Tetanus: Pathophysiology - Spore Wars
- Agent: Clostridium tetani (anaerobic); spores in soil, dust, feces.
- Toxin: Tetanospasmin (neurotoxin).
- Pathogenesis:
- Spores enter wound → germinate.
- Toxin via retrograde axonal transport to CNS.
- Inhibits glycine & GABA release (Renshaw cells) → disinhibition.
- Manifestations: Incubation 3-21 days.
- Trismus (lockjaw), risus sardonicus, opisthotonus.
- Autonomic dysfunction.
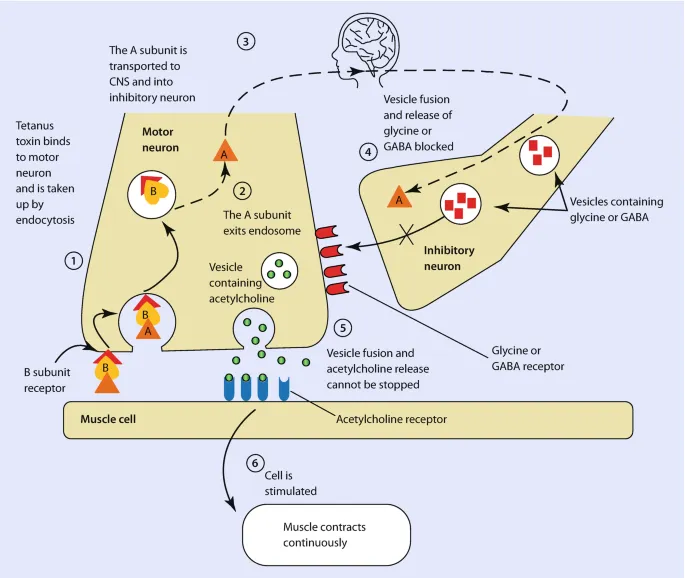
⭐ Tetanospasmin, the neurotoxin from Clostridium tetani, acts by blocking the release of inhibitory neurotransmitters (GABA and glycine) in the central nervous system, leading to unopposed muscle contraction and spasm.
Tetanus: Wound Risk - Danger Zones
Understanding wound type is crucial for appropriate tetanus prophylaxis.
| Feature | Clean Minor Wounds | Tetanus-Prone Wounds |
|---|---|---|
| Age of Wound | <6 hours | >6 hours |
| Depth | Superficial, <1 cm | >1 cm |
| Configuration | Linear | Stellate, avulsion, puncture |
| Tissue Viability | Healthy | Devitalized tissue |
| Contamination | Minimal | Soil, feces, saliva, foreign body, GSW |
| Other | Crush injuries, burns, frostbite, open fractures, denervated/ischemic tissue, septic abortion |
⭐ Wounds older than 6 hours, or those with devitalized tissue, contaminants (soil, feces, saliva), puncture type, crush injury, burns, or frostbite are considered tetanus-prone.
Tetanus: Immunization - Shot Sleuthing
- Primary Immunization:
- Childhood: 3 doses (DTP/DT/TT).
- Adults: 3 doses (Td/Tdap).
- Booster Doses:
- Every 10 years.
- Every 5 years for tetanus-prone wound if last dose >5 years ago.
- History: Documented vs. unreliable. Serological testing not routine.
⭐ A patient is adequately immunized if they have documented completion of a primary series of at least 3 doses of tetanus toxoid-containing vaccine, with the last dose within 10 years (or 5 years for a tetanus-prone wound).
Tetanus: Prophylaxis Protocol - Guard Up!
Key Agents for Prophylaxis:
- Active Immunity: Tetanus Toxoid (TT/Td/Tdap) 0.5 mL IM.
- Passive Immunity: Tetanus Immunoglobulin (TIG).
- Human (hTIG): 250 IU IM.
- Equine: 1500-3000 IU IM (after sensitivity test).
- 📌 Administer TT & TIG at separate sites if both indicated.
Categorize wound: Clean/Minor vs. Tetanus-Prone (e.g., contaminated with dirt/faeces/saliva, devitalized tissue, >6h old, puncture, avulsion, crush, burn, frostbite).
⭐ For a tetanus-prone wound in a patient with unknown or incomplete (<3 doses) vaccination history, both Tetanus Toxoid (e.g., Td 0.5 mL IM) and Tetanus Immunoglobulin (TIG 250 IU IM for human) should be administered at separate sites.
Tetanus: Special Cases - Handle with Care
- Pregnancy: Tdap preferred, ideally 27-36 weeks (2nd/3rd trimester); Td if Tdap unavailable.
⭐ Tdap in each pregnancy (27-36 weeks) gives neonatal passive immunity (tetanus, diphtheria, pertussis).
- HIV/Immunocompromised: Full primary series + boosters. TIG per guidelines; response may be suboptimal.
- Incomplete/Unknown History: Treat as unimmunized (<3 doses).
- Elderly: Standard guidelines; consider immunosenescence.
- Prior Vaccine Reaction: Assess severity; specialist consultation if severe_
High‑Yield Points - ⚡ Biggest Takeaways
- Clean minor wounds: If <3 doses or unknown history, give Td. If ≥3 doses, Td only if >10 years since last dose.
- All other wounds (dirty/major): If <3 doses or unknown, give Td + TIG. If ≥3 doses, Td if >5 years since last dose.
- TIG (Tetanus Immunoglobulin): Standard prophylactic dose is 250 IU IM.
- Full primary immunization: Requires three properly spaced doses of tetanus toxoid.
- Booster doses: Every 10 years routinely; or after 5 years for tetanus-prone wounds in immunized individuals.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

