Quick Overview
Heart failure (HF) affects >900,000 UK adults with 5-year mortality ~50%. HFrEF (reduced ejection fraction, LVEF ≤40%) and HFpEF (preserved ejection fraction, LVEF ≥50%) require distinct management strategies. NICE NG106 emphasizes BNP-guided diagnosis and quadruple therapy for HFrEF.
Core Facts & Concepts
Diagnostic Criteria
- BNP thresholds (NICE NG106):
- BNP >400 pg/mL or NT-proBNP >2000 pg/mL → urgent echo within 2 weeks
- BNP 100-400 pg/mL or NT-proBNP 400-2000 pg/mL → routine echo within 6 weeks
- Previous MI → refer regardless of BNP
- Classification by LVEF:
- HFrEF: LVEF ≤40%
- HFmrEF (mildly reduced): LVEF 41-49%
- HFpEF: LVEF ≥50%
HFrEF Pharmacological Pillars (NICE NG106 quadruple therapy):
| Drug Class | First-line Agents | Target Dose | Key Benefit |
|---|---|---|---|
| ARNI/ACEi | Sacubitril-valsartan 97/103mg BD OR Ramipril 10mg OD | Mortality ↓25-30% | Start ACEi, switch to ARNI if stable |
| Beta-blocker | Bisoprolol 10mg OD, Carvedilol 25mg BD | Mortality ↓35% | Start low, titrate slowly |
| MRA | Spironolactone 25-50mg OD, Eplerenone 50mg OD | Mortality ↓30% | Monitor K⁺ and creatinine |
| SGLT2i | Dapagliflozin 10mg OD, Empagliflozin 10mg OD | Mortality ↓13%, HF admission ↓30% | Even if non-diabetic |
⭐ Clinical Pearl: Start all 4 pillars within 4-6 weeks; don't wait for sequential titration to max doses.
Diuretic Management
- Loop diuretics (furosemide 40-240mg OD) for symptom relief only-no mortality benefit
- Adjust dose based on daily weights and fluid status
- IV if oral absorption poor (bowel oedema)
Problem-Solving Approach
Step-by-Step HF Diagnosis
- Clinical suspicion: Breathlessness, orthopnoea, ankle oedema, fatigue
- Order BNP/NT-proBNP: Elevated in >95% of HF cases
- Transthoracic echo: Assess LVEF, valves, wall motion
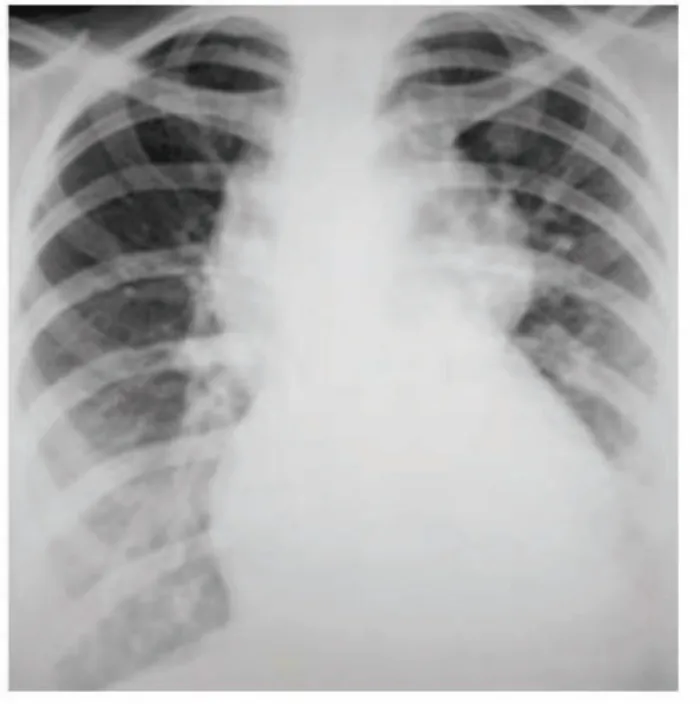
- ECG + CXR: Identify arrhythmias, cardiomegaly, pulmonary oedema
- Bloods: FBC, U&E, TFTs, HbA1c, lipids (exclude reversible causes)
HFrEF Medication Initiation Algorithm
- Start ACEi + beta-blocker simultaneously at low doses
- Add MRA if NYHA II-IV persists (K⁺ <5.0 mmol/L, eGFR >30)
- Switch ACEi to ARNI after 4 weeks if symptomatic
- Add SGLT2i immediately (regardless of diabetes status)
- Titrate each drug to target/max tolerated dose every 2-4 weeks
