Reproductive Health

On this page
Reproductive Transitions: Foundations of Contraception and Menopausal Care
Women's reproductive health spans decades, from menarche through menopause, requiring clinicians to master both contraceptive strategies and the management of oestrogen decline. A 32-year-old requesting reliable contraception and a 51-year-old experiencing vasomotor symptoms represent distinct but interconnected challenges in reproductive medicine. Understanding the epidemiology, hormonal physiology, and evidence-based interventions for both and forms the foundation for comprehensive women's health care.
Contraceptive Epidemiology and Classifications:
-
Failure rates expressed as Pearl Index (pregnancies per 100 woman-years):
- Long-acting reversible contraception (LARC): 0.2-0.8%
- Combined hormonal contraception (CHC): 0.3% perfect use, 9% typical use
- Barrier methods: 2% (male condom, perfect use), 18% typical use
- Emergency contraception: levonorgestrel 1.5-2.4% failure, ulipristal acetate 1.4%
-
UK usage patterns: 44% of women aged 16-49 use contraception; 28% use oral contraceptives, 10% LARC methods
-
Unmet contraceptive need: 17% of sexually active women report unplanned pregnancy risk due to inconsistent or no contraceptive use
Menopausal Epidemiology and Definitions:
-
Average age of menopause: 51 years (UK); premature ovarian insufficiency (POI) defined as <40 years
-
Prevalence of symptoms: 80% experience vasomotor symptoms, 50% report moderate-to-severe impact on quality of life
-
Duration: Median symptom duration 7.4 years; 10% experience symptoms >12 years
📌 Mnemonic for LARC methods: "IIDD" - Implant, Intrauterine (copper/hormonal), Depot injection, Duration (years: 3-5-10)
| Contraceptive Method | Failure Rate (Perfect/Typical) | Duration of Action | Return to Fertility |
|---|---|---|---|
| Copper IUD (Cu-IUD) | 0.6% / 0.8% | 5-10 years | Immediate |
| Levonorgestrel IUS (52mg) | 0.2% / 0.2% | 5 years | Immediate |
| Etonogestrel implant | 0.05% / 0.05% | 3 years | Immediate |
| DMPA injection | 0.2% / 6% | 12 weeks | 6-12 months delay |
| CHC (pill/patch/ring) | 0.3% / 9% | Daily/weekly | Immediate |
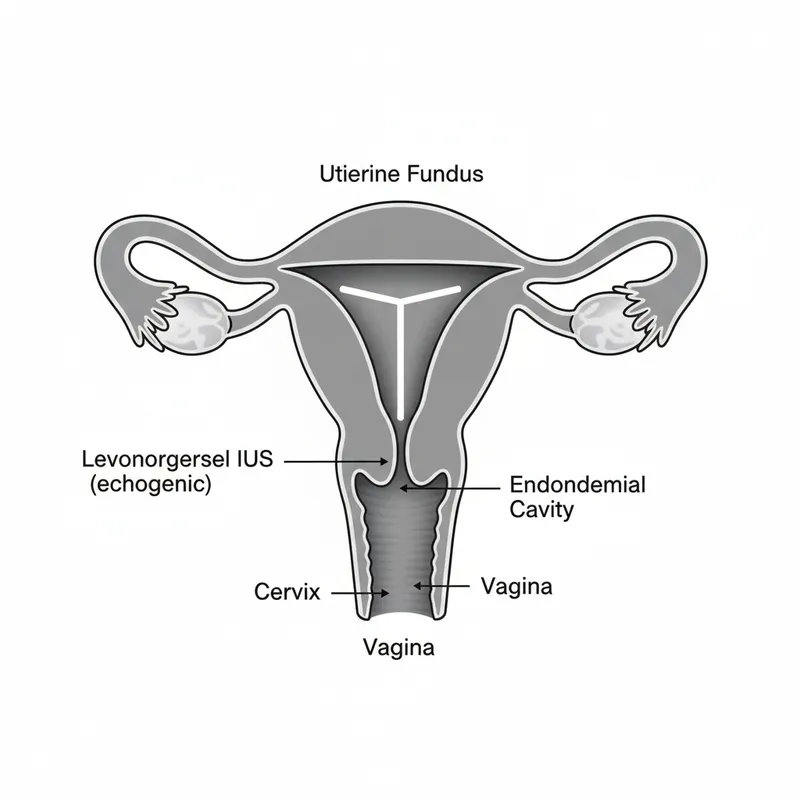
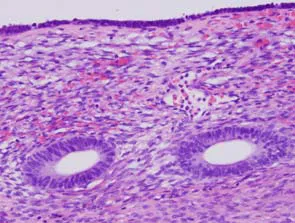
Reproductive Transitions: Foundations of Contraception and Menopausal Care
2 - Hormonal Mechanisms: From Ovulation Suppression to Oestrogen Decline
Contraceptive efficacy and menopausal symptoms both hinge on understanding hypothalamic-pituitary-ovarian (HPO) axis regulation. Combined hormonal contraceptives suppress the mid-cycle LH surge through negative feedback, preventing follicular maturation and ovulation, while progestogen-only methods primarily thicken cervical mucus and thin the endometrium. In contrast, menopause results from follicular depletion, causing erratic then absent oestradiol production, with FSH rising >25 IU/L as negative feedback diminishes. These opposing hormonal states-therapeutic suppression versus physiological decline-require different management approaches detailed in and .
