Quick Overview
Neck of femur (NOF) fractures are common orthopaedic emergencies, predominantly affecting elderly patients with osteoporosis. Time-critical management within 36 hours reduces mortality and complications. NICE CG124 mandates orthogeriatric co-management and structured perioperative care bundles. Classification determines surgical approach: intracapsular fractures risk avascular necrosis (AVN) due to disrupted blood supply; extracapsular fractures preserve blood supply but cause significant blood loss.
Core Facts & Concepts
📊 Classification & Blood Supply
| Fracture Type | Location | Blood Supply | AVN Risk | Surgical Options |
|---|---|---|---|---|
| Intracapsular | Within joint capsule | Disrupted (retrograde vessels) | High (10-30%) | DHS if undisplaced; hemiarthroplasty/THR if displaced |
| Extracapsular | Intertrochanteric/subtrochanteric | Preserved (periosteal) | Low | DHS (intertrochanteric); intramedullary nail (subtrochanteric) |
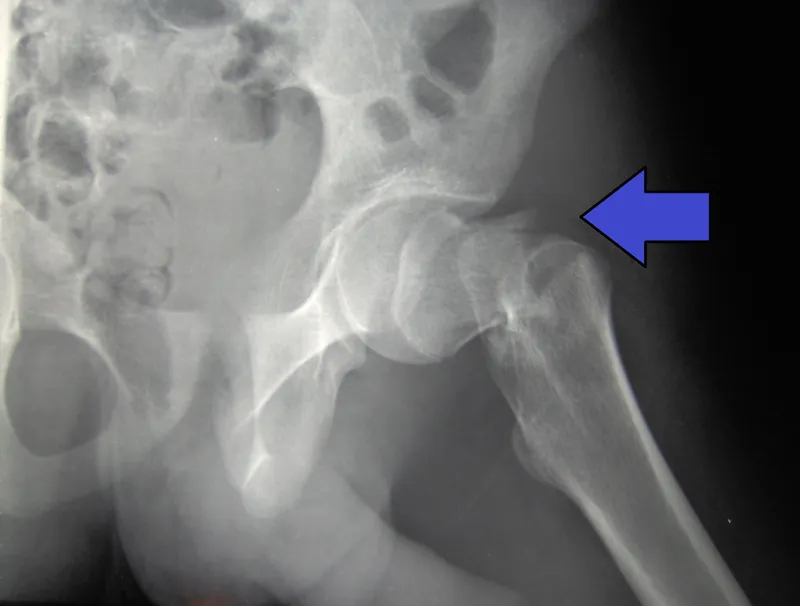
⏰ Time-Critical Thresholds (NICE CG124)
- Surgery within 36 hours of admission (or diagnosis if already inpatient)
- Delays >36h increase 30-day mortality by 30%
- Pre-op assessment by orthogeriatrician within 72 hours of admission
Garden Classification (Intracapsular)
- Type I: Incomplete/impacted (undisplaced)
- Type II: Complete but undisplaced
- Type III: Complete, partially displaced
- Type IV: Complete, fully displaced
- Types III-IV have highest AVN risk (30%)
🚩 Red Flags
- Age <60 with NOF fracture → investigate pathological cause (metastases, myeloma)
- Inability to straight leg raise → suggests fracture
- Shortened, externally rotated leg (classic presentation)
Problem-Solving Approach
1️⃣ Immediate Management (First Hour)
- Analgesia: Fascia iliaca block (preferred) or femoral nerve block
- NBM status, IV access, bloods (FBC, U&E, coagulation, G&S)
- Pressure area care (heel protection)
- VTE prophylaxis (LMWH unless contraindicated)
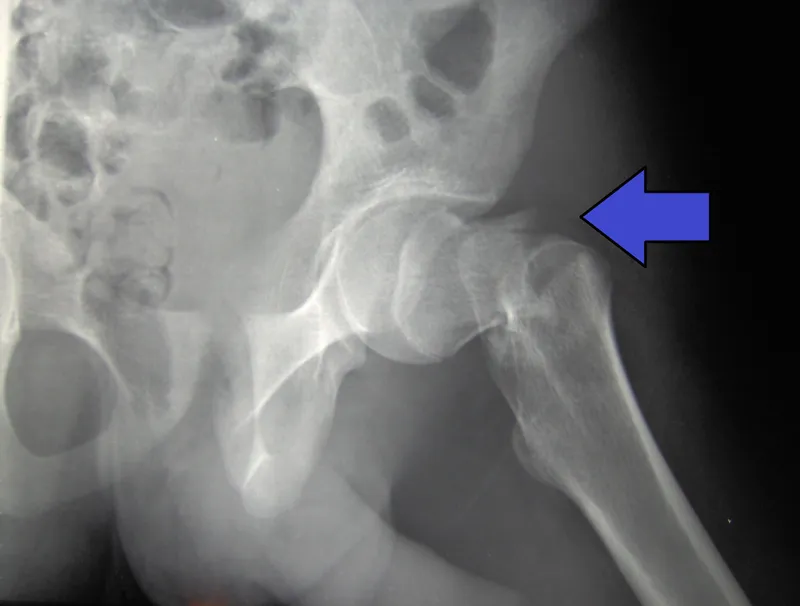
2️⃣ Surgical Decision Algorithm
- Intracapsular undisplaced (Garden I-II) → Internal fixation (cannulated screws/DHS)
- Intracapsular displaced (Garden III-IV):
- Independent walker → Total hip replacement (THR)
- Limited mobility/comorbidities → Hemiarthroplasty (cemented if age >70)
- Extracapsular intertrochanteric → Dynamic hip screw (DHS)
