System Overview - The Body's Filter
- Primary Role: Filters blood to produce urine, removing waste while retaining essential substances. Regulates blood volume, pressure, pH, and electrolyte balance.
- Key Components:
- Kidneys: Paired, bean-shaped organs; the primary filtration units.
- Ureters: Tubes carrying urine from kidneys to the bladder.
- Bladder: Muscular sac for urine storage.
- Urethra: Tube for urine excretion.

⭐ The kidneys are retroperitoneal organs (except for the anterior surface), making them accessible from a posterior surgical approach, which avoids entering the peritoneal cavity.
📌 Mnemonic (Retroperitoneal Organs): SAD PUCKER
Kidney Gross Anatomy - Bean-Shaped Powerhouse

- Location: Retroperitoneal, at T12-L3 level. The right kidney is slightly lower than the left.
- Structure (External to Internal):
- Renal Capsule: Fibrous outer covering.
- Cortex: Outer parenchyma containing glomeruli and convoluted tubules.
- Medulla: Inner parenchyma arranged in pyramids, containing Loops of Henle and collecting ducts. Renal columns are cortical extensions between pyramids.
- Urine Flow: Papilla → Minor Calyx → Major Calyx → Renal Pelvis → Ureter.
- Hilum (Anterior → Posterior): Renal Vein, Artery, Ureter. 📌 Mnemonic: VAU.
⭐ The left renal vein is longer than the right and passes between the superior mesenteric artery (SMA) and the aorta. This anatomical course makes it susceptible to compression, leading to "Nutcracker Syndrome".
Ureters, Bladder, Urethra - The Plumbing Crew
-
Ureters: Muscular tubes carrying urine from kidneys to bladder; retroperitoneal.
- Three constrictions (sites of stone impaction): ureteropelvic jct (UPJ), pelvic inlet, ureterovesical jct (UVJ).
- 📌 Mnemonic: "Water (urine) flows under the bridge (uterine a. / vas deferens)."
-
Bladder: Hollow organ with detrusor muscle; stores urine.
- Lined by transitional epithelium (urothelium).
- Trigone: Smooth triangular area between ureteric orifices and internal urethral orifice.
-
Urethra: Drains urine from bladder.
- Female: Short (~4 cm); ↑ risk of UTIs.
- Male: Long (~20 cm); 3 parts (prostatic, membranous, spongy).
⭐ High-Yield: The most common site for kidney stone obstruction is the ureterovesical junction (UVJ), the narrowest point of the ureter.
Vasculature & Innervation - Power and Control
- Arterial Supply: Follows a precise path to the glomerulus.
- Venous Drainage: Mirrors the arterial path, exiting via the renal vein into the IVC.
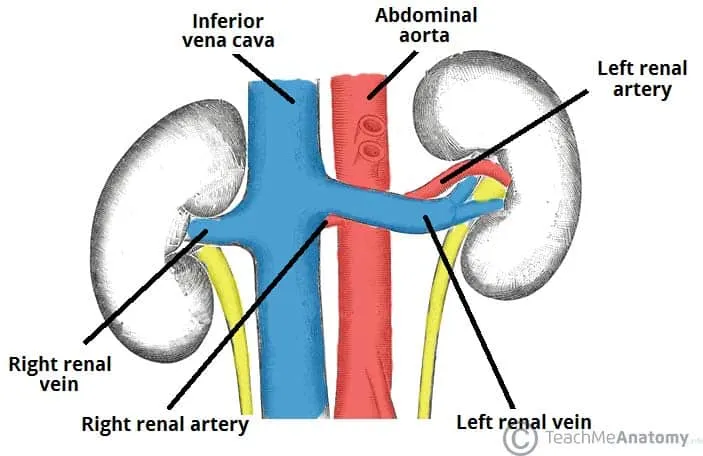
- Innervation: Primarily autonomic.
- Sympathetic (T10-L1): Vasoconstricts afferent arterioles → ↓ RBF & GFR. Stimulates renin release.
- Parasympathetic (Vagus/Pelvic Splanchnic): Vagal fibers to kidney (role unclear); pelvic splanchnics (S2-S4) cause detrusor contraction for micturition.
⭐ Exam Favorite: Kidneys receive 20-25% of the total cardiac output, highlighting their immense filtration role.
- The kidneys are retroperitoneal organs located at the T12-L3 vertebral level; the right kidney is typically lower than the left.
- From anterior to posterior, the structures at the renal hilum are the Renal Vein, Renal Artery, and Renal Pelvis (VAP).
- Ureters have three physiological constrictions where stones often lodge: the ureteropelvic junction (UPJ), the pelvic brim, and the ureterovesical junction (UVJ).
- The left renal vein is longer and passes between the superior mesenteric artery (SMA) and the aorta.
- The adrenal glands sit superior to the kidneys but are embryologically and functionally distinct.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

