Quick Overview
Inflammatory bowel disease (IBD) comprises Crohn's disease (CD) and ulcerative colitis (UC), chronic relapsing-remitting inflammatory conditions affecting the GI tract. NICE NG129 provides evidence-based guidance on inducing/maintaining remission, biologics use, and monitoring complications. Key focus: distinguishing CD vs UC, escalating therapy appropriately, and surveillance for strictures, fistulae, and malignancy risk.
Core Facts & Concepts
Key Distinctions:
| Feature | Crohn's Disease | Ulcerative Colitis |
|---|---|---|
| Location | Mouth to anus (skip lesions) | Colon only (continuous) |
| Depth | Transmural | Mucosa/submucosa only |
| Smoking | Worsens disease | Protective (paradoxically) |
| Fistulae/strictures | Common | Rare |
| Malignancy risk | Moderate | Higher (↑ with extent/duration) |

Disease Activity Indices:
- UC: Truelove-Witts severity (mild <4 stools/day, severe ≥6 + systemic toxicity)
- CD: Harvey-Bradshaw Index (clinical score without endoscopy)
📊 Critical Numbers:
- Malignancy surveillance colonoscopy: Start at 10 years post-diagnosis for extensive colitis
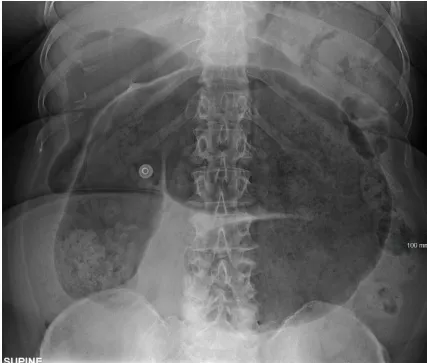
- Toxic megacolon: Colon diameter >6cm on AXR
- Thiopurine metabolites: Target 6-TGN 235-450 pmol/8×10⁸ RBC
Problem-Solving Approach
Inducing Remission (NICE NG129):
- Mild-moderate UC: Topical (rectal) aminosalicylate (5-ASA) ± oral 5-ASA
- Moderate-severe UC: IV corticosteroids (hydrocortisone 100mg QDS)
- If no response in 72 hours → consider rescue therapy (infliximab or ciclosporin) or colectomy
- Mild-moderate CD: Consider exclusive enteral nutrition (first-line in children) or oral prednisolone
- Moderate-severe CD: Corticosteroids ± add azathioprine for maintenance
Maintaining Remission:
- UC: Oral/rectal 5-ASA (not steroids long-term)
- CD: Azathioprine/mercaptopurine or methotrexate (steroids NOT for maintenance)
🚩 Red Flags for Biologics (Anti-TNF):
- Disease refractory to conventional therapy
- ≥2 acute severe UC flares in 12 months
- Steroid-dependent disease
- Perianal fistulising CD
⚠️ Warning: Screen for latent TB (CXR + IGRA) before starting anti-TNF therapy
Analysis Framework
Surgical Indications:
| Indication | Crohn's Disease | Ulcerative Colitis |
|---|---|---|
| Emergency | Perforation, obstruction, toxic megacolon | Toxic megacolon, perforation, haemorrhage |
| Elective | Strictures, fistulae, abscess | Failed medical therapy, dysplasia/cancer |
| Surgery type | Resection (recurrence common) | Colectomy (curative) |
Monitoring Complications:
- Strictures: MR enterography for small bowel (CD)
- Fistulae: MRI pelvis ± examination under anaesthesia
- Malignancy: Colonoscopy q1-2 years after 10 years (extensive disease)
- Nutritional: Check vitamin B12 (terminal ileum CD), vitamin D, iron
Visual Aid
Nutritional Support in CD:
- Exclusive enteral nutrition: Polymeric formula for 6-8 weeks (induces remission, especially paediatric)
- Parenteral nutrition if intestinal failure/short bowel post-resection
Key Points Summary
✓ UC affects colon only (continuous); CD affects any GI site (skip lesions, transmural)
✓ Acute severe UC: IV hydrocortisone → if no response at 72h consider infliximab/ciclosporin/colectomy
✓ Maintenance: 5-ASA for UC; thiopurines/methotrexate for CD (NEVER long-term steroids)
✓ Biologics (anti-TNF): For steroid-dependent, refractory disease, or fistulising CD; screen for TB first
✓ Surveillance colonoscopy: Start at 10 years post-diagnosis for extensive colitis; q1-2 years thereafter
✓ Toxic megacolon: Colon >6cm on AXR; medical emergency requiring urgent surgical review
✓ Exclusive enteral nutrition: First-line for inducing remission in paediatric CD
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

