Orthopaedics & MSK

On this page
Recognising Orthopaedic Emergencies: Foundations
A 78-year-old woman presents to the Emergency Department after a mechanical fall at home. She reports severe left hip pain and is unable to bear weight. Her left leg appears shortened and externally rotated. This classic presentation of a neck of femur fracture represents one of the most time-critical orthopaedic emergencies, with mortality reaching 30% at one year if management is delayed. Meanwhile, in the adjacent bay, a 45-year-old man complains of sudden-onset lower back pain radiating to both legs, accompanied by urinary retention-a constellation suggesting cauda equina syndrome requiring urgent MRI and surgical decompression.
Epidemiology and burden:
-
Neck of femur fractures: 75,000 cases annually in the UK; 90% occur in patients >65 years
- 30-day mortality: 8-10%; one-year mortality: 20-30%
- Female:male ratio 3:1 due to osteoporosis prevalence
- Direct cost to NHS: >£2 billion annually
-
Cauda equina syndrome: Incidence 1-3 per 100,000; peak age 30-50 years
- Permanent neurological deficit occurs if decompression delayed >48 hours
- Most common cause: massive central disc herniation (L4/5 or L5/S1)
Critical anatomical classifications:
-
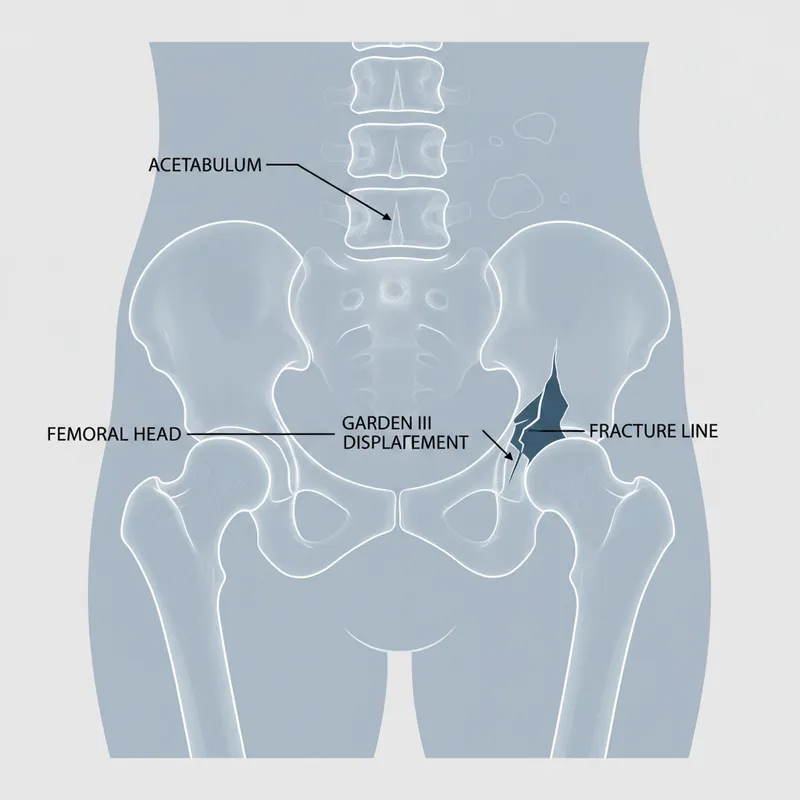
Neck of femur fractures classified by Garden classification (intracapsular) or extracapsular location
- Intracapsular: High risk of avascular necrosis due to retrograde blood supply from femoral circumflex arteries
- Extracapsular: Intertrochanteric or subtrochanteric; lower AVN risk but higher surgical blood loss
-
**Spinal red flags ** require systematic anatomical localisation
- Cauda equina: Bilateral leg pain, saddle anaesthesia, bladder/bowel dysfunction
- Spinal cord compression: Upper motor neuron signs, sensory level, bilateral symptoms
- Vertebral infection/malignancy: Progressive pain, night pain, systemic features
📌 Mnemonic for Cauda Equina RED FLAGS: SINE - Saddle anaesthesia, Incontinence (urinary retention), Numbness (bilateral), Emergency (MRI within 24h)
| Classification | Location | AVN Risk | Typical Management |
|---|---|---|---|
| Garden I-II (undisplaced) | Intracapsular | 10-15% | Internal fixation (cannulated screws) |
| Garden III-IV (displaced) | Intracapsular | 30-40% | Hemiarthroplasty (>65y) or total hip replacement |
| Intertrochanteric | Extracapsular | <5% | Dynamic hip screw or intramedullary nail |
| Subtrochanteric | Extracapsular | <5% | Intramedullary nail (cephalomedullary) |


Recognising Orthopaedic Emergencies: Foundations
2 - Pathophysiological Mechanisms: From Injury to Complication
