Pregnancy Medicine

On this page
Foundation: Risk Stratification and Screening Architecture in Pregnancy Medicine
A 32-year-old woman books her first antenatal appointment at 8 weeks gestation. Her BMI is 34 kg/m², she has a family history of type 2 diabetes, and her booking blood pressure is 138/86 mmHg. This scenario exemplifies why systematic risk assessment forms the cornerstone of modern pregnancy medicine. The National Institute for Health and Care Excellence (NICE) NG201 mandates structured screening at defined gestational windows, transforming pregnancy care from reactive symptom management to proactive risk mitigation. Understanding the temporal architecture of screening schedules and the physiological thresholds that trigger intervention pathways is essential for postgraduate clinicians managing complex obstetric populations.
-
Booking appointment (ideally 8-12 weeks):
- Risk stratification for hypertensive disorders: BMI >35, pre-existing hypertension, chronic kidney disease, autoimmune disease, family history of pre-eclampsia
- Aspirin 150 mg once daily from 12 weeks if ≥1 high-risk factor or ≥2 moderate-risk factors (NICE NG133)
- Baseline blood pressure, urinalysis for proteinuria, renal function
-
Gestational diabetes screening thresholds (NICE NG3):
- Oral glucose tolerance test (OGTT) at 24-28 weeks if: BMI >30 kg/m², previous macrosomia (≥4.5 kg), previous gestational diabetes, first-degree relative with diabetes, South Asian/Black Caribbean/Middle Eastern ethnicity
- Diagnostic criteria: fasting glucose ≥5.6 mmol/L OR 2-hour glucose ≥7.8 mmol/L
- Earlier OGTT (16-18 weeks) if previous with immediate post-booking HbA1c if high suspicion
-
Blood pressure monitoring frequency:
- Uncomplicated pregnancy: each antenatal contact (minimum 10 visits for nulliparous, 7 for multiparous)
- Chronic hypertension: every 2-4 weeks until 28 weeks, then weekly
- Gestational hypertension: twice-weekly BP and urinalysis until delivery
| Risk Category | Screening Timing | Intervention Threshold | Escalation Action |
|---|---|---|---|
| Pre-eclampsia (high-risk) | Weekly from 20 weeks | BP ≥140/90 + proteinuria ≥300 mg/24h | Twice-weekly monitoring, consider admission |
| Gestational diabetes | OGTT 24-28 weeks | Fasting ≥5.6 mmol/L or 2h ≥7.8 mmol/L | Dietary modification, self-monitoring |
| Chronic hypertension | Every 2-4 weeks pre-28 weeks | BP ≥150/100 mmHg | Increase antihypertensive therapy |
| Fetal growth restriction | Serial USS from 24 weeks if risk factors | Abdominal circumference <10th centile | Umbilical artery Doppler, twice-weekly CTG |
📌 Mnemonic for Pre-eclampsia Risk Factors (HIGH-RISK): "CHRONIC KIDNEY PROBLEMS" - Chronic hypertension, History of pre-eclampsia, Renal disease, Older age (>40), Nulliparity, Immune conditions, Chronic diabetes
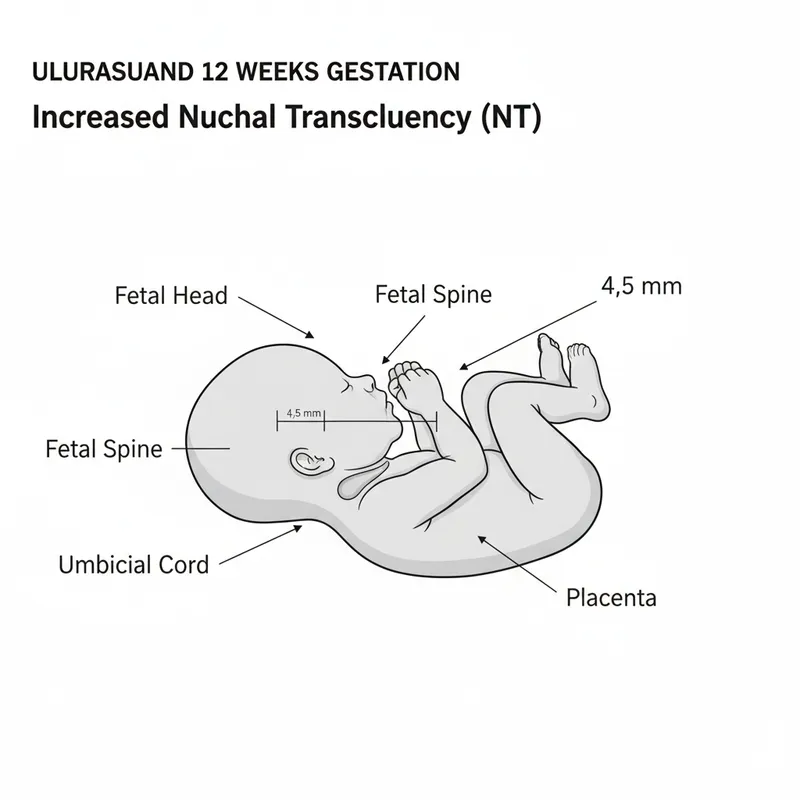
Foundation: Risk Stratification and Screening Architecture in Pregnancy Medicine
