Acute Surgical Presentations

On this page
Recognition of Acute Surgical Emergencies
A 68-year-old man arrives in the emergency department at 2 AM, clutching his abdomen and describing pain that started suddenly during dinner. His face is pale, he's lying motionless on the trolley, and his abdomen is rigid to even the gentlest touch. This presentation-sudden onset, severe pain, and peritonism-immediately triggers the acute surgical pathway. Recognizing presentations within the first minutes of patient contact can be life-saving, as delays in diagnosis and intervention directly correlate with morbidity and mortality in conditions requiring emergency surgery.
Cardinal Features of Acute Surgical Presentations:
-
Pain characteristics with surgical significance:
- Sudden onset (<1 hour to peak) suggests perforation or vascular catastrophe
- Pain preventing movement or coughing indicates peritoneal inflammation
- Pain out of proportion to examination findings: mesenteric ischemia until proven otherwise
- Migration of pain (periumbilical to RIF in appendicitis) reflects visceral to parietal peritoneum involvement
-
Peritonism-the hallmark of surgical pathology:
- Involuntary guarding (rigid abdomen) vs voluntary guarding (patient-controlled tensing)
- Rebound tenderness: sensitivity 63%, specificity 69% for peritonitis
- Percussion tenderness is more specific and less distressing than rebound testing
- Absent bowel sounds for >3 minutes suggests ileus or advanced obstruction
-
Immediate red flags requiring surgical review within 30 minutes:
- Haemodynamic instability (systolic BP <90 mmHg, HR >120 bpm) with abdominal pain
- Rigid, board-like abdomen suggesting
- Abdominal pain with syncope (ruptured AAA, ectopic pregnancy)
- Absolute constipation (no flatus or stool >48 hours) with vomiting
🚩 Red Flag: Any patient with abdominal pain who lies completely still (peritonitis) or writhes continuously (colic) requires immediate senior assessment-the former suggests surgical pathology, the latter often medical, but both need rapid evaluation.
| Clinical Sign | Sensitivity | Specificity | Surgical Implication |
|---|---|---|---|
| Rigidity | 45% | 92% | High specificity for peritonitis requiring laparotomy |
| Absent bowel sounds | 28% | 88% | Suggests advanced obstruction or ileus |
| Percussion tenderness | 71% | 82% | More reliable than rebound for peritoneal inflammation |
| Guarding | 62% | 76% | Moderate accuracy for surgical pathology |

Recognition of Acute Surgical Emergencies
2 - Pathophysiology of Obstruction, Perforation, and Peritoneal Inflammation
The progression from visceral discomfort to life-threatening peritonitis follows predictable pathophysiological stages that guide both diagnosis and timing of intervention. Understanding why causes pain before vomiting, or why produces sudden-onset symptoms, allows clinicians to anticipate complications and intervene before irreversible damage occurs. The common pathway-tissue ischemia, bacterial translocation, and systemic inflammatory response-explains why seemingly localized abdominal pathology can rapidly progress to septic shock.
Mechanisms of Acute Surgical Pathology:
-
Bowel obstruction cascade:
- Proximal dilatation increases intraluminal pressure (normally 2-4 mmHg, rises to >20 mmHg)
- Venous congestion → arterial compromise → mucosal ischemia within 6-12 hours
- Bacterial overgrowth and translocation trigger SIRS
- Closed-loop obstruction (volvulus, incarcerated hernia) progresses to strangulation within 4-6 hours
-
Perforation and peritoneal contamination:
- Chemical peritonitis (gastric acid, bile) causes immediate severe pain
- Bacterial peritonitis develops over 6-12 hours as bowel flora proliferate
- Third-space fluid losses: 4-6 liters can sequester in peritoneal cavity within 24 hours
- Systemic absorption of endotoxin drives septic shock if source control delayed >12 hours
-
Ischemia-reperfusion injury in acute mesenteric ischemia:
- Oxygen-free radical production peaks during reperfusion, not ischemia
- Lactate >2.5 mmol/L with normal pH suggests compensated shock
- Lactate >4 mmol/L: 28% mortality, rising to 89% if intervention delayed >24 hours
| Mechanism | Time to Critical Complication | Key Biomarker | Intervention Window |
|---|---|---|---|
| Closed-loop obstruction | 4-6 hours to strangulation | Lactate, WCC | <6 hours for best outcomes |
| Hollow viscus perforation | 6-12 hours to bacterial peritonitis | WCC >15, CRP >150 | <12 hours reduces mortality by 40% |
| Mesenteric ischemia | 6-8 hours to transmural infarction | Lactate >4, D-dimer >500 | <6 hours for bowel salvage |
2 — Pathophysiology of Obstruction, Perforation, and Peritoneal Inflammation
3 - Structured Assessment and Diagnostic Imaging
A 45-year-old woman presents with 12 hours of colicky central abdominal pain, now constant, with four episodes of bilious vomiting. She last opened her bowels yesterday morning and has a previous laparotomy scar. Your systematic approach begins with recognizing the pattern-pain before vomiting suggests obstruction-and proceeds through structured examination and targeted imaging. The assessment framework combines clinical probability estimation with investigation selection to minimize diagnostic delays while avoiding unnecessary radiation exposure.
