Male Reproductive System - The Production Line
- Primary Function: Produce, maintain, and transport sperm & protective fluid (semen).
- Key Structures & Pathway:
- Testis: Site of spermatogenesis (Seminiferous tubules) & testosterone production (Leydig cells).
- Epididymis: Sperm maturation and storage.
- Vas Deferens: Transports mature sperm.
- Accessory Glands: Add seminal fluid.
- Seminal Vesicles: Fructose (energy), prostaglandins.
- Prostate Gland: Citrate, PSA.
- Bulbourethral Glands: Pre-ejaculate (lubrication).
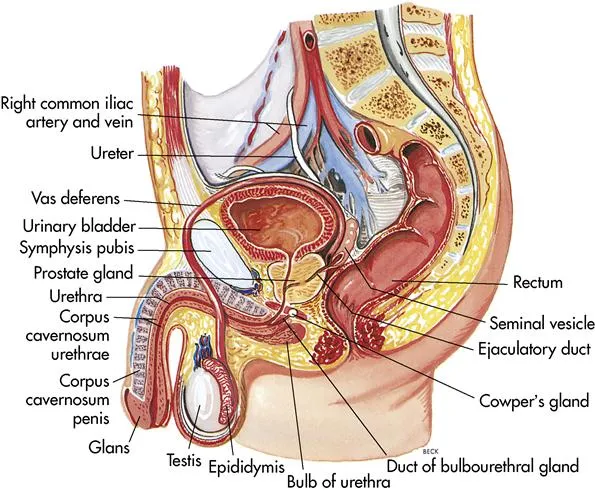
⭐ Exam Favorite: Seminal vesicles contribute ~70% of semen volume, providing fructose as the primary energy source for sperm motility.
📌 Mnemonic (Sperm Pathway): SEVEN UP - Seminiferous tubules, Epididymis, Vas deferens, Ejaculatory duct, Nothing, Urethra, Penis.
Female Reproductive System - The Ovarian Odyssey
- Ovary Anatomy: Cortex contains follicles; Medulla has blood vessels. Dual function: oogenesis & hormone production (estrogen, progesterone).
- Ovarian Cycle: A two-phase process driven by gonadotropins.
- Follicular Phase (Days 1-14): FSH stimulates follicle growth, leading to ↑ estrogen.
- Ovulation (Day 14): A surge in LH triggers the release of the oocyte.
- Luteal Phase (Days 15-28): Corpus luteum forms, secreting progesterone.
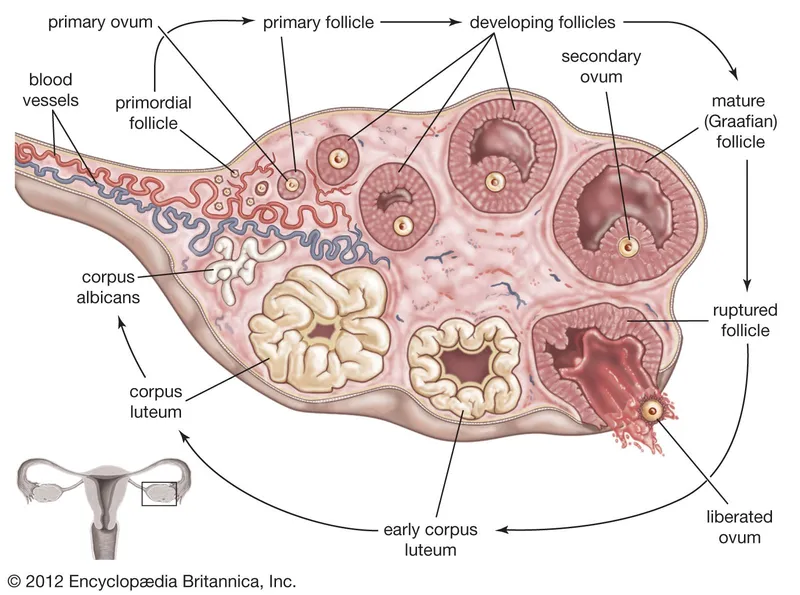
⭐ High-Yield: The pre-ovulatory LH surge is the critical trigger for the primary oocyte (arrested in Prophase I) to complete Meiosis I, becoming a secondary oocyte (arrested in Metaphase II).
