Acute Medical Presentations

On this page
Recognition and Classification of Acute Medical Emergencies
A 68-year-old woman presents to the Emergency Department with confusion, fever, and hypotension. Her NEWS2 score is 11. Within minutes, you recognize this as a potential life-threatening emergency requiring immediate intervention. The ability to rapidly identify and classify acute medical presentations determines patient outcomes-sepsis mortality increases 7.6% per hour of delayed antibiotic administration, while anaphylaxis can progress to cardiovascular collapse within minutes. Mastering foundational definitions, epidemiological patterns, and clinical recognition criteria forms the bedrock of emergency medicine competence.
-
Sepsis : Life-threatening organ dysfunction caused by dysregulated host response to infection
- qSOFA criteria (≥2 predicts poor outcome): Respiratory rate ≥22/min, altered mentation, systolic BP ≤100 mmHg
- Septic shock: Persisting hypotension requiring vasopressors (MAP ≥65 mmHg) + lactate >2 mmol/L despite adequate fluid resuscitation
- UK incidence: 250,000 cases/year; in-hospital mortality 30-50% for septic shock
-
Anaphylaxis : Severe, life-threatening systemic hypersensitivity reaction
- Incidence: 1-3 per 10,000 person-years; case fatality rate 0.3-1%
- Recognition requires acute onset with skin/mucosal involvement PLUS either respiratory compromise OR cardiovascular instability
-
Acute chest pain: 1-2% of UK ED presentations; 5-10% have acute coronary syndrome
- Troponin elevation at 3 hours has 99% sensitivity for NSTEMI
-
Collapse and syncope: Accounts for 1-3% of ED attendances; 6% of hospital admissions
- 40% cardiac causes in patients >60 years versus 10% in younger patients
| Emergency | Time-Critical Threshold | Mortality if Delayed |
|---|---|---|
| Septic shock | Antibiotics within 1 hour | +7.6% per hour |
| Anaphylaxis | Adrenaline within 5 minutes | 1-3% fatal if untreated |
| STEMI | PCI within 120 minutes | 1% per 30-min delay |
| Cardiac arrest | CPR within 3-5 minutes | 10% survival decrease per minute |
📌 Mnemonic for Anaphylaxis Recognition - FAST:
Flushing/urticaria, Angioedema, Stridor/wheeze, Tachycardia/hypotension
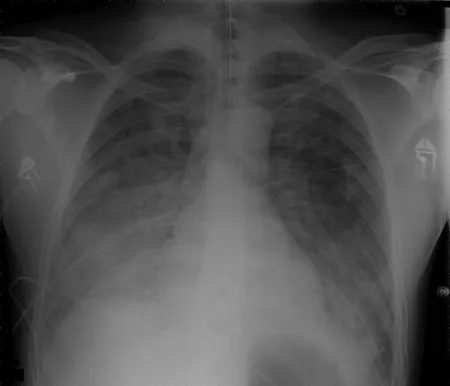
Recognition and Classification of Acute Medical Emergencies
2 - Pathophysiological Mechanisms Driving Acute Deterioration
Understanding why patients deteriorate guides rational treatment selection. In sepsis , pathogen-associated molecular patterns (PAMPs) trigger toll-like receptors, unleashing a cytokine storm (TNF-α, IL-1, IL-6) that causes widespread endothelial dysfunction, capillary leak, and microvascular thrombosis. This explains why septic patients require both fluid resuscitation AND vasopressor support-distributive shock with relative hypovolaemia. The progression from systemic inflammatory response syndrome (SIRS) to multiple organ dysfunction syndrome (MODS) follows predictable patterns: cardiovascular collapse → acute respiratory distress syndrome (ARDS) → acute kidney injury → disseminated intravascular coagulation (DIC).