🚩 Red Flags for Specialist Referral
- NYHA III-IV despite optimal medical therapy
- Symptomatic hypotension preventing up-titration
- Refractory fluid overload
- Consider device therapy: ICD if LVEF ≤35%, CRT if QRS ≥130ms
Analysis Framework
HFrEF vs HFpEF Key Differences
| Feature | HFrEF (LVEF ≤40%) | HFpEF (LVEF ≥50%) |
|---|---|---|
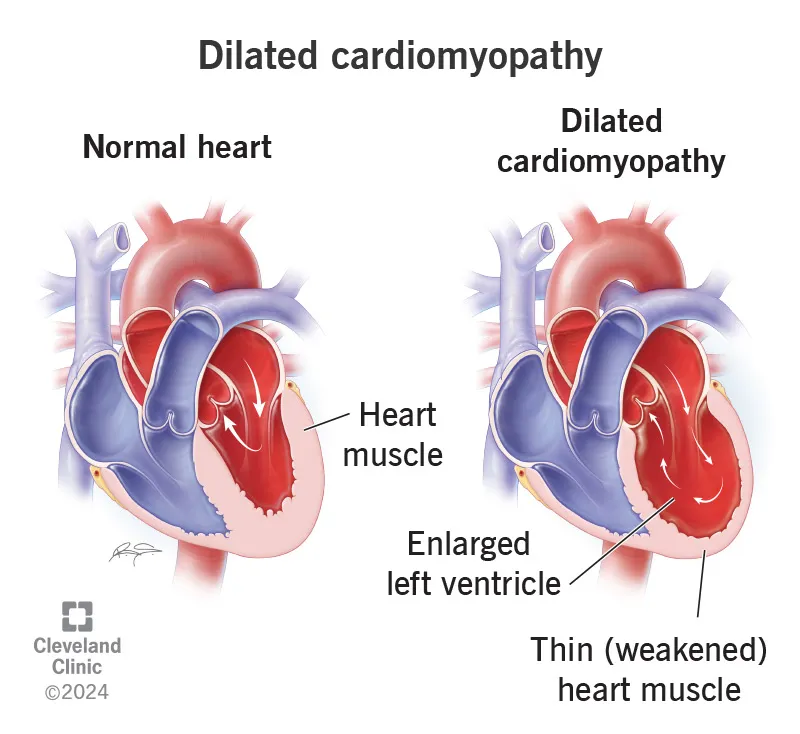
| Pathophysiology | Systolic dysfunction, dilated LV | Diastolic dysfunction, stiff LV |
| Evidence-based Rx | Quadruple therapy (ARNI, BB, MRA, SGLT2i) | SGLT2i (dapagliflozin), diuretics |
| Mortality benefit | 50-60% reduction with optimal therapy | Minimal proven therapies |
| Device therapy | ICD, CRT if indicated | Rarely indicated |
| Prognosis | Better with treatment | Poorer, limited options |
⚠️ Warning: HFpEF lacks robust evidence-focus on treating comorbidities (HTN, AF, obesity) and symptom control with diuretics.
Drug Monitoring Essentials
- ACEi/ARNI: Check U&E at 1-2 weeks; accept Cr rise <30%, K⁺ <5.5 mmol/L
- MRA: Stop if K⁺ >5.5 mmol/L or eGFR <30 mL/min
- SGLT2i: Monitor for genital infections, DKA (rare)
Visual Aid
NYHA Functional Classification
| Class | Symptoms | Activity Limitation |
|---|---|---|
| I | No symptoms | No limitation |
| II | Symptoms with moderate exertion | Slight limitation |
| III | Symptoms with minimal exertion | Marked limitation |
| IV | Symptoms at rest | Unable to carry out any activity |
Key Points Summary
✓ Diagnosis: BNP >400 pg/mL (or NT-proBNP >2000) + echo showing LVEF ≤40% confirms HFrEF
✓ HFrEF quadruple therapy: ARNI (or ACEi) + beta-blocker + MRA + SGLT2i-start all within 4-6 weeks for maximum mortality benefit (50-60% reduction)
✓ Diuretics: For symptom relief only; no mortality benefit. Titrate loop diuretics to euvolaemia
✓ HFpEF management: Limited evidence-SGLT2i (dapagliflozin 10mg OD) only proven therapy. Focus on BP control and treating comorbidities
✓ Device therapy: ICD if LVEF ≤35% post-MI or dilated cardiomyopathy; CRT if QRS ≥130ms with LBBB
✓ Monitoring: Accept Cr rise <30% and K⁺ <5.5 mmol/L when initiating RAAS inhibitors-don't stop prematurely
✓ Common pitfall: Sequential drug titration delays benefit-initiate all 4 pillars early, then up-titrate simultaneously
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more