Gynaecology

On this page
Recognising Bleeding Disorders: Foundations of Abnormal and Ectopic Bleeding
A 32-year-old woman presents with heavy periods requiring pad changes every hour, describing clots "the size of golf balls." Meanwhile, in the emergency department, a 28-year-old with 6 weeks amenorrhoea reports unilateral pelvic pain and light vaginal bleeding. These scenarios represent two critical gynaecological presentations-abnormal uterine bleeding and ectopic pregnancy -that demand systematic evaluation and timely intervention. Understanding their classifications, epidemiology, and diagnostic frameworks forms the cornerstone of competent gynaecological practice.
Abnormal Uterine Bleeding (AUB) Classification:
- PALM-COEIN system (FIGO 2011) stratifies causes into structural and non-structural:
- Structural (PALM): Polyp, Adenomyosis, Leiomyoma, Malignancy
- Non-structural (COEIN): Coagulopathy, Ovulatory dysfunction, Endometrial, Iatrogenic, Not classified
- Heavy menstrual bleeding (HMB): Excessive blood loss (>80ml/cycle) interfering with quality of life
- Affects 25% of women of reproductive age
- Accounts for 20% of gynaecology referrals in UK primary care
- Intermenstrual bleeding (IMB): Bleeding between regular cycles
- Postcoital bleeding (PCB): Bleeding after sexual intercourse-requires cervical assessment
Ectopic Pregnancy Essentials:
- Definition: Pregnancy implanted outside the uterine cavity
- 95% tubal (ampulla most common site)
- Rare sites: ovarian (3%), cervical, caesarean scar, abdominal
- Epidemiology:
- Incidence 11 per 1,000 pregnancies in UK
- Leading cause of maternal death in first trimester (6% of maternal deaths)
- Recurrence risk 10-15% after one ectopic
| Parameter | AUB | Ectopic Pregnancy |
|---|---|---|
| UK Prevalence | 25% reproductive-age women | 1.1% of all pregnancies |
| Peak Age | 40-50 years (HMB) | 30-34 years |
| Emergency Risk | Anaemia, rarely life-threatening | Life-threatening rupture |
| Mortality | <0.1% | 0.2-0.5% (if ruptured) |
📌 Mnemonic for Ectopic Risk Factors: PIPES
PID, IUD, Previous ectopic, Endometriosis, Surgery (tubal)