Mechanisms: Pathophysiological Drivers of Pregnancy-Specific Disorders
The placenta functions as an endocrine and immunological interface, and its dysfunction underpins both hypertensive disorders and metabolic complications. In , inadequate trophoblast invasion during early gestation results in failure of spiral artery remodeling-vessels remain high-resistance rather than transforming into low-resistance conduits. This placental hypoperfusion triggers release of anti-angiogenic factors (sFlt-1, soluble endoglin) that overwhelm circulating pro-angiogenic factors (VEGF, PlGF), causing systemic endothelial dysfunction. The resulting syndrome manifests as hypertension (BP ≥140/90 mmHg after 20 weeks), proteinuria (≥300 mg/24h), and end-organ damage affecting kidneys (creatinine >90 μmol/L), liver (transaminases >70 IU/L), and brain (visual disturbances, hyperreflexia).
-
Insulin resistance cascade in :
- Placental hormones (human placental lactogen, progesterone, cortisol) antagonize insulin receptor signaling
- Pancreatic β-cell dysfunction prevents compensatory insulin hypersecretion
- Maternal hyperglycemia → fetal hyperinsulinemia → macrosomia (birthweight >4 kg in 15-25% of untreated cases)
-
Cardiovascular adaptations necessitating monitoring:
- Plasma volume increases 40-50% by 32 weeks (physiological dilutional anemia)
- Cardiac output increases 30-50% (stroke volume and heart rate both rise)
- Systemic vascular resistance decreases 25-30% (progesterone-mediated smooth muscle relaxation)
- Why BP typically falls in second trimester: Maximal vasodilation at 20-24 weeks, then gradual rise toward term
| Physiological Parameter | Pre-Pregnancy | Peak Pregnancy Change | Clinical Implication |
|---|---|---|---|
| Plasma volume | 2600 mL | +1200 mL (46% increase) | Dilutional anemia (Hb <110 g/L acceptable) |
| Cardiac output | 4.5 L/min | 6.0-7.0 L/min | Decompensation in pre-existing cardiac disease |
| Glomerular filtration rate | 110 mL/min | 150 mL/min (36% increase) | Lower creatinine threshold for concern (>75 μmol/L) |
| Fasting glucose | 4.0-5.5 mmol/L | 3.5-5.0 mmol/L | Lower diagnostic threshold for gestational diabetes |
Mechanisms: Pathophysiological Drivers of Pregnancy-Specific Disorders
Clinical Application: Implementing NICE Guidance in Common Scenarios
A 28-year-old woman at 32 weeks gestation presents with headache and right upper quadrant pain. Her blood pressure is 156/102 mmHg (baseline 118/72 mmHg at booking), and urinalysis shows 2+ protein. This presentation demands immediate assessment for pre-eclampsia with severe features, as outlined in protocols. The diagnostic sequence prioritizes time-critical investigations: platelet count (thrombocytopenia <100×10⁹/L suggests HELLP syndrome), liver transaminases (AST/ALT >70 IU/L), creatinine (rising values indicate renal involvement), and quantified proteinuria (spot protein:creatinine ratio >30 mg/mmol or 24-hour collection ≥300 mg).
