Renal & Urology

On this page
Foundations of Renal and Urological Medicine
A 68-year-old man presents to the Emergency Department with confusion and reduced urine output over 48 hours. His creatinine has risen from a baseline of 95 μmol/L to 280 μmol/L. This scenario exemplifies the critical importance of recognizing , which affects 15-20% of hospital admissions and carries a mortality rate of 20-50% in severe cases. Understanding the classification systems for renal disease-from acute insults to progressive -forms the foundation for effective clinical practice. The spectrum of renal and urological conditions extends from common presentations like , affecting 150 million people globally each year, to life-threatening complications requiring immediate intervention.
Key Classification Systems:
-
AKI staging (KDIGO criteria):
- Stage 1: Creatinine rise ≥26 μmol/L within 48h OR 1.5-1.9× baseline; urine output <0.5 mL/kg/h for 6-12h
- Stage 2: Creatinine 2.0-2.9× baseline; urine output <0.5 mL/kg/h for ≥12h
- Stage 3: Creatinine ≥354 μmol/L OR ≥3× baseline OR requiring RRT; urine output <0.3 mL/kg/h for ≥24h
-
CKD staging combines eGFR and albuminuria:
- G1-G5 (eGFR ≥90, 60-89, 45-59, 30-44, 15-29, <15 mL/min/1.73m²)
- A1-A3 (ACR <3, 3-30, >30 mg/mmol)
| Classification | Definition | Clinical Significance |
|---|---|---|
| AKI Stage 1 | Cr ↑26 μmol/L or 1.5× baseline | 2-fold mortality increase |
| CKD G3a | eGFR 45-59 | Annual monitoring adequate |
| CKD G4 | eGFR 15-29 | Nephrology referral mandatory |
| Complicated UTI | Structural abnormality/immunocompromise | Extended antibiotic course needed |
📌 Mnemonic for AKI causes: "STOP MEDS" - Sepsis, Toxins (NSAIDs, gentamicin), Obstruction, Perfusion (hypotension), Myeloma/Myoglobin, Emboli, Drugs, Stones
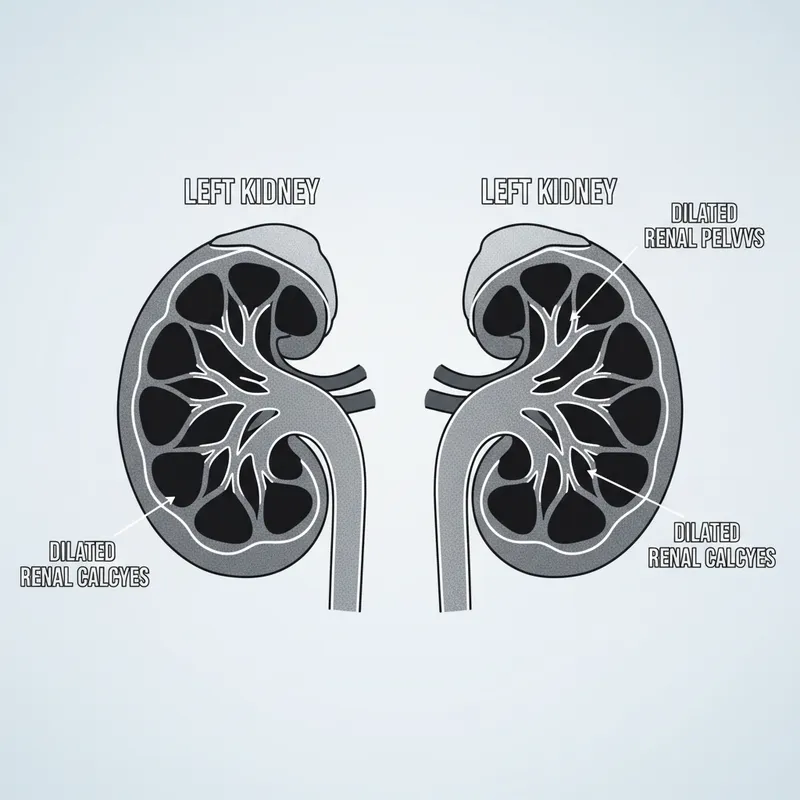
Foundations of Renal and Urological Medicine
2 - Pathophysiological Mechanisms in Renal Dysfunction
The pathophysiology of involves three primary mechanisms: pre-renal (hypoperfusion reducing GFR by 60-70%), intrinsic renal (tubular necrosis, glomerulonephritis), and post-renal (obstruction causing backpressure). In pre-renal AKI, the renin-angiotensin-aldosterone system activates within minutes, attempting to preserve GFR through efferent arteriolar constriction. However, when mean arterial pressure falls below the autoregulatory threshold of 80 mmHg, GFR declines precipitously. frequently complicate AKI, with hyperkalaemia developing when tubular secretion fails and potassium rises >0.5 mmol/L/day. The pathogenesis of involves crystal formation (calcium oxalate 75%, uric acid 10%, struvite 10%) causing ureteric spasm and intense pain radiating from loin to groin.
