Quick Overview
Epilepsy affects 0.5-1% of children, defined as ≥2 unprovoked seizures >24 hours apart or 1 seizure with high recurrence risk. NICE NG217 provides evidence-based guidance on classification, treatment selection by seizure type, and emergency management. Correct seizure classification determines appropriate antiepileptic drug (AED) choice-misclassification leads to treatment failure or seizure exacerbation.
Core Facts & Concepts
Seizure Classification (ILAE 2017)
| Seizure Type | Key Features | First-Line AED |
|---|---|---|
| Focal onset | Aware/impaired awareness, motor/non-motor | Carbamazepine or Levetiracetam |
| Generalised tonic-clonic | Loss of consciousness, tonic then clonic phase | Sodium valproate (males), Lamotrigine or Levetiracetam (females) |
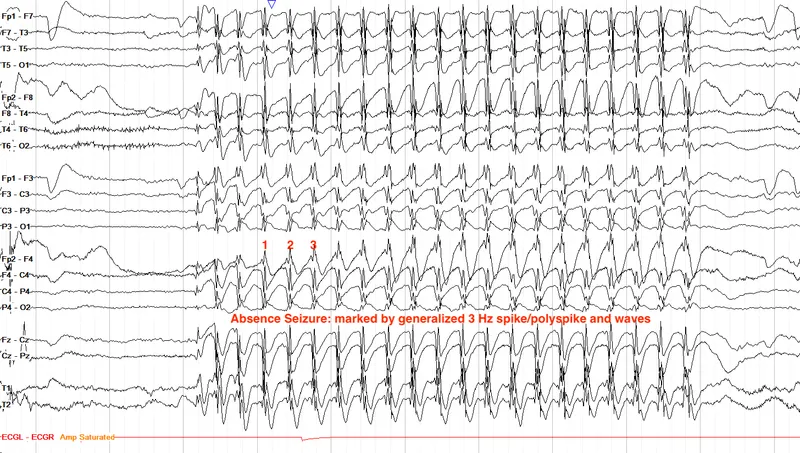
| Absence | Brief (<10s) staring, abrupt onset/offset | Ethosuximide or Sodium valproate (males) |
| Myoclonic | Brief muscle jerks, consciousness preserved | Sodium valproate (males), Levetiracetam (females) |
| Tonic/Atonic | Sudden stiffening or loss of tone | Specialist referral required |
💊 Sodium Valproate Restrictions (Pregnancy Prevention Programme)
- Contraindicated in females of childbearing potential unless conditions met
- Must use ≥1 effective contraception, annual risk acknowledgement form
- Teratogenic risk: 10% major congenital malformations, 30-40% neurodevelopmental disorders
📊 Key Numbers
- Status epilepticus definition: ≥5 minutes continuous seizure or ≥2 seizures without recovery
- Treatment threshold: After 5 minutes of seizure activity
- Refer to paediatric neurology: Diagnosis confirmation, treatment failure, <1 year age
Problem-Solving Approach
Status Epilepticus Emergency Protocol
- 0-5 minutes: ABCDE assessment, high-flow oxygen, check glucose, position safely
- 5 minutes: Buccal midazolam 0.5mg/kg (max 10mg) OR IV lorazepam 0.1mg/kg (max 4mg)
- 10 minutes (if continuing): Repeat benzodiazepine (same dose)
- 15 minutes: Call senior help, prepare IV phenytoin 20mg/kg or IV levetiracetam 40mg/kg
- 25 minutes: Second-line IV AED, consider ICU transfer

🚩 Red Flags for Urgent Referral
- Focal neurological signs post-ictally (>Todd's paresis duration)
- Developmental regression or loss of skills
- Myoclonic seizures in infancy (consider infantile spasms-hypsarrhythmia on EEG)
- Seizures <6 months age (structural/metabolic cause likely)
Rescue Medication (Home Management)
- Buccal midazolam: First-line, 0.5mg/kg (1-3 months: 2.5mg; 3-12 months: 2.5mg; 1-5 years: 5mg; 5-10 years: 7.5mg; 10+ years: 10mg)
- Give after 5 minutes of seizure, call ambulance if no response in 5 minutes
Analysis Framework
AED Selection Decision Tree
When to Avoid Specific AEDs
| AED | AVOID in | Reason |
|---|---|---|
| Carbamazepine | Generalised epilepsies, myoclonic/absence | May worsen seizures |
| Sodium Valproate | Females (unless no alternative) | Teratogenicity, neurodevelopmental risk |
| Phenytoin | Routine use | Narrow therapeutic index, cosmetic effects |
| Lamotrigine | Myoclonic seizures | May exacerbate myoclonus |
Key Points Summary
✓ Epilepsy diagnosis: ≥2 unprovoked seizures >24h apart; seizure classification determines AED choice
✓ Status epilepticus: Treat after 5 minutes-buccal midazolam 0.5mg/kg or IV lorazepam 0.1mg/kg
✓ Sodium valproate: Most effective for generalised epilepsies but contraindicated in females of childbearing potential (10% teratogenicity)
✓ Focal seizures: Carbamazepine or levetiracetam first-line; never use carbamazepine for generalised epilepsy
✓ Absence seizures: Ethosuximide first-line; brief (<10s) staring with 3Hz spike-wave on EEG
✓ Refer to specialist: All new diagnoses, treatment failure, age <1 year, diagnostic uncertainty
✓ Rescue medication: Buccal midazolam at 5 minutes, call ambulance if no response by 10 minutes total
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

