Epithelial Tissue - Body's Border Patrol
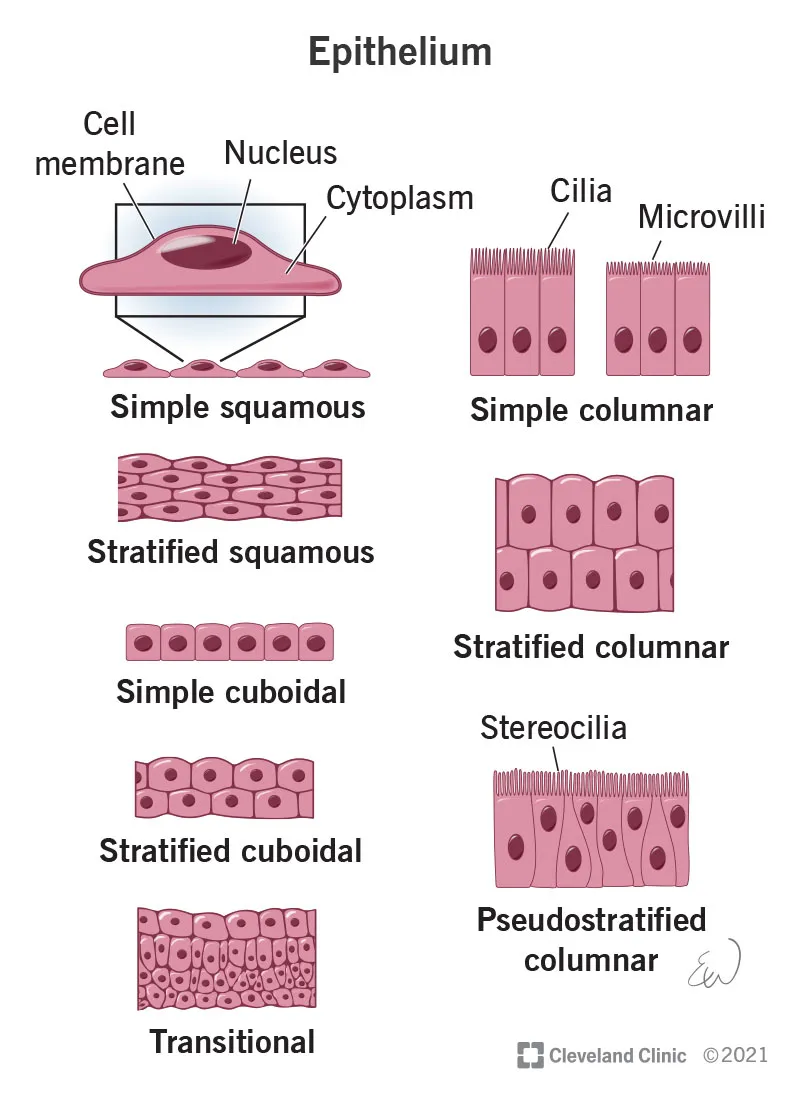
- Core Functions: Protection (skin), absorption (gut), secretion (glands), filtration (kidney), sensation.
- Classification: Based on layers (simple, stratified, pseudostratified) and cell shape (squamous, cuboidal, columnar).
- Polarity:
- Apical surface: Faces lumen/exterior; may have microvilli or cilia.
- Basal surface: Rests on the basement membrane.
- Intercellular Junctions:
- Tight junctions (Zonula Occludens): Prevent paracellular diffusion.
- Adherens junctions (Zonula Adherens): Link actin cytoskeletons.
- Desmosomes (Macula Adherens): Anchor intermediate filaments.
- Gap junctions: Allow direct communication.
⭐ Kartagener Syndrome: A primary ciliary dyskinesia where dynein arm defects impair cilia function. This disrupts mucociliary clearance, causing recurrent sinusitis, bronchiectasis, and situs inversus.
Connective Tissue - The Matrix Masters
- Components: Cells + Extracellular Matrix (ECM).
- ECM: Ground Substance (support) + Fibers (strength).
- Ground Substance: Glycosaminoglycans (GAGs), proteoglycans, glycoproteins.
