Quick Overview
Acute severe asthma is a life-threatening emergency requiring immediate recognition and treatment. Misclassification of severity or delayed intervention significantly increases morbidity and mortality. NICE NG80 emphasizes structured assessment using objective criteria (PEF, oxygen saturation, respiratory rate) and escalating therapy based on severity markers.
Core Facts & Concepts
Severity Classification (NICE NG80)
| Severity | PEF | SpO₂ | Clinical Features |
|---|---|---|---|
| Moderate | >50-75% best/predicted | ≥92% | Increasing symptoms, no severe features |
| Acute Severe | 33-50% best/predicted | ≥92% | RR ≥25/min, HR ≥110/min, inability to complete sentences |
| Life-Threatening | <33% best/predicted | <92% | Silent chest, cyanosis, exhaustion, arrhythmia, hypotension, altered consciousness |
| Near-Fatal | Any severity | Any | Raised PaCO₂ and/or requiring mechanical ventilation |
📊 Critical Thresholds
- PEF <33% = life-threatening
- SpO₂ <92% = life-threatening
- Normal PaCO₂ (4.6-6.0 kPa) in acute asthma = exhaustion warning (should be low due to hyperventilation)
- RR ≥25/min or HR ≥110/min = acute severe
Problem-Solving Approach
Immediate Management Algorithm (NICE NG80)
- Oxygen therapy: Target SpO₂ 94-98% via high-flow or reservoir mask
- Bronchodilators (within 15 minutes):
- Salbutamol 5mg nebulized (back-to-back if life-threatening)
- Ipratropium bromide 0.5mg nebulized (add in acute severe/life-threatening)
- Steroids (within 1 hour):
- Prednisolone 40-50mg PO OR hydrocortisone 100mg IV
- Continue 5-7 days (no taper needed)
- Magnesium sulfate 2g IV over 20 minutes if:
- Life-threatening features OR
- Acute severe not responding to initial bronchodilators
🚩 Red Flags for ICU Referral
- Deteriorating PEF despite treatment
- Persisting/worsening hypoxia (SpO₂ <92%)
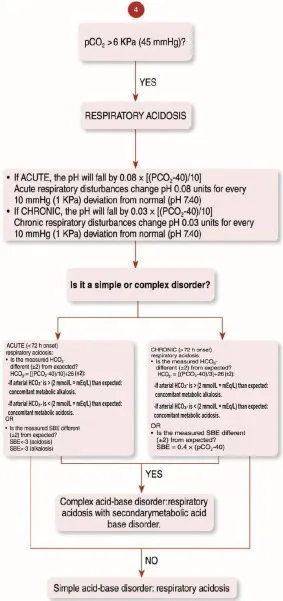
- Hypercapnia (PaCO₂ >6.0 kPa)
- Exhaustion, drowsiness, altered consciousness
- Respiratory arrest
Analysis Framework
Decision Points for Escalation
Key Discriminators: Severe vs Life-Threatening
| Feature | Acute Severe | Life-Threatening |
|---|---|---|
| Can speak | In words | Unable/monosyllabic |
| Chest sounds | Wheeze present | Silent chest |
| Conscious level | Agitated | Confused/drowsy |
| PaCO₂ | Low (hyperventilation) | Normal or high |
Key Points Summary
✓ PEF <33% or SpO₂ <92% = life-threatening asthma requiring immediate full treatment
✓ Normal PaCO₂ in acute asthma = near-fatal (should be hypocapnic from hyperventilation)
✓ First-line treatment: Oxygen (target 94-98%) + salbutamol 5mg nebulized + prednisolone 40-50mg
✓ Magnesium sulfate 2g IV for life-threatening or poor response to initial bronchodilators (within 1 hour)
✓ Add ipratropium 0.5mg to nebulizers in acute severe/life-threatening cases
✓ ICU referral criteria: Deteriorating PEF, hypercapnia (PaCO₂ >6.0 kPa), exhaustion, altered consciousness
✓ Silent chest = life-threatening (insufficient airflow to generate wheeze), NOT improvement
⚠️ Warning: Patients can deteriorate rapidly despite initial response-continuous monitoring essential for first 24 hours
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