-
Sepsis cascade: Endotoxin → macrophage activation → TNF-α/IL-1 release → nitric oxide-mediated vasodilatation → capillary leak → tissue hypoperfusion
- Lactate >2 mmol/L indicates tissue hypoxia and anaerobic metabolism
- Myocardial depression occurs in 40% (reversible within 7-10 days if patient survives)
-
Syncope mechanisms :
- Reflex (vasovagal): Vagal overactivity → bradycardia + vasodilatation → cerebral hypoperfusion
- Orthostatic: Autonomic failure → inadequate vasoconstriction → BP drop >20 mmHg systolic within 3 minutes of standing
- Cardiac: Arrhythmia (VT, complete heart block) or structural (AS, HOCM) → reduced cardiac output → cerebral hypoperfusion <60 mmHg MAP
-
Acute chest pain pathophysiology :
- ACS: Plaque rupture → thrombus formation → coronary occlusion → myocardial ischemia/necrosis
- Aortic dissection: Intimal tear → blood enters media → propagates distally/proximally → branch vessel occlusion
- Pulmonary embolism: Thrombus → pulmonary arterial obstruction → V/Q mismatch + right ventricular strain
| Mechanism | Clinical Manifestation | Quantitative Marker |
|---|---|---|
| Endothelial leak | Pulmonary oedema, hypotension | Lactate >4 mmol/L |
| Myocardial depression | Reduced ejection fraction | Troponin elevation in 50% |
| Coagulopathy | DIC, bleeding | Platelets <100, PT >1.5x normal |
2 — Pathophysiological Mechanisms Driving Acute Deterioration
3 - Structured Assessment and Immediate Interventions
A 45-year-old man presents with sudden-onset central chest pain radiating to the jaw. You immediately apply the ABCDE approach: Airway patent, Breathing 22/min with normal saturations, Circulation shows BP 90/60 mmHg with weak radial pulse, Disability GCS 15, Exposure reveals diaphoresis. Your systematic assessment identifies high-risk features requiring immediate ECG and troponin. The ABCDE framework prevents cognitive errors and ensures no critical abnormality is missed.
-
ABCDE approach (NICE NG51 recommendation for all acute presentations):
- A (Airway): Look for obstruction, stridor, inability to speak; prepare for intubation if GCS <8
- B (Breathing): RR >25 or <10, SpO₂ <92%, use of accessory muscles; target SpO₂ 94-98% (88-92% if COPD risk)
- C (Circulation): HR >130 or <40, SBP <90 mmHg, capillary refill >2 seconds, urine output <0.5 mL/kg/hr
- D (Disability): GCS <15, AVPU score, blood glucose (exclude hypoglycaemia <4 mmol/L)
- E (Exposure): Temperature >38°C or <36°C, rashes (petechiae in meningococcal sepsis)
-
NEWS2 scoring (NICE NG51): Aggregate score predicting mortality and ICU admission
- Score ≥7: High-risk, urgent senior review within 30 minutes
- Score 5-6: Medium-risk, urgent review within 1 hour
- Score 1-4: Low-risk, monitor at least 12-hourly
-
Sepsis management (Sepsis Six within 1 hour):
- Oxygen to maintain SpO₂ ≥94%
- Blood cultures before antibiotics
- IV antibiotics (e.g., piperacillin-tazobactam 4.5g TDS)
- IV fluid resuscitation: 500 mL crystalloid bolus over 15 minutes, reassess
- Lactate and full blood count measurement
- Urine output monitoring (catheterize if needed)
-
Anaphylaxis immediate treatment :
- Adrenaline 500 mcg IM (0.5 mL of 1:1000) into anterolateral thigh, repeat every 5 minutes if no improvement
- High-flow oxygen 15 L/min via non-rebreathe mask
- IV fluid bolus 500-1000 mL crystalloid for hypotension
- Second-line: Chlorphenamine 10 mg IV, hydrocortisone 200 mg IV (prevent biphasic reaction)
-
Acute chest pain :
- STEMI: Aspirin 300 mg, ticagrelor 180 mg loading, morphine 5-10 mg IV, GTN spray, urgent PCI
- High-sensitivity troponin at presentation and 3 hours; HEART score for risk stratification

3 — Structured Assessment and Immediate Interventions
4 - Diagnostic Reasoning and Risk Stratification
Distinguishing between life-threatening and benign causes of chest pain requires systematic analysis. A 55-year-old diabetic with 20-minute central chest pain, diaphoresis, and ECG showing 2 mm ST elevation in V2-V4 has >95% probability of anterior STEMI. Contrast this with a 28-year-old with sharp, positional, left-sided chest pain and normal troponin-likely musculoskeletal. Clinical gestalt alone misses 2-5% of ACS cases; structured risk stratification tools reduce diagnostic errors.