The pathophysiology of neck of femur fractures centres on the disruption of a precarious blood supply. The femoral head receives 70% of its blood from the medial and lateral femoral circumflex arteries, which enter at the base of the neck and travel proximally beneath the synovium. When an intracapsular fracture occurs, these vessels are torn or kinked, initiating a race against time. Within 6-12 hours, osteocyte death begins; by 24-48 hours, avascular necrosis becomes irreversible. This explains why NICE CG124 mandates surgery within 36 hours of admission-and ideally within 24 hours of injury.
Biomechanical failure patterns:
-
Osteoporotic bone: T-score ≤-2.5 reduces bone mineral density by 30-40%
- Trabecular architecture loss reduces energy absorption capacity
- Low-energy falls (from standing height) sufficient to cause fracture
-
Vascular compromise sequence:
- Immediate: Haemarthrosis increases intracapsular pressure to 50-80 mmHg
- 6-12 hours: Tamponade effect reduces femoral head perfusion by 60%
- 24-48 hours: Irreversible osteocyte death and AVN established
Spinal compression pathophysiology :
-
Cauda equina: L2-S5 nerve roots compressed by disc herniation or tumour
- Venous congestion → axonal oedema → demyelination → permanent deficit
- Critical window: 48 hours before irreversible bladder dysfunction
-
Cord compression: Direct mechanical pressure + vascular insufficiency
- Arterial watershed zones (T4, T10) most vulnerable
- Epidural abscess expands at 1-2 vertebral levels per day
| Complication | Timeframe | Mechanism | Prevention |
|---|---|---|---|
| Avascular necrosis | 6-48 hours | Vascular disruption | Surgery <24h |
| Fat embolism | 24-72 hours | Marrow contents → pulmonary circulation | Early fixation, careful reaming |
| Pressure ulcers | 2-6 hours | Immobility on hard trolley | Pressure-relieving mattress |
| Permanent bladder dysfunction | >48 hours | Cauda equina compression | MRI + decompression <24h |
2 — Pathophysiological Mechanisms: From Injury to Complication
3 - Clinical Assessment and Diagnostic Pathways
A 72-year-old woman arrives by ambulance following a fall in her garden. Your primary survey reveals stable vital signs, but she's in severe pain and cannot lift her left leg. You notice the classic triad: shortened limb (2-3 cm), external rotation (40-90°), and abduction. Before ordering imaging, you perform a focused neurovascular examination-dorsalis pedis pulse present, sensation intact, no compartment syndrome features. This systematic approach, mandated by NICE CG124, ensures you don't miss concurrent injuries or complications.