-
NICE NG133 thresholds for intervention:
- Mild gestational hypertension (140-149/90-99 mmHg): Weekly BP/urinalysis, no antihypertensives unless chronic hypertension
- Moderate hypertension (150-159/100-109 mmHg): Labetalol 200 mg TDS (first-line), nifedipine MR 10 mg BD (second-line), methyldopa 250 mg TDS (third-line)
- Severe hypertension (≥160/110 mmHg): Same-day assessment, admit if systolic ≥160 mmHg sustained, IV labetalol or hydralazine if oral therapy fails
-
** management thresholds:**
- Dietary modification alone if fasting glucose <7.0 mmol/L and 1-hour post-prandial <7.8 mmol/L (or 2-hour <6.4 mmol/L)
- Metformin (start 500 mg OD, titrate to 1 g BD) if fasting ≥7.0 mmol/L at diagnosis OR targets not met within 1-2 weeks of dietary changes
- Insulin if fasting ≥7.0 mmol/L despite maximal metformin (2 g/day) or fasting ≥6.0 mmol/L with macrosomia/polyhydramnios
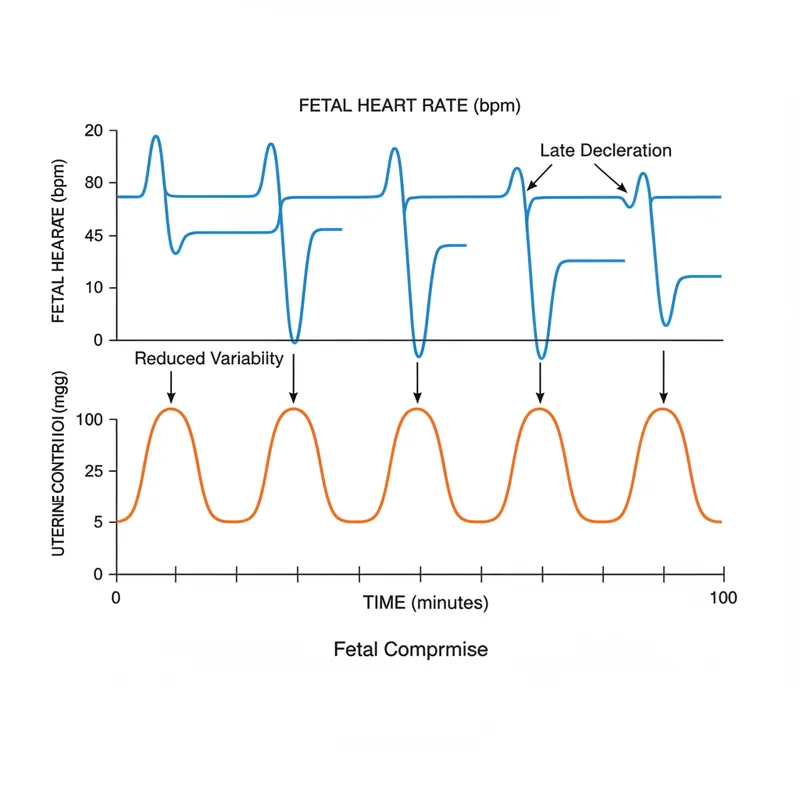
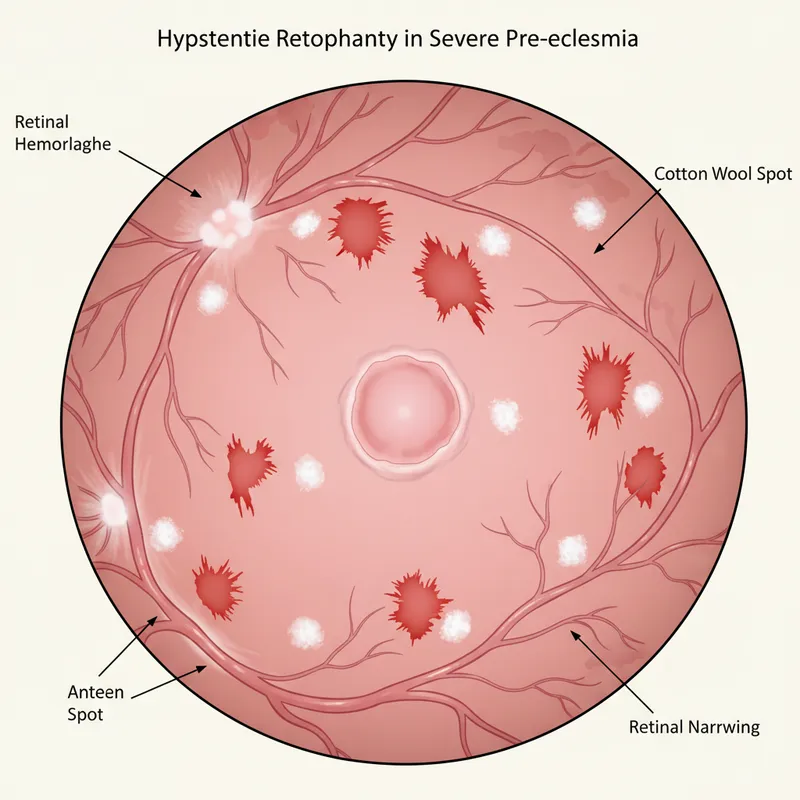
Clinical Application: Implementing NICE Guidance in Common Scenarios
Analysis: Differentiating Hypertensive Syndromes and Interpreting Risk Profiles
The critical distinction between chronic hypertension, gestational hypertension, and pre-eclampsia determines management intensity and delivery timing. Chronic hypertension (present before 20 weeks or pre-conception) carries 15-25% risk of superimposed pre-eclampsia, requiring enhanced surveillance as outlined in . Gestational hypertension emerging after 20 weeks without proteinuria has 25% progression risk to pre-eclampsia-the key discriminator is end-organ involvement. Pre-eclampsia with severe features (thrombocytopenia, pulmonary edema, cerebral symptoms, hepatic dysfunction) mandates delivery regardless of gestational age if maternal stabilization fails within 24-48 hours.
-
Risk factor interpretation for escalation decisions:
- Nulliparity increases pre-eclampsia risk 3-fold (baseline 2-5% → 6-15%)
