Quick Overview
Pulmonary embolism (PE) is a life-threatening condition requiring rapid diagnosis and treatment. NICE NG158 provides a structured approach using clinical probability assessment (Wells score), D-dimer testing, and imaging to confirm diagnosis, with immediate anticoagulation for most suspected cases. Risk stratification guides safe outpatient management versus admission.
Core Facts & Concepts
Two-Level PE Wells Score
- PE likely (>4 points): Proceed directly to CTPA
- PE unlikely (≤4 points): D-dimer first; if positive → CTPA
| Clinical Feature | Points |
|---|---|
| Clinical signs of DVT | 3 |
| PE most likely diagnosis | 3 |
| Heart rate >100 bpm | 1.5 |
| Immobilisation/surgery (past 4 weeks) | 1.5 |
| Previous PE/DVT | 1.5 |
| Haemoptysis | 1 |
| Malignancy (active/within 6 months) | 1 |
D-dimer Limitations
- High sensitivity (>95%), low specificity (~50%)
- False positives: pregnancy, malignancy, infection, post-op, elderly, hospitalised patients
- Age-adjusted threshold: age × 10 μg/L (for age >50 years)
- 🚩 Never use in "PE likely" patients - delays diagnosis
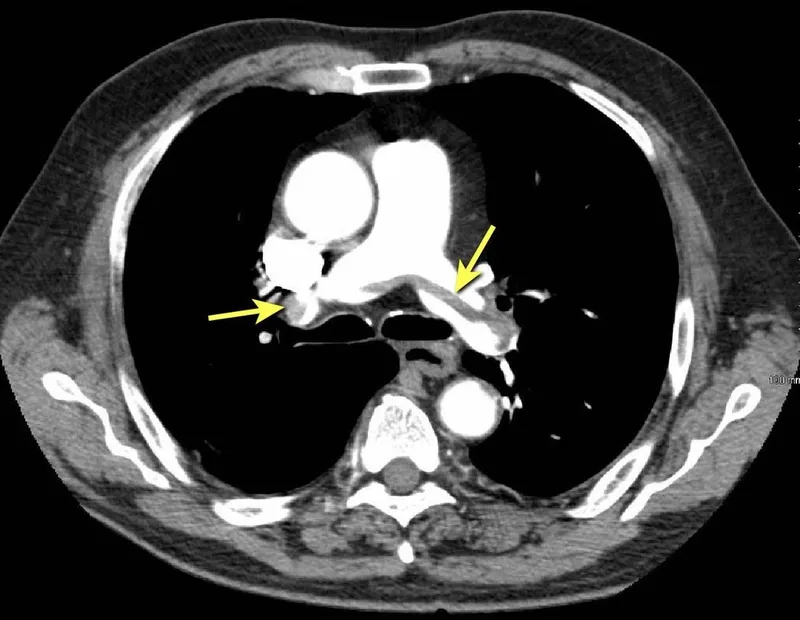
Imaging Selection (NICE NG158)
- First-line: CTPA - sensitivity 83%, specificity 96%
- V/Q scan if: contrast allergy, renal impairment (eGFR <30), pregnancy with normal CXR
- V/Q reported as: normal, low/intermediate/high probability
Immediate Anticoagulation
- Start before imaging if Wells >4 AND delay >1 hour expected
- Options: DOAC (apixaban/rivaroxaban), LMWH, or fondaparinux
- 📊 Contraindications: active bleeding, platelets <50×10⁹/L, recent neurosurgery
Problem-Solving Approach
Step-by-Step Diagnostic Pathway
- Calculate two-level Wells score immediately
- Wells ≤4 (PE unlikely):
- Measure D-dimer (age-adjusted if >50 years)
- Negative D-dimer → PE excluded, no imaging
- Positive D-dimer → CTPA (or V/Q if contraindicated)
- Wells >4 (PE likely):
- Start anticoagulation if imaging delay >1 hour
- Arrange immediate CTPA (or V/Q)
- PE confirmed → Risk stratify using sPESI
🚩 Red Flags for Massive PE
- Systolic BP <90 mmHg or drop >40 mmHg
- Syncope, altered consciousness
- Severe hypoxia (SpO₂ <90%)
- Cardiac arrest
- → Consider thrombolysis (alteplase 50 mg IV over 1-2 hours)
Analysis Framework
Risk Stratification: Simplified PESI (sPESI)
| Parameter | Points if Present |
|---|---|
| Age >80 years | 1 |
| Cancer | 1 |
| Chronic cardiopulmonary disease | 1 |
| Heart rate ≥110 bpm | 1 |
| Systolic BP <100 mmHg | 1 |
| SpO₂ <90% | 1 |
- sPESI = 0: Low risk → outpatient management safe (mortality <1%)
- sPESI ≥1: Higher risk → consider admission, troponin/BNP, echo
Outpatient Management Criteria (All Must Apply)
- sPESI = 0
- No active bleeding/high bleeding risk
- Adequate social support
- Normal renal/hepatic function (for DOACs)
- Follow-up within 24 hours arranged
Visual Aid
CTPA vs V/Q Selection
| Factor | CTPA | V/Q Scan |
|---|---|---|
| First-line | ✓ | |
| Renal impairment (eGFR <30) | ✓ | |
| Contrast allergy | ✓ | |
| Pregnancy with normal CXR | ✓ | |
| Availability | Widely available | Limited centres |
Key Points Summary
✓ Two-level Wells >4 = PE likely → skip D-dimer, go straight to CTPA; start anticoagulation if imaging delayed >1 hour
✓ Age-adjusted D-dimer (age × 10 μg/L for >50 years) reduces false positives in elderly; never use in "PE likely" patients
✓ CTPA is first-line imaging; V/Q scan reserved for renal impairment, contrast allergy, or pregnancy with normal CXR
✓ sPESI = 0 permits safe outpatient management (mortality <1%); sPESI ≥1 requires admission and further risk assessment
✓ DOACs (apixaban/rivaroxaban) are first-line anticoagulation; no bridging with LMWH needed unlike warfarin
✓ Massive PE (hypotension/arrest) → consider thrombolysis with alteplase 50 mg IV; contraindications include recent surgery/stroke
✓ Common pitfall: Delaying anticoagulation in high-probability PE waiting for imaging - start treatment first if Wells >4 and delay expected
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