Structured examination for neck of femur fracture :
-
Inspection: Limb position, leg length discrepancy (measure ASIS to medial malleolus)
- Intracapsular: 1-3 cm shortening, 40-90° external rotation
- Extracapsular: Greater shortening (3-5 cm), more severe rotation
-
Palpation: Tenderness over greater trochanter (extracapsular) vs groin (intracapsular)
- Check for ipsilateral knee pain (referred from hip)
-
Neurovascular assessment: Mandatory before and after any manipulation
- Sciatic nerve (foot dorsiflexion/plantarflexion)
- Femoral nerve (knee extension, anterior thigh sensation)
Imaging protocol:
-
AP pelvis + lateral hip: First-line; sensitivity 90-95% for displaced fractures
- Shenton's line: Smooth arc from inferior femoral neck to superior obturator foramen-disrupted in fracture
- Trabecular patterns: Loss of normal compressive and tensile trabeculae
-
MRI hip: If X-ray negative but high clinical suspicion (occult fracture)
- Sensitivity 99%, specificity 95%
- Detects bone marrow oedema within 24 hours of injury
Spinal red flag assessment :
-
Cauda equina screening (MANDATORY for all back pain presentations):
- Saddle anaesthesia (S3-S5 dermatomes): Test perianal sensation with cotton wool
- Bladder dysfunction: Post-void residual >200 mL on catheterisation
- Bilateral leg symptoms: Weakness, numbness, or radicular pain
-
Spinal cord compression features:
- Sensory level: Test pinprick ascending from feet
- Upper motor neuron signs: Hyperreflexia, upgoing plantars, clonus
- Sphincter tone: Digital rectal examination (reduced in cauda equina, preserved in cord compression)
🚩 Red Flag: Urinary retention with painless bladder distension = late cauda equina sign. If present, MRI must occur within 4 hours, decompression within 24 hours.
| Investigation | Sensitivity | Specificity | Timing | Cost |
|---|---|---|---|---|
| AP/Lateral X-ray | 90-95% | 95% | Immediate | £30 |
| MRI hip | 99% | 95% | <24h if X-ray negative | £200 |
| MRI whole spine | 93% | 97% | <24h for cauda equina | £250 |
| CT spine | 87% | 90% | If MRI contraindicated | £100 |
3 — Clinical Assessment and Diagnostic Pathways
4 - Differential Diagnosis: Distinguishing Hip and Spinal Pathology
The challenge in orthopaedic emergencies lies in recognising mimics. A patient with groin pain and inability to weight-bear doesn't always have a neck of femur fracture -pubic ramus fractures, hip dislocations, and pathological fractures present similarly. Meanwhile, back pain with leg symptoms could represent benign radiculopathy, spinal stenosis, or life-threatening cauda equina syndrome . The key is systematic evaluation of discriminating features.
Hip pathology differentials:
-
Pubic ramus fracture: Groin pain, weight-bearing difficulty, but NO limb shortening or rotation
- Often missed on initial X-ray; MRI shows bone marrow oedema
- Common in osteoporotic patients; can coexist with NOF fracture (10% of cases)
-
Hip dislocation: Severe pain, limb position depends on direction
- Posterior (90%): Flexed, adducted, internally rotated
- Anterior (10%): Extended, abducted, externally rotated
- Requires immediate reduction (<6 hours) to prevent AVN
-
Pathological fracture: Minimal trauma, history of malignancy or bone pain
- X-ray shows lytic lesions; requires oncology input before fixation
Spinal pathology discriminators:
-
Cauda equina vs. severe sciatica:
- Cauda equina: Bilateral symptoms, saddle anaesthesia, bladder dysfunction
- Sciatica: Unilateral leg pain, normal bladder function, straight leg raise <30°
-
Cord compression vs. cauda equina:
- Cord: Upper motor neuron signs, sensory level, preserved anal tone
- Cauda: Lower motor neuron signs, no sensory level, reduced anal tone
⭐ Clinical Pearl: Always check post-void residual in back pain patients. Normal is <50 mL; >200 mL = cauda equina until proven otherwise.
| Feature | NOF Fracture | Pubic Ramus | Hip Dislocation | Cauda Equina | Sciatica |
|---|---|---|---|---|---|
| Limb shortening | 1-5 cm | Absent | Variable | N/A | N/A |
| Rotation | External 40-90° | Normal | Internal (post) / External (ant) | N/A | N/A |
| Bilateral symptoms | No | No | No | Yes | No |
| Bladder dysfunction | No | No | No | Yes | No |
| Saddle anaesthesia | No | No | No | Yes | No |
4 — Differential Diagnosis: Distinguishing Hip and Spinal Pathology
5 - Evidence-Based Management: Surgical Timing and Technique
The management philosophy for neck of femur fractures is simple: surgery saves lives. NICE CG124 mandates surgery within 36 hours of admission because every 12-hour delay increases 30-day mortality by 6%. The choice of procedure depends on fracture type, patient age, and pre-morbid mobility. For intracapsular fractures in patients >65 years, arthroplasty (hemiarthroplasty or total hip replacement) is superior to fixation because it eliminates AVN risk and allows immediate weight-bearing.
