General Surgery

On this page
Foundations of General Surgical Diagnosis
A 28-year-old man presents to the emergency department at 2 AM with severe right iliac fossa pain that began periumbilically 8 hours ago. He's now reluctant to move, lying still with his right hip flexed. This classic presentation exemplifies why systematic knowledge of surgical anatomy and classification remains the cornerstone of acute surgical assessment. Understanding anatomical landmarks, scoring systems, and disease classifications enables rapid triage between conditions requiring immediate intervention and those suitable for conservative management.
-
Anatomical landmarks for acute abdomen assessment:
- McBurney's point: junction of lateral 1/3 and medial 2/3 of line from ASIS to umbilicus (maximal tenderness in )
- Rovsing's sign: RIF pain on LIF palpation (peritoneal irritation)
- Psoas sign: pain on hip extension (retrocaecal inflammation)
-
Hernia classification by anatomical location :
- Inguinal (75%): indirect (lateral to inferior epigastric vessels) vs direct (medial)
- Femoral (5%): below inguinal ligament, medial to femoral vein, high strangulation risk (15-20%)
- Incisional (10%): through previous surgical wounds
- Umbilical/paraumbilical (10%)
-
Alvarado Score for appendicitis (maximum 10 points):
- Symptoms: migration of pain (1), anorexia (1), nausea/vomiting (1)
- Signs: RIF tenderness (2), rebound tenderness (1), fever >37.3°C (1)
- Laboratory: leucocytosis >10×10⁹/L (2), neutrophilia >75% (1)
- Score ≥7: high probability, consider surgical intervention
- Score 5-6: equivocal, imaging recommended
- Score ≤4: appendicitis unlikely

| Classification | Duke's Stage | TNM Equivalent | 5-Year Survival |
|---|---|---|---|
| A: Mucosa/submucosa only | T1-2 N0 M0 | 95% | |
| B: Through muscularis propria | T3-4 N0 M0 | 70-85% | |
| C: Lymph node involvement | Any T N1-2 M0 | 45-65% | |
| D: Distant metastases | Any T Any N M1 | 5-10% |
📌 Mnemonic for hernia complications: INCS - Incarceration, Necrosis, Cough impulse absent, Strangulation
Foundations of General Surgical Diagnosis
2 - Pathophysiological Mechanisms in Surgical Disease
The progression from simple inflammation to surgical emergency follows predictable pathways that dictate management urgency. In , luminal obstruction by faecolith, lymphoid hyperplasia, or parasites initiates a cascade: mucus accumulation raises intraluminal pressure, venous congestion develops, bacterial overgrowth (predominantly E. coli and Bacteroides) causes transmural inflammation, and ultimately arterial compromise leads to gangrene and perforation within 24-48 hours. This timeline explains why diagnostic accuracy must be balanced against the risks of observation.
-
Appendicitis progression timeline:
- 0-12 hours: visceral pain (T10), periumbilical, poorly localised
- 12-24 hours: parietal peritoneum involvement, pain localises to RIF
- 24-48 hours: risk of perforation increases exponentially (20% at 24h, 65% at 48h)
- Post-perforation: abscess formation or generalised peritonitis
-
Hernia pathophysiology:
- Increased intra-abdominal pressure (chronic cough, constipation, ascites, pregnancy)
- Weakness in abdominal wall (congenital patent processus vaginalis, collagen disorders)
- Strangulation: venous outflow obstruction → oedema → arterial compromise → necrosis within 6 hours
- Richter's hernia: only anti-mesenteric border strangulated, bowel lumen patent, easily missed
- Colorectal carcinogenesis:
- Adenoma-carcinoma sequence: 10-15 years progression
- APC gene mutation → β-catenin accumulation → Wnt pathway activation
- KRAS mutation (40%): predicts resistance to anti-EGFR therapy
- Microsatellite instability (15%): Lynch syndrome, better prognosis
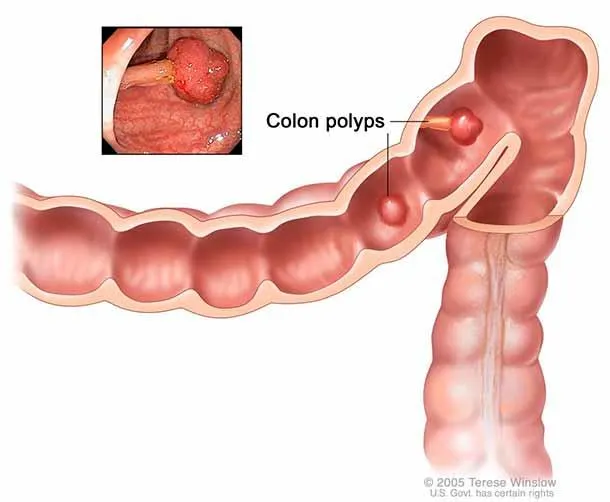
2 — Pathophysiological Mechanisms in Surgical Disease
3 - Diagnostic Strategies in Acute Surgical Presentations
A 72-year-old woman with altered bowel habit presents with iron-deficiency anaemia (Hb 89 g/L, MCV 76 fL, ferritin 8 μg/L). No overt PR bleeding reported. This mandates investigation for regardless of age, as right-sided lesions frequently present insidiously. The diagnostic pathway integrates clinical probability with investigation sensitivity, recognising that no single test achieves 100% accuracy.
