Quick Overview
Acute abdomen represents a spectrum of surgical and medical emergencies requiring rapid triage and assessment. NICE NG158 provides structured guidance for early recognition of life-threatening conditions and timely surgical referral within 2 hours for high-risk presentations. Systematic evaluation using clinical examination, targeted investigations, and risk stratification prevents missed diagnoses and delays in definitive management.
Core Facts & Concepts
🚩 Red Flags for 2-Hour Surgical Referral (NICE NG158):
- Signs of peritonitis (guarding, rigidity, rebound tenderness)
- Suspected ruptured AAA (age >50, pulsatile mass, shock)
- Suspected intestinal obstruction with ischaemia
- Unexplained shock or sepsis with abdominal pain
- Evidence of free intraperitoneal gas
📊 Key Clinical Parameters:
- Bowel ischaemia: Lactate >2 mmol/L with disproportionate pain
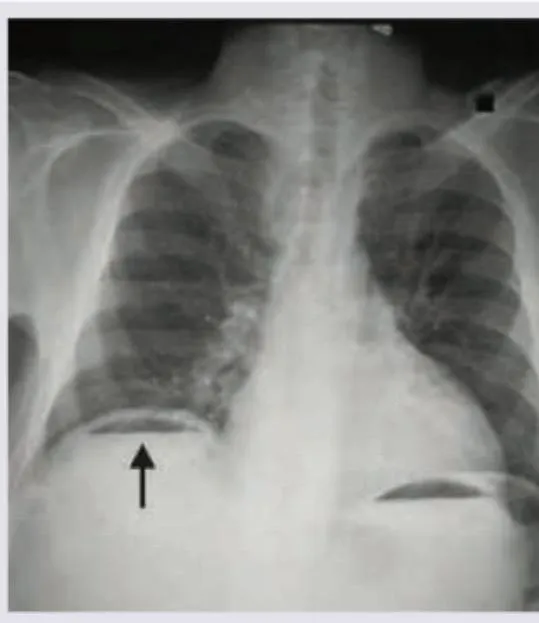
- Perforation: Air under diaphragm on erect CXR (70-80% sensitivity)
- AAA rupture: Mortality 50% if delayed; systolic BP <90 mmHg
- Appendicitis: Alvarado score ≥7 indicates high probability
Initial Resuscitation Priorities:
- IV access (2 large-bore cannulae if shocked)
- Fluid resuscitation: 500ml crystalloid bolus if systolic <90 mmHg
- Analgesia: Do NOT withhold (does not mask peritonism)
- NBM status and NG tube if obstruction/ileus suspected
- Catheterise for fluid balance monitoring
Problem-Solving Approach
Systematic Assessment Framework:
-
Rapid triage (ABCDE approach):
- Airway/Breathing: Assess for aspiration risk, respiratory compromise
- Circulation: BP, HR, capillary refill (<2 seconds normal)
- Disability: Conscious level (pain may cause agitation)
- Exposure: Full abdominal examination
-
Focused history (<5 minutes):
- Pain characteristics: Onset (sudden vs gradual), location, radiation
- Associated symptoms: Vomiting (obstruction), diarrhoea, fever
- Last menstrual period (ectopic pregnancy in women of childbearing age)
- Previous surgery (adhesions), medications (anticoagulation)
-
Examination sequence:
- Inspection: Distension, scars, hernias
- Auscultation BEFORE palpation: Bowel sounds (absent/tinkling)
- Palpation: Start away from pain; assess for peritonism
- Percussion: Shifting dullness (ascites), tympany (obstruction)
- Digital rectal examination: Masses, melaena, tenderness
- Immediate investigations:
- Bloods: FBC, U&E, LFTs, amylase, lactate, group & save
- Imaging: Erect CXR (perforation), AXR (obstruction), USS (biliary/gynae)
- Pregnancy test in all women of childbearing age
Analysis Framework
| Condition | Key Discriminators | Investigation | Timeframe |
|---|---|---|---|
| Perforated viscus | Sudden onset, board-like rigidity, peritonism | Erect CXR (free gas), CT if unclear | Immediate surgery |
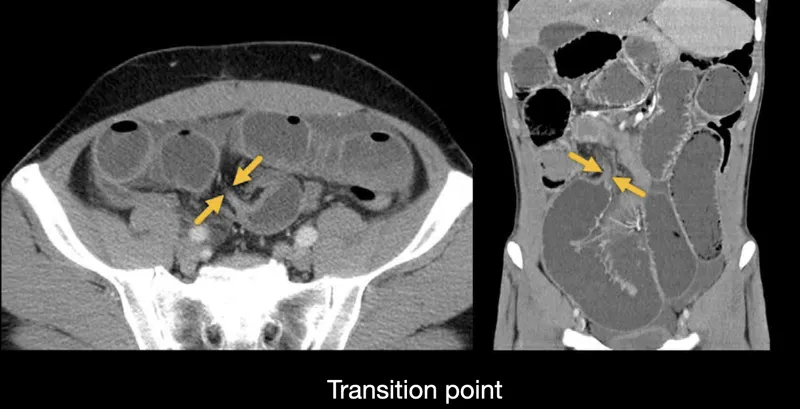
| Bowel obstruction | Colicky pain, distension, vomiting, tinkling bowel sounds | AXR (dilated loops), CT (transition point) | <2h if ischaemia suspected |
| Ruptured AAA | Age >50, shock, pulsatile mass, back pain | No CT if unstable - direct to theatre | Immediate vascular surgery |
| Acute appendicitis | RIF pain, McBurney's point tenderness, fever | USS/CT if diagnostic uncertainty | 6-12h surgical review |
| Acute pancreatitis | Epigastric pain radiating to back, amylase >3× normal | CT after 72h (complications), USS (gallstones) | Conservative initially |
| Mesenteric ischaemia | Pain out of proportion, AF/CVS disease, lactate ↑ | CT angiography | Urgent surgery (<6h) |
🎯 Key Discriminating Features:
- Peritonism = Surgical abdomen until proven otherwise
- Lactate >2 mmol/L + abdominal pain = Ischaemia until excluded
- Sudden onset = Perforation, AAA, ectopic pregnancy
- Gradual onset = Inflammation (appendicitis, cholecystitis, diverticulitis)
Visual Aid
Differential Diagnosis by Location:
| RUQ | Epigastric | RIF | LIF | Diffuse |
|---|---|---|---|---|
| Cholecystitis | Pancreatitis | Appendicitis | Diverticulitis | Peritonitis |
| Hepatitis | Peptic ulcer | Ectopic pregnancy | Colitis | Obstruction |
| Pneumonia | MI | Ovarian torsion | Ovarian pathology | AAA |
Key Points Summary
✓ NICE NG158: Refer within 2 hours if peritonism, suspected ischaemia, ruptured AAA, or unexplained shock
✓ Do NOT withhold analgesia - does not mask peritoneal signs and improves examination compliance
✓ Lactate >2 mmol/L with abdominal pain = bowel ischaemia until proven otherwise; requires urgent CT angiography
✓ Ruptured AAA: If unstable (SBP <90), go directly to theatre - CT causes fatal delay
✓ Pregnancy test mandatory in all women of childbearing age (ectopic pregnancy can present atypically)
✓ Erect CXR detects 70-80% of perforations; if clinical suspicion high but CXR negative, proceed to CT with oral contrast
✓ Bowel sounds: Absent = ileus/peritonitis; High-pitched/tinkling = obstruction; Normal does NOT exclude pathology
⚠️ Warning: Elderly and immunocompromised patients may have minimal abdominal signs despite life-threatening pathology - maintain high index of suspicion
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