Contraceptive Mechanisms:
-
CHC (ethinylestradiol 20-35 mcg + progestogen):
- Suppresses FSH → prevents follicular development
- Suppresses LH surge → prevents ovulation
- Thickens cervical mucus (progestogen effect)
- Thins endometrium → reduces implantation potential
-
Progestogen-only methods:
- Levonorgestrel IUS: local endometrial suppression (plasma levels 150-200 pg/mL)
- Desogestrel pill (75 mcg): ovulation suppression in 97% of cycles
- DMPA injection: suppresses ovulation, reduces oestradiol to early follicular phase levels
-
Copper IUD mechanism: Creates sterile inflammatory response toxic to sperm and ova; copper ions impair sperm motility and fertilisation
Menopausal Hormonal Changes:
-
Follicular depletion: Ovarian reserve declines from 300,000 at puberty to <1,000 by age 51
-
Hormonal transition (perimenopause):
- Early: FSH rises during follicular phase, cycles remain regular
- Late: FSH persistently >25 IU/L, oestradiol <100 pmol/L, amenorrhoea >60 days
-
Vasomotor symptom pathophysiology: Oestrogen withdrawal narrows thermoneutral zone in hypothalamus, triggering inappropriate heat-dissipation responses (flushing, sweating)
2 — Hormonal Mechanisms: From Ovulation Suppression to Oestrogen Decline
3 - Clinical Assessment: Selecting Contraception and Diagnosing Menopause
A 28-year-old with BMI 32 and migraine with aura requests contraception; a 49-year-old reports irregular periods and night sweats. Both scenarios require structured assessment using UK Medical Eligibility Criteria (UKMEC) for contraceptive safety and clinical diagnosis of menopause per NICE NG23. The contraceptive history must identify UKMEC 3-4 conditions (absolute/relative contraindications), while menopausal assessment focuses on symptom impact and cardiovascular/bone health risk stratification, as detailed in and .
Contraceptive Assessment Using UKMEC:
-
UKMEC categories:
- Category 1: No restriction
- Category 2: Benefits generally outweigh risks
- Category 3: Risks usually outweigh benefits (specialist input advised)
- Category 4: Unacceptable health risk (absolute contraindication)
-
Key UKMEC 4 conditions for CHC:
- Migraine with aura (5-fold stroke risk)
- Current/history of VTE or thrombophilia
- BMI ≥35 kg/m² (relative contraindication; consider UKMEC 3)
- Smoking ≥15 cigarettes/day if age ≥35
- Uncontrolled hypertension (≥160/100 mmHg)
-
LARC advantages: UKMEC 1-2 for most women, including those with cardiovascular risk factors
Menopausal Diagnosis (NICE NG23):
-
Clinical diagnosis (age >45): Based on vasomotor symptoms + menstrual irregularity; FSH testing not routinely required
-
FSH testing indicated:
- Age 40-45 with atypical symptoms
- Age <40 (suspected POI): FSH >25 IU/L on two occasions 4-6 weeks apart
-
Symptom severity assessment: Greene Climacteric Scale or Menopause-Specific Quality of Life questionnaire
| UKMEC Category | CHC Contraindications | Alternative Safe Options |
|---|---|---|
| 4 (Absolute) | Migraine with aura, VTE history, age ≥35 + smoking ≥15/day | Copper IUD, LNG-IUS, implant, POP |
