Quick Overview
Meningitis is inflammation of the meninges requiring emergency recognition and treatment. NICE NG240 emphasizes immediate antibiotic administration before transfer/investigations if suspected. Bacterial meningitis (mortality 10-15%) demands urgent intervention; viral is self-limiting. Key skills: recognizing clinical features, interpreting CSF parameters, administering pre-hospital antibiotics, and providing chemoprophylaxis to contacts.
Core Facts & Concepts
Clinical Features (Classical Triad in 44% only)
- Headache (severe, sudden-onset)
- Fever (>38°C)
- Neck stiffness (meningism)
- Additional: photophobia, altered consciousness (GCS <14), seizures, non-blanching rash
Emergency Antibiotic Timing (NICE NG240)
- Pre-hospital: IM/IV benzylpenicillin 1.2g (adult) if suspected bacterial meningitis
- Hospital <1 hour: IV ceftriaxone 2g (adult) before LP if no contraindication
- Do NOT delay antibiotics for LP/imaging if bacterial meningitis suspected
LP Contraindications
- GCS ≤12 or deteriorating consciousness
- Focal neurological signs
- Papilloedema
- Signs of raised ICP (bradycardia, hypertension, irregular respirations)
- Coagulopathy (platelets <100, INR >1.4)
- Infection at LP site

CSF Interpretation Thresholds
| Parameter | Bacterial | Viral | Normal |
|---|---|---|---|
| Appearance | Turbid/cloudy | Clear | Clear |
| WCC (cells/mm³) | >1000 (PMN) | 10-1000 (lymph) | <5 |
| Protein (g/L) | >1.0 | 0.4-1.0 | <0.45 |
| Glucose (CSF:blood) | <0.4 | >0.6 | >0.6 |
| Opening pressure | ↑↑ (>25 cmH₂O) | Normal/↑ | 10-20 cmH₂O |
Problem-Solving Approach
Emergency Management Sequence
- Recognize meningitis signs (headache + fever ± meningism)
- Assess severity: GCS, signs of raised ICP, septic shock
- Blood cultures + blood glucose (for CSF:blood ratio)
- Antibiotics within 1 hour: IV ceftriaxone 2g BD (+ ampicillin if >55 years/immunocompromised for Listeria)
- CT head before LP if: GCS ≤12, focal signs, papilloedema, seizures, immunocompromised
- LP if safe: opening pressure, cell count/differential, protein, glucose, Gram stain, culture, PCR (meningococcal/pneumococcal)
- Dexamethasone: 10mg IV QDS for 4 days if bacterial suspected (before/with first antibiotic dose)
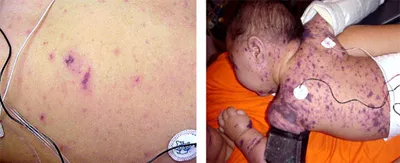
🚩 Red Flags
- Non-blanching rash = meningococcal septicaemia (antibiotics IMMEDIATELY)
- Rapid deterioration in GCS
- Signs of raised ICP (Cushing's triad)
Analysis Framework
Bacterial vs Viral Differentiation
| Feature | Bacterial | Viral |
|---|---|---|
| Onset | Hours (rapid) | Days (gradual) |
| Severity | Critically unwell | Mild-moderate |
| Rash | Purpuric (meningococcal) | Absent |
| CSF WCC | >1000 PMN | 10-1000 lymphocytes |
| CSF protein | >1.0 g/L | 0.4-1.0 g/L |
| CSF glucose | <40% blood | >60% blood |
| Gram stain | Positive (60-90%) | Negative |
Chemoprophylaxis for Contacts (NICE NG240)
- Who: Household/kissing contacts within 7 days of illness onset
- When: Within 24 hours of index case diagnosis
- Regimen:
- Ciprofloxacin 500mg single dose (adult) OR
- Rifampicin 600mg BD for 2 days (adult)
- Applies to: Meningococcal and Hib meningitis only
Visual Aid
Common Causative Organisms by Age
| Age Group | Most Common Organisms |
|---|---|
| Neonates (<3 months) | Group B Strep, E. coli, Listeria |
| Children/Adults | N. meningitidis, S. pneumoniae |
| >55 years | S. pneumoniae, Listeria, Gram-negatives |
| Immunocompromised | Listeria, TB, Cryptococcus |
Key Points Summary
✓ Antibiotics <1 hour: IV ceftriaxone 2g before LP if bacterial meningitis suspected (NICE NG240)
✓ CSF thresholds: Bacterial = WCC >1000 PMN, protein >1.0, glucose <40% blood; Viral = lymphocytic, protein 0.4-1.0, glucose >60%
✓ LP contraindications: GCS ≤12, focal signs, papilloedema, raised ICP signs, coagulopathy
✓ Dexamethasone 10mg IV QDS for 4 days if bacterial meningitis (give before/with antibiotics)
✓ Chemoprophylaxis: Ciprofloxacin 500mg single dose for household/kissing contacts within 24 hours (meningococcal/Hib only)
✓ Non-blanching rash = meningococcal septicaemia requiring immediate antibiotics (don't wait for LP)
✓ Add ampicillin to ceftriaxone if >55 years/immunocompromised for Listeria coverage
⚠️ Warning: Never delay antibiotics for imaging or LP in suspected bacterial meningitis - mortality increases significantly with treatment delay
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

