Quick Overview
The UK NHS offers population-based screening programmes targeting conditions where early detection improves outcomes. Programmes cover cancer (bowel, breast, cervical, AAA), antenatal/newborn, and adult vascular risk. Understanding age criteria, intervals, and referral thresholds is essential for GP practice and patient counseling per NICE PH16 guidelines.
Core Facts & Concepts
Cancer Screening Programmes
| Programme | Age Range | Interval | Method | Referral Threshold |
|---|---|---|---|---|
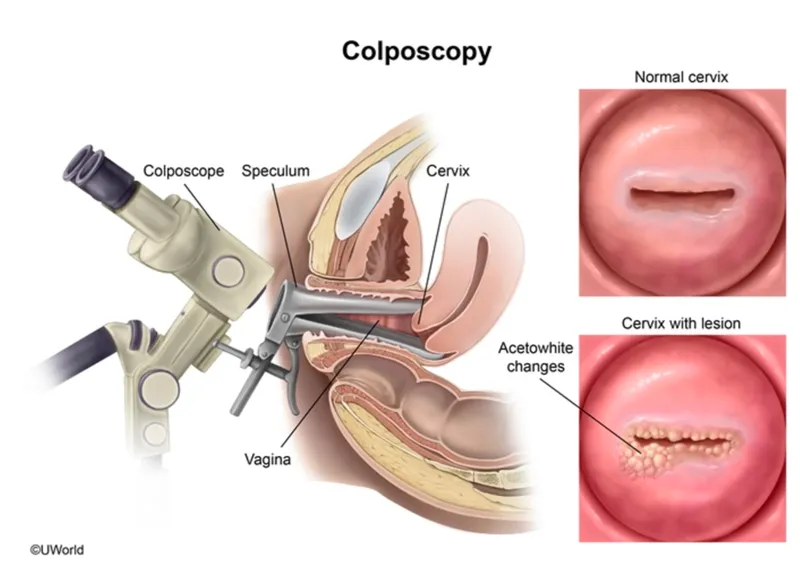
| Cervical | 25-64 years | 25-49: 3-yearly 50-64: 5-yearly | HPV primary testing | HPV+ with cytology abnormality → colposcopy |
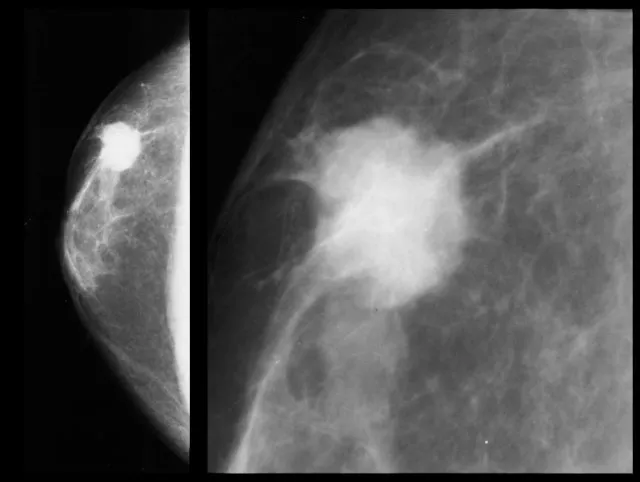
| Breast | 50-71 years | 3-yearly | Mammography (2 views) | Suspicious lesion (R4/R5) → 2-week wait |
| Bowel | 60-74 years | 2-yearly | FIT (Faecal Immunochemical Test) | ≥120 μg Hb/g faeces → colonoscopy |
| AAA | Men 65 years | One-off | Abdominal ultrasound | ≥5.5cm → vascular referral |
Antenatal Screening
- Infectious diseases (booking): HIV, syphilis, hepatitis B, rubella immunity
- Fetal anomaly scan: 18-20+6 weeks (11 structural conditions)
- Down syndrome screening:
- Combined test (11-14 weeks): nuchal translucency + βhCG + PAPP-A
- Quadruple test (14-20 weeks): if missed combined
- Risk ≥1:150 → offer invasive testing (amniocentesis/CVS)
- Sickle cell/thalassaemia: universal at booking
Newborn & Child Screening
- Newborn blood spot (day 5): 9 conditions including PKU, MCADD, sickle cell, CF, hypothyroidism
- Newborn hearing: automated otoacoustic emissions (AOAE) within 4-5 weeks
- Newborn physical examination: within 72 hours + 6-8 weeks (hips, heart, eyes, testes)
⭐ Clinical Pearl: FIT replaced guaiac-based FOBt in 2019 - more sensitive and doesn't require dietary restriction
Problem-Solving Approach
Screening Eligibility Assessment
- Verify age criteria: Automatic invitations sent; manual checks for new registrations
- Identify exclusions:
- Cervical: total hysterectomy for benign disease (if cervix removed)
- Breast: symptomatic patients → 2-week wait, NOT screening
- Bowel: active IBD, previous CRC → surveillance colonoscopy instead
- AAA: women not screened (low prevalence); known AAA → surveillance
- Document informed choice: Screening is voluntary; record acceptance/decline
- Manage abnormal results:
- Cervical HPV+/cytology abnormal → colposcopy within 6 weeks
- Breast recall (R3-R5) → assessment clinic within 3 weeks
- FIT positive → colonoscopy within 2 weeks
- AAA 3.0-4.4cm → annual USS; 4.5-5.4cm → 3-monthly USS
Red Flags - Screening Inappropriate 🚩
- Symptoms present → diagnostic pathway, NOT screening
- High-risk individuals → intensified surveillance (e.g., Lynch syndrome)
- Life expectancy <5 years → discuss risks/benefits
Analysis Framework
Screening vs Surveillance vs Diagnosis
| Feature | Screening | Surveillance | Diagnosis |
|---|---|---|---|
| Population | Asymptomatic, average risk | High-risk/previous disease | Symptomatic |
| Pathway | Invitation-based | Specialist-led protocol | 2-week wait/urgent |
| Example | FIT at age 62 | Annual colonoscopy (Lynch) | Rectal bleeding → sigmoidoscopy |
Wilson-Jungner Screening Criteria (applied to NHS programmes)
- Condition: important, understood natural history, detectable latent phase
- Test: acceptable, valid (sensitive/specific), agreed threshold
- Treatment: effective intervention, agreed policy on whom to treat
- Programme: cost-effective, continuous process, quality-assured
Visual Aid
Key Points Summary
✓ Cervical screening: HPV primary test, 25-64 years (3-yearly then 5-yearly); HPV+/abnormal cytology → colposcopy
✓ Breast screening: 50-71 years, 3-yearly mammography; R4/R5 lesions → urgent referral
✓ Bowel screening: 60-74 years, 2-yearly FIT; ≥120 μg Hb/g → colonoscopy within 2 weeks
✓ AAA screening: Men at 65, one-off USS; ≥5.5cm or symptomatic → vascular surgery
✓ Antenatal: Combined test 11-14 weeks (risk ≥1:150 → invasive testing); anomaly scan 18-20 weeks
✓ Newborn: Blood spot day 5 (9 conditions), hearing screen within 4-5 weeks, physical exam <72 hours
✓ Key exclusion: Symptomatic patients require diagnostic pathways (2-week wait), NOT screening
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