| 3 (Relative) | BMI 35-39, controlled hypertension, diabetes >20 years | LNG-IUS (first-line), copper IUD, desogestrel POP |
| 2 (Caution) | BMI 30-34, family history VTE, age ≥35 + smoking <15/day | CHC acceptable; counsel on VTE risk |
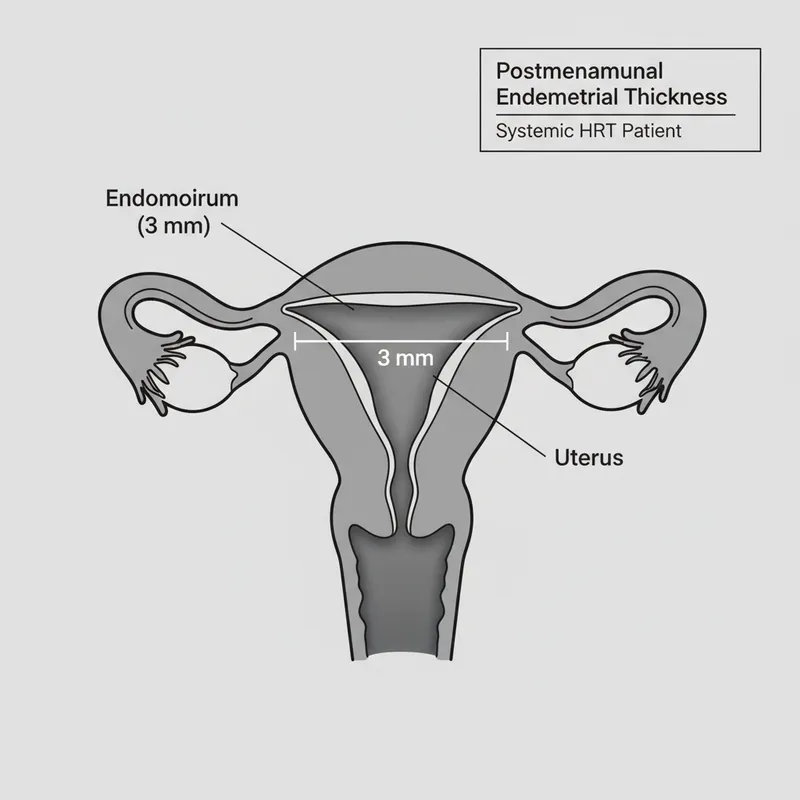
3 — Clinical Assessment: Selecting Contraception and Diagnosing Menopause
4 - Differential Considerations: Contraceptive Complications and Menopausal Mimics
Distinguishing contraceptive side effects from serious complications, and menopausal symptoms from pathology, requires analytical precision. Breakthrough bleeding on the levonorgestrel IUS may represent benign progestogenic endometrial changes or endometrial pathology requiring investigation. Similarly, vasomotor symptoms at age 45 could indicate perimenopause, hyperthyroidism, or carcinoid syndrome. Clinical reasoning must weigh probabilities, identify red flags, and avoid anchoring bias, as explored in and .
Contraceptive Complication Differentials:
-
Unscheduled bleeding on CHC/POP:
- Benign adaptation (first 3 months): 30-50% incidence
- Missed pills, drug interactions (enzyme inducers)
- Pregnancy (perform test if suspicious)
- STI (chlamydia/gonorrhoea), cervical pathology
- Red flag: Persistent bleeding >3 months requires examination ± investigation
-
Pelvic pain with IUD:
- Expulsion (5% copper IUD, 3% LNG-IUS)
- Infection (PID risk 1:500, highest in first 20 days post-insertion)
- Ectopic pregnancy (risk 0.02% annually, but 50% of IUD failures are ectopic)
Menopausal Symptom Differentials:
-
Vasomotor symptoms:
- Hyperthyroidism: check TSH if palpitations, weight loss, tremor
- Carcinoid syndrome: flushing + diarrhoea + wheeze
- Phaeochromocytoma: episodic hypertension, headache, sweating
-
Irregular bleeding (age >45):
- Perimenopause (most common)
- Endometrial hyperplasia/cancer: refer if persistent IMB, PMB, or risk factors (obesity, PCOS, tamoxifen)
- Thyroid dysfunction: check TSH
| Feature | Perimenopause | Hyperthyroidism | Endometrial Cancer |
|---|---|---|---|
| Vasomotor symptoms | Yes (gradual onset) | Yes (abrupt, with tremor) | No |
| Menstrual pattern | Irregular, lengthening cycles | Variable | Persistent IMB/PMB |
| Key investigation | Clinical diagnosis | TSH <0.1 mIU/L | TVUS (endometrium >4mm) |
| Management | HRT if symptomatic | Carbimazole, propranolol | 2-week-wait referral |
4 — Differential Considerations: Contraceptive Complications and Menopausal Mimics
5 - Evidence-Based Management: Optimising Contraception and HRT
A 26-year-old with dysmenorrhoea requests contraception; a 53-year-old with moderate hot flushes and no contraindications seeks HRT. NICE NG68 recommends LARC as first-line contraception for efficacy and non-compliance independence, while NICE NG23 advocates body-identical HRT (transdermal oestradiol + micronised progesterone) to minimise VTE risk. Treatment selection integrates guideline recommendations, patient preferences, and individualised risk-benefit analysis, as detailed in and .