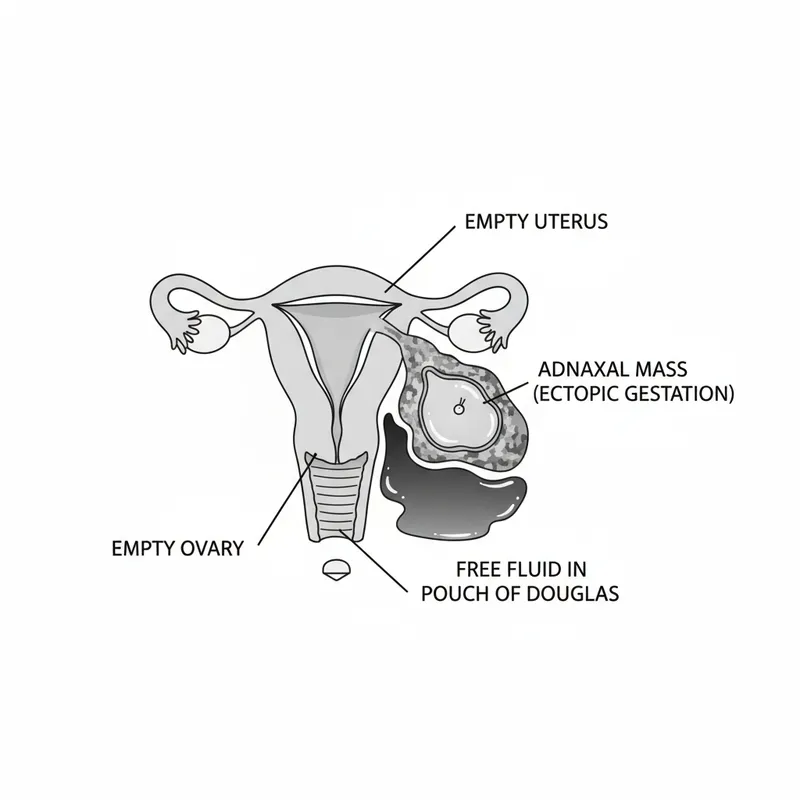
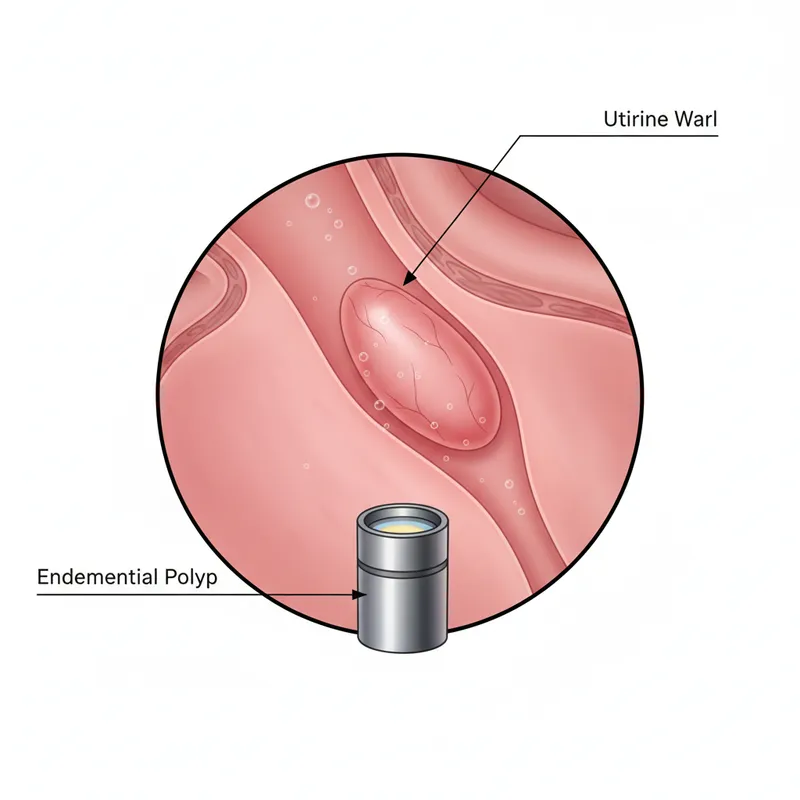
Recognising Bleeding Disorders: Foundations of Abnormal and Ectopic Bleeding
2 - Pathophysiological Mechanisms: Why Bleeding Occurs
The mechanisms underlying abnormal bleeding diverge fundamentally between structural uterine pathology and ectopic implantation. In abnormal uterine bleeding , disrupted endometrial haemostasis results from either anatomical distortion (fibroids creating increased surface area, adenomyosis disrupting myometrial contractility) or molecular dysregulation (increased prostaglandin E2/prostacyclin ratio, impaired vasoconstriction). Anovulatory cycles-common in PCOS and perimenopause-produce unopposed oestrogen stimulation, causing irregular endometrial proliferation without progesterone-mediated stabilisation, leading to unpredictable breakthrough bleeding.
AUB Mechanistic Pathways:
- Structural causes:
- Fibroids: Distort endometrial vasculature, increase surface area (submucosal worst)
- Adenomyosis: Ectopic endometrial glands in myometrium → impaired uterine contractility
- Polyps: Localised endometrial overgrowth with fragile vasculature
- Coagulopathy (13% of HMB):
- Von Willebrand disease most common (1% population prevalence)
- Platelet dysfunction, factor deficiencies
- Endometrial dysfunction:
- Altered prostaglandin ratios (↑ PGE2:PGF2α)
- Increased fibrinolysis (elevated tissue plasminogen activator)
- Impaired vasoconstriction
Ectopic Pregnancy Pathophysiology:
In ectopic pregnancy , impaired tubal transport allows blastocyst implantation in the fallopian tube. Risk factors-previous PID causing tubal scarring, endometriosis creating inflammatory milieu, tubal surgery disrupting ciliary function-all compromise the tube's ability to propel the embryo uterine-ward. The trophoblast invades the tubal wall, eroding blood vessels and causing bleeding into the peritoneal cavity. Unlike the muscular uterus, the thin-walled tube cannot accommodate growing gestational tissue, leading to rupture typically at 6-8 weeks gestation when β-hCG reaches 3,000-5,000 IU/L.
