Quick Overview
Back pain affects 80% of adults during their lifetime; most cases are non-specific low back pain (NSLBP) resolving within 6 weeks. The critical skill is identifying red flags requiring urgent investigation/referral (cauda equina syndrome, malignancy, infection, fracture). NICE NG59 emphasizes avoiding routine imaging for NSLBP while ensuring serious pathology isn't missed. Systematic red flag screening is essential for safe management.
Core Facts & Concepts
Red Flag Categories (4 Major Groups):
| Category | Key Features | Urgency |
|---|---|---|
| Cauda Equina Syndrome (CES) | Bilateral sciatica, saddle anaesthesia, urinary retention/incontinence, fecal incontinence, progressive leg weakness | Emergency MRI <24h |
| Spinal Infection | Fever, IV drug use, immunosuppression, recent UTI/bacteremia, night sweats, TB risk factors | Urgent MRI + bloods |
| Malignancy | Age >50, unexplained weight loss, past cancer history, night pain, thoracic pain, progressive symptoms >4-6 weeks | Urgent MRI ± XR |
| Fracture | Significant trauma, age >50 + minor trauma, prolonged corticosteroid use, osteoporosis | XR spine ± MRI |
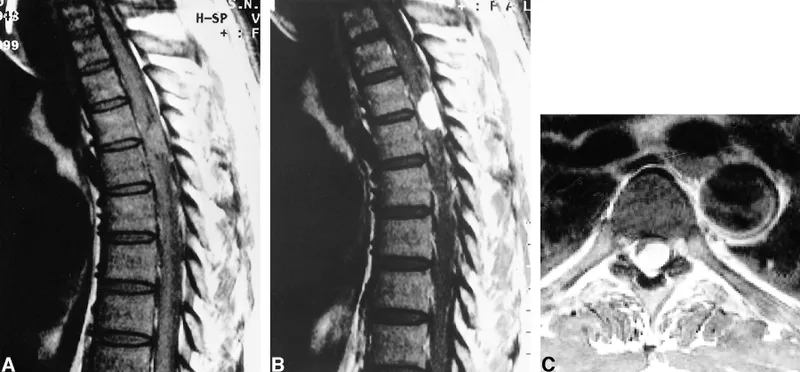
NICE NG59 Imaging Guidance:
- DO NOT routinely offer imaging for NSLBP without red flags
- Avoid XR in <55 years without trauma/red flags (low yield, radiation exposure)
- MRI spine is investigation of choice for suspected serious pathology
- 📊 85% of acute NSLBP improves within 6 weeks without imaging
Timeframes:
- Acute: <6 weeks | Subacute: 6-12 weeks | Chronic: >12 weeks
- Refer to spinal surgery if CES suspected (same-day emergency)
- Refer to specialist if red flags present or symptoms persist >12 weeks despite conservative management
Problem-Solving Approach
Systematic Red Flag Assessment (Every Patient):
-
Screen for CES (medical emergency):
- Ask specifically: "Any numbness between legs/around back passage?"
- "Any difficulty passing urine or loss of control?"
- Perform PR exam if any suspicion (reduced anal tone = CES until proven otherwise)
-
Age & Trauma Screen:
- Age >50 + new-onset back pain = consider malignancy/fracture
- Significant trauma at any age = XR spine
- Minor trauma + age >50/osteoporosis = XR spine
-
Infection Risk:
- Fever + back pain = discitis/osteomyelitis until proven otherwise
- Check: IV drug use, immunosuppression, recent procedures
- Bloods: CRP, ESR, WCC, blood cultures
-
Malignancy Screen:
- Red flags: unexplained weight loss, night pain, thoracic pain, progressive neurological deficit
- Past cancer history (especially breast, prostate, lung, kidney, thyroid)
- Age >50 with first episode or changed pain character
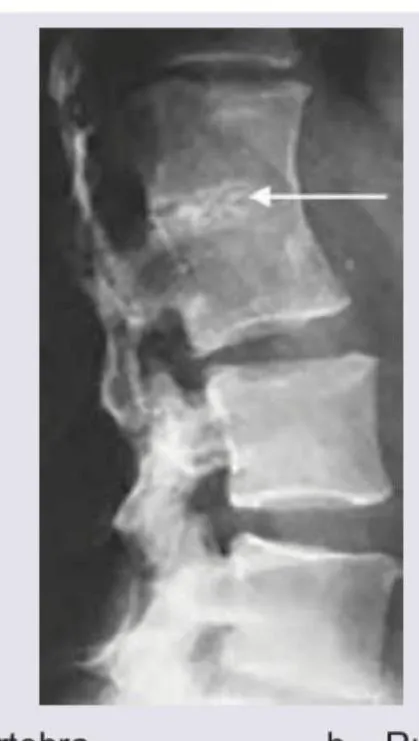
When to Refer Urgently:
- 🚩 Same-day emergency: Suspected CES (bilateral symptoms, saddle anaesthesia, sphincter dysfunction)
- 🚩 Urgent (<2 weeks): Red flags for malignancy/infection/progressive neurology
- 🚩 Routine specialist: Persistent symptoms >12 weeks, diagnostic uncertainty, failed conservative management
Analysis Framework
Differentiating Serious vs Non-Specific Low Back Pain:
| Feature | Non-Specific LBP | Serious Pathology |
|---|---|---|
| Onset | Mechanical, related to activity | Insidious or post-minor trauma |
| Age | Any (typically 20-55) | >50 years or <20 years |
| Pain pattern | Improves with rest, varies with position | Constant, night pain, thoracic |
| Systemic features | None | Fever, weight loss, malaise |
| Neurology | None or unilateral radiculopathy | Bilateral, progressive, sphincter involvement |
| Response | Improves over days-weeks | Progressive worsening |
📌 Remember: TUNA FISH for CES red flags - Tail (saddle anaesthesia), Urinary retention, Numbness bilateral, Anal tone reduced, Fecal incontinence, Impotence, Sciatica bilateral, Hip flexion weakness
Visual Aid
Key Points Summary
✓ CES is a surgical emergency: bilateral sciatica + saddle anaesthesia + sphincter dysfunction = MRI <24h and same-day neurosurgical referral
✓ Four red flag categories: CES (emergency), infection (fever/IVDU/immunosuppression), malignancy (age >50/weight loss/night pain), fracture (trauma/steroids/osteoporosis)
✓ NICE NG59: DO NOT routinely image NSLBP without red flags; 85% resolve within 6 weeks with conservative management
✓ MRI is gold standard for suspected serious pathology; avoid XR in <55 years without trauma (low yield, unnecessary radiation)
✓ Urgent referral (<2 weeks) for red flags; routine referral if symptoms persist >12 weeks despite conservative treatment
✓ Always perform PR exam if any suspicion of CES (reduced anal tone confirms diagnosis)
✓ Common pitfall: Missing bilateral symptoms in CES-always ask specifically about saddle numbness and sphincter function, don't wait for complete syndrome
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