Systematic Clinical Assessment:
-
History elements that change management:
- Previous abdominal surgery (adhesional obstruction likelihood ratio 3.4)
- Cardiovascular disease with abdominal pain: consider mesenteric ischemia (30% mortality)
- Immunosuppression: higher perforation risk with minimal signs
- Anticoagulation: complicates both diagnosis and surgical intervention
-
Examination sequence for surgical pathology:
- Inspection: surgical scars, distension, visible peristalsis (obstruction), bruising (retroperitoneal bleeding)
- Auscultation before palpation: high-pitched tinkling sounds in early obstruction
- Palpation: start furthest from pain; assess for peritonism systematically
- Digital rectal examination mandatory: 15% of diagnoses made or changed
-
Laboratory interpretation in acute surgical context:
- WCC >15 × 10⁹/L: sensitivity 70% for surgical pathology, but normal WCC doesn't exclude it
- Lactate >2 mmol/L: 92% sensitivity for bowel ischemia (specificity only 50%)
- Amylase >1000 IU/L suggests pancreatitis, but <1000 doesn't exclude it
- CRP <50 mg/L makes bacterial peritonitis less likely if symptoms >12 hours
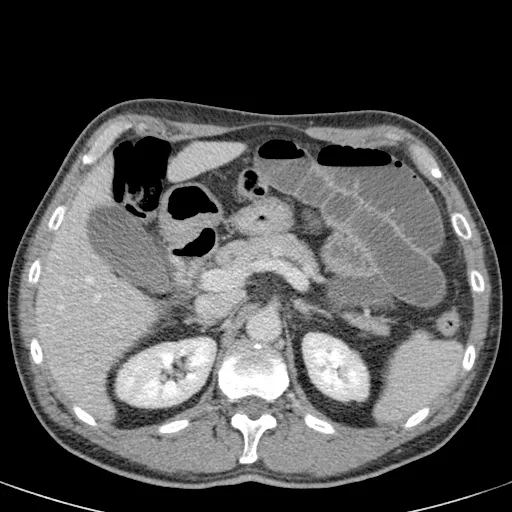

Imaging Protocol for Diagnosis:
| Investigation | Sensitivity | Specificity | Clinical Application |
|---|---|---|---|
| AXR for obstruction | 69% | 57% | Initial screen; CT required if clinical suspicion high |
| CT for obstruction | 94% | 96% | Gold standard; identifies transition point and ischemia |
| Erect CXR for perforation | 78% | 82% | Misses 20% of perforations; CT if high suspicion |
| CT for perforation | 95% | 97% | Detects small volume free air and localized collections |
3 — Structured Assessment and Diagnostic Imaging
4 - Differentiating Surgical from Medical Causes
The diagnostic challenge in presentations lies not in recognizing severe pathology-the rigid abdomen announces itself-but in distinguishing early surgical disease from medical mimics. A 72-year-old diabetic with vague abdominal discomfort and mild tenderness could have early mesenteric ischemia (requiring emergency surgery), diabetic ketoacidosis (requiring insulin), or inferior MI (requiring cardiology input). The stakes are high: operating unnecessarily causes harm, but delayed surgery for true surgical pathology increases mortality by 2-3% per hour after the optimal intervention window.