| Mechanism | Clinical Consequence | Investigation Marker |
|---|---|---|
| Unopposed oestrogen | Irregular heavy bleeding | Anovulatory progesterone <3 nmol/L |
| Fibroid distortion | Predictable HMB | MRI shows submucosal location |
| Tubal trophoblast invasion | Unilateral pain + bleeding | β-hCG plateau or slow rise |
| Tubal rupture | Haemodynamic collapse | Free fluid on USS, falling Hb |
2 — Pathophysiological Mechanisms: Why Bleeding Occurs
3 - Clinical Assessment: History, Examination, and Investigations
A 45-year-old presents with "flooding" periods lasting 9 days, passing clots, and requiring time off work. You quantify impact using a structured history, examine for structural causes, and order targeted investigations per NICE NG88 guidance. Meanwhile, a 26-year-old with positive pregnancy test and cramping requires urgent assessment for potential ectopic pregnancy , where clinical gestalt combined with serial β-hCG and transvaginal ultrasound determines management pathway.
History-Taking Priorities:
- AUB assessment:
- Quantify bleeding: Pictorial Blood Assessment Chart (PBAC >100 = HMB)
- Pattern: Regular/irregular, cycle length, intermenstrual/postcoital bleeding
- Impact: Anaemia symptoms (fatigue, palpitations), quality of life, fertility plans
- Risk factors: Obesity (anovulation), anticoagulation, PCOS, thyroid disease
- Ectopic pregnancy red flags:
- Triad: Amenorrhoea (6-8 weeks) + pelvic pain (unilateral) + vaginal bleeding
- Rupture indicators: Sudden severe pain, shoulder tip pain (diaphragmatic irritation), dizziness/syncope
Examination Findings:
- AUB: Abdominal masses (fibroids), bimanual examination (enlarged/tender uterus), speculum (exclude cervical pathology)
- Ectopic: Abdominal tenderness, cervical motion tenderness, adnexal mass (50%), peritonism if ruptured
Investigation Algorithm (NICE NG88 & NG126):
- AUB first-line:
- Full blood count: Hb <120 g/L indicates significant blood loss
- Ferritin: <15 μg/L confirms iron deficiency
- Coagulation screen if HMB since menarche or family history
- Pelvic USS: First-line imaging for structural causes
- Ectopic pregnancy pathway:
- Serum β-hCG: Discriminatory zone 1,500 IU/L (transvaginal USS should visualise intrauterine pregnancy)
- Transvaginal USS: Intrauterine gestational sac (confirms IUP), adnexal mass, free fluid
- Serial β-hCG (48h): Normal IUP rises >63%, ectopic typically <50% increase
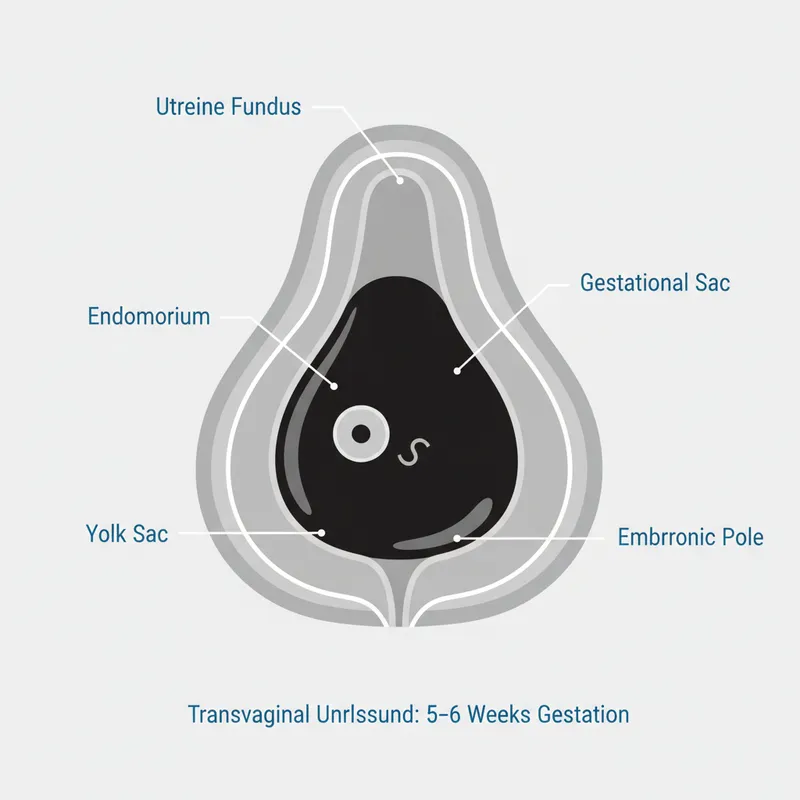
| Investigation | Threshold | Sensitivity | Specificity |
|---|---|---|---|
| β-hCG rise >63% (48h) | Normal IUP | 99% | 93% |
| β-hCG plateau/fall | Failing pregnancy | 88% | 95% |