Gametogenesis - Crafting the Cells
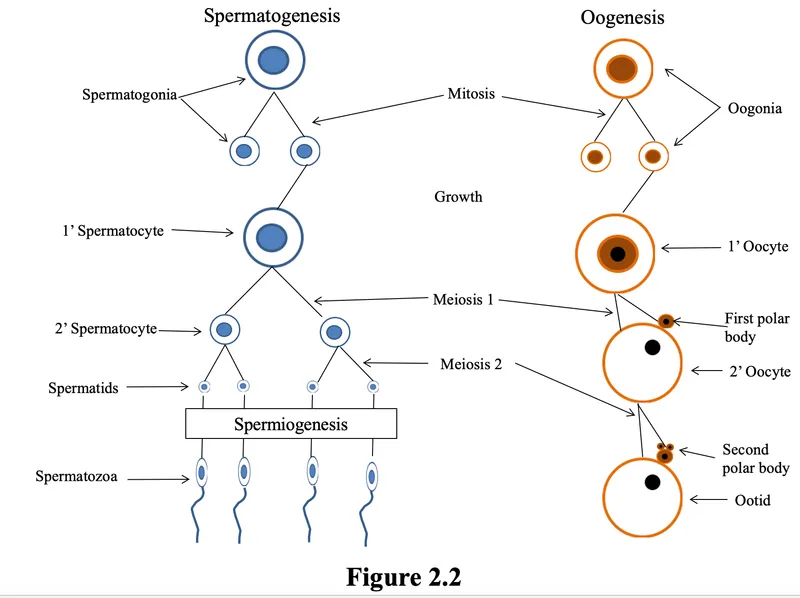
- Gametogenesis: Production of gametes (sperm & ova) via meiosis, reducing chromosome number from diploid (2n) to haploid (n).
-
Spermatogenesis:
- Location: Seminiferous tubules.
- Onset: Puberty; a continuous process.
- Duration: ~74 days.
- Result: 1 primary spermatocyte → 4 spermatozoa.
-
Oogenesis:
- Location: Ovaries.
- Onset: In utero; a discontinuous process.
- Result: 1 primary oocyte → 1 ovum + polar bodies.
⭐ Oocytes arrest in Prophase I from fetal life until puberty. After ovulation, the secondary oocyte arrests in Metaphase II until fertilization.
Hormonal Regulation - The Endocrine Orchestra

- HPG Axis: Pulsatile GnRH from the hypothalamus drives the pituitary to release LH & FSH, which target the gonads. Negative feedback regulates the system.
- Male Action:
- LH → Leydig cells → Testosterone.
- FSH → Sertoli cells → Spermatogenesis & Inhibin B.
- 📌 LH stimulates Leydig; Sertoli Sustains Sperm.
- Female Action:
- LH → Theca cells → Androgens.
- FSH → Granulosa cells → Estradiol (via aromatase).
⭐ Failure of GnRH-producing neurons to migrate from the olfactory placode results in Kallmann syndrome (hypogonadotropic hypogonadism + anosmia).
High‑Yield Points - ⚡ Biggest Takeaways
- The left gonadal vein drains to the left renal vein; the right gonadal vein drains directly to the IVC.
- Testicular/ovarian lymph drains to paraaortic nodes; scrotal/vulvar lymph drains to superficial inguinal nodes.
- The suspensory ligament of the ovary contains the crucial ovarian artery and vein.
- Erection is parasympathetic (S2-S4); ejaculation is sympathetic (L1-L2).
- The round ligament of the uterus passes through the deep inguinal ring.
- The vas deferens joins the seminal vesicle duct, forming the ejaculatory duct within the prostate.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

