Quick Overview
Stable angina is predictable chest discomfort due to reversible myocardial ischaemia during exertion/stress. NICE CG126 emphasises clinical assessment, CT coronary angiography (CTCA) as first-line imaging, and structured anti-anginal therapy. Key goals: symptom control, cardiovascular risk reduction, and appropriate revascularisation when indicated.
Core Facts & Concepts
📊 Diagnostic Pathway (NICE CG126)
- Clinical assessment: Typical angina requires 3 features-constricting chest discomfort, provoked by exertion, relieved by rest/GTN within 5 minutes
- Atypical angina = 2 features; Non-anginal = ≤1 feature
- First-line investigation: CT coronary angiography (CTCA) for all with typical/atypical angina (unless revascularisation already planned)
- Invasive coronary angiography if CTCA shows severe disease (≥70% stenosis) or equivocal results

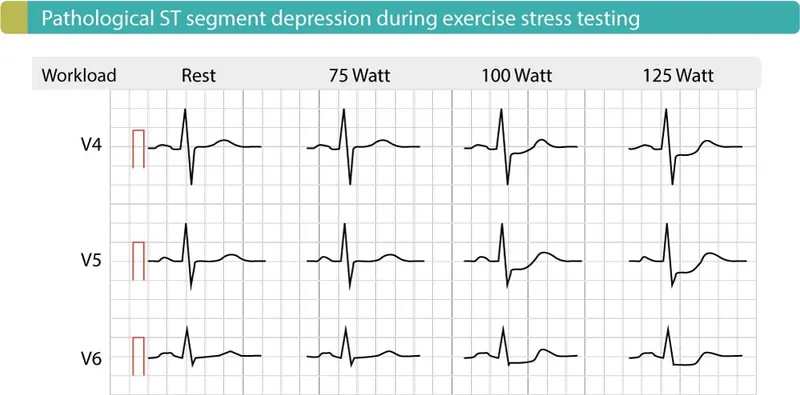
- Functional testing: Exercise ECG no longer recommended as first-line (low sensitivity/specificity)
- Cardiovascular risk management: All patients require statin (atorvastatin 80mg), aspirin 75mg, BP control (<140/90mmHg)
💊 Anti-Anginal Medication Ladder
| Line | Options | Key Points |
|---|---|---|
| 1st-line | β-blocker OR rate-limiting CCB | Avoid combination of both (risk of bradycardia/heart block) |
| 2nd-line | Add long-acting nitrate, ivabradine, nicorandil, or ranolazine | If β-blocker + CCB needed, use dihydropyridine CCB (amlodipine) |
| Rescue | Sublingual GTN spray | Use prophylactically before exertion |
- 🚩 β-blocker contraindications: Asthma, severe peripheral vascular disease, heart block
- CCB choice: Verapamil/diltiazem (rate-limiting) vs amlodipine (non-rate-limiting)
Problem-Solving Approach
Step-by-Step Management
- Confirm diagnosis: Clinical assessment → CTCA (identifies anatomy + severity)
- Risk stratification: Consider invasive angiography if CTCA shows ≥70% stenosis in proximal vessels or left main stem disease
- Initiate dual therapy: Anti-anginal (symptom control) + antiplatelet/statin (event prevention)
- Optimise anti-anginals: Titrate to maximum tolerated dose before adding second agent
- Revascularisation indications:
- Persistent symptoms despite optimal medical therapy (OMT)
- High-risk anatomy (left main stem, proximal LAD, 3-vessel disease)
- Evidence of large ischaemic burden on functional imaging
🚩 Red Flags for Acute Coronary Syndrome
- Pain at rest, crescendo pattern, or lasting >15 minutes
- New-onset severe angina (<24 hours)
- Immediate 12-lead ECG and troponin required
Post-Revascularisation Antiplatelet Therapy
- PCI (stents): Dual antiplatelet therapy (DAPT) = aspirin 75mg + ticagrelor 90mg BD (or clopidogrel 75mg) for 12 months
- CABG: Aspirin 75mg lifelong (no routine DAPT unless specific indication)
⭐ Clinical Pearl: Always check renal function before CTCA (contrast nephropathy risk if eGFR <30ml/min)
Analysis Framework
Differentiating Chest Pain Types
| Feature | Stable Angina | ACS | Pericarditis | Musculoskeletal |
|---|---|---|---|---|
| Onset | Exertional, predictable | Sudden, at rest | Gradual | After movement/injury |
| Duration | 2-10 minutes | >15 minutes | Hours-days | Variable |
| Relief | Rest/GTN <5 min | Not relieved by GTN | Sitting forward | Positional change |
| Character | Constricting, heavy | Crushing, severe | Sharp, pleuritic | Sharp, localised |
| ECG | Normal/ST depression on exertion | ST changes/T-wave inversion | Widespread ST elevation (saddle-shaped) | Normal |
Key Discriminators
- Troponin: Normal in stable angina (elevated in ACS)
- Timing: Stable angina = predictable exertional trigger; ACS = unpredictable/rest symptoms
Visual Aid
Anti-Anginal Optimisation Table
| Drug Class | Mechanism | Dose Titration | Key Side Effects |
|---|---|---|---|
| β-blockers | ↓ HR, ↓ contractility | Bisoprolol 2.5→10mg OD | Fatigue, bradycardia |
| CCB (rate-limiting) | ↓ HR, vasodilation | Diltiazem 60→120mg BD | Constipation, ankle oedema |
| Long-acting nitrates | Venodilation, ↓ preload | Isosorbide mononitrate 30→120mg OD | Headache, tolerance (nitrate-free period needed) |
| Nicorandil | K⁺ channel opener | 10→30mg BD | Oral/anal ulceration |
Key Points Summary
✓ CTCA is first-line imaging for suspected stable angina (NICE CG126)-identifies anatomy and guides revascularisation decisions
✓ Typical angina = 3 features: constricting discomfort, exertional provocation, relief with rest/GTN <5 minutes
✓ Anti-anginal ladder: Start β-blocker OR rate-limiting CCB (never combine both initially); add second agent if symptoms persist despite optimal dosing
✓ All patients need dual therapy: Anti-anginal for symptoms + aspirin 75mg + atorvastatin 80mg for event prevention
✓ Post-PCI DAPT: Aspirin + ticagrelor (or clopidogrel) for 12 months; post-CABG aspirin monotherapy lifelong
✓ Revascularisation indications: Symptoms despite optimal medical therapy, or high-risk anatomy (left main stem, proximal LAD, 3-vessel disease)
✓ 🚩 Red flag for ACS: Chest pain at rest, crescendo pattern, or >15 minutes duration-requires immediate ECG and troponin
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