- Fibers:
- Collagen: Main structural protein. 📌 Cartilage (type II), Bone (type I), Reticulin (type III), Basement membrane (type IV).
- Elastin: Provides stretch/recoil; found in skin, lungs, large arteries.
- Primary Cells:
- Fibroblasts/cytes: Synthesize ECM fibers and ground substance.
- Adipocytes: Store fat.
- Mast Cells: Mediate inflammation (histamine, heparin).
- Macrophages: Phagocytosis.
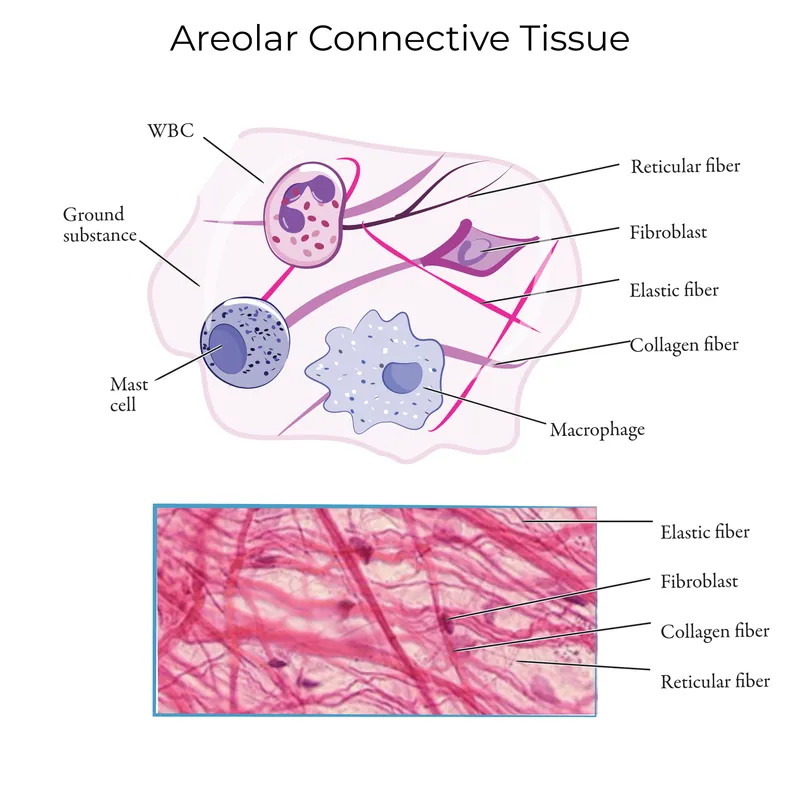
⭐ Marfan Syndrome: An autosomal dominant genetic disorder caused by a defect in the FBN1 gene, which codes for fibrillin-1. This affects elastic fibers, leading to issues in the aorta, ligaments, and eyes.
Muscle Tissue - The Contraction Crew
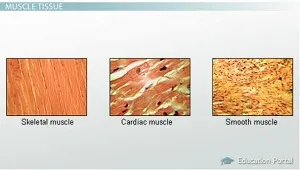
A comparative overview of the three muscle types, essential for identifying histological slides.