-
CT imaging in acute appendicitis:
- Sensitivity 94%, specificity 95% (reduces negative appendicectomy rate from 20% to <5%)
- Positive findings: appendiceal diameter >6mm, wall thickening >3mm, periappendiceal fat stranding, appendicolith (30%)
- NICE NG104 recommends CT for adults with Alvarado 5-6 (equivocal cases)
- Ultrasound first-line in children/pregnancy (sensitivity 88%, specificity 94%)
-
Hernia examination findings :
- Reducibility: can contents be returned to abdominal cavity?
- Cough impulse: expansile impulse indicates patent neck
- Absence of cough impulse + tenderness = strangulation until proven otherwise
- Bowel sounds in hernia sac suggest bowel content
- Femoral vs inguinal: femoral emerges below and lateral to pubic tubercle
- Colorectal cancer investigation pathway (NICE NG151):
- Faecal immunochemical test (FIT): ≥10 μg Hb/g faeces = 2-week-wait referral
- Colonoscopy: gold standard, sensitivity >95% for lesions >1cm, allows biopsy
- CT colonography: if colonoscopy incomplete/contraindicated, 90% sensitivity for >1cm polyps
- Staging CT chest/abdomen/pelvis: mandatory before treatment planning
- MRI pelvis: essential for rectal cancer (assesses mesorectal fascia involvement)
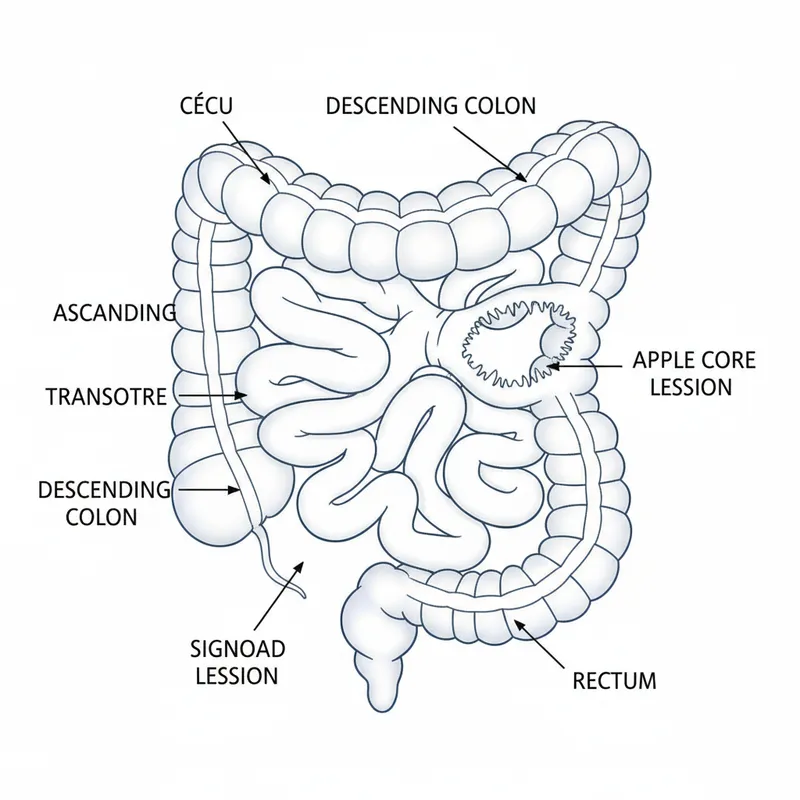
| Investigation | Sensitivity | Specificity | Key Advantage | Limitation |
|---|---|---|---|---|
| CT abdomen (appendicitis) | 94% | 95% | Identifies complications | Radiation, contrast |
| Ultrasound (appendicitis) | 88% | 94% | No radiation | Operator-dependent |
| Colonoscopy (CRC) | 95% | 100% | Biopsy capability | Invasive, perforation risk |
| FIT (CRC screening) | 79% | 94% | Non-invasive | False negatives |
3 — Diagnostic Strategies in Acute Surgical Presentations
4 - Differential Diagnosis and Clinical Reasoning
Distinguishing surgical from non-surgical acute abdomen prevents unnecessary operations while avoiding delayed intervention in true emergencies. Right iliac fossa pain in must be differentiated from ectopic pregnancy (β-hCG mandatory in women of reproductive age), ovarian pathology (torsion, cyst rupture), mesenteric adenitis (preceding viral URTI, mobile tenderness), and inflammatory bowel disease (chronic symptoms, extra-intestinal features). The key lies in recognising patterns rather than relying on single features.
