Quick Overview
GI perforation is a surgical emergency requiring immediate recognition and management. Mortality ranges from 10-40% depending on site, time to intervention, and patient factors. NICE NG158 emphasizes early imaging, broad-spectrum antibiotics within 1 hour, and urgent surgical review. Upper GI perforations (gastroduodenal) differ significantly in management from lower GI (colorectal) perforations.
Core Facts & Concepts
Clinical Presentation
- Sudden-onset severe abdominal pain (may be localized initially, then generalized)
- Peritonism: guarding, rigidity, rebound tenderness, absent bowel sounds
- Systemic features: tachycardia >100 bpm, hypotension, fever, sepsis
- Silent abdomen: rigid, board-like on palpation
Key Investigations
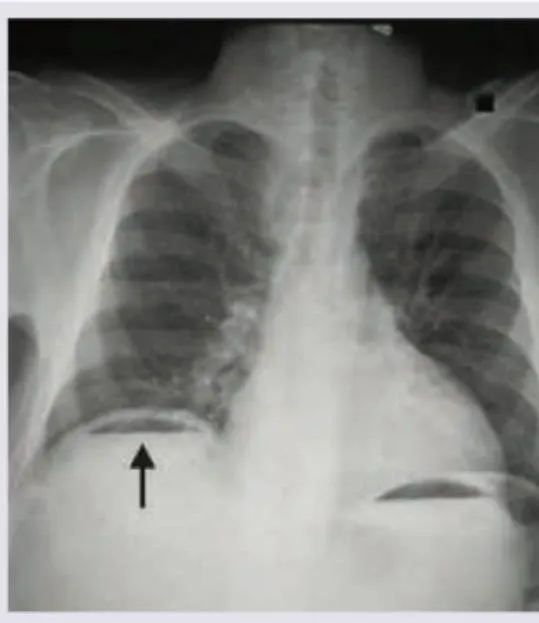
- Erect CXR: detects 70-80% of perforations (free gas under diaphragm)
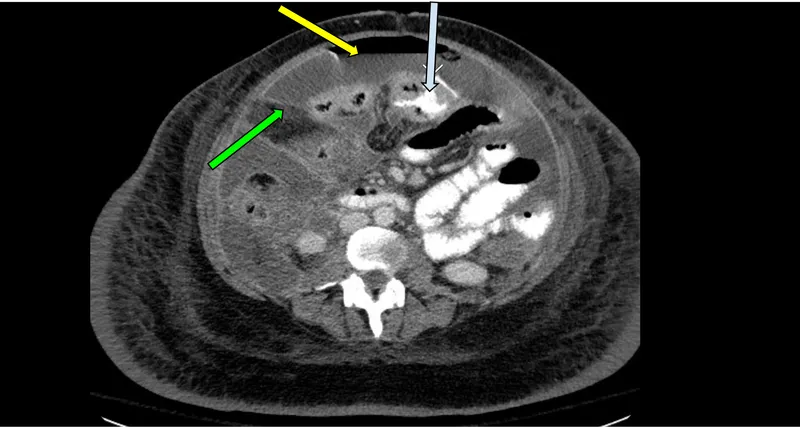
- CT abdomen/pelvis with contrast: >95% sensitivity, shows site and cause
- Lactate >2 mmol/L: marker of tissue hypoperfusion and sepsis severity
- Bloods: FBC, U&Es, CRP, clotting, G&S/crossmatch
Common Causes by Site
| Site | Common Causes | Key Features |
|---|---|---|
| Upper GI | Peptic ulcer (60%), malignancy, iatrogenic | Anterior perforations → pneumoperitoneum |
| Lower GI | Diverticulitis (40%), malignancy, IBD, ischaemia | Faecal peritonitis, higher mortality |
| Small bowel | Obstruction, Crohn's, trauma, foreign body | Rapid clinical deterioration |
Critical Numbers
- Golden period: Surgery within 6 hours reduces mortality by 50%
- Boey score (peptic ulcer perforation): predicts mortality based on shock, comorbidity, delayed presentation
Problem-Solving Approach
1. Immediate Recognition & Resuscitation (ABCDE)
- Airway/Breathing: High-flow O₂ to maintain SpO₂ >94%
- Circulation: 2× large-bore IV access, fluid resuscitation (500mL crystalloid boluses)
- Disability: GCS, analgesia (IV morphine titrated)
- Exposure: Full abdominal examination
2. Sepsis Six Bundle (within 1 hour)
- Give: Oxygen, IV fluids, IV antibiotics
- Take: Blood cultures, Lactate, Urine output monitoring
3. Antibiotic Protocol (NICE NG158)
- Broad-spectrum within 1 hour: Co-amoxiclav 1.2g IV TDS + Metronidazole 500mg IV TDS
- Penicillin allergy: Gentamicin + Metronidazole + Teicoplanin
- Adjust based on local guidelines and sepsis severity
4. Imaging Pathway
- Stable patient: Erect CXR → CT abdomen/pelvis with IV contrast
- Unstable patient: Consider direct to theatre if peritonitis obvious
5. Surgical Referral (urgent)
- Immediate if peritonitis, free gas, or clinical deterioration
- Upper GI perforation: Primary repair ± omental patch vs conservative (selected cases)
- Lower GI perforation: Resection ± stoma (Hartmann's procedure common)
⚠️ Warning: Up to 30% of perforations have no free gas on CXR - CT is gold standard if clinical suspicion persists
Analysis Framework
Upper vs Lower GI Perforation Management
| Feature | Upper GI | Lower GI |
|---|---|---|
| Conservative option | Possible if <24h, minimal contamination, sealed | Rarely appropriate |
| Operative approach | Laparoscopic repair + washout | Laparotomy, resection, often stoma |
| Mortality | 10-20% | 20-40% |
| Post-op NGT | Yes, for gastric decompression | Variable |
| PPI therapy | High-dose IV (omeprazole 80mg then 8mg/h) | Not routinely indicated |
Red Flags for Deterioration 🚩
- Lactate >4 mmol/L or rising
- Systolic BP <90 mmHg despite fluids
- Urine output <0.5 mL/kg/h
- Worsening peritonism or new organ dysfunction
📌 Remember: PERFORATION - Pain sudden, Erect CXR, Rigid abdomen, Free gas, Operative urgency, Resuscitate first, Antibiotics <1h, Time critical, Imaging CT, Outcome depends on speed, Notify surgeons immediately
Visual Aid
Key Points Summary
✓ Mortality 10-40%: Time to surgery is the single most modifiable factor - aim for <6 hours
✓ Imaging hierarchy: Erect CXR (70-80% sensitive) → CT with contrast (>95% sensitive, shows site/cause)
✓ Sepsis Six within 1 hour: Antibiotics (co-amoxiclav + metronidazone), fluids, lactate, cultures, O₂, urine output
✓ Upper GI: May consider conservative management if <24h, minimal contamination, and sealed; otherwise laparoscopic repair + high-dose PPI
✓ Lower GI: Usually requires laparotomy with resection ± stoma (Hartmann's procedure); higher mortality than upper GI
✓ 30% have no free gas on CXR - don't exclude perforation without CT if clinical suspicion remains
✓ Boey score predicts mortality in peptic ulcer perforation: shock + comorbidity + delay >24h
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

