Quick Overview
Thyroid disorders are common endocrine conditions requiring precise TFT interpretation and evidence-based management. NICE NG145 emphasizes systematic approach to subclinical vs overt disease, appropriate levothyroxine dosing (1.6 mcg/kg ideal body weight), and recognition of thyroid storm. Mastery of TFT patterns and treatment thresholds is essential for safe prescribing and complication prevention.
Core Facts & Concepts
TFT Interpretation Thresholds:
| Condition | TSH | Free T4 | Free T3 |
|---|---|---|---|
| Overt hypothyroidism | ↑ (>10 mU/L) | ↓ (<12 pmol/L) | Normal/↓ |
| Subclinical hypothyroidism | ↑ (4.5-10 mU/L) | Normal | Normal |
| Overt hyperthyroidism | ↓ (<0.1 mU/L) | ↑ (>22 pmol/L) | ↑ |
| Subclinical hyperthyroidism | ↓ (<0.4 mU/L) | Normal | Normal |

Key Numbers:
- Levothyroxine dosing: 1.6 mcg/kg ideal body weight (typically 100-125 mcg daily in adults)
- Dose adjustment: 25-50 mcg increments every 6-8 weeks
- Target TSH: 0.5-2.5 mU/L (pregnancy: trimester-specific targets)
- Carbimazole starting dose: 15-40 mg daily (titration regimen) OR 40 mg daily (block-and-replace)
- Thyroid storm mortality: 20-30% despite treatment
Thyroid Storm Criteria (≥45 points):
- Temperature >38.5°C (5-30 points)
- HR >130 bpm (10-25 points)
- Heart failure present (15 points)
- CNS effects: agitation/delirium/psychosis/coma (10-30 points)
Autoantibodies:
- TPO antibodies: Hashimoto's thyroiditis (95%), Graves' disease (75%)
- TSH receptor antibodies (TRAb): Graves' disease (diagnostic, 90% sensitivity)
- Thyroglobulin antibodies: Hashimoto's thyroiditis
Problem-Solving Approach
Step 1: Confirm Diagnosis
- Repeat TFTs in 3 months for subclinical disease (exclude transient dysfunction)
- Check TPO/TRAb antibodies to determine etiology
- Thyroid ultrasound if nodules palpable or cancer suspected
Step 2: Decide Treatment Threshold
Hypothyroidism:
- Treat if: TSH >10 mU/L OR TSH 4.5-10 mU/L + symptoms/pregnancy/TPO+
- Levothyroxine: 1.6 mcg/kg IBW (reduce to 1.2 mcg/kg if >65 years or IHD)
- Check TFTs 6-8 weeks after initiation/dose change
Hyperthyroidism:
- Carbimazole regimens (NICE NG145):
- Titration: 15-40 mg daily, reduce by 5 mg every 4-6 weeks (12-18 months total)
- Block-and-replace: 40 mg carbimazole + 50-100 mcg levothyroxine (6 months)
- Propylthiouracil: Use in first trimester pregnancy (lower teratogenicity) or carbimazole allergy
Step 3: Monitor for Complications
🚩 Red Flags:
- Agranulocytosis (0.3% on carbimazole): Sore throat/fever → stop drug, urgent FBC
- Thyroid storm: ICU admission, propylthiouracil 600 mg loading + propranolol + hydrocortisone 100 mg QDS
- Atrial fibrillation: Present in 10-25% of hyperthyroidism (anticoagulate per CHA₂DS₂-VASc)
⚠️ Warning: Never start levothyroxine at full replacement dose in elderly/IHD patients-risk of MI. Start 25 mcg daily and titrate slowly.