-
Critical discriminators for RIF pain:
- Appendicitis: anorexia (80%), migration of pain (50%), maximal tenderness at McBurney's point
- Ectopic pregnancy: amenorrhoea, positive β-hCG, adnexal mass on USS
- Ovarian torsion: sudden onset, intermittent (torsion/detorsion), whirl sign on Doppler USS
- Crohn's disease: chronic diarrhoea, weight loss, perianal disease, transmural inflammation on imaging
-
Colorectal cancer red flags :
- Change in bowel habit >6 weeks (especially looser/more frequent in >50s)
- Rectal bleeding with altered bowel habit (not attributed to haemorrhoids)
- Iron-deficiency anaemia without overt bleeding (Hb <110 g/L women, <120 g/L men)
- Palpable rectal/abdominal mass
- Unexplained weight loss >5% in 6 months
| Feature | Appendicitis | Ectopic Pregnancy | Ovarian Torsion | Mesenteric Adenitis |
|---|---|---|---|---|
| Onset | Gradual (hours) | Sudden/gradual | Sudden | Gradual |
| Pain migration | Yes (periumbilical→RIF) | No | No | No |
| Anorexia | Prominent | Variable | Minimal | Variable |
| β-hCG | Negative | Positive | Negative | Negative |
| Fever | Low-grade | Absent | Variable | Often present |
| Key investigation | CT/USS | Transvaginal USS + β-hCG | Pelvic USS Doppler | Clinical diagnosis |
4 — Differential Diagnosis and Clinical Reasoning
5 - Evidence-Based Management Approaches
Treatment decisions in general surgery increasingly incorporate risk stratification and patient-specific factors rather than universal operative approaches. For uncomplicated , NICE NG104 supports initial conservative management with antibiotics (co-amoxiclav 1.2g TDS IV for 48h, then oral 625mg TDS for 5 days) in selected patients, though appendicectomy remains definitive with lower recurrence risk (5% vs 20-30% at 1 year). management balances operative risk against strangulation risk, with watchful waiting acceptable for asymptomatic inguinal hernias in men (annual strangulation risk 0.3%), but urgent repair mandatory for femoral hernias given 15-20% strangulation risk.
- Appendicectomy timing and approach:
- Emergency operation within 6-8 hours if peritonitis/sepsis
- Laparoscopic preferred: lower wound infection (5% vs 10%), faster recovery, better cosmesis
- Complicated appendicitis: IV antibiotics (piperacillin-tazobactam 4.5g TDS) + source control
- Appendix mass: conservative management + interval appendicectomy at 6-8 weeks (controversial)
- Colorectal cancer management :
- Colon cancer: segmental colectomy (right/left hemicolectomy, sigmoid colectomy)
- Rectal cancer: total mesorectal excision (TME), consider neoadjuvant chemoradiotherapy if T3/T4 or node-positive
- Adjuvant chemotherapy (FOLFOX): stage III (node-positive) mandatory, stage II high-risk (T4, perforation, <12 nodes examined)
- Metastatic disease: resection if oligometastatic liver/lung disease, palliative chemotherapy (FOLFOX/FOLFIRI ± biologics)
| Condition | First-Line Treatment | Dosing/Timing | Alternative | Complication Rate |
|---|---|---|---|---|
| Uncomplicated appendicitis | Laparoscopic appendicectomy | Within 24h of admission | IV antibiotics (conservative) | 5-10% |
| Inguinal hernia | Lichtenstein mesh repair | Elective day-case | Laparoscopic TEP/TAPP | <1% recurrence |
| Stage III colon cancer | Resection + adjuvant FOLFOX | 6 months chemotherapy | CAPOX (oral alternative) | 15% anastomotic leak |
| Rectal cancer (T3) | Neoadjuvant CRT + TME | 6 weeks RT, surgery 8-12 weeks | Short-course RT | 10-15% LARS |
5 — Evidence-Based Management Approaches
6 - Complex Cases and Advanced Integration
Real-world surgical decision-making confronts multimorbidity, atypical presentations, and special populations requiring individualised strategies. An 85-year-old with , severe frailty (Clinical Frailty Scale 7), and multiple comorbidities presents a management dilemma: operative mortality may exceed 10%, yet conservative management risks progression to perforation and sepsis with >30% mortality. Shared decision-making incorporating patient values becomes paramount. Similarly, in pregnancy (rare, 1:13,000) demands MDT coordination: second-trimester surgery feasible, third-trimester may require delayed treatment post-delivery.