- Previous pre-eclampsia confers 15% recurrence risk (higher if severe disease <28 weeks)
- Chronic kidney disease (pre-pregnancy creatinine >120 μmol/L) increases risk 5-fold
- Multiple pregnancy doubles risk (7-10% vs 3-5% in singletons)
-
Comparing management pathways in :
- Gestational hypertension without proteinuria: Deliver at 37 weeks if controlled
- Pre-eclampsia without severe features: Deliver at 37 weeks
- Pre-eclampsia with severe features: Deliver immediately if ≥34 weeks, consider expectant management with corticosteroids if 24-34 weeks in tertiary center
| Condition | Timing of Onset | Proteinuria | Delivery Threshold | Key Discriminator |
|---|---|---|---|---|
| Chronic hypertension | <20 weeks or pre-conception | Absent (unless superimposed pre-eclampsia) | 37-38 weeks if controlled | Pre-existing diagnosis or booking BP ≥140/90 |
| Gestational hypertension | ≥20 weeks | Absent | 37 weeks | No end-organ damage |
| Pre-eclampsia | ≥20 weeks | ≥300 mg/24h or PCR ≥30 | 37 weeks (earlier if severe features) | Proteinuria + end-organ dysfunction |
| HELLP syndrome | Usually ≥28 weeks | Variable | Immediate delivery | Hemolysis, elevated liver enzymes, low platelets |
Analysis: Differentiating Hypertensive Syndromes and Interpreting Risk Profiles
Evaluation: Evidence-Based Pharmacotherapy and Monitoring Strategies
The therapeutic goal in hypertensive disorders balances maternal cerebrovascular protection (reducing stroke risk at BP ≥160/110 mmHg) against maintaining uteroplacental perfusion. NICE NG133 stratifies antihypertensive choice by safety profile and efficacy data. Labetalol (combined α/β-blocker) achieves BP control in 70-80% of cases without compromising fetal growth, but is contraindicated in asthma. Nifedipine modified-release (calcium channel blocker) serves as second-line with similar efficacy, while methyldopa (centrally-acting α₂-agonist) is relegated to third-line due to higher rates of maternal sedation and depression.
