Quick Overview
Mental capacity assessment is a legal and ethical cornerstone of UK medical practice, governed by the Mental Capacity Act 2005 (MCA). Capacity is decision-specific and time-specific-assume capacity unless proven otherwise. NICE NG108 emphasizes that all practicable steps must be taken to support decision-making before concluding someone lacks capacity.
Core Facts & Concepts
Mental Capacity Act 2005 - Five Statutory Principles:
- Presumption of capacity until established otherwise
- Support all practicable steps to aid decision-making
- Unwise decisions do not prove incapacity
- Best interests guide actions for those lacking capacity
- Least restrictive option must be chosen
Two-Stage Capacity Test:
| Stage | Assessment Criteria |
|---|---|
| 1. Diagnostic threshold | Is there impairment/disturbance of mind/brain function? (temporary/permanent) |
| 2. Functional test | Can the person: Understand, Retain, Use/weigh, Communicate the decision? |
📌 Remember: URUC - Understand, Retain, Use/weigh, Communicate

Consent Requirements by Scenario:
- Valid consent needs: Capacity + Voluntary + Informed
- Emergency treatment: Proceed in best interests if capacity cannot be assessed (life/limb-threatening)
- Advance decisions: Legally binding if valid and applicable; must be written and witnessed for life-sustaining treatment refusal
- Lasting Power of Attorney (LPA): Health & Welfare LPA can consent/refuse treatment (only active when patient lacks capacity)
- Court of Protection: Resolves disputes; appoints deputies for ongoing decisions
Age-Specific Thresholds:
- ≥16 years: Presumed capacity (can consent; refusal may be overridden if life-threatening)
- <16 years: Gillick competence if sufficient maturity (Fraser guidelines for contraception)
- Parental responsibility: Overrides child refusal if in best interests until age 18
Problem-Solving Approach
Capacity Assessment Protocol (NICE NG108):
- Optimize conditions: Quiet environment, appropriate timing, communication aids, involve family/advocates
- Apply diagnostic threshold: Document impairment (delirium, dementia, learning disability, mental illness, intoxication)
- Conduct functional test (URUC):
- Understand: Explain in simple terms; ask patient to repeat back
- Retain: Even brief retention sufficient (minutes acceptable)
- Use/weigh: Can they appreciate consequences? Compare options?
- Communicate: Any method counts (speech, writing, blinking, Makaton)
- Document thoroughly: Record what information given, how assessed, reasons for conclusion, who consulted
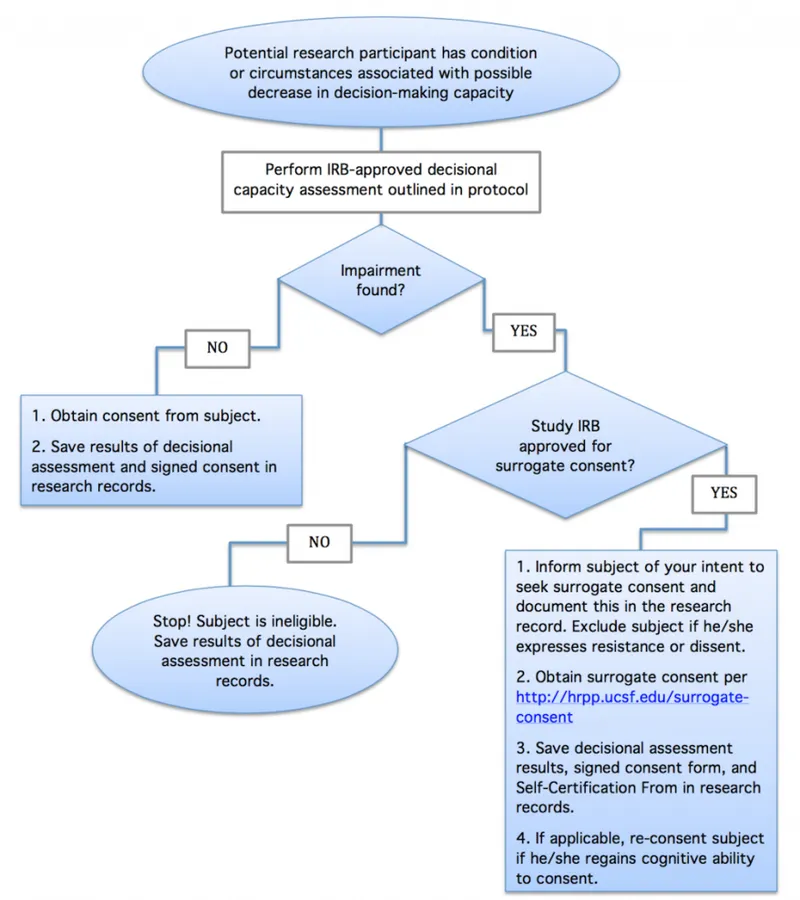
Best Interests Checklist (if capacity lacking):
- Consult: Family, carers, LPA, IMCA (Independent Mental Capacity Advocate if no one available)
- Consider: Past/present wishes, beliefs, values, other relevant factors
- Encourage participation: Support patient involvement maximally
- Life-sustaining treatment: Do not assume withholding is in best interests
⚠️ Warning: Deprivation of Liberty Safeguards (DoLS) required if restricting freedom in hospital/care home-apply via supervisory body
Analysis Framework
Capacity vs Consent Scenarios:
| Scenario | Capacity Status | Action Required |
|---|---|---|
| Fluctuating capacity (delirium) | Assess when optimal; defer if possible | Treat urgently in best interests; reassess when improved |
| Refuses life-saving treatment | Has capacity | Respect refusal; explore reasons; document clearly |
| Refuses life-saving treatment | Lacks capacity | Treat in best interests; consider advance decisions/LPA |
| Advance decision exists | Currently lacks capacity | Follow if valid and applicable to current situation |
| Disagreement with family | Lacks capacity | Family views inform but don't determine best interests |
Red Flags Suggesting Incapacity:
- 🚩 Cannot retain information even momentarily
- 🚩 Repeats same questions without incorporating answers
- 🚩 Cannot describe consequences of choices
- 🚩 Decision based on delusional beliefs directly
⭐ Clinical Pearl: Capacity can fluctuate-reassess if clinical state changes. A patient may have capacity for simple decisions (what to eat) but not complex ones (surgery consent).
Visual Aid
Capacity Assessment Documentation Template:
| Element | Record |
|---|---|
| Decision | Specific treatment/intervention |
| Impairment | Diagnosis affecting capacity |
| URUC assessment | Evidence for each component |
| Conclusion | Capacity present/absent with rationale |
| Best interests | If lacking capacity: who consulted, factors considered |
Key Points Summary
✓ Presume capacity for every decision unless impairment proven; capacity is decision-specific and time-specific
✓ Two-stage test: (1) Diagnostic threshold-impairment present? (2) Functional test-URUC (Understand, Retain, Use/weigh, Communicate)
✓ Valid consent requires: Capacity + Voluntary + Informed; unwise decisions ≠ incapacity
✓ Best interests: Consult widely (family, LPA, IMCA); consider patient's wishes, beliefs, values; choose least restrictive option
✓ Advance decisions: Legally binding if valid/applicable; must be written and witnessed for life-sustaining treatment refusal
✓ Age thresholds: ≥16 presumed capacity; <16 Gillick competence possible; parental responsibility until 18
✓ Emergency treatment: Proceed in best interests if capacity assessment impossible and treatment urgent-document retrospectively
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