| Feature | Skeletal Muscle | Cardiac Muscle | Smooth Muscle |
|---|---|---|---|
| Appearance | Striated, ordered | Striated, less ordered | Non-striated |
| Cell Shape | Long, cylindrical fibers | Branched, shorter cells | Fusiform (spindle-shaped) |
| Nuclei | Multinucleated, peripheral | 1-2 nuclei, central | Single nucleus, central |
| Control | Voluntary (somatic) | Involuntary (autonomic) | Involuntary (autonomic) |
| Key Features | Triads (T-tubule & 2 terminal cisternae) | Intercalated discs, gap junctions | Dense bodies, caveolae |
Nervous Tissue - The Command Network
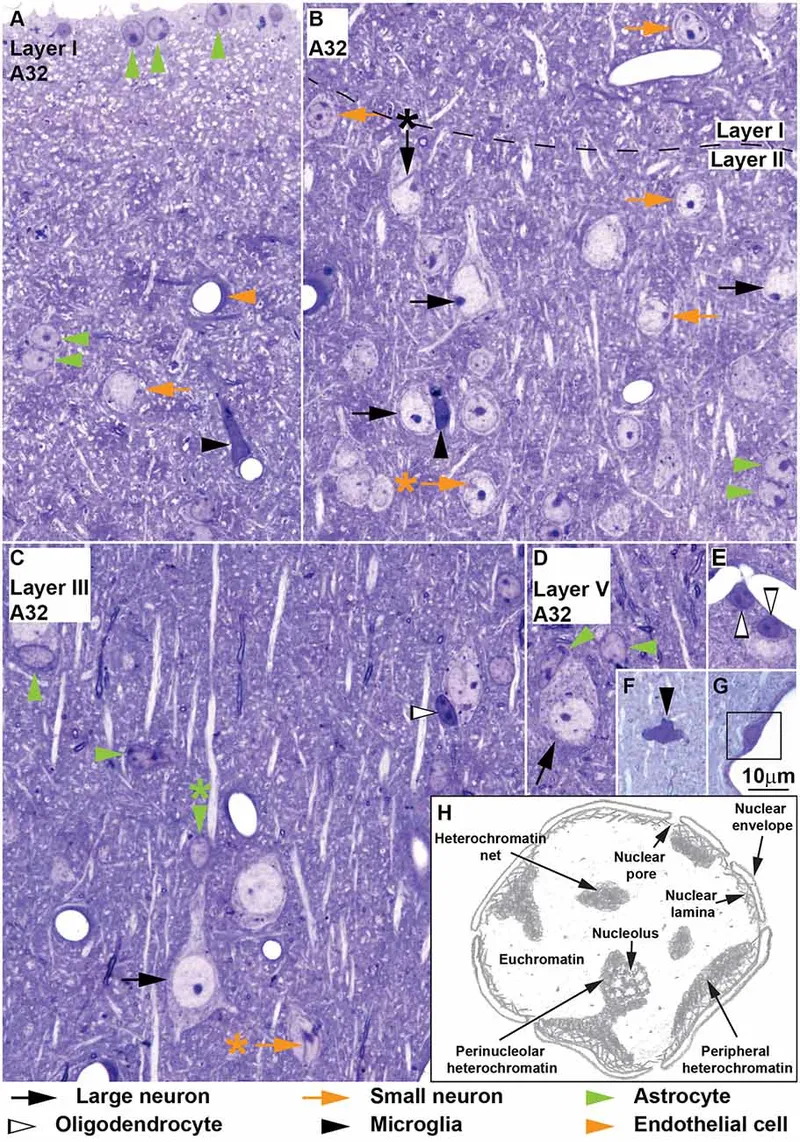
-
Neurons: The primary signaling units.
- Soma (Cell Body): Metabolic core with nucleus.
- Dendrites: Branched extensions that receive incoming signals.
- Axon: Single long process that transmits outgoing signals.
-
Glial Cells: Non-neuronal cells providing crucial support.
- CNS: Astrocytes (support, BBB), Microglia (phagocytes), Oligodendrocytes (myelinate multiple axons), Ependymal cells (line ventricles).
- PNS: Schwann Cells (myelinate single axons), Satellite Cells (support ganglia).
⭐ Nissl bodies (rough ER) are prominent in the soma and dendrites, reflecting high protein synthesis, but are absent from the axon and axon hillock.
High‑Yield Points - ⚡ Biggest Takeaways
- Epithelium lines surfaces and forms glands; it's avascular, rests on a basement membrane, and shows apical-basal polarity.
- Connective tissue is defined by its extracellular matrix (fibers and ground substance) and is derived from mesenchyme.
- Muscle tissue is specialized for contraction; skeletal muscle is voluntary, while cardiac and smooth are involuntary.
- Nervous tissue consists of neurons for signal transmission and glial cells for support.
- Cell junctions are critical: tight junctions create barriers, desmosomes provide strength, and gap junctions allow communication.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