Surgical decision algorithm:
-
Intracapsular undisplaced (Garden I-II):
- Internal fixation: 3 cannulated screws in inverted triangle configuration
- Weight-bearing: Partial for 6 weeks, then full
- Failure rate: 15% requiring revision to arthroplasty
-
Intracapsular displaced (Garden III-IV):
- Age >65 years: Hemiarthroplasty (cemented Austin-Moore or Thompson)
- Age <65 years OR high functional demand: Total hip replacement (lower revision rate)
- Cognitively impaired/low mobility: Hemiarthroplasty (faster surgery, lower dislocation risk)
-
Extracapsular (intertrochanteric/subtrochanteric):
- Stable pattern: Dynamic hip screw (DHS) with 135° plate
- Unstable pattern/subtrochanteric: Cephalomedullary nail (e.g., Gamma nail)
- Weight-bearing: Immediate full weight-bearing in most cases
Perioperative optimisation (NICE CG124):
-
Analgesia: Fascia iliaca block (20 mL 0.25% levobupivacaine) within 30 minutes
- Reduces opioid requirements by 60%; improves pre-operative mobility
-
VTE prophylaxis: LMWH (enoxaparin 40 mg SC daily) started on admission
- Continue for 28 days post-operatively (extended prophylaxis)
-
Bone protection: Vitamin D 800 IU + calcium 1000 mg daily
- Start bisphosphonate (alendronate 70 mg weekly) at 2 weeks post-op
| Procedure | Operative Time | Blood Loss | Hospital Stay | Complication Rate |
|---|---|---|---|---|
| Cannulated screws | 45 min | 100 mL | 5-7 days | 15% failure |
| Hemiarthroplasty | 60 min | 300 mL | 7-10 days | 5% dislocation |
| Total hip replacement | 90 min | 400 mL | 5-7 days | 3% dislocation |
| Dynamic hip screw | 60 min | 250 mL | 5-7 days | 5% fixation failure |
5 — Evidence-Based Management: Surgical Timing and Technique
6 - Multidisciplinary Care: Beyond the Operating Theatre
Real-world patients rarely fit textbook categories. Consider an 85-year-old with dementia, atrial fibrillation on warfarin, and chronic kidney disease who sustains a displaced intracapsular fracture. Surgical decision-making must balance fracture fixation with anticoagulation reversal, renal-adjusted anaesthesia dosing, and post-operative delirium prevention. NICE CG124 emphasises orthogeriatric co-management, which reduces mortality by 20% and length of stay by 3 days through comprehensive geriatric assessment.