Mechanistic Pathways:
-
Pre-renal azotaemia:
- Activation of RAAS → efferent vasoconstriction → maintains GFR initially
- Urea reabsorption increases → urea:creatinine ratio >100:1
- FeNa <1% indicates avid sodium retention (tubules intact)
-
Acute tubular necrosis:
- Ischaemic injury → loss of brush border → tubular cell death within 24-36h
- Cast formation obstructs tubules → FeNa >2% (tubular dysfunction)
- Recovery phase: polyuria as tubules regenerate but concentrating ability impaired
-
Hyperkalaemia mechanisms:
- Reduced K⁺ secretion in distal tubule (principal cells)
- Acidosis causes K⁺ shift from ICF to ECF (0.6 mmol/L per 0.1 pH drop)
- Risk of cardiac arrhythmia when K⁺ >6.5 mmol/L
2 — Pathophysiological Mechanisms in Renal Dysfunction
3 - Diagnostic Approaches and Investigation Strategies
A 45-year-old woman presents with dysuria, frequency, and suprapubic pain. Dipstick shows nitrites positive and leucocytes 3+. This straightforward presentation of contrasts sharply with the diagnostic challenge of unexplained AKI, where systematic investigation must distinguish between pre-renal, intrinsic, and post-renal causes. The diagnostic sequence begins with bedside tests (urine output monitoring, dipstick), progresses through blood tests (creatinine, urea, electrolytes, venous gas), and culminates in imaging when obstruction is suspected. For , non-contrast CT KUB has 95-98% sensitivity for stones >3 mm, far exceeding ultrasound (45% sensitivity). require interpretation in clinical context: a sodium of 128 mmol/L may be asymptomatic chronic hyponatraemia or acute symptomatic requiring urgent correction.
Investigation Hierarchy:
-
First-line (all suspected renal presentations):