-
HEART score for chest pain (predicts 6-week MACE):
- History (2 points if highly suspicious), ECG (2 points if significant ST deviation), Age (2 points if ≥65), Risk factors (2 points if ≥3), Troponin (2 points if >3x normal)
- Score 0-3: 1.7% MACE risk (safe discharge); 4-6: 17% risk (admit); 7-10: 50% risk (urgent intervention)
-
Syncope risk stratification :
- High-risk features: Age >60, cardiac history, exertional syncope, abnormal ECG, family history sudden death
- Canadian Syncope Risk Score: Predicts 30-day serious adverse events (arrhythmia, MI, death)
- ECG red flags: QTc >480 ms (torsades risk), Brugada pattern, epsilon wave (ARVC), Q waves (prior MI)
| Condition | Key Discriminator | Sensitivity | Specificity |
|---|---|---|---|
| STEMI | ST elevation ≥1 mm in ≥2 contiguous leads | 60-70% | 95-97% |
| Pulmonary embolism | D-dimer + Wells score ≥4 | 95% (D-dimer) | 40% (D-dimer) |
| Aortic dissection | Widened mediastinum on CXR | 60% | 85% |
| Cardiac syncope | Troponin elevation + ECG changes | 70% | 90% |
⭐ Clinical Pearl: Troponin elevation occurs in 50% of septic shock patients without ACS-interpret in clinical context, not isolation.
- Common pitfalls:
- Assuming normal ECG excludes ACS (10-15% of NSTEMI have normal initial ECG)
- Attributing syncope to "vasovagal" without ECG in patients >40 years (misses 15% of cardiac causes)
- Using D-dimer in high-probability PE (low specificity leads to false reassurance if negative)
4 — Diagnostic Reasoning and Risk Stratification
5 - Treatment Response Evaluation and Escalation Criteria
After initiating sepsis treatment , you reassess at 1 hour: lactate decreased from 4.2 to 2.8 mmol/L, BP improved to 105/65 mmHg on 500 mL fluid bolus, urine output 30 mL/hr. These markers indicate treatment response, but persistent tachycardia (HR 115) and ongoing confusion suggest evolving organ dysfunction requiring ICU escalation. Knowing when initial measures suffice versus when to escalate determines survival-delayed ICU admission in severe sepsis increases mortality by 1.5-fold.
-
Sepsis treatment response markers (reassess hourly):
- Lactate clearance: Aim for >10% reduction per hour; persistent lactate >4 mmol/L after 6 hours predicts 50% mortality
- Urine output: Target >0.5 mL/kg/hr (35 mL/hr for 70 kg patient); oliguria <0.3 mL/kg/hr indicates renal hypoperfusion
- MAP target: ≥65 mmHg; may require noradrenaline infusion if not achieved with 30 mL/kg fluid bolus
- Mental status: Persistent confusion despite BP correction suggests cerebral hypoperfusion
-
Escalation criteria for ICU (NICE NG51):
- Requiring vasopressor/inotrope support beyond initial resuscitation
- Respiratory failure needing mechanical ventilation (PaO₂/FiO₂ <200)
- Acute kidney injury requiring renal replacement therapy (creatinine >300 μmol/L with oliguria)
- Lactate >4 mmol/L persisting after 2 hours despite treatment
-
Syncope admission decisions :
- Admit if: Age >60, cardiac history, exertional syncope, abnormal ECG, injury from fall, no prodrome
- Safe discharge: Young patient, clear vasovagal trigger (pain, prolonged standing), normal ECG, rapid recovery
- Telemetry monitoring for 24 hours if intermediate risk (detects arrhythmia in 15%)
| Parameter | Target | Escalation Threshold |
|---|---|---|
| MAP | ≥65 mmHg | <65 despite 30 mL/kg fluid + vasopressor |
| Lactate | <2 mmol/L | >4 mmol/L after 6 hours |
| Urine output | >0.5 mL/kg/hr | <0.3 mL/kg/hr for 3 hours |
| PaO₂/FiO₂ | >300 | <200 (ARDS) |
5 — Treatment Response Evaluation and Escalation Criteria
6 - Protocol Development and Quality Improvement
Anaphylaxis management protocols reduce time-to-adrenaline from 15 minutes to 3 minutes when implemented with simulation training. Your hospital's acute chest pain pathway decreased door-to-balloon time from 140 to 85 minutes, improving STEMI survival by 8%. Systematic approaches to acute presentations-standardized order sets, early warning systems, and structured handovers-transform individual clinical excellence into reliable organizational performance.