| USS gestational sac | β-hCG >1,500 IU/L | 90% | 100% |
| Endometrial thickness | >16mm (AUB) | 67% for pathology | 89% |
3 — Clinical Assessment: History, Examination, and Investigations
4 - Differential Diagnosis: Distinguishing Bleeding Causes
Separating benign from life-threatening bleeding requires systematic analysis. A 34-year-old with irregular bleeding and negative pregnancy test differs fundamentally from one with positive test and pain-the latter demands urgent ectopic exclusion . Similarly, distinguishing ovulatory HMB (regular cycles, structural causes) from anovulatory bleeding (irregular, endocrine dysfunction) guides targeted management for abnormal uterine bleeding .
Key Discriminators:
- Pregnancy status: β-hCG positive = ectopic/miscarriage/molar until proven otherwise
- Cycle regularity:
- Regular cycles (21-35 days) → structural causes (fibroids, polyps, adenomyosis)
- Irregular cycles → anovulation (PCOS, thyroid, hyperprolactinaemia)
- Age stratification:
- <20 years: Coagulopathy (13% of adolescent HMB)
- 30-40 years: Fibroids, adenomyosis
-
45 years: Endometrial cancer (2% of PMB)-requires urgent investigation
Common Diagnostic Pitfalls:
- Assuming negative urine pregnancy test excludes ectopic: False negatives occur with low β-hCG
- Missing coagulopathy: Ask about bruising, dental bleeding, family history
- Overlooking cervical pathology: Always visualise cervix with speculum
- Attributing all irregular bleeding to PCOS: Exclude endometrial hyperplasia/cancer
| Feature | Ectopic Pregnancy | Miscarriage | Ovulatory HMB | Anovulatory Bleeding |
|---|---|---|---|---|
| Cycle Pattern | Amenorrhoea then bleeding | Amenorrhoea then bleeding | Regular heavy cycles | Irregular unpredictable |
| Pain | Unilateral, severe | Midline cramping | Dysmenorrhoea | Minimal |
| β-hCG Pattern | Slow rise (<50% in 48h) | Falling | N/A | N/A |
| USS Findings | Adnexal mass, no IUP | Products in uterus | Structural pathology | Thickened endometrium |
| Urgency | EMERGENCY | Urgent | Routine | Routine |
4 — Differential Diagnosis: Distinguishing Bleeding Causes
5 - Evidence-Based Management: Medical, Surgical, and Conservative Options
NICE NG88 advocates a stepwise approach to abnormal uterine bleeding , prioritising medical management unless structural pathology mandates surgery. First-line treatment-levonorgestrel intrauterine system (LNG-IUS)-reduces menstrual blood loss by 94% at 12 months, superior to all oral therapies. For ectopic pregnancy , NICE NG126 stratifies management by haemodynamic stability, β-hCG level, and patient preference, balancing tubal preservation against treatment success.