-
Labetalol dosing in :
- Start 200 mg TDS, titrate to 400 mg TDS (maximum 1200 mg/day in divided doses)
- Monitor for maternal bradycardia (target heart rate >60 bpm)
- Contraindications: asthma, heart block, heart failure
-
Nifedipine MR regimen:
- Start 10 mg BD, increase to 20 mg BD (maximum 40 mg BD)
- Avoid immediate-release formulation (precipitous BP drop risks placental hypoperfusion)
- Caution with concurrent magnesium sulfate (potentiated hypotension)
-
** pharmacotherapy:**
- Metformin 500 mg OD with meals, increase by 500 mg weekly to maximum 1 g BD
- Crosses placenta but no teratogenicity in randomized trials (MiG trial: similar neonatal outcomes to insulin)
- Insulin regimen: Basal-bolus with human insulin (e.g., Insulatard 10 units bedtime, Actrapid 4 units pre-meals), titrate to targets
- Targets: Fasting <5.3 mmol/L, 1-hour post-prandial <7.8 mmol/L, 2-hour <6.4 mmol/L
| Medication | Starting Dose | Maximum Dose | Monitoring Parameter | Contraindication |
|---|---|---|---|---|
| Labetalol | 200 mg TDS | 400 mg TDS (1200 mg/day) | Heart rate >60 bpm, BP target 135/85 | Asthma, heart block |
| Nifedipine MR | 10 mg BD | 40 mg BD | BP target 135/85, avoid immediate-release | Avoid with MgSO₄ |
| Metformin | 500 mg OD | 1 g BD | Fasting and post-prandial glucose, renal function | eGFR <45 mL/min |
| Insulin (Actrapid) | 4 units pre-meals | Titrate to glucose targets | Capillary glucose 4× daily, HbA1c monthly | Hypoglycemia awareness |
Evaluation: Evidence-Based Pharmacotherapy and Monitoring Strategies
Advanced Integration: Multimorbidity and Special Populations
A 38-year-old woman with pre-existing type 2 diabetes (HbA1c 7.2% pre-conception) and BMI 38 kg/m² presents at 10 weeks gestation. She requires integrated care across , , and pathways. Pre-existing diabetes mandates immediate conversion from oral hypoglycemics to insulin (metformin continued if previously established), retinal screening at booking and 28 weeks, and early fetal echocardiography at 20 weeks (cardiac anomaly risk 3-5%). Her elevated BMI necessitates aspirin 150 mg daily from 12 weeks, serial growth scans from 28 weeks (macrosomia risk 20-30%), and anesthetic consultation by 36 weeks for delivery planning.