- Urinalysis: nitrites (specificity 98% for UTI), protein (ACR >70 suggests glomerular disease)
- U&Es: urea:creatinine ratio >100:1 suggests pre-renal; <40:1 suggests intrinsic disease
- Venous gas: K⁺, pH, bicarbonate (metabolic acidosis if HCO₃⁻ <22 mmol/L)
-
Second-line (guided by clinical suspicion):
- Renal ultrasound: hydronephrosis (post-renal), cortical thickness (CKD), echogenicity
- Urine microscopy: RBC casts (glomerulonephritis), WBC casts (pyelonephritis)
- FeNa calculation: [(UNa × PCr)/(PNa × UCr)] × 100 - <1% pre-renal, >2% ATN
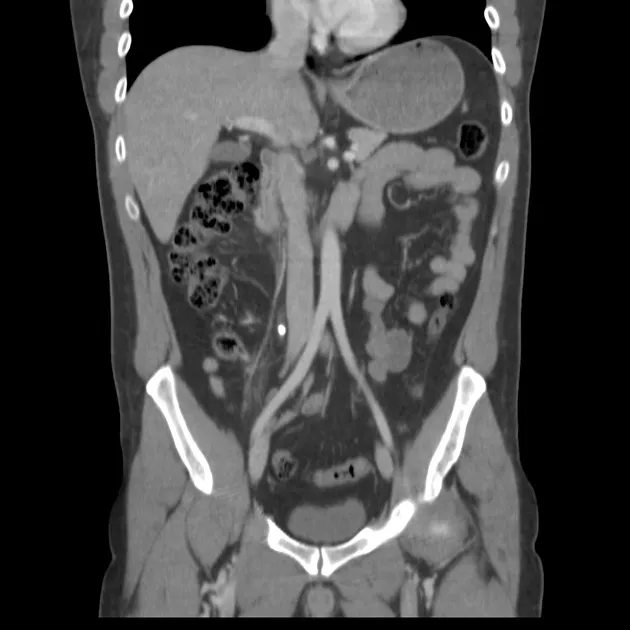
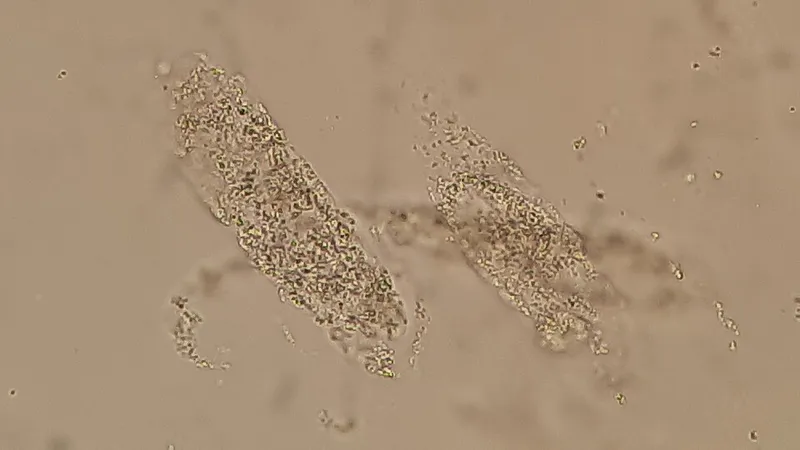
| Investigation | Sensitivity | Specificity | Clinical Application |
|---|---|---|---|
| Urine nitrites | 45-60% | 98% | High PPV for UTI if positive |
| CT KUB (stones >5mm) | 98% | 100% | Gold standard for renal colic |
| USS (hydronephrosis) | 90% | 95% | First-line for suspected obstruction |
| FeNa <1% | 85% | 80% | Distinguishes pre-renal from ATN |
3 — Diagnostic Approaches and Investigation Strategies
4 - Differential Diagnosis and Clinical Reasoning
Distinguishing between and acute-on-chronic kidney disease requires knowledge of baseline function-a creatinine of 180 μmol/L may represent AKI in a young person or stable in an elderly diabetic. The clinical context provides crucial discriminators: sudden onset over hours suggests AKI, whereas months of fatigue and anaemia point to CKD. Small kidneys on ultrasound (<9 cm) virtually confirm chronicity, while normal-sized kidneys in AKI suggest reversibility. Urea:creatinine ratio helps differentiate causes: >100:1 indicates pre-renal pathology (avid urea reabsorption), while ratios <40:1 suggest intrinsic renal disease where tubular function is impaired.
