Quick Overview
Acute pancreatitis is pancreatic inflammation causing severe abdominal pain with raised amylase/lipase (>3× upper limit). Gallstones (40%) and alcohol (30%) account for 70% of cases. NICE NG104 emphasizes early severity assessment, aggressive fluid resuscitation, early enteral nutrition, and timely ERCP for gallstone pancreatitis. Mortality ranges from <1% (mild) to 30% (severe necrotizing).
Core Facts & Concepts
Diagnosis (requires ≥2 of 3):
- Characteristic abdominal pain (epigastric, radiating to back)
- Serum lipase/amylase >3× upper limit of normal (lipase more specific)
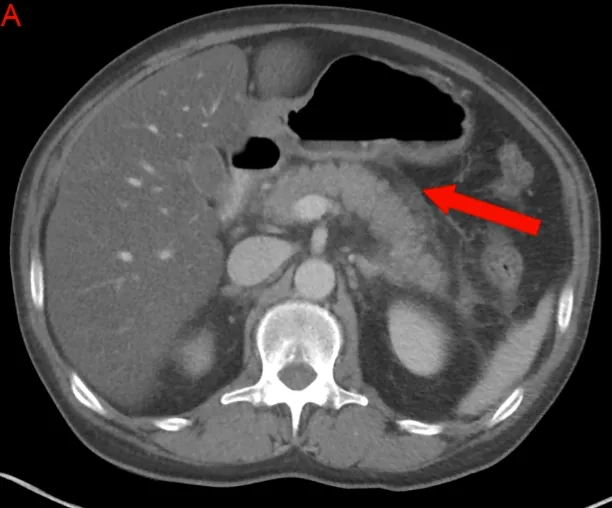
- Characteristic imaging findings (CT/MRI/USS)
Severity Assessment (NICE NG104):
- Glasgow score (≥3 = severe) or APACHE II within 24 hours
- CRP >150 mg/L at 48-72 hours predicts severe disease
- Persistent organ failure >48 hours = severe pancreatitis
| Glasgow Score (≥3 severe) | Values |
|---|---|
| PaO₂ | <8 kPa |
| Age | >55 years |
| Neutrophils | >15 × 10⁹/L |
| Calcium | <2 mmol/L |
| Renal (urea) | >16 mmol/L |
| Enzymes (LDH/AST) | LDH >600 IU/L, AST >200 IU/L |
| Albumin | <32 g/L |
| Sugar (glucose) | >10 mmol/L |
📌 Remember: PANCREAS - PaO₂, Age, Neutrophils, Calcium, Renal, Enzymes, Albumin, Sugar
Aetiology (I GET SMASHED):
- Idiopathic, Gallstones, Ethanol, Trauma, Steroids, Mumps/malignancy, Autoimmune, Scorpion venom, Hyperlipidaemia/Hypercalcaemia, ERCP, Drugs (azathioprine, sodium valproate)
Problem-Solving Approach
Initial Management (first 24 hours):
-
Fluid resuscitation (NICE NG104): Ringer's lactate preferred over 0.9% saline
- Target urine output ≥0.5 mL/kg/hour
- Aim for 2.5-4 L in first 24 hours (individualized)
-
Early enteral nutrition: Start within 72 hours via oral/NG route (reduces infection/mortality vs parenteral)
-
Analgesia: Opioids (morphine/fentanyl) appropriate; no evidence NSAIDs superior
-
ERCP timing for gallstone pancreatitis:
- Within 72 hours if concurrent cholangitis/biliary obstruction
- NOT routinely indicated for predicted mild gallstone pancreatitis without cholangitis
-
Antibiotics: NOT prophylactic; only for confirmed infected necrosis (FNA/clinical deterioration + gas on CT)

🚩 Red Flags:
- Persistent organ failure >48 hours (respiratory/renal/cardiovascular)
- Rising CRP after 48-72 hours
- Clinical deterioration after initial improvement (suspect infected necrosis)
Analysis Framework
Severity Stratification:
| Feature | Mild | Moderate | Severe |
|---|---|---|---|
| Organ failure | None | Transient (<48h) | Persistent (>48h) |
| Local complications | None | Sterile necrosis/collections | Infected necrosis |
| Mortality | <1% | ~3-5% | 20-30% |
| Hospital stay | 5-7 days | 7-14 days | Weeks-months |
Infected vs Sterile Necrosis:
- Clinical: fever, rising inflammatory markers after week 1
- CT signs: Gas bubbles within necrotic tissue (pathognomonic)
- Confirmation: FNA for culture (if intervention planned)
- Management: Antibiotics + delayed necrosectomy (≥4 weeks if stable)
Visual Aid
Key Investigations Timeline:
| Investigation | Timing | Purpose |
|---|---|---|
| Lipase/amylase | Admission | Diagnosis (>3× ULN) |
| USS abdomen | Within 24h | Identify gallstones |
| CRP | 48-72h | Severity prediction (>150 mg/L) |
| CT abdomen | Day 6-10 | Assess necrosis if severe/deteriorating |
Key Points Summary
✓ Diagnosis: ≥2 of pain + lipase >3× ULN + imaging; lipase more specific than amylase
✓ Severity: Glasgow ≥3 or persistent organ failure >48h = severe; CRP >150 mg/L at 48-72h predicts severity
✓ Fluids: Ringer's lactate preferred; target 2.5-4 L first 24h with urine output ≥0.5 mL/kg/h (NICE NG104)
✓ Nutrition: Early enteral feeding within 72h reduces complications; oral/NG preferred over parenteral
✓ ERCP: Only within 72h if gallstone pancreatitis + cholangitis/obstruction; NOT routine for mild cases
✓ Antibiotics: Only for confirmed infected necrosis (gas on CT/positive FNA); NO prophylactic use
✓ Gallstone pancreatitis: Cholecystectomy during same admission (or within 2 weeks) to prevent recurrence
⚠️ Warning: Persistent organ failure >48h defines severe pancreatitis regardless of other scores
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