Complex scenarios requiring MDT input:
-
Anticoagulation: Warfarin requires vitamin K 5 mg IV + prothrombin complex concentrate (PCC) for INR >1.5
- DOACs: Delay surgery 24-48 hours for renal clearance; idarucizumab for dabigatran reversal if urgent
-
Chronic kidney disease (eGFR <30):
- Avoid NSAIDs; reduce morphine dose by 50%
- Cemented prosthesis preferred (uncemented requires good bone quality)
-
Cognitive impairment/dementia:
- Higher dislocation risk with total hip replacement (10% vs. 3%)
- Hemiarthroplasty preferred; consider constrained liner if severe
Cauda equina surgical decompression :
-
Timing: NICE NG59 recommends decompression within 48 hours of symptom onset
- Best outcomes if surgery within 24 hours
- Bladder function recovery: 70% if <24h, 30% if >48h
-
Technique: Posterior laminectomy + discectomy at affected level(s)
- Bilateral decompression for central disc herniation
- Duraplasty if dural tear occurs (10% of cases)
-
Post-operative management:
- Urinary catheter for 48-72 hours; teach clean intermittent self-catheterisation
- Pelvic floor physiotherapy; bladder retraining programme
Long-term sequelae:
-
NOF fracture: 50% never regain pre-fracture mobility; 20% require long-term care
- Bone protection essential: DEXA scan at 3 months; treat osteoporosis
-
Cauda equina: Permanent bladder dysfunction in 30-50%; sexual dysfunction in 40%
- Lifelong urology follow-up; intermittent catheterisation training
| Population | Specific Consideration | Management Adjustment |
|---|---|---|
| Renal impairment (eGFR <30) | Morphine accumulation | Reduce dose by 50%; use oxycodone |
| Dementia | High dislocation risk | Hemiarthroplasty over THR |
| Anticoagulation (warfarin) | Bleeding risk | Reverse with PCC + vitamin K |
| Pregnancy (rare) | Radiation exposure | MRI for diagnosis; avoid CT |
6 — Multidisciplinary Care: Beyond the Operating Theatre
High Yield Summary
Key Take-Aways:
- Neck of femur fractures: Surgery within 36 hours (ideally <24h) reduces 30-day mortality by 6% per 12-hour delay; intracapsular displaced fractures in patients >65 years require arthroplasty, not fixation
- Cauda equina syndrome: MRI within 24 hours + surgical decompression within 48 hours prevents permanent bladder dysfunction (70% recovery if <24h vs. 30% if >48h)
- Garden classification: I-II (undisplaced) → internal fixation; III-IV (displaced) → arthroplasty in elderly; extracapsular → DHS or intramedullary nail
- Red flag triad for cauda equina: Saddle anaesthesia + bilateral leg symptoms + bladder dysfunction (post-void residual >200 mL) = emergency MRI
- Fascia iliaca block: Administer within 30 minutes of arrival; reduces opioid use by 60% and improves pre-operative mobility
- Orthogeriatric co-management: Reduces mortality by 20% and length of stay by 3 days through comprehensive geriatric assessment and multidisciplinary rehabilitation
Essential Orthopaedics & MSK Numbers:
| Parameter | Value | Clinical Significance |
|---|---|---|
| NOF 30-day mortality | 8-10% | Increases 6% per 12h delay |
| NOF 1-year mortality | 20-30% | 50% never regain mobility |
| AVN risk (displaced intracapsular) | 30-40% | Arthroplasty preferred >65y |
| Cauda equina incidence | 1-3 per 100,000 | Bladder recovery 70% if <24h |
| Post-void residual (normal) | <50 mL | >200 mL = cauda equina |
| Surgery timing (NICE CG124) | <36 hours | Ideally <24 hours from injury |
Key Principles/Pearls:
- Always check Shenton's line on AP pelvis X-ray-disruption indicates intracapsular fracture even if subtle
- Post-void residual bladder scan is mandatory for all back pain presentations with leg symptoms; don't rely on patient's subjective report
- Cemented hemiarthroplasty is faster and safer than uncemented in frail elderly patients with osteoporotic bone
- Fat embolism syndrome (confusion, hypoxia, petechial rash) peaks 24-72 hours post-fracture; early surgical fixation reduces risk
- Pathological fractures require oncology input before fixation-standard implants may fail in lytic bone
Quick Reference:
| Emergency | Diagnostic Test | Critical Timing | Definitive Management |
|---|---|---|---|
| Displaced intracapsular NOF | AP pelvis + lateral hip X-ray | Surgery <36h | Hemiarthroplasty (>65y) |
| Cauda equina syndrome | MRI whole spine | MRI <24h | Decompression <48h |
| Extracapsular NOF (stable) | AP pelvis X-ray | Surgery <36h | Dynamic hip screw |
| Extracapsular NOF (unstable) | AP pelvis X-ray | Surgery <36h | Cephalomedullary nail |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app