Key Discriminating Features:
-
AKI versus CKD:
- Anaemia (Hb <100 g/L) + hypocalcaemia + hyperphosphataemia = CKD
- Previous creatinine results: review 3-12 months prior
- Renal size: bilateral <9 cm indicates chronicity (except diabetic nephropathy, amyloid)
- Nocturia and polyuria suggest CKD (loss of concentrating ability)
-
Pre-renal versus intrinsic AKI:
- Response to 500 mL fluid bolus: creatinine improvement suggests pre-renal
- Urine osmolality: >500 mOsm/kg = pre-renal; <350 mOsm/kg = ATN
- Urine sodium: <20 mmol/L = pre-renal; >40 mmol/L = intrinsic
-
Complicated versus uncomplicated UTI:
- Systemic features (fever >38°C, rigors) suggest pyelonephritis
- Structural abnormality, immunosuppression, pregnancy = complicated
- Male sex always classified as complicated UTI
| Feature | Pre-renal AKI | Intrinsic AKI (ATN) | Post-renal AKI |
|---|---|---|---|
| Urine output | Variable | Oliguric | Anuria or polyuria |
| FeNa | <1% | >2% | Variable |
| Response to fluids | Rapid improvement | Minimal | None |
| USS findings | Normal | Normal/increased echogenicity | Hydronephrosis |
4 — Differential Diagnosis and Clinical Reasoning
5 - Evidence-Based Management and Treatment Optimization
NICE NG148 emphasizes that management focuses on slowing progression through BP control (target <120/90 mmHg if ACR >70 mg/mmol) and RAAS inhibition. Ramipril 10 mg once daily or losartan 100 mg once daily reduces proteinuria by 30-40% and slows eGFR decline by 2-3 mL/min/year. For , hyperkalaemia >6.5 mmol/L with ECG changes requires immediate treatment: 10 mL 10% calcium gluconate IV (cardiac protection), 10 units actrapid insulin with 50 mL 50% glucose (shifts K⁺ intracellularly within 15 minutes), and 10-20 mg salbutamol nebulized (lowers K⁺ by 0.5-1.0 mmol/L). treatment follows NICE NG109: nitrofurantoin 100 mg BD for 3 days (uncomplicated lower UTI), or co-amoxiclav 500/125 mg TDS for 7-10 days (pyelonephritis after culture).
Specific Treatment Protocols:
-
AKI supportive care:
- Stop nephrotoxins: NSAIDs, ACE-I/ARBs, gentamicin, metformin
- Fluid balance: aim euvolaemia (CVP 8-12 mmHg if monitored)
- RRT indications: K⁺ >7 mmol/L refractory, pH <7.15, pulmonary oedema, uraemic pericarditis
-
CKD progression prevention:
- ACE-I/ARB: start if ACR >3 mg/mmol, titrate to max tolerated dose
- SGLT2 inhibitor: dapagliflozin 10 mg OD if eGFR >25 (DAPA-CKD trial: 39% RRR)
- Sodium bicarbonate: if HCO₃⁻ <22 mmol/L, give 500 mg TDS to slow progression
-
Hyperkalaemia management sequence:
- 10 mL 10% calcium gluconate IV over 5 minutes (repeat if ECG changes persist)
- 10 units actrapid + 50 mL 50% glucose IV (check BM hourly × 4)
- Calcium resonium 15 g TDS PO (delayed effect, 6-24h)
| Drug | Dose | Onset | Duration | Monitoring |
|---|---|---|---|---|
| Calcium gluconate 10% | 10 mL IV | 1-3 min | 30-60 min | Continuous ECG |
| Actrapid + glucose | 10 U + 50 mL 50% | 15 min | 4-6 h | BM hourly × 4 |
| Salbutamol nebulizer | 10-20 mg | 30 min | 2-4 h | HR, tremor |
| Ramipril (CKD) | 10 mg OD | Days-weeks | Ongoing | U&Es at 1-2 weeks |
5 — Evidence-Based Management and Treatment Optimization
6 - Complex Cases and Long-Term Management
A 72-year-old with G4 (eGFR 22 mL/min), heart failure, and diabetes presents with Stage 2 following a UTI. This exemplifies the challenge of balancing competing risks: continuing ACE inhibitors risks worsening AKI, but stopping them may precipitate heart failure decompensation. NICE CG182 recommends temporarily withholding RAAS inhibitors during acute illness, restarting once creatinine returns to within 20% of baseline. in pregnancy requires careful imaging choices-ultrasound first-line, MRI if inconclusive, avoiding CT radiation exposure. Long-term CKD monitoring includes annual ACR, eGFR every 6 months (G3a-b) or 3 months (G4-5), and bone profile screening (PTH, calcium, phosphate) when eGFR <45 mL/min.
