Quick Overview
Bowel obstruction is a surgical emergency requiring rapid assessment to distinguish small bowel (SBO) from large bowel obstruction (LBO), identify strangulation/ischaemia, and determine operative vs conservative management. NICE NG158 emphasizes early imaging, fluid resuscitation, and timely surgical referral. Mortality increases significantly with delayed recognition of strangulation (up to 30% vs 5% in simple obstruction).
Core Facts & Concepts
Key Definitions
- Simple obstruction: Mechanical blockage without vascular compromise
- Strangulation: Vascular compromise causing ischaemia (requires urgent surgery within 6 hours)
- Closed-loop obstruction: Obstruction at two points (e.g., volvulus, hernia) with high strangulation risk
Common Causes
| Small Bowel (80%) | Large Bowel (20%) |
|---|---|
| Adhesions (60%) | Colorectal cancer (60%) |
| Hernias (15%) | Diverticular disease (20%) |
| Malignancy (10%) | Volvulus (15%) |
| Crohn's disease (5%) | Pseudo-obstruction (5%) |
Critical Numbers
- 📊 >6cm caecal diameter: High perforation risk (15-20%)
- 📊 72 hours: Conservative trial duration for SBO (if no strangulation features)
- 📊 Lactate >2mmol/L: Suggests ischaemia/strangulation
- 📊 WCC >15×10⁹/L: Red flag for strangulation
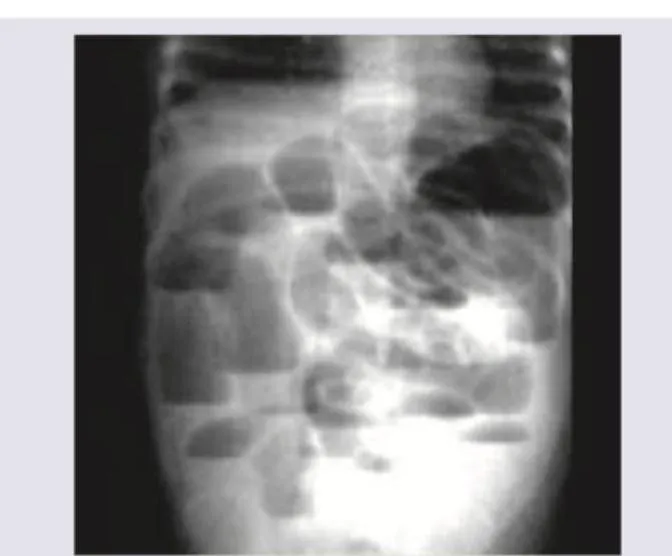
Imaging Findings
| Feature | Small Bowel | Large Bowel |
|---|---|---|
| Dilatation threshold | >3cm | >6cm (>9cm caecum) |
| X-ray pattern | Central, valvulae conniventes (full width) | Peripheral, haustra (partial width) |
| CT sensitivity | 90-95% | 95-100% |
Problem-Solving Approach
1. Initial Assessment (ABCDE)
- Resuscitate: 2L crystalloid bolus, urinary catheter (target >0.5mL/kg/h)
- NGT insertion if vomiting (decompression)
- Bloods: FBC, U&E, lactate, VBG, G&S
2. Imaging Strategy
- Erect CXR: Exclude perforation (pneumoperitoneum)
- AXR: Identify SBO vs LBO pattern
- CT abdomen/pelvis with IV contrast (gold standard): Transition point, cause, strangulation features

3. Identify Strangulation Features 🚩
- Continuous severe pain (not colicky)
- Fever, tachycardia, peritonism
- CT signs: Bowel wall thickening, mesenteric haziness, reduced enhancement, ascites, "whirl sign"
4. Management Decision
5. Surgical Intervention Criteria
- Absolute: Strangulation, perforation, closed-loop with ischaemia
- Relative: Failed conservative trial (72h SBO, 48h LBO), caecal diameter >6cm, complete obstruction with cancer
Analysis Framework
Differentiating SBO from LBO
| Clinical Feature | Small Bowel | Large Bowel |
|---|---|---|
| Vomiting | Early, profuse, bilious | Late, faeculent |
| Pain frequency | High (every 2-3 min) | Low (every 10-15 min) |
| Distension | Minimal initially | Marked, early |
| Bowel sounds | High-pitched, tinkling | Low-pitched, infrequent |
| Dehydration | Rapid, severe | Gradual |
Conservative Management Success Predictors
- Partial obstruction (passage of flatus/stool)
- Previous adhesional SBO
- No peritonism or fever
- Improving on serial examination (4-6 hourly)
⚠️ Warning: Virgin abdomen (no previous surgery) with SBO = malignancy or hernia until proven otherwise
Key Points Summary
✓ Strangulation features (fever, continuous pain, peritonism, lactate >2) mandate emergency surgery within 6 hours
✓ CT with IV contrast is gold standard (90-95% sensitivity); identifies transition point, cause, and ischaemia
✓ Conservative trial: 72 hours for SBO, 48 hours for LBO (with NGT, IV fluids, nil by mouth)
✓ Caecal diameter >6cm or closed-loop obstruction = high perforation risk requiring urgent surgery
✓ Adhesions cause 60% of SBO; colorectal cancer causes 60% of LBO
✓ Serial examination (4-6 hourly) essential to detect deterioration during conservative management
✓ Virgin abdomen with obstruction = think hernia (examine groins) or malignancy first
📌 Remember: The 6s - Strangulation Surgery within 6 hours; Caecum >6cm = danger; 6-hourly reviews
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