-
Complex risk stratification interactions:
- Chronic hypertension + diabetes: 30-40% risk of superimposed pre-eclampsia (vs 15% with hypertension alone)
- Obesity + gestational diabetes: Stillbirth risk 1.3% (vs 0.4% background), requiring twice-weekly CTG from 38 weeks
- Renal impairment (creatinine >120 μmol/L) + hypertension: Monthly creatinine monitoring, deliver by 37 weeks
-
Emerging evidence considerations:
- PlGF-based testing (NICE DG23): PlGF <100 pg/mL between 20-35 weeks has 96% negative predictive value for pre-eclampsia requiring delivery within 14 days
- Continuous glucose monitoring in type 1 diabetes pregnancy reduces neonatal hypoglycemia (CONCEPTT trial: 53% vs 70% with self-monitoring)
- Magnesium sulfate neuroprotection: 4 g IV loading dose, then 1 g/hour infusion if delivery anticipated <30 weeks (reduces cerebral palsy risk by 30%)
| Comorbidity Combination | Compounded Risk | Enhanced Surveillance | Delivery Timing |
|---|---|---|---|
| Chronic HTN + diabetes | Pre-eclampsia 30-40% | Weekly BP/urinalysis from 20 weeks, fortnightly growth scans | 37-38 weeks if stable |
| Obesity (BMI >40) + GDM | Stillbirth 1.3%, macrosomia 25% | Twice-weekly CTG from 38 weeks, growth scans every 3 weeks | 38-39 weeks |
| Renal disease + pre-eclampsia | Acute kidney injury 15% | Weekly creatinine, twice-weekly BP | 34-37 weeks depending on function |
| Multiple pregnancy + GDM | Preterm birth 50%, NICU admission 40% | Fortnightly growth scans from 24 weeks | 36-37 weeks for dichorionic twins |
Advanced Integration: Multimorbidity and Special Populations
High Yield Summary
Key Take-Aways:
- Aspirin 150 mg daily from 12 weeks reduces pre-eclampsia risk by 60% in high-risk women (≥1 major or ≥2 moderate risk factors)
- Gestational diabetes diagnostic thresholds: fasting ≥5.6 mmol/L OR 2-hour OGTT ≥7.8 mmol/L at 24-28 weeks
- Severe hypertension (≥160/110 mmHg) requires same-day assessment and treatment to prevent maternal stroke
- Labetalol 200 mg TDS is first-line antihypertensive; nifedipine MR 10 mg BD second-line (avoid immediate-release)
- Pre-eclampsia with severe features mandates delivery at ≥34 weeks after maternal stabilization
- Metformin initiated if fasting glucose ≥7.0 mmol/L at diagnosis or dietary measures fail within 1-2 weeks
- PlGF <100 pg/mL has 96% NPV for pre-eclampsia requiring delivery within 14 days
Essential Pregnancy Medicine Numbers:
| Parameter | Threshold | Action |
|---|---|---|
| Blood pressure | ≥140/90 mmHg after 20 weeks | Twice-weekly monitoring, consider treatment at ≥150/100 |
| Proteinuria | ≥300 mg/24h or PCR ≥30 mg/mmol | Diagnoses pre-eclampsia if BP elevated |
| Fasting glucose (OGTT) | ≥5.6 mmol/L | Gestational diabetes diagnosis |
| 2-hour glucose (OGTT) | ≥7.8 mmol/L | Gestational diabetes diagnosis |
| Platelets | <100×10⁹/L | Suggests HELLP syndrome, deliver if ≥34 weeks |
| Aspirin dose | 150 mg daily from 12 weeks | Pre-eclampsia prophylaxis in high-risk women |
Key Principles/Pearls:
- Blood pressure typically falls in second trimester (nadir at 20-24 weeks) due to maximal vasodilation-interpret readings in gestational context
- Never use ACE inhibitors or ARBs in pregnancy (teratogenic); labetalol/nifedipine/methyldopa are safe antihypertensives
- Gestational diabetes targets are tighter than non-pregnant diabetes: fasting <5.3 mmol/L (vs <7.0 mmol/L outside pregnancy)
- Pre-eclampsia can present without headache or visual symptoms-proteinuria + hypertension alone warrants close monitoring
- Avoid immediate-release nifedipine (precipitous BP drop risks placental hypoperfusion); use modified-release formulations only
Quick Reference:
| Condition | Diagnostic Criterion | First-Line Treatment | Delivery Timing |
|---|---|---|---|
| Gestational hypertension | BP ≥140/90, no proteinuria | Labetalol 200 mg TDS if ≥150/100 | 37 weeks |
| Pre-eclampsia | BP ≥140/90 + proteinuria ≥300 mg/24h | Labetalol, deliver at 37 weeks | 37 weeks (earlier if severe) |
| Gestational diabetes | Fasting ≥5.6 or 2h ≥7.8 mmol/L | Diet ± metformin 500 mg OD | 38-40 weeks if controlled |
| Chronic hypertension | BP ≥140/90 pre-conception or <20 weeks | Continue safe antihypertensive | 37-38 weeks if stable |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app