Key Discriminating Features:
-
Surgical vs medical acute abdomen:
- Surgical: pain intensity increasing over time, localized peritonism developing
- Medical: pain intensity fluctuating, diffuse tenderness without guarding
- Surgical: pain preventing movement or coughing
- Medical: patient able to move freely despite pain
-
High-risk presentations requiring urgent surgical input:
- Age >65 + abdominal pain + cardiovascular disease = mesenteric ischemia risk
- Previous aortic surgery + abdominal/back pain = graft complication until proven otherwise
- Immunosuppressed + abdominal pain = higher perforation risk with minimal signs
- Abdominal pain + atrial fibrillation = embolic mesenteric ischemia (20% mortality even with intervention)
-
** vs ileus:**
- Obstruction: colicky pain, high-pitched bowel sounds early, visible peristalsis
- Ileus: constant discomfort, absent bowel sounds, no colicky pattern
- Obstruction: vomiting precedes distension in proximal obstruction
- Ileus: distension without significant vomiting
| Feature | Surgical Cause | Medical Cause | Likelihood Ratio |
|---|---|---|---|
| Rigidity | Peritonitis, perforation | Rare (severe pancreatitis) | LR+ 8.4 for surgical |
| Rebound tenderness | Peritoneal inflammation | Uncommon | LR+ 2.5 for surgical |
| Pain before vomiting | Obstruction, appendicitis | Gastroenteritis (vomiting first) | LR+ 3.1 for surgical |
| Pain out of proportion | Mesenteric ischemia | Rare | LR+ 6.2 for ischemia |
⭐ Clinical Pearl: In elderly patients with abdominal pain and atrial fibrillation, treat as mesenteric ischemia until proven otherwise-start anticoagulation (if no contraindications), obtain urgent CT angiography, and involve surgeons early. Mortality exceeds 70% if diagnosis delayed beyond 12 hours.
Common Diagnostic Pitfalls:
-
False reassurance from normal investigations:
- Normal lactate doesn't exclude early ischemia (sensitivity 90% only when disease advanced)
- Normal WCC in 30% of proven appendicitis and 25% of
- CT performed too early (<4 hours from symptom onset) may miss evolving pathology
-
Cognitive biases in acute surgical assessment:
- Anchoring on initial diagnosis (gastroenteritis) despite evolving peritonism
- Availability bias: recent benign cases leading to underestimation of current presentation
- Premature closure: accepting first plausible diagnosis without considering surgical causes
4 — Differentiating Surgical from Medical Causes
5 - Evidence-Based Management Decisions and Timing
The decision to operate, when to operate, and what operation to perform represents the synthesis of clinical assessment, investigation findings, and risk stratification. NICE NG158 emphasizes early involvement of senior surgical decision-makers for patients with suspected acute surgical pathology, recognizing that delayed intervention significantly increases morbidity and mortality. For , the question is not just "is this obstruction?" but "is this simple or strangulated?" because the latter requires surgery within 6 hours, while selected simple obstructions may resolve with conservative management.
Conservative vs Operative Management:
-
** management strategy:**
- Adhesional obstruction without ischemia signs: 70% resolve with conservative management in 48-72 hours
- Nasogastric decompression, IV fluids (2-3 L crystalloid initially), nil by mouth
- Water-soluble contrast study at 24 hours: if contrast reaches colon by 24 hours, 95% resolve without surgery
- Failure criteria: no improvement by 72 hours, or any deterioration (increasing pain, peritonism, rising lactate)
-
** requires emergency surgery:**
- Resuscitation followed by laparotomy/laparoscopy within 6 hours of diagnosis
- Exception: sealed perforations in stable patients may be managed conservatively with antibiotics
- Mortality increases 2.5% per hour delay beyond 12 hours from symptom onset
-
Damage control surgery principles for unstable patients:
- Control contamination (resection without anastomosis, exteriorization)
- Abbreviated procedure <90 minutes to prevent hypothermia/coagulopathy
- Planned return to theatre in 24-48 hours for definitive reconstruction
| Condition | Intervention Timing | Evidence | Mortality Impact |
|---|---|---|---|
| Strangulated obstruction | <6 hours | Mortality 8% if <6h, 25% if >12h | 3-fold increase with delay |
| Perforated viscus | <12 hours | Mortality 10% if <12h, 30% if >24h | 2.5% increase per hour delay |
| Mesenteric ischemia | <6 hours | Bowel salvage 70% if <6h, 20% if >12h | 5-fold mortality increase |
5 — Evidence-Based Management Decisions and Timing
6 - Comprehensive Perioperative and MDT Coordination
A 58-year-old man with known Crohn's disease presents with his fourth episode of small bowel obstruction. Previous episodes resolved conservatively, but this time CT shows a closed-loop obstruction with early ischemic changes. His case exemplifies the complexity of real-world surgical decision-making: balancing surgical risk against disease progression, coordinating between gastroenterology and surgery, and planning for potential complications including short bowel syndrome. The pathway must integrate resuscitation, multidisciplinary input, and contingency planning for both operative and postoperative complications.