Analysis Framework
Differential Diagnosis by TFT Pattern:
| TSH | T4 | T3 | Likely Diagnosis |
|---|---|---|---|
| High | Low | Low/N | Primary hypothyroidism |
| Low | Low | Low | Central hypothyroidism (check pituitary) |
| Low | High | High | Graves', toxic nodule, thyroiditis |
| Low | Normal | High | T3 toxicosis |
| High | High | High | TSH-secreting adenoma (rare), assay interference |
Discriminating Features: Causes of Hyperthyroidism
| Feature | Graves' Disease | Toxic Nodule | Thyroiditis |
|---|---|---|---|
| Onset | Gradual | Gradual | Acute/subacute |
| Goiter | Diffuse, smooth | Nodular | Tender (subacute) |
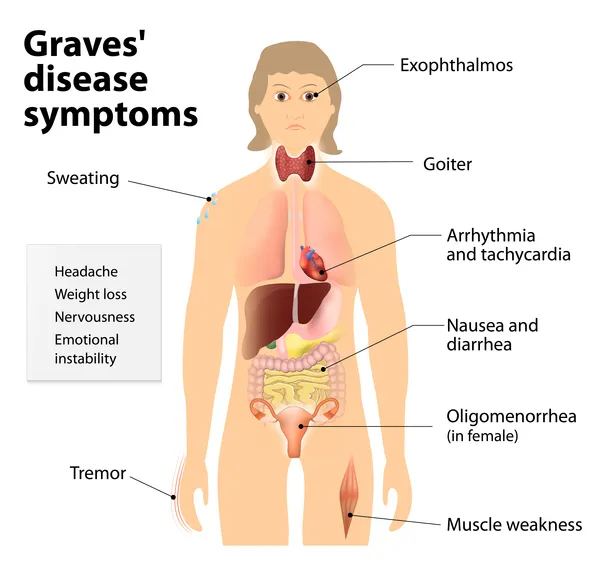
| Eye signs | Exophthalmos (30%) | Absent | Absent |
| TRAb | Positive | Negative | Negative |
| Radioiodine uptake | Diffusely ↑ | Focal ↑ | ↓ (key difference) |
| Treatment | Carbimazole/RAI | RAI/surgery | NSAIDs/beta-blockers |
📌 Remember: The 3 T's of Thyroid Storm - Temperature >38.5°C, Tachycardia >130 bpm, Tremor/agitation (CNS dysfunction)
Visual Aid
Levothyroxine Dose Adjustment Guide:
| Clinical Scenario | Starting Dose | Titration |
|---|---|---|
| Healthy adult <65 years | 100-125 mcg (1.6 mcg/kg) | 25-50 mcg every 6-8 weeks |
| Elderly/IHD | 25 mcg daily | 12.5-25 mcg every 4 weeks |
| Pregnancy | Increase pre-pregnancy dose by 25-30% | Check TFTs every 4 weeks |
Key Points Summary
✓ TFT interpretation: Subclinical = TSH abnormal but T4/T3 normal; treat subclinical hypothyroidism if TSH >10 OR TSH 4.5-10 + symptoms/pregnancy/TPO+
✓ Levothyroxine dosing: 1.6 mcg/kg ideal body weight (typically 100-125 mcg), reduce to 1.2 mcg/kg if >65 years or IHD; check TFTs 6-8 weeks after dose changes
✓ Carbimazole regimens: Titration (15-40 mg, reduce every 4-6 weeks, 12-18 months) OR block-and-replace (40 mg + levothyroxine, 6 months)
✓ Thyroid storm: Mortality 20-30%; treat with propylthiouracil 600 mg loading, propranolol, hydrocortisone 100 mg QDS, supportive ICU care
✓ Agranulocytosis risk: 0.3% on carbimazole-warn patients to stop drug and seek urgent FBC if sore throat/fever develops
✓ TRAb positive = Graves' disease (90% sensitivity); radioiodine uptake differentiates thyroiditis (low uptake) from Graves'/toxic nodule (high uptake)
✓ Common pitfall: Starting full-dose levothyroxine in elderly/IHD patients-always start 25 mcg and titrate slowly to avoid precipitating MI
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

