Quick Overview
Headache is one of the most common presentations in primary and secondary care. This chapter focuses on migraine (primary headache disorder affecting ~15% of UK population) and red flag features requiring urgent investigation to exclude secondary causes (subarachnoid haemorrhage, temporal arteritis, raised ICP). NICE CG150 provides evidence-based guidance on diagnosis, acute management, and prophylaxis strategies essential for safe practice.
Core Facts & Concepts
🚩 Red Flags (SNOOP4):
- Systemic symptoms (fever, weight loss, immunosuppression)
- Neurological signs/symptoms (focal deficit, seizure, altered consciousness)
- Onset sudden/thunderclap (<1 minute to peak = SAH until proven otherwise)
- Older age (new onset >50 years = consider temporal arteritis)
- Pattern change (frequency, severity, character)
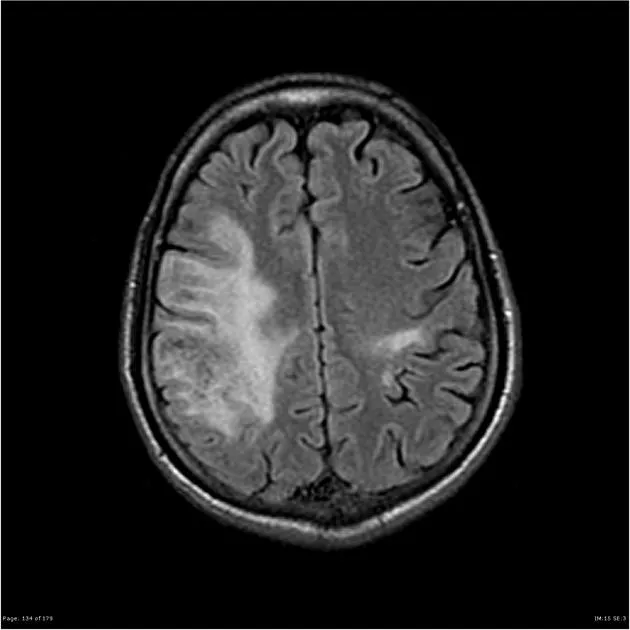
- Positional (worse lying down = ↑ICP; worse standing = ↓CSF pressure)
- Precipitated by Valsalva (cough, sneeze = space-occupying lesion)
- Papilloedema or pregnancy
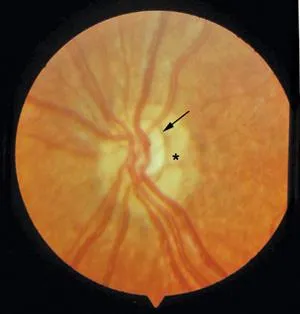
Migraine Diagnostic Criteria (≥5 attacks):
- Headache lasting 4-72 hours (untreated)
- ≥2 of: unilateral, pulsating, moderate-severe intensity, aggravated by routine activity
- ≥1 of: nausea/vomiting, photophobia + phonophobia
- Aura: reversible visual/sensory/speech symptoms developing over 5-60 minutes
Medication Overuse Headache (MOH):
- Headache ≥15 days/month in patient with pre-existing headache disorder
- Regular overuse for >3 months: triptans/opioids/combination analgesics ≥10 days/month OR simple analgesics ≥15 days/month
Problem-Solving Approach
Acute Migraine Management Ladder (NICE CG150):
- First-line: Oral triptan (e.g., sumatriptan 50-100mg) + NSAID (ibuprofen 400-600mg) OR triptan + paracetamol 1g
- If vomiting/rapid relief needed: Consider nasal/SC triptan or antiemetic (metoclopramide 10mg)
- Contraindications to triptans: Uncontrolled HTN, IHD, previous stroke, hemiplegic migraine
- Avoid: Opioids (risk of MOH) and ergots (inferior efficacy)
Prophylaxis Indications (offer if ≥2 attacks/month impacting QoL):
| First-line | Dose/Duration | Key Points |
|---|---|---|
| Topiramate | 25mg titrate to 50-100mg BD | ⚠️ Teratogenic - contraception essential |
| Propranolol | 80-240mg daily | CI: asthma, heart block |
| Amitriptyline | 10mg titrate to 75mg nocte | Useful if comorbid insomnia/pain |
- Trial each for 3 months before switching
- Botulinum toxin A: Specialist option for chronic migraine (≥15 headache days/month)
Analysis Framework
Differentiating Primary vs Secondary Headaches:
| Feature | Migraine | Tension-type | Cluster | ⚠️ Secondary |
|---|---|---|---|---|
| Duration | 4-72h | 30min-7 days | 15-180min | Variable |
| Quality | Pulsating | Pressing/tight | Severe boring | Depends on cause |
| Location | Unilateral | Bilateral | Unilateral (periorbital) | Any |
| Associated | N/V, photo/phonophobia | Mild photo/phonophobia | Lacrimation, rhinorrhoea, ptosis | Red flags present |
| Activity | Worsens | No change | Restless/agitated | Variable |
⭐ Clinical Pearl: Cluster headache occurs in circadian patterns (same time daily, often waking from sleep). Male predominance 3:1.
Visual Aid
MOH Management Protocol:
- Abruptly stop overused medication (no evidence for gradual withdrawal)
- Warn: headache may worsen initially for 2-4 weeks before improvement
- Offer prophylaxis after withdrawal period
- Follow-up at 4-8 weeks
Key Points Summary
✓ Red flags (SNOOP4) mandate urgent investigation - thunderclap headache = SAH until proven otherwise
✓ Acute migraine: Triptan + NSAID/paracetamol first-line (avoid opioids)
✓ MOH criteria: Headache ≥15 days/month + overuse >3 months (triptans ≥10 days/month, simple analgesics ≥15 days/month)
✓ Prophylaxis if ≥2 attacks/month: topiramate/propranolol/amitriptyline for 3-month trial each
✓ Topiramate is teratogenic - ensure effective contraception in women of childbearing age
✓ Cluster headache triad: Unilateral periorbital pain + autonomic features + circadian pattern (15-180 min duration)
✓ New headache >50 years = temporal arteritis until proven otherwise (check ESR/CRP urgently)
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