Contraceptive Management (NICE NG68):
-
First-line LARC options:
- Levonorgestrel IUS 52 mg: Reduces menstrual blood loss by 90%, licensed for heavy menstrual bleeding; also provides endometrial protection in HRT
- Copper IUD: Hormone-free, 10-year duration; increases menstrual bleeding 20-50%
- Etonogestrel implant 68 mg: Single-rod subdermal, 3-year duration; 50% amenorrhoea rate
-
Specific dosing:
- Emergency contraception: levonorgestrel 1.5 mg (within 72 hours) or ulipristal acetate 30 mg (within 120 hours)
- Desogestrel POP: 75 mcg daily (12-hour window, unlike traditional POP 3-hour window)
- DMPA: 150 mg IM every 12 weeks (maximum 2-year continuous use due to bone density concerns)
HRT Management (NICE NG23):
-
Body-identical HRT (first-line):
- Oestradiol: Transdermal gel 0.5-1.5 mg daily or patch 50-100 mcg twice weekly (lower VTE risk than oral)
- Progesterone: Micronised progesterone 200 mg nightly (if uterus present) for endometrial protection
- Duration: Minimum 3 months to assess efficacy; continue if symptomatic
-
Monitoring: Annual review of symptoms, bleeding pattern, cardiovascular risk; no routine FSH testing
-
Contraindications (absolute): Current breast cancer, undiagnosed vaginal bleeding, active VTE, untreated endometrial hyperplasia
| Contraceptive Method | Specific Indication | Dose/Route | Key Monitoring |
|---|---|---|---|
| LNG-IUS 52 mg | HMB, dysmenorrhoea, endometrial protection | Intrauterine, 5 years | Threads check 4-6 weeks |
| Copper IUD | Hormone-free, emergency contraception | Intrauterine, 5-10 years | STI screen at insertion |
| Desogestrel POP | Breastfeeding, UKMEC 3-4 for CHC | 75 mcg daily oral | BP annually |
| Transdermal oestradiol | Menopausal symptoms, lower VTE risk | 50-100 mcg patch twice weekly | Annual cardiovascular review |
5 — Evidence-Based Management: Optimising Contraception and HRT
6 - Complex Scenarios: Comorbidities, Special Populations, and Emerging Evidence
A 38-year-old with BMI 42, type 2 diabetes, and previous VTE requests contraception; a 55-year-old on tamoxifen for breast cancer reports severe vasomotor symptoms. These scenarios demand synthesis of multiple guidelines, understanding absolute contraindications, and recognising when specialist input is essential. The levonorgestrel IUS offers UKMEC 1 contraception and may improve glycaemic control in the first patient, while the oncology patient requires non-hormonal symptom management, as discussed in and .
