Quick Overview
Acute Kidney Injury (AKI) is a sudden decline in renal function occurring within hours-days, affecting 15-20% of hospital admissions. NICE NG148 emphasizes early detection via creatinine rise or reduced urine output, with prompt categorization into pre-renal (60-70%), intrinsic (25-40%), or post-renal (5-10%) causes to guide management and prevent progression to chronic kidney disease.
Core Facts & Concepts
KDIGO Staging Criteria (defines AKI severity):
| Stage | Creatinine Rise | Urine Output |
|---|---|---|
| 1 | ≥26.5 μmol/L in 48h OR 1.5-1.9× baseline | <0.5 mL/kg/h for 6-12h |
| 2 | 2.0-2.9× baseline | <0.5 mL/kg/h for ≥12h |
| 3 | ≥3× baseline OR ≥354 μmol/L OR RRT initiated | <0.3 mL/kg/h for ≥24h OR anuria ≥12h |
Classification by Cause:
- Pre-renal (70%): Hypoperfusion → hypovolemia, sepsis, cardiac failure, renal artery stenosis
- Urine Na⁺ <20 mmol/L, FENa <1%, urine osmolality >500 mOsm/kg
- Intrinsic (25%): Tubular (ATN), glomerular, interstitial, vascular damage
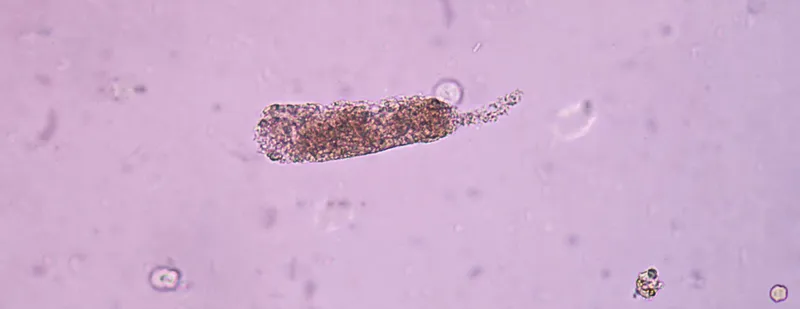
- Urine Na⁺ >40 mmol/L, FENa >2%, muddy brown casts (ATN)
- Post-renal (5%): Obstruction → stones, BPH, malignancy, retroperitoneal fibrosis
- Bilateral obstruction OR unilateral with solitary kidney required

📊 Critical Numbers:
- Baseline creatinine: use lowest value in past 3-12 months
- Nephrotoxins to stop: NSAIDs, ACE-i/ARBs, aminoglycosides, diuretics (if hypovolemic)
- Target MAP >65-70 mmHg for renal perfusion
Problem-Solving Approach
NICE NG148 Diagnostic Algorithm:
- Confirm AKI: Check creatinine rise/urine output against KDIGO criteria
- Assess volume status: JVP, mucous membranes, skin turgor, postural BP, fluid balance charts
- Urinalysis: Dipstick (blood/protein suggests glomerular), microscopy (casts, cells)
- Identify cause:
- Pre-renal: Trial fluid challenge (250-500 mL crystalloid over 15 min); response suggests pre-renal
- Intrinsic: Check eosinophils (AIN), CK (rhabdomyolysis), immunology (vasculitis)
- Post-renal: Urgent USS within 24h if cause unclear or anuria
- Stop nephrotoxins immediately (NICE NG148 recommendation)
- Monitor: Daily U&Es, fluid balance, weight, urine output (catheterize if Stage 3)
🚩 Red Flags for Urgent Nephrology Referral:
- Stage 3 AKI or rapidly rising creatinine
- K⁺ >6.5 mmol/L despite treatment
- Pulmonary edema unresponsive to diuretics
- Suspected glomerulonephritis/vasculitis (hematuria + proteinuria)
- pH <7.2 (metabolic acidosis)
Analysis Framework
Differentiating AKI Causes:
| Feature | Pre-renal | Intrinsic (ATN) | Post-renal |
|---|---|---|---|
| Urine Na⁺ | <20 mmol/L | >40 mmol/L | Variable |
| FENa | <1% | >2% | Variable |
| Urine osmolality | >500 mOsm/kg | <350 mOsm/kg | Variable |
| Urine sediment | Bland/hyaline casts | Muddy brown/epithelial casts | Normal |
| Response to fluids | Improves | No improvement | No improvement |
| USS findings | Normal | Normal/echogenic | Hydronephrosis (if bilateral) |
📌 Remember: RIFLE - Risk, Injury, Failure, Loss, ESKD (older AKI classification, now superseded by KDIGO)
Visual Aid
Key Points Summary
✓ KDIGO Stage 1: Creatinine ≥26.5 μmol/L rise in 48h OR 1.5× baseline; Stage 3 requires RRT consideration
✓ Pre-renal (70%): Low urine Na⁺ (<20), FENa <1%, responds to fluid challenge within 2-4h
✓ Stop nephrotoxins immediately: NSAIDs, ACE-i/ARBs, gentamicin, metformin (NICE NG148)
✓ Urgent USS within 24h if cause unclear, anuria, or suspected obstruction
✓ Refer nephrology urgently for Stage 3, K⁺ >6.5 mmol/L, pH <7.2, suspected GN/vasculitis
✓ Muddy brown casts = ATN (intrinsic); hydronephrosis = post-renal obstruction
✓ Monitor daily: U&Es, fluid balance, weight; catheterize for accurate output in Stage 3
⚠️ Warning: Diuretics worsen pre-renal AKI-assess volume status first before administering
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

