Quick Overview
Collapse and syncope are common emergency presentations requiring rapid differentiation from seizures and cardiac arrest. Syncope = transient loss of consciousness (TLOC) with loss of postural tone due to cerebral hypoperfusion, followed by spontaneous complete recovery. NICE CG109 provides structured risk stratification to identify high-risk patients needing admission and those suitable for outpatient management.
Core Facts & Concepts
Key Definitions:
- Syncope: TLOC <20 seconds, rapid onset, spontaneous complete recovery
- Cardiac syncope: 30-day mortality up to 10% vs <1% for reflex syncope
- Postural hypotension: ≥20 mmHg systolic OR ≥10 mmHg diastolic drop within 3 minutes of standing
Critical Time Points:
- Measure BP at 0, 1, and 3 minutes during postural assessment
- ECG within 1 hour of presentation (NICE CG109)
- Observe 4-6 hours if suspected arrhythmic syncope
Classification by Mechanism:
| Type | Frequency | Key Features |
|---|---|---|
| Reflex (vasovagal) | 60% | Prodrome, triggers, young patients |
| Orthostatic | 15% | Postural drop, medications, elderly |
| Cardiac | 10-15% | No warning, exertional, FH sudden death |
| Unexplained | 10-15% | Requires risk stratification |
Problem-Solving Approach
Distinguishing TLOC Causes:
-
Syncope vs Seizure:
- Syncope: Brief (<20s), rapid recovery, pallor, upright position
- Seizure: Prolonged (>5 min), post-ictal confusion, cyanosis, any position, tongue-biting (lateral), incontinence common
-
Cardiac Arrest vs Syncope:
- Cardiac arrest: No pulse, no breathing, requires CPR
- Syncope: Pulse present, breathing continues, self-limiting
🚩 ECG Red Flags (NICE CG109):
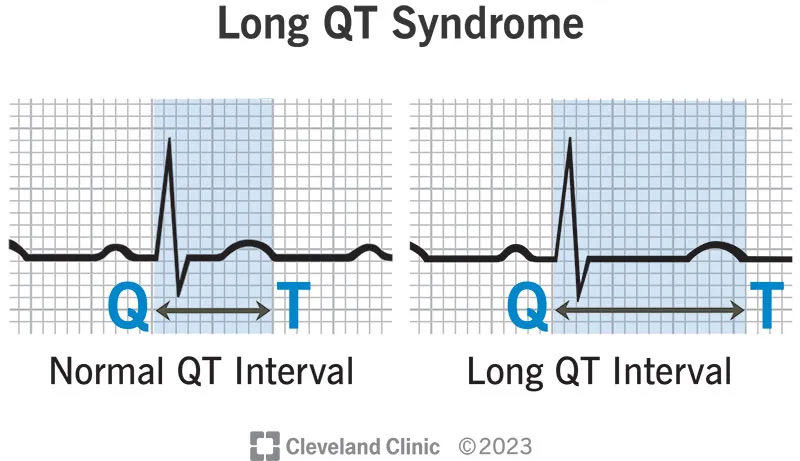
- QTc >450 ms (men) or >470 ms (women) → Long QT syndrome
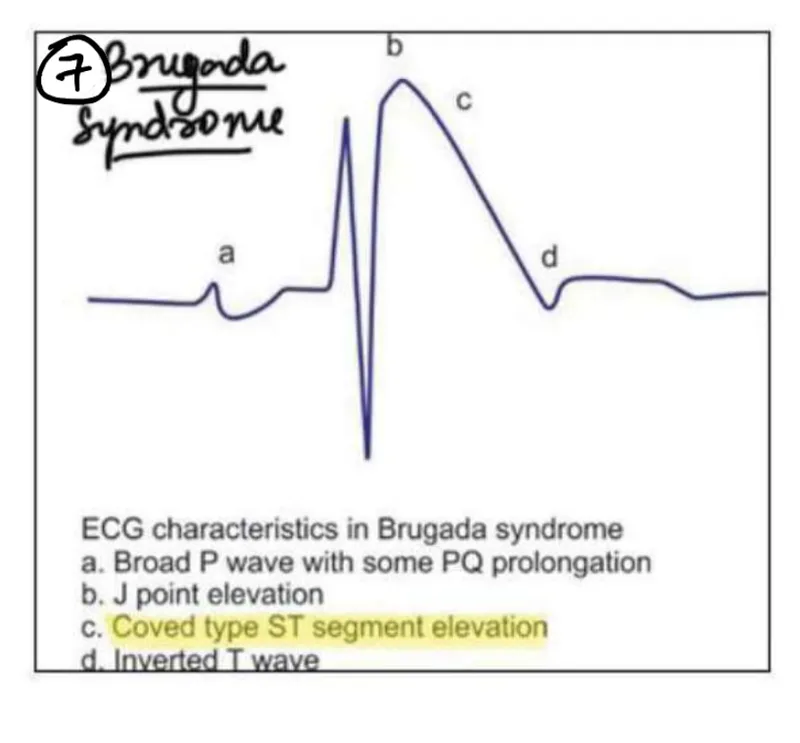
- Brugada pattern (coved ST elevation V1-V2)
- Epsilon waves or TWI V1-V3 → ARVC
- Q waves suggesting MI
- Mobitz II or complete heart block
- Alternating LBBB/RBBB
- SVT/VT on ECG
Analysis Framework
Canadian Syncope Risk Score (7-day serious outcome):
| Risk Factor | Points |
|---|---|
| Clinical judgment predicts serious cause | +2 |
| Vasovagal features absent | +1 |
| Heart disease history | +1 |
| Systolic BP <90 or >180 mmHg | +2 |
| Elevated troponin | +2 |
| Abnormal QRS axis | +1 |
| QTc >450 ms | +1 |
- Score 0: <1% risk (safe discharge)
- Score ≥3: 10% risk (admit)
NICE CG109 Admission Criteria:
- ECG abnormality suggesting arrhythmia
- Heart failure (clinical or ECG evidence)
- Exertional syncope or FH sudden cardiac death <40 years
- New/unexplained breathlessness
- Murmur suggesting valvular disease
Visual Aid
Postural BP Measurement Technique:
| Step | Action | Normal Response |
|---|---|---|
| 1 | Supine BP after 5 min rest | Baseline |
| 2 | Stand patient | Monitor symptoms |
| 3 | Measure at 1 minute | <10 mmHg drop |
| 4 | Measure at 3 minutes | <20/10 mmHg drop |
Key Points Summary
✓ Syncope = TLOC <20s with rapid complete recovery; differentiate from seizure (post-ictal confusion) and cardiac arrest (no pulse)
✓ Immediate ECG mandatory within 1 hour; red flags include QTc >450/470 ms, Brugada pattern, heart block (NICE CG109)
✓ Postural BP: measure at 0, 1, 3 minutes; positive if ≥20/10 mmHg drop
✓ Canadian Syncope Risk Score ≥3 or any NICE admission criteria → admit for monitoring
✓ Cardiac syncope warning signs: exertional, no prodrome, FH sudden death <40 years, abnormal ECG
✓ Score 0 Canadian + normal ECG + no red flags = <1% risk, safe for discharge with outpatient follow-up
✓ Common pitfall: Missing orthostatic hypotension by not waiting 3 minutes or measuring only once
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

