Quick Overview
COPD is a progressive obstructive airway disease diagnosed by post-bronchodilator spirometry showing FEV1/FVC <0.7. Management focuses on symptom control, exacerbation prevention, and timely escalation during acute deteriorations. NICE NG115 emphasizes individualized inhaler therapy based on exacerbation frequency and blood eosinophil counts.
Core Facts & Concepts
Diagnostic Criteria (NICE NG115)
- Spirometry: Post-bronchodilator FEV1/FVC <0.7 confirms airflow obstruction
- Perform in stable state (≥6 weeks post-exacerbation)
- FEV1 % predicted determines severity but doesn't guide treatment alone
MRC Dyspnoea Scale (guides treatment escalation)
| Grade | Description |
|---|---|
| 1 | Breathless on strenuous exercise only |
| 2 | Breathless on walking uphill |
| 3 | Stops for breath after ~100m on level ground |
| 4 | Too breathless to leave house |
| 5 | Breathless dressing/undressing |
Severity Classification by FEV1
- Stage 1 (Mild): ≥80% predicted
- Stage 2 (Moderate): 50-79% predicted
- Stage 3 (Severe): 30-49% predicted
- Stage 4 (Very severe): <30% predicted
📊 Key Thresholds
- Eosinophil count ≥300 cells/μL: Consider ICS addition
- ≥2 exacerbations/year: Escalate therapy
- pH <7.35: Consider NIV in type 2 respiratory failure
Problem-Solving Approach
Acute Exacerbation Management (Stepwise)
- Assess severity: Respiratory rate, oxygen saturations, ability to speak, consciousness level
- Oxygen therapy: Target SpO2 88-92% (controlled oxygen to avoid CO2 retention)
- Bronchodilators: Nebulized salbutamol 5mg + ipratropium 500mcg QDS
- Corticosteroids: Prednisolone 30mg daily for 5 days (all exacerbations requiring hospital treatment)
- Antibiotics if ≥2 of: ↑dyspnoea, ↑sputum volume, purulent sputum (Anthonisen criteria)
- First-line: amoxicillin 500mg TDS or doxycycline 200mg loading then 100mg daily (5 days)
🚩 NIV Criteria (pH-driven)
- pH 7.25-7.35 with pCO2 >6.5 kPa despite optimal medical therapy
- pH <7.25: Consider ICU/intubation
- Contraindications: Impaired consciousness, facial trauma, vomiting
Inhaler Escalation Algorithm (NICE NG115)
- No asthmatic features: LABA+LAMA dual therapy
- Asthmatic features + eosinophils ≥300: LABA+LAMA+ICS triple therapy
- Frequent exacerbations (≥2/year) on LABA+LAMA: Add ICS if eosinophils ≥100
Analysis Framework
Differentiating Exacerbation Triggers
| Feature | Infective | Cardiac | PE |
|---|---|---|---|
| Sputum | Purulent, ↑volume | Frothy/pink | Normal |
| Fever | Common | Rare | Low-grade |
| JVP | Normal | ↑↑ | May be ↑ |
| Leg oedema | Absent | Bilateral | Unilateral DVT |
| BNP | Normal | ↑↑↑ | Variable |
Asthmatic Features Suggesting ICS Benefit
- Previous asthma/atopy diagnosis
- Diurnal/day-to-day variability
- Eosinophils ≥300 cells/μL
- FeNO ≥40 ppb (if available)
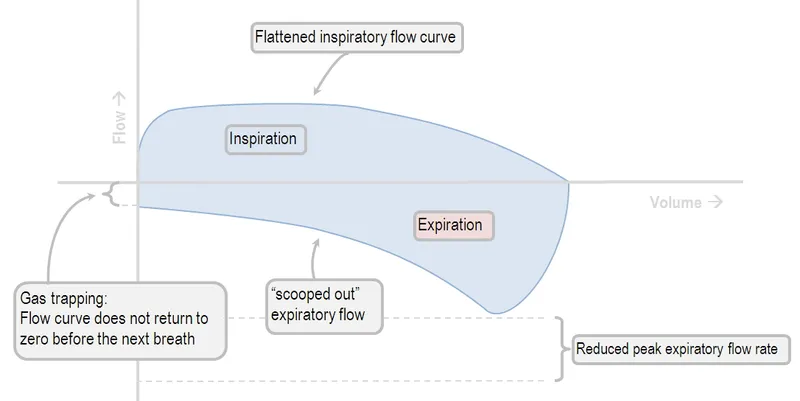
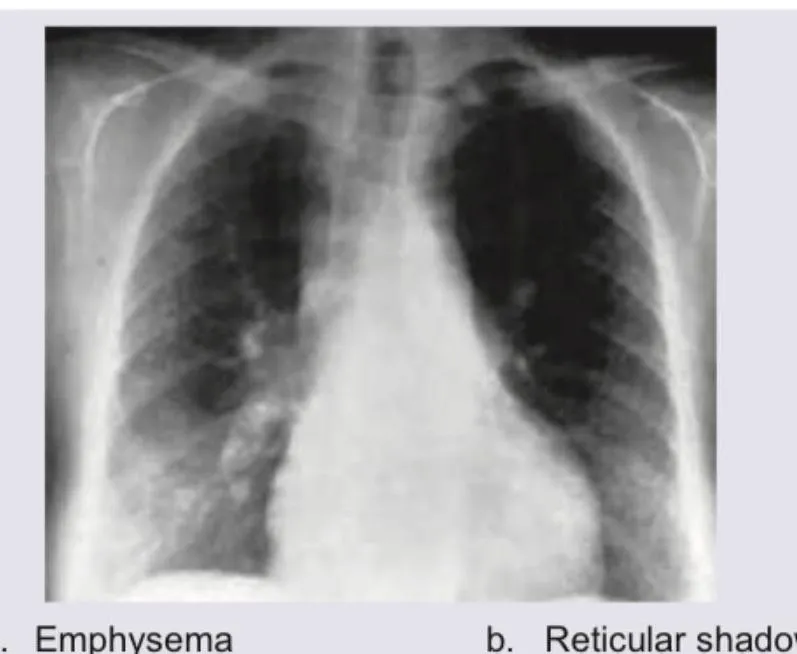
Visual Aid
Anthonisen Criteria for Antibiotics
- Increased dyspnoea
- Increased sputum volume
- Purulent sputum (most specific)
Key Points Summary
✓ Diagnosis: Post-bronchodilator FEV1/FVC <0.7 on spirometry (perform when stable)
✓ Exacerbation antibiotics: Only if ≥2 Anthonisen criteria (↑dyspnoea, ↑sputum volume, purulent sputum)
✓ Oxygen target: 88-92% SpO2 to prevent hypercapnia in acute setting
✓ NIV threshold: pH 7.25-7.35 with pCO2 >6.5 kPa despite maximal medical therapy
✓ Inhaler escalation: LABA+LAMA baseline; add ICS if eosinophils ≥300 cells/μL or ≥100 with frequent exacerbations
✓ Steroids: Prednisolone 30mg for 5 days in all hospitalized exacerbations
✓ MRC grade ≥3: Significant functional impairment-consider pulmonary rehabilitation referral
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