Resuscitation Priorities Before Surgery:
-
Fluid resuscitation targets:
- Initial bolus: 500 mL crystalloid over 15 minutes, reassess
- Target urine output >0.5 mL/kg/h (not >1 mL/kg/h-avoid fluid overload)
- Third-space losses in : replace 2-3 L deficit before induction
- Lactate clearance >10% per hour indicates adequate resuscitation
-
Antibiotic timing in surgical sepsis:
- Administer within 1 hour of diagnosis: reduces mortality by 7.6% per hour delay
- Empirical regimen for intra-abdominal sepsis: co-amoxiclav 1.2 g IV TDS or piperacillin-tazobactam 4.5 g IV TDS
- Add metronidazole 500 mg IV TDS if beta-lactam allergy (use ciprofloxacin + metronidazole)
MDT Coordination Points:
-
Preoperative optimization within intervention window:
- Anaesthetic review for high-risk patients (ASA ≥3): balance delay against optimization benefit
- Critical care involvement if predicted need for postoperative organ support
- Stoma nurse review if high likelihood of stoma formation
-
Special population considerations:
- Elderly (>75 years): 30-day mortality 15-25% for emergency laparotomy vs 2-5% for elective
- Frailty assessment: Clinical Frailty Scale ≥6 associated with 3-fold mortality increase
- Pregnancy: MRI preferred over CT when feasible; involve obstetrics early
| Complication | Incidence | Prevention Strategy | Early Recognition |
|---|---|---|---|
| Anastomotic leak | 5-10% | Adequate perfusion, no tension, no distal obstruction | Rising CRP day 3-5, tachycardia |
| Intra-abdominal collection | 10-15% | Source control, appropriate drainage | Persistent fever, rising inflammatory markers |
| Wound infection | 15-25% | Prophylactic antibiotics within 60 min of incision | Erythema, purulent discharge by day 5-7 |
⭐ Clinical Pearl: For emergency laparotomy in high-risk patients, the decision is not "operate or not" but "operate now or optimize first." If lactate >4 mmol/L or signs of organ dysfunction, proceed immediately-further delay worsens outcomes. If lactate <2 mmol/L and stable, 2-4 hours of optimization (fluid resuscitation, antibiotics, senior anaesthetic input) may reduce perioperative mortality without compromising surgical outcomes.
6 — Comprehensive Perioperative and MDT Coordination
High Yield Summary
Key Take-Aways:
- Peritonism (rigidity, percussion tenderness) has 92% specificity for surgical pathology requiring laparotomy-normal examination doesn't exclude early disease
- Intervention timing is critical: mortality increases 2.5% per hour for perforation and 3-fold for strangulated obstruction if surgery delayed >6-12 hours
- Pain out of proportion to examination findings = mesenteric ischemia until proven otherwise (30% mortality even with treatment)
- Conservative management appropriate for adhesional bowel obstruction without ischemia signs-70% resolve in 48-72 hours with NG decompression and IV fluids
- CT abdomen/pelvis with IV contrast is gold standard (94-96% sensitivity/specificity) for obstruction and perforation-don't rely on plain films if clinical suspicion high
- Antibiotics within 1 hour of diagnosis reduce mortality by 7.6% per hour delay-co-amoxiclav 1.2 g IV or piperacillin-tazobactam 4.5 g IV empirically
- Lactate >4 mmol/L indicates advanced disease requiring immediate surgery-lactate 2-4 mmol/L suggests compensated shock needing urgent intervention
Essential Acute Surgical Presentations Numbers:
| Parameter | Threshold | Clinical Significance |
|---|---|---|
| Lactate | >2 mmol/L | 92% sensitivity for bowel ischemia |
| WCC | >15 × 10⁹/L | 70% sensitivity for surgical pathology |
| Time to surgery (strangulation) | <6 hours | Mortality 8% vs 25% if >12 hours |
| Time to surgery (perforation) | <12 hours | Mortality 10% vs 30% if >24 hours |
| Urine output target | >0.5 mL/kg/h | Adequate resuscitation marker |
Key Principles:
- Early senior surgical involvement is mandatory-NICE NG158 emphasizes consultant-level assessment for suspected acute surgical abdomen within 30 minutes
- Serial examination is more valuable than single assessment-deterioration (increasing pain, peritonism, rising lactate) mandates surgical intervention
- Elderly patients with atrial fibrillation and abdominal pain = embolic mesenteric ischemia until proven otherwise-obtain urgent CT angiography
- Conservative management of obstruction requires strict monitoring: failure to improve by 72 hours or any deterioration triggers surgical intervention
Quick Reference-Red Flags Requiring Immediate Surgical Review:
| Clinical Scenario | Action | Time Frame |
|---|---|---|
| Rigid abdomen + shock | Emergency laparotomy | <1 hour |
| Closed-loop obstruction on CT | Emergency surgery | <6 hours |
| Perforation + peritonitis | Emergency surgery | <6 hours |
| Pain out of proportion + lactate >4 | Mesenteric ischemia protocol | <2 hours to CT angiography |
| Failed conservative management | Surgical intervention | By 72 hours |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app