Complex Contraceptive Scenarios:
-
Obesity + VTE history: Copper IUD or LNG-IUS (UKMEC 1); avoid all oestrogen-containing methods (UKMEC 4)
-
Enzyme-inducing drugs (carbamazepine, rifampicin): LARC unaffected; CHC/POP efficacy reduced (use alternative or increase dose)
-
Postpartum contraception: LARC insertion immediate post-placental (IUD) or at 6 weeks; CHC contraindicated if breastfeeding <6 weeks postpartum (UKMEC 4)
-
Learning disability/capacity concerns: LARC preferred (reduces compliance burden); consider safeguarding if coercion suspected
Complex Menopausal Scenarios:
-
Premature ovarian insufficiency (age <40): HRT recommended until natural menopause age (51) to prevent osteoporosis, cardiovascular disease; FSH >25 IU/L diagnostic
-
Breast cancer survivors: Avoid systemic HRT; consider venlafaxine 37.5-75 mg, CBT, or vaginal oestrogen (minimal absorption) for genitourinary symptoms
-
Cardiovascular disease: Transdermal oestradiol preferred (no first-pass hepatic effect, lower VTE/stroke risk than oral); initiate within 10 years of menopause (window of opportunity)
-
Osteoporosis prevention: HRT reduces fracture risk 30-40%; bisphosphonates if HRT contraindicated
| Special Population | Contraceptive Choice | HRT Considerations |
|---|---|---|
| BMI >35 + VTE history | Copper IUD, LNG-IUS | Transdermal oestradiol (if no breast cancer history) |
| Migraine with aura | POP, implant, IUD | HRT not contraindicated (stroke risk lower than CHC) |
| Type 1 diabetes | LARC preferred | HRT safe; monitor glycaemic control |
| Breast cancer history | Copper IUD, barrier | Avoid systemic HRT; venlafaxine, CBT |
6 — Complex Scenarios: Comorbidities, Special Populations, and Emerging Evidence
High Yield Summary
Key Take-Aways:
- LARC methods (IUS, IUD, implant) have failure rates <1% and are first-line per NICE NG68 due to efficacy and compliance independence
- UKMEC Category 4 contraindications for CHC include migraine with aura, VTE history, BMI ≥35 with additional risk factors, and smoking ≥15/day if age ≥35
- Menopause is a clinical diagnosis in women >45 with vasomotor symptoms and irregular periods; FSH testing is not routinely required (NICE NG23)
- Body-identical HRT (transdermal oestradiol + micronised progesterone) minimises VTE risk and is first-line for symptomatic women without contraindications
- Levonorgestrel IUS provides dual benefits: highly effective contraception (0.2% failure) and 90% reduction in menstrual blood loss, plus endometrial protection in HRT users
- Absolute HRT contraindications: current breast cancer, undiagnosed vaginal bleeding, active VTE, untreated endometrial hyperplasia
- Premature ovarian insufficiency (menopause <40 years) requires HRT until age 51 to prevent long-term cardiovascular and bone complications
Essential Reproductive Health Numbers/Formulas:
| Parameter | Value | Clinical Significance |
|---|---|---|
| LNG-IUS failure rate | 0.2% | Most effective reversible contraception |
| CHC typical-use failure | 9% | Highlights compliance challenges |
| Copper IUD duration | 10 years | Longest-acting reversible method |
| Average menopause age | 51 years | POI if <40; perimenopause typically 45-55 |
| FSH diagnostic threshold | >25 IU/L (×2, 4-6 weeks apart) | Confirms POI in women <40 |
| HRT VTE risk (oral) | 2-fold increase | Transdermal avoids first-pass effect, lower risk |
| Median symptom duration | 7.4 years | Justifies long-term HRT consideration |
Key Principles/Pearls:
- LARC-first approach: Recommend IUS/IUD/implant before pills/patches to maximise efficacy and reduce unintended pregnancy
- UKMEC trumps preference: Absolute contraindications (Category 4) must be respected; never prescribe CHC to women with migraine with aura
- Menopause is clinical: Stop over-investigating with FSH in women >45; focus on symptom relief and shared decision-making
- Transdermal oestradiol preferred: Lower VTE/stroke risk than oral; essential in women with cardiovascular risk factors or obesity
- Avoid CHC pitfalls: Enzyme inducers (rifampicin, carbamazepine) reduce efficacy; missed pills in Week 1 carry highest pregnancy risk
Quick Reference:
| Scenario | First-Line Management | Key Monitoring/Follow-Up |
|---|---|---|
| Nulliparous woman requesting contraception | LNG-IUS 52 mg or copper IUD | Threads check 4-6 weeks, STI screen |
| BMI 38 + previous VTE | Copper IUD (UKMEC 1) | Annual cardiovascular review |
| Age 52, moderate hot flushes | Transdermal oestradiol 50 mcg + micronised progesterone 200 mg | 3-month symptom review, annual thereafter |
| Age 38, POI confirmed | HRT until age 51 (natural menopause) | DEXA scan, cardiovascular risk assessment |
| Breakthrough bleeding on CHC >3 months | Examine, STI screen, pregnancy test; consider switching formulation | Refer if persistent or red flags |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




