Quick Overview
Skin and soft tissue infections (SSTIs) range from superficial impetigo to life-threatening necrotizing fasciitis. NICE NG190 provides evidence-based guidance for diagnosis, severity assessment, and antibiotic selection. Rapid recognition of severity (Eron classification) and necrotizing infection is critical for appropriate management and preventing complications.
Core Facts & Concepts
NICE NG190 Classification:
| Condition | Clinical Features | Depth |
|---|---|---|
| Impetigo | Golden crusted lesions, bullous or non-bullous | Epidermis only |
| Erysipelas | Well-demarcated, raised, bright red, painful | Superficial dermis + lymphatics |
| Cellulitis | Poorly demarcated, spreading erythema, warmth | Deep dermis + subcutaneous |
| Abscess | Fluctuant collection, pointing | Dermis/subcutaneous |
Eron Classification (Cellulitis Severity):
- Class I: No systemic toxicity, no comorbidities → oral antibiotics, outpatient
- Class II: Systemically unwell OR significant comorbidity → oral/IV antibiotics, consider admission
- Class III: Systemic toxicity (confusion, tachycardia, hypotension) OR limb-threatening → IV antibiotics, admission
- Class IV: Sepsis/life-threatening (necrotizing fasciitis) → urgent surgical review + IV antibiotics
Key Numbers:
- 📊 Bilateral leg cellulitis = consider alternative diagnosis (venous stasis, lipodermatosclerosis)
- 📊 LRINEC score ≥6 = 92% PPV for necrotizing fasciitis
- 📊 Impetigo contagious until 48h after starting antibiotics or lesions crusted
Problem-Solving Approach
Step 1: Classify the SSTI
- Assess depth and extent (superficial vs deep)
- Look for systemic features (fever, tachycardia, hypotension)
- Identify comorbidities (diabetes, immunosuppression, PVD)
Step 2: Assess Severity (Eron Classification)
- Measure vital signs, assess mental status
- Mark borders with pen + date/time for progression monitoring
Step 3: First-Line Antibiotic Selection (NICE NG190)
| Infection | First-Line | Duration |
|---|---|---|
| Impetigo (localized) | Topical fusidic acid | 5 days |
| Impetigo (widespread) | Oral flucloxacillin | 5-7 days |
| Cellulitis/Erysipelas | Oral flucloxacillin 500mg-1g QDS | 5-7 days |
| Severe cellulitis (Class III-IV) | IV flucloxacillin 1-2g QDS | Until improved, then oral |
- Penicillin allergy: Clarithromycin or doxycycline
- MRSA suspected: Add doxycycline or clindamycin
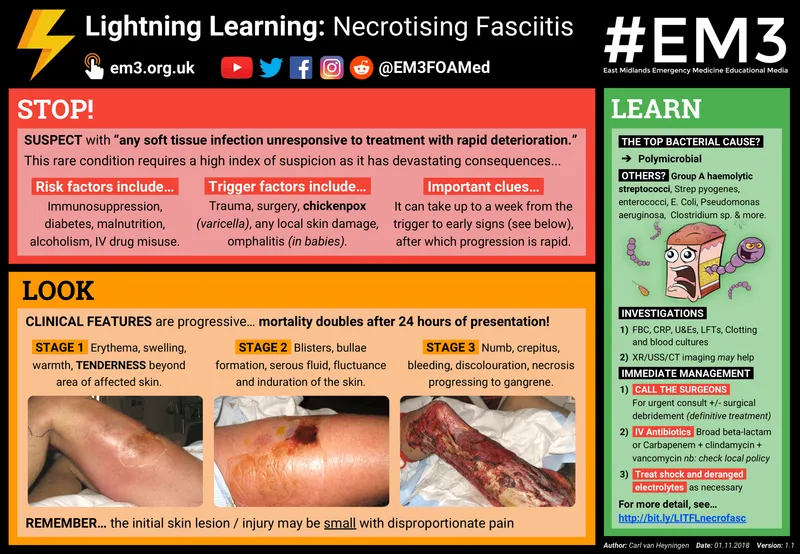
