Quick Overview
Acute coronary syndromes (ACS) encompass STEMI, NSTEMI, and unstable angina, representing a spectrum of myocardial ischaemia/infarction requiring immediate intervention. Differentiation relies on ECG findings and troponin elevation. NICE NG185 emphasises rapid reperfusion, dual antiplatelet therapy (DAPT), and risk stratification using GRACE score to guide management and reduce mortality.
Core Facts & Concepts
Definitions & Classification:
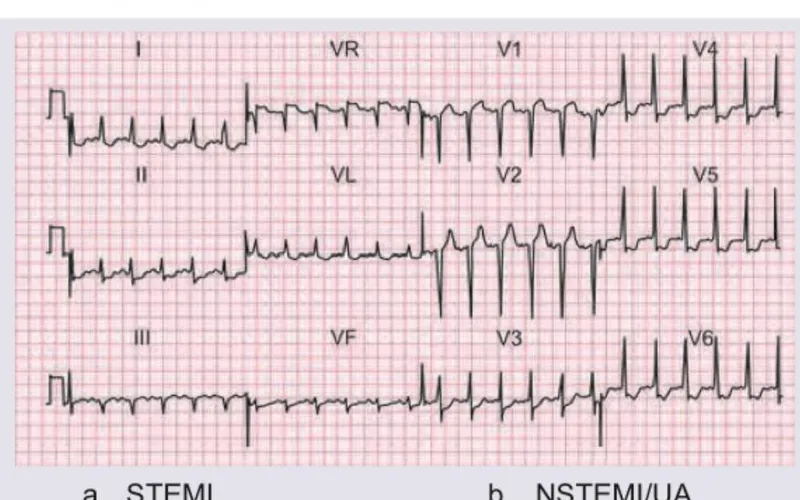
- STEMI: ST elevation ≥1mm in ≥2 contiguous limb leads OR ≥2mm in ≥2 contiguous chest leads OR new LBBB
- NSTEMI: Troponin elevation WITHOUT ST elevation (may show ST depression/T-wave inversion)
- Unstable angina: Cardiac chest pain WITHOUT troponin rise
Critical Timeframes:
- Primary PCI: Target <120 minutes from diagnosis (NICE NG185)
- Thrombolysis: If PCI unavailable, give within 12 hours of symptom onset; door-to-needle <30 minutes
- Angiography in NSTEMI: <72 hours if GRACE score >3% (intermediate-high risk)
Immediate Management (First Hour):
- 📊 MONA-BAT: Morphine + antiemetic, Oxygen (only if SpO₂<94%), Nitrates (GTN sublingual), Aspirin 300mg, Beta-blocker, Antiplatelet (P2Y12 inhibitor), Troponin
DAPT Loading Doses:
- Aspirin 300mg (all ACS) + one of:
- Ticagrelor 180mg (preferred, NICE NG185)
- Prasugrel 60mg (if proceeding to PCI, avoid if age >75 or weight <60kg)
- Clopidogrel 300-600mg (if above contraindicated)
GRACE Score Application:
- Predicts 6-month mortality/MI risk
- >3% = high risk → angiography <72 hours
- 1.5-3% = intermediate → consider angiography
- <1.5% = low → conservative management
Problem-Solving Approach
Step-by-Step ACS Management:
- Immediate recognition: Cardiac chest pain >15 minutes, radiating to jaw/arm, associated sweating/nausea
- 12-lead ECG within 10 minutes of presentation
- Differentiate STEMI vs NSTEMI:
- STEMI → activate primary PCI pathway immediately
- Non-STEMI → high-sensitivity troponin at 0 and 3 hours
- STEMI reperfusion decision:
- PCI available <120 minutes? → Primary PCI
- PCI unavailable/delayed? → Thrombolysis (if <12 hours from onset and no contraindications)
- NSTEMI risk stratification: Calculate GRACE score
- Anticoagulation: Fondaparinux 2.5mg SC daily (preferred) OR unfractionated heparin if PCI imminent
🚩 Red Flags for STEMI Mimics:
- Pericarditis (widespread concave ST elevation, PR depression)
- Takotsubo cardiomyopathy (apical ballooning, emotional trigger)
- Early repolarisation (J-point elevation, young patients)
Thrombolysis Contraindications:
- Previous intracranial haemorrhage, ischaemic stroke <6 months, active bleeding, suspected aortic dissection
Analysis Framework
| Feature | STEMI | NSTEMI | Unstable Angina |
|---|---|---|---|
| ECG | ST elevation/new LBBB | ST depression/T-wave inversion/normal | Normal or dynamic changes |
| Troponin | Elevated | Elevated | Normal |
| Management urgency | Immediate reperfusion (<120 min) | Angiography based on GRACE | Conservative unless high-risk features |
| Mortality risk | Highest (5-10% in-hospital) | Intermediate (3-5%) | Lowest (<2%) |
Secondary Prevention (All ACS):
- 💊 "A-B-C-D-E":
- Aspirin 75mg lifelong + P2Y12 inhibitor 12 months
- Beta-blocker (bisoprolol/carvedilol)
- Cholesterol lowering: Atorvastatin 80mg
- Dual antiplatelet (see above)
- Enalapril/ACE inhibitor (especially if LV dysfunction)
Visual Aid
| GRACE Score Risk | 6-Month Mortality | Management |
|---|---|---|
| Low (<1.5%) | <2% | Conservative, outpatient follow-up |
| Intermediate (1.5-3%) | 2-5% | Consider angiography |
| High (>3%) | >5% | Angiography <72 hours |
Key Points Summary
✓ STEMI diagnosis: ST elevation ≥1mm (limbs) or ≥2mm (chest) in contiguous leads; target primary PCI <120 minutes (NICE NG185)
✓ Immediate DAPT: Aspirin 300mg + ticagrelor 180mg (preferred) or prasugrel 60mg; continue dual therapy 12 months
✓ NSTEMI stratification: GRACE score >3% = high risk → angiography within 72 hours; troponin at 0 and 3 hours
✓ Thrombolysis criteria: STEMI with PCI unavailable, <12 hours from onset, no contraindications (previous ICH, recent stroke)
✓ Secondary prevention "A-B-C-D-E": Aspirin + P2Y12 inhibitor, Beta-blocker, atorvastatin 80mg, ACE inhibitor (especially if LVEF <40%)
✓ Don't miss: Posterior STEMI (tall R waves V1-V3, check posterior leads V7-V9); right ventricular infarction (avoid nitrates/diuretics)
✓ Common pitfall: Giving beta-blockers in acute phase if signs of heart failure/shock-wait until stabilised
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