- Extracapsular subtrochanteric → Intramedullary nail (higher biomechanical stress)
3️⃣ Perioperative Care Bundle (NICE CG124)
- Orthogeriatric review within 72h
- Bone protection: Calcium/Vitamin D supplementation
- Falls assessment and prevention plan
- Mobilise day 1 post-op with physiotherapy
- FRAX score for future fracture risk
Analysis Framework
Surgical Option Selection by Patient Factors
| Patient Profile | Fracture Type | Preferred Surgery | Rationale |
|---|---|---|---|
| Independent, mobile, cognitively intact | Displaced intracapsular | THR (cemented/uncemented) | Lower revision rate, better function |
| Limited mobility, dementia, frail | Displaced intracapsular | Cemented hemiarthroplasty | Faster surgery, adequate for low demand |
| Any mobility status | Undisplaced intracapsular | Internal fixation (screws) | Preserve native joint, lower morbidity |
| Any mobility status | Intertrochanteric | DHS | Gold standard, stable fixation |
| Any mobility status | Subtrochanteric | Intramedullary nail | Biomechanically superior for shaft extension |
🚩 Complications by Timeframe
- Immediate: Fat embolism, blood loss (500-1000ml extracapsular)
- Early (<6 weeks): DVT/PE, pneumonia, pressure sores, delirium
- Late (>6 weeks): AVN (intracapsular), non-union, implant failure, leg length discrepancy
Visual Aid
Key Points Summary
✓ 36-hour rule: Surgery within 36h of admission/diagnosis mandatory (NICE CG124) - delays increase mortality 30%
✓ Intracapsular fractures: High AVN risk (disrupted blood supply); displaced → arthroplasty; undisplaced → internal fixation
✓ Extracapsular fractures: Preserved blood supply, low AVN risk; DHS for intertrochanteric, IM nail for subtrochanteric
✓ Surgical selection: Independent mobile patients with displaced intracapsular → THR; limited mobility → cemented hemiarthroplasty
✓ Perioperative bundle: Fascia iliaca block, orthogeriatric co-management within 72h, mobilise day 1, bone protection (calcium/vitamin D)
✓ Garden classification: I-II undisplaced (fixation), III-IV displaced (arthroplasty) - higher numbers = higher AVN risk
✓ Red flags: Age <60 (pathological fracture?), inability to straight leg raise, shortened externally rotated leg
⚠️ Warning: Never delay surgery for "medical optimization" beyond 36h unless life-threatening condition - mortality benefit of early surgery outweighs most medical risks
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