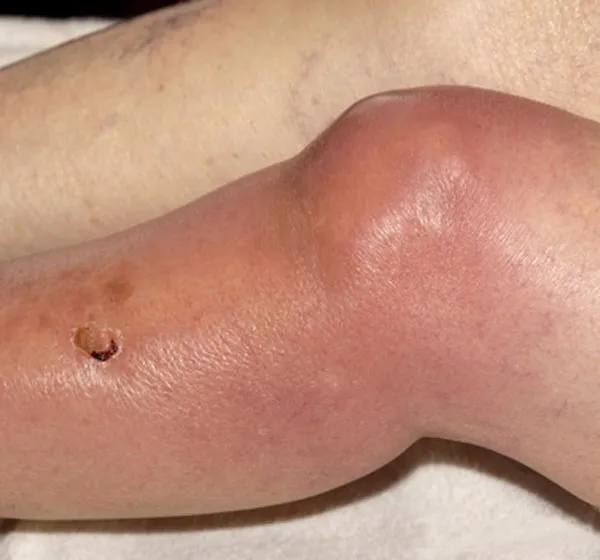
🚩 Red Flags for Necrotizing Fasciitis:
- Severe pain disproportionate to clinical signs
- Rapid progression (hours)
- Dusky/purple discoloration, bullae, crepitus
- Systemic toxicity (shock, organ failure)
- Hypoaesthesia (nerve involvement)
Step 4: When to Suspect MRSA
- Recent hospitalization/nursing home resident
- IV drug use
- Known MRSA colonization/previous infection
- Recurrent SSTIs despite appropriate antibiotics
Analysis Framework
Cellulitis vs DVT vs Venous Insufficiency:
| Feature | Cellulitis | DVT | Venous Insufficiency |
|---|---|---|---|
| Onset | Acute (days) | Acute/subacute | Chronic |
| Distribution | Unilateral | Unilateral | Often bilateral |
| Erythema | Present, spreading | Absent | Hemosiderin staining |
| Warmth | Marked | Mild | Absent |
| Fever | Common | Rare | Absent |
| D-dimer | Variable | Elevated | Normal |
LRINEC Score Components (for necrotizing fasciitis):
- CRP >150mg/L (4 points)
- WCC >25 (2 points), 15-25 (1 point)
- Haemoglobin <110g/L (2 points), 110-135 (1 point)
- Sodium <135mmol/L (2 points)
- Creatinine >141μmol/L (2 points)
- Glucose >10mmol/L (1 point)
⚠️ Warning: LRINEC score has limited sensitivity (68%) - clinical suspicion overrides negative score
Visual Aid
MRSA Coverage Indications:
| Scenario | Action |
|---|---|
| Healthcare-associated risk factors | Add doxycycline/clindamycin |
| Culture-confirmed MRSA | Switch to appropriate agent |
| Recurrent infections | Consider decolonization (nasal mupirocin + chlorhexidine washes) |
Key Points Summary
✓ Eron Classification determines management: Class I outpatient oral, Class III-IV admission + IV antibiotics
✓ First-line cellulitis: Flucloxacillin 500mg-1g QDS for 5-7 days; clarithromycin if penicillin-allergic
✓ Necrotizing fasciitis red flags: Pain >> signs, rapid progression, dusky skin, crepitus, systemic toxicity → emergency surgical debridement
✓ Bilateral leg cellulitis is rare - consider venous insufficiency, lipodermatosclerosis, or systemic causes
✓ MRSA coverage indicated for healthcare-associated risk, IV drug use, or recurrent infections despite treatment
✓ Mark cellulitis borders with pen + time to monitor progression objectively
✓ LRINEC score ≥6 suggests necrotizing infection but clinical suspicion overrides negative score (68% sensitivity)
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

