cases
- Minors (<18 years): Generally lack legal capacity; require parental consent.
- Assent: A child's affirmative agreement (sought if age >7). Ethically important but not legally sufficient.
- Dissent: A child's refusal. Can be overridden by parents for beneficial, necessary medical care.
- Exceptions: Emancipated or mature minors may consent independently.
- Psychiatric Patients: A diagnosis does not automatically mean lack of capacity. Capacity is decision-specific and must be formally assessed.
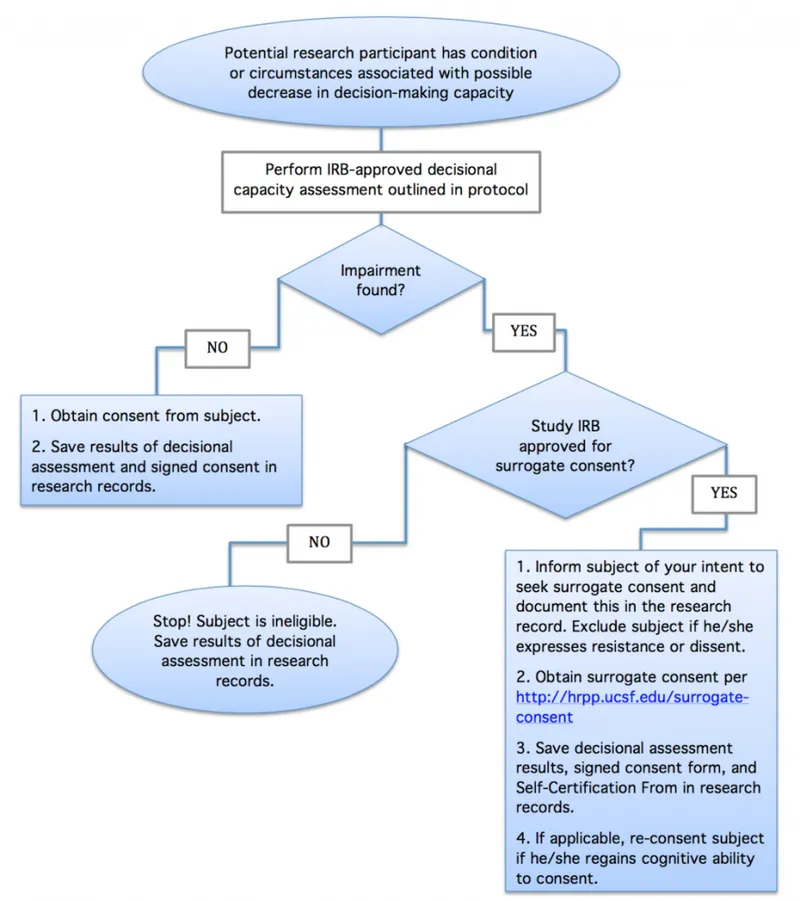
- Lack of Capacity (Adults): For patients unable to understand risks, benefits, and alternatives, use a surrogate decision-maker.
- Hierarchy: Healthcare proxy → spouse → adult child → parent.
⭐ In a true emergency, if a patient lacks capacity and no surrogate is available, treatment can proceed under the principle of implied consent.
Research Context - Trial & Error
- Equipoise: Ethical prerequisite for clinical trials, signifying genuine uncertainty among experts about which treatment arm is superior. Without it, a physician is ethically obligated to offer the known superior treatment.
- No-Fault Withdrawal: Patients can withdraw from a study at any time for any reason without penalty. Their access to standard medical care must not be compromised.
- Data Usage Post-Withdrawal:
- No new data can be collected from the participant.
- Data collected prior to withdrawal is typically retained and analyzed to prevent bias and maintain the statistical integrity of the trial.
⭐ A patient can withdraw consent for future participation and data collection, but cannot demand the removal of their already collected data from the research database, especially in FDA-regulated trials.
High‑Yield Points - ⚡ Biggest Takeaways
- Patients can withdraw consent at any time, for any reason, even if treatment has already begun.
- The withdrawal can be verbal or non-verbal and requires no formal process.
- All non-essential medical intervention must cease immediately upon withdrawal.
- The physician must respect the patient's decision, regardless of medical opinion.
- Thorough documentation of the withdrawal event in the medical record is crucial.
- Withdrawal does not invalidate consent given for previously performed procedures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

