Quick Overview
Diabetes complications are leading causes of preventable blindness, renal failure, and amputation in the UK. NICE NG28 mandates structured annual screening for microvascular (retinopathy, nephropathy, neuropathy) and macrovascular complications, with specific referral thresholds and foot risk stratification. Early detection through systematic surveillance reduces morbidity by 30-50%.
Core Facts & Concepts
Annual Screening Requirements (NICE NG28):
- Retinopathy: Digital retinal photography annually from diagnosis (Type 2) or 5 years post-diagnosis (Type 1)
- Nephropathy: Urinary ACR (albumin:creatinine ratio) + eGFR annually
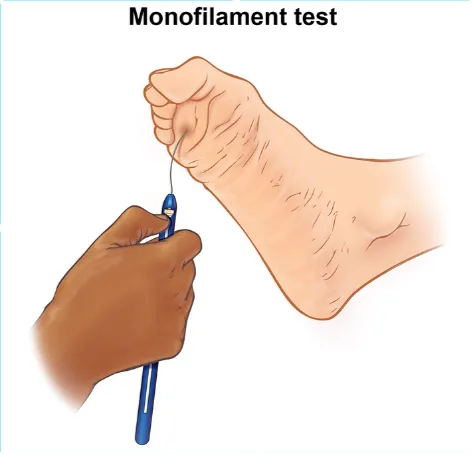
- Neuropathy: 10g monofilament testing + vibration sense annually
- Foot examination: Visual inspection + risk stratification annually
Key Thresholds:
| Parameter | Normal | Microalbuminuria | Macroalbuminuria |
|---|---|---|---|
| ACR (mg/mmol) | <3 | 3-30 | >30 |
| Action | Annual review | Confirm x2, start ACEi/ARB | Nephrology referral if declining eGFR |
CKD Staging in Diabetes:
- Stage 1-2 (eGFR ≥60): Monitor annually if ACR <30
- Stage 3a (eGFR 45-59): 6-monthly review
- Stage 3b-5 (eGFR <45): Nephrology referral
Diabetic Foot Risk Stratification:
- Low risk (normal sensation, palpable pulses): Annual review
- Moderate risk (neuropathy OR absent pulses): 3-6 monthly podiatry
- High risk (neuropathy + absent pulses/deformity/previous ulcer): 1-3 monthly multidisciplinary team
- Active ulcer/Charcot: Urgent specialist referral (≤24 hours)
Problem-Solving Approach
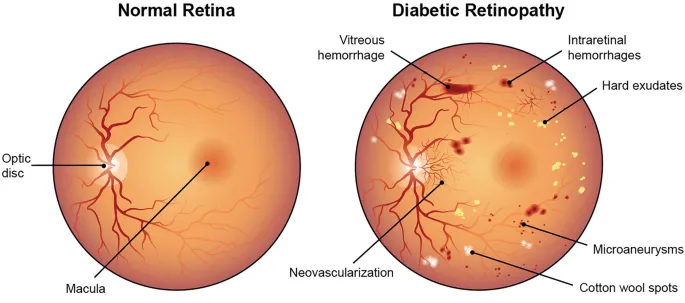
Retinopathy Referral Pathway:
- Background retinopathy (microaneurysms, hard exudates): Continue annual screening
- Pre-proliferative (cotton wool spots, venous beading): Ophthalmology referral within 4 weeks
- Proliferative (new vessels): Urgent referral within 1 week
- Maculopathy (exudates within 1 disc diameter of fovea): Referral within 6 weeks
Nephropathy Management Steps:
- Confirm elevated ACR with 2 out of 3 samples over 3 months
- Optimize BP target: <130/80 mmHg (or <120/80 if ACR >70)
- Start ACEi or ARB regardless of BP if ACR >3
- Check U&Es 1-2 weeks after starting (expect creatinine rise <25%, K+ <5.5)
- Refer nephrology if eGFR <45, ACR >70, or declining eGFR >5 ml/min/year
🚩 Red Flags: Rapidly declining eGFR (>5 ml/min/year), non-visible haematuria with ACR >30, resistant hypertension - consider alternative renal pathology
Analysis Framework
Neuropathy Classification:
| Type | Features | Management |
|---|---|---|
| Peripheral sensory | Glove-stocking loss, reduced monofilament | Foot protection education, annual screening |
| Painful neuropathy | Burning/shooting pain, worse at night | Duloxetine 60mg OD or pregabalin 150-300mg BD |
| Autonomic | Postural hypotension, gastroparesis, erectile dysfunction | Treat symptoms, exclude other causes |
| Mononeuropathy | CN III palsy (pupil-sparing), carpal tunnel | Usually self-limiting over 6-12 weeks |
Foot Ulcer Assessment (SINBAD Score):
- Site (forefoot/midfoot/hindfoot), Ischaemia (pedal pulses), Neuropathy, Bacterial infection, Area, Depth
- Score ≥3: High amputation risk - urgent MDT referral
Visual Aid
Key Points Summary
✓ Annual screening triad: Digital retinal photography, ACR + eGFR, 10g monofilament testing (NICE NG28)
✓ ACR thresholds: 3-30 mg/mmol = microalbuminuria (start ACEi/ARB), >30 = macroalbuminuria (nephrology if eGFR <45)
✓ Retinopathy referral: Pre-proliferative (4 weeks), proliferative (1 week), maculopathy (6 weeks)
✓ BP target in nephropathy: <130/80 mmHg, or <120/80 if ACR >70 mg/mmol
✓ Foot risk: High risk = neuropathy + absent pulses/deformity - 1-3 monthly MDT review
✓ Active ulcer: Urgent referral ≤24 hours; assess ischaemia (ABPI <0.9 = vascular referral)
✓ Painful neuropathy: First-line duloxetine 60mg OD or pregabalin 150-300mg BD
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