-
Sepsis protocol elements:
- Electronic alerts: NEWS2 ≥7 triggers automatic sepsis screening questions
- Order sets: Pre-populated blood cultures, lactate, antibiotics based on likely source
- Audit metrics: % receiving antibiotics within 1 hour (target >90%), 30-day mortality, ICU length of stay
-
Anaphylaxis emergency box:
- Pre-loaded adrenaline syringes (1:1000, 0.5 mL) in all clinical areas
- Cognitive aid cards with dosing algorithms at point-of-care
- Quarterly simulation drills to maintain team competency
-
SBAR handover structure (NICE CG50 recommendation):
- Situation: "68-year-old with septic shock from urosepsis"
- Background: "Type 2 diabetes, baseline creatinine 95 μmol/L"
- Assessment: "Received 2 L fluids, piperacillin-tazobactam, lactate 3.2 mmol/L down from 5.1"
- Recommendation: "Needs HDU bed for noradrenaline if BP doesn't improve"
-
Quality improvement cycles:
- Run charts tracking time-to-antibiotic in sepsis (identify delays >1 hour)
- Root cause analysis of missed anaphylaxis diagnoses (common: attributing wheeze to asthma exacerbation)
- Mortality and morbidity review of delayed escalations
| Protocol Component | Impact on Outcome | Implementation Barrier |
|---|---|---|
| Electronic sepsis alerts | 20% mortality reduction | Alert fatigue (false positives) |
| Standardized chest pain pathway | 30-min reduction door-to-balloon | Requires 24/7 cath lab access |
| Simulation training | 50% reduction time-to-adrenaline | Staff time/cost |
6 — Protocol Development and Quality Improvement
High Yield Summary
Key Take-Aways:
- Sepsis recognition: qSOFA ≥2 (RR ≥22, altered mentation, SBP ≤100) predicts poor outcomes; septic shock requires vasopressors + lactate >2 mmol/L
- Time-critical interventions: Sepsis antibiotics within 1 hour (mortality increases 7.6% per hour delay); anaphylaxis adrenaline 500 mcg IM within 5 minutes
- NEWS2 ≥7 mandates urgent senior review within 30 minutes; score predicts ICU admission and mortality
- HEART score 0-3 for chest pain allows safe discharge (1.7% MACE risk); score ≥7 requires urgent intervention (50% MACE risk)
- Escalation criteria: Persistent lactate >4 mmol/L, MAP <65 mmHg despite fluids, urine output <0.3 mL/kg/hr for 3 hours
- Syncope red flags: Age >60, cardiac history, exertional syncope, abnormal ECG, no prodrome-all require admission and telemetry
- Anaphylaxis treatment: Adrenaline 500 mcg IM (0.5 mL of 1:1000), repeat every 5 minutes; chlorphenamine 10 mg IV and hydrocortisone 200 mg IV prevent biphasic reactions
Essential Acute Medical Presentations Numbers:
| Parameter | Critical Threshold | Action |
|---|---|---|
| NEWS2 | ≥7 | Senior review within 30 minutes |
| Lactate | >4 mmol/L persisting | Consider ICU escalation |
| MAP | <65 mmHg | Start vasopressor support |
| Troponin rise/fall | >20% change | Diagnostic for MI |
| Adrenaline dose | 500 mcg IM | Repeat every 5 minutes if needed |
| Sepsis fluid bolus | 500 mL over 15 min | Reassess after each bolus |
Key Principles:
- Systematic ABCDE assessment prevents missed critical abnormalities-never skip steps even in time-critical emergencies
- Sepsis Six within 1 hour: Oxygen, cultures, antibiotics, fluids, lactate, urine output monitoring
- Risk stratification tools (HEART score, qSOFA, Canadian Syncope Risk Score) outperform clinical gestalt alone
- Common mistake: Interpreting troponin elevation as ACS in septic patients-50% have troponin rise without coronary occlusion
- Escalation threshold: If initial treatment doesn't improve lactate by >10%/hour or maintain MAP ≥65 mmHg, escalate to ICU
Quick Reference:
| Emergency | Immediate Action | Time Target | Escalation Trigger |
|---|---|---|---|
| Septic shock | Antibiotics + 500 mL fluid bolus | Within 1 hour | Lactate >4 mmol/L at 6 hours |
| Anaphylaxis | Adrenaline 500 mcg IM | Within 5 minutes | No response after 2 doses |
| STEMI | Aspirin + PCI activation | Door-to-balloon <120 min | Cardiogenic shock |
| High-risk syncope | ECG + telemetry + troponin | Within 30 minutes | Arrhythmia detected |
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for UKMLA prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app