AUB Medical Management:
- First-line: LNG-IUS (Mirena®)
- Dose: 52mg levonorgestrel, releases 20μg/day
- Efficacy: 94% reduction in menstrual blood loss
- Contraindications: Current breast cancer, distorted uterine cavity
- Tranexamic acid: 1g TDS days 1-4 of menses (39% reduction)
- Mefenamic acid: 500mg TDS days 1-4 (20-25% reduction)
- Combined oral contraceptive: Regulates cycle, reduces flow (43% reduction)
AUB Surgical Options:
- Endometrial ablation: For completed childbearing, normal cavity
- Success: 80% satisfaction at 5 years
- 24% require further surgery
- Hysterectomy: Definitive treatment
- Laparoscopic preferred (shorter recovery, fewer complications)
- Mortality risk 0.38 per 1,000
Ectopic Pregnancy Management:
- Expectant management (selected cases):
- Criteria: β-hCG <1,000 IU/L, falling, minimal symptoms, reliable patient
- Success: 69% resolve without intervention
- Medical: Methotrexate
- Criteria: β-hCG <1,500 IU/L, unruptured, no fetal heartbeat, mass <35mm
- Dose: 50mg/m² IM single dose (or multi-dose protocol)
- Success: 88% (single dose), 93% (multi-dose)
- Monitoring: β-hCG days 4 and 7 (expect 15% drop); repeat if <15% fall
- Contraindications: Breastfeeding, immunodeficiency, renal/hepatic impairment
- Surgical: Laparoscopy
- Salpingectomy: Removes affected tube (preferred if damaged tube, recurrent ectopic)
- Salpingotomy: Preserves tube (if contralateral tube damaged, desire fertility)
- Emergency laparotomy: If haemodynamically unstable
| Treatment | Indication | Success Rate | Key Monitoring |
|---|---|---|---|
| LNG-IUS | First-line HMB | 94% reduction MBL | Review 3-6 months |
| Methotrexate | Ectopic β-hCG <1,500 | 88% single dose | β-hCG days 4, 7 |
| Salpingotomy | Ectopic + fertility desire | 93% success | 7% persistent trophoblast |
| Hysterectomy | Failed medical Rx | 100% cure | Surgical complications |
5 — Evidence-Based Management: Medical, Surgical, and Conservative Options
6 - Complex Scenarios: Special Populations and Advanced Cases
Real-world patients present nuanced challenges. A 38-year-old with HMB and concurrent anticoagulation for prosthetic heart valve requires coordinated cardiology input before considering surgical management . Similarly, a woman with recurrent ectopic pregnancy and single remaining tube faces difficult decisions balancing fertility preservation against treatment success . These scenarios demand synthesis of clinical evidence, patient values, and multidisciplinary expertise.