-
Special population considerations:
- Elderly surgical patients: comprehensive geriatric assessment, frailty scoring, avoid polypharmacy
- Pregnancy: defer non-urgent surgery to second trimester, laparoscopy safe with precautions
- Immunosuppressed: higher infection risk, consider CT liberally, lower threshold for intervention
- Anticoagulation: assess bleeding vs thrombotic risk, bridging protocols for high-risk patients
-
Hernia complications requiring advanced management :
- Strangulated hernia with bowel ischemia: emergency laparotomy, bowel resection if non-viable
- Mesh infection (1-2%): remove mesh if persistent sepsis despite antibiotics
- Chronic post-herniorrhaphy pain (10-12%): neuropathic agents (gabapentin 300mg TDS), nerve blocks, rarely mesh removal
-
Colorectal cancer emerging evidence:
- Watch-and-wait for complete clinical response post-neoadjuvant therapy in rectal cancer (selected cases)
- Immunotherapy (pembrolizumab) for MSI-high/dMMR tumours: 40% response rate in metastatic disease
- Circulating tumour DNA (ctDNA) for minimal residual disease detection post-resection (investigational)
| Complication | Incidence | Management | Prevention |
|---|---|---|---|
| Anastomotic leak (colorectal) | 5-10% | IV antibiotics, percutaneous drainage, defunctioning stoma | Adequate blood supply, tension-free anastomosis |
| Incisional hernia | 10-20% | Mesh repair if symptomatic | Mass closure, avoid infection |
| Low anterior resection syndrome | 60-80% | Pelvic floor physiotherapy, loperamide | Sphincter-preserving surgery |
| Post-appendicectomy abscess | 2-5% | Percutaneous drainage + antibiotics | Adequate source control |
6 — Complex Cases and Advanced Integration
High Yield Summary
Key Take-Aways:
- Alvarado score ≥7 indicates high appendicitis probability; CT recommended for equivocal cases (score 5-6) to reduce negative appendicectomy rate to <5%
- Femoral hernias carry 15-20% strangulation risk and require urgent repair regardless of symptoms; inguinal hernias have 0.3% annual strangulation risk
- NICE NG151: FIT ≥10 μg Hb/g faeces or iron-deficiency anaemia mandates 2-week-wait colorectal cancer referral
- Colorectal cancer 5-year survival: Duke's A (95%), B (70-85%), C (45-65%), D (5-10%)
- Laparoscopic appendicectomy reduces wound infection (5% vs 10%) and accelerates recovery compared to open approach
- Stage III colon cancer requires adjuvant FOLFOX chemotherapy for 6 months post-resection
- Strangulated hernia without cough impulse requires emergency surgery within 6 hours to prevent bowel necrosis
Essential General Surgery Numbers:
| Parameter | Value | Clinical Significance |
|---|---|---|
| Appendix diameter (abnormal) | >6mm | CT diagnostic threshold |
| Appendicitis perforation risk | 20% at 24h, 65% at 48h | Justifies early intervention |
| Femoral hernia strangulation risk | 15-20% | Urgent repair mandatory |
| FIT threshold (2WW referral) | ≥10 μg Hb/g | NICE NG151 criterion |
| Colorectal anastomotic leak | 5-10% | Major complication requiring vigilance |
| Adenoma-carcinoma progression | 10-15 years | Screening opportunity |
Key Principles:
- Absence of cough impulse in hernia examination indicates strangulation until proven otherwise-surgical emergency
- Right iliac fossa pain in women of reproductive age requires β-hCG to exclude ectopic pregnancy before considering appendicitis
- Iron-deficiency anaemia in patients >50 years is colorectal cancer until proven otherwise
- Rectal cancer requires MRI pelvis for staging (assesses mesorectal fascia) unlike colon cancer
- Conservative appendicitis management acceptable in selected uncomplicated cases but carries 20-30% recurrence at 1 year
Quick Reference:
| Clinical Scenario | Immediate Action | Key Investigation | Definitive Management |
|---|---|---|---|
| RIF pain + peritonism | IV access, analgesia, NBM | CT abdomen (adults) | Laparoscopic appendicectomy |
| Irreducible tender hernia | Emergency surgical referral | Clinical diagnosis | Emergency repair ± bowel resection |
| Altered bowel habit + anaemia | 2-week-wait referral | Colonoscopy + biopsy | Surgical resection ± chemotherapy |
| Palpable rectal mass | DRE, urgent referral | MRI pelvis + staging CT | Neoadjuvant CRT + TME |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app