Special Population Considerations:
-
Elderly with multimorbidity:
- Adjust drug doses for eGFR: metformin contraindicated <30, DOACs dose-reduce <50
- Consider frailty: conservative management may be appropriate over RRT
- Polypharmacy review: stop nephrotoxins, adjust for renal function
-
Pregnancy-related considerations:
- Physiological GFR increase: creatinine >75 μmol/L abnormal in pregnancy
- Asymptomatic bacteriuria: treat (7-day nitrofurantoin) to prevent pyelonephritis
- Avoid ACE-I/ARBs (teratogenic), NSAIDs >32 weeks (premature ductus closure)
-
CKD complications requiring intervention:
- Renal anaemia: start erythropoietin if Hb <100 g/L despite iron repletion (ferritin >200 μg/L)
- Secondary hyperparathyroidism: start alfacalcidol if PTH >2× upper limit
- Metabolic acidosis: target HCO₃⁻ >22 mmol/L with sodium bicarbonate
| CKD Stage | eGFR | Monitoring Frequency | Referral Threshold |
|---|---|---|---|
| G3a | 45-59 | Annually | ACR >70 or progressive decline |
| G3b | 30-44 | 6-monthly | ACR >30 or decline >5 mL/min/year |
| G4 | 15-29 | 3-monthly | All patients for RRT planning |
| G5 | <15 | Monthly | Urgent nephrology input |
6 — Complex Cases and Long-Term Management
High Yield Summary
Key Take-Aways:
- AKI defined by creatinine rise ≥26 μmol/L in 48h or 1.5× baseline; Stage 3 has 50% mortality
- FeNa <1% indicates pre-renal AKI (tubules intact); >2% suggests intrinsic ATN
- Hyperkalaemia >6.5 mmol/L with ECG changes requires immediate calcium gluconate + insulin/glucose
- CKD progression slowed by ACE-I/ARB (titrate to max dose) + SGLT2 inhibitor (39% RRR in DAPA-CKD)
- Uncomplicated UTI: nitrofurantoin 100 mg BD × 3 days; pyelonephritis: co-amoxiclav 500/125 TDS × 7-10 days
- Renal colic: non-contrast CT KUB gold standard (98% sensitivity); stones <5 mm pass spontaneously 90% of cases
- Small kidneys (<9 cm bilateral) confirm CKD chronicity; normal size in AKI suggests reversibility
Essential Renal & Urology Numbers/Formulas:
| Parameter | Value | Clinical Significance |
|---|---|---|
| AKI Stage 1 threshold | Cr ↑26 μmol/L or 1.5× baseline | 2× mortality risk |
| Hyperkalaemia emergency | K⁺ >6.5 mmol/L | Cardiac arrest risk |
| CKD nephrology referral | eGFR <30 or ACR >70 | Plan RRT/transplant |
| FeNa formula | [(UNa×PCr)/(PNa×UCr)]×100 | <1% pre-renal, >2% ATN |
| Urea:creatinine ratio | >100:1 | Pre-renal azotaemia |
Key Principles/Pearls:
- Always review previous creatinine-"acute" may be acute-on-chronic requiring different management approach
- Stop "DAMN" drugs in AKI: Diuretics, ACE-I/ARBs, Metformin, NSAIDs-restart cautiously when stable
- Bladder scan mandatory in anuria before declaring intrinsic AKI-post-renal obstruction is immediately reversible
- Nitrofurantoin ineffective if eGFR <45 mL/min (inadequate urinary concentration)-use alternative for UTI
Quick Reference:
| Condition | Key Diagnostic | Immediate Action | Target/Endpoint |
|---|---|---|---|
| AKI Stage 3 | Cr ≥354 or 3× baseline | Stop nephrotoxins, fluid balance | Urine output >0.5 mL/kg/h |
| Hyperkalaemia | K⁺ >6.5 + ECG changes | Ca gluconate + insulin/glucose | K⁺ <6.0 mmol/L |
| Pyelonephritis | Fever + loin pain + pyuria | Blood cultures, IV antibiotics | Apyrexial 48h |
| Renal colic | CT stone + hydronephrosis | Analgesia, antiemetic, α-blocker | Stone passage or intervention |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app