Challenging AUB Cases:
- Anticoagulation + HMB:
- Tranexamic acid safe with warfarin/DOACs (no thrombotic risk increase)
- LNG-IUS preferred (local effect, minimal systemic absorption)
- Avoid NSAIDs if on antiplatelet therapy
- Adolescent HMB:
- 13% have underlying coagulopathy-screen with PT, APTT, vWF antigen/activity
- Combined OCP first-line (regulates cycle, reduces flow)
- Avoid LNG-IUS (insertion difficult, poor tolerance)
- Perimenopausal bleeding:
- Exclude malignancy: Endometrial biopsy if >45 years with persistent IMB
- LNG-IUS prevents endometrial hyperplasia during HRT
- Failed medical management:
- Consider GnRH analogues (3-6 months pre-surgery to reduce fibroid size)
- Uterine artery embolisation: 85% satisfaction, preserves fertility potential
Complex Ectopic Scenarios:
- Pregnancy of unknown location (PUL):
- β-hCG <1,500, no USS findings
- Serial β-hCG protocol: 48h intervals until location confirmed or resolved
- 10-15% ultimately ectopic
- Caesarean scar ectopic:
- Rare (1:2,000) but increasing with rising CS rates
- High rupture risk-requires specialist management (methotrexate + local injection or surgery)
- Cornual/interstitial ectopic:
- Implantation in uterine horn
- Later rupture (12-16 weeks), catastrophic haemorrhage
- Requires laparotomy (not laparoscopy)-mortality 2-2.5%
| Scenario | Key Consideration | Management Modification |
|---|---|---|
| Anticoagulation + HMB | Bleeding risk vs thrombosis | Tranexamic acid safe, avoid NSAIDs |
| Single tube + ectopic | Fertility preservation | Salpingotomy if feasible, counsel re: IVF |
| β-hCG >5,000 + ectopic | High rupture risk | Surgery preferred over methotrexate |
| Perimenopausal IMB | Malignancy risk | Mandatory endometrial sampling |
6 — Complex Scenarios: Special Populations and Advanced Cases
High Yield Summary
Key Take-Aways:
- HMB affects 25% of women; LNG-IUS is first-line medical management (94% reduction in menstrual blood loss)
- Ectopic pregnancy occurs in 1.1% of pregnancies; discriminatory β-hCG threshold is 1,500 IU/L for transvaginal USS
- PALM-COEIN classification systematically categorises AUB causes into structural and non-structural
- Methotrexate criteria for ectopic: β-hCG <1,500, unruptured, mass <35mm, no fetal heartbeat-88% success rate
- Serial β-hCG in normal IUP rises >63% in 48 hours; slower rise suggests ectopic or failing pregnancy
- Endometrial sampling mandatory for women >45 years with persistent intermenstrual bleeding (exclude cancer)
- Ruptured ectopic presents with triad: sudden severe pain, shoulder tip pain (diaphragmatic irritation), haemodynamic instability
Essential Gynaecology Numbers:
| Parameter | Threshold | Clinical Significance |
|---|---|---|
| β-hCG discriminatory zone | 1,500 IU/L | USS should show IUP if present |
| Normal IUP β-hCG rise | >63% in 48h | <50% suggests ectopic/failing |
| Methotrexate β-hCG limit | <1,500 IU/L | Higher levels = surgery preferred |
| LNG-IUS MBL reduction | 94% at 12 months | Superior to all oral therapies |
| Endometrial thickness (AUB) | >16mm abnormal | Warrants further investigation |
| Ectopic recurrence risk | 10-15% | After one previous ectopic |
Key Principles:
- Always exclude pregnancy in reproductive-age women with bleeding-urine test insufficient if symptoms suggest ectopic
- Structured history trumps investigations: PBAC score, impact on quality of life, and fertility plans guide AUB management
- Haemodynamic stability determines urgency: Unstable ectopic requires immediate laparotomy regardless of investigations
- Medical management first for AUB unless contraindications (distorted cavity, malignancy) or patient preference for surgery
- Serial monitoring essential in pregnancy of unknown location: 10-15% ultimately ectopic, requiring vigilant β-hCG tracking
Quick Reference:
| Condition | First Investigation | First-Line Management | Red Flag |
|---|---|---|---|
| HMB (regular cycles) | FBC, ferritin, pelvic USS | LNG-IUS 52mg | Postmenopausal bleeding |
| HMB (irregular cycles) | Add TSH, prolactin | Combined OCP or LNG-IUS | Age >45 + IMB (cancer risk) |
| Suspected ectopic | β-hCG + transvaginal USS | Depends on stability/β-hCG | Shoulder tip pain, syncope |
| Pregnancy unknown location | Serial β-hCG (48h) | Expectant if falling | β-hCG plateau or slow rise |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Partner, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




