STI Classification - Skin Deep Trouble
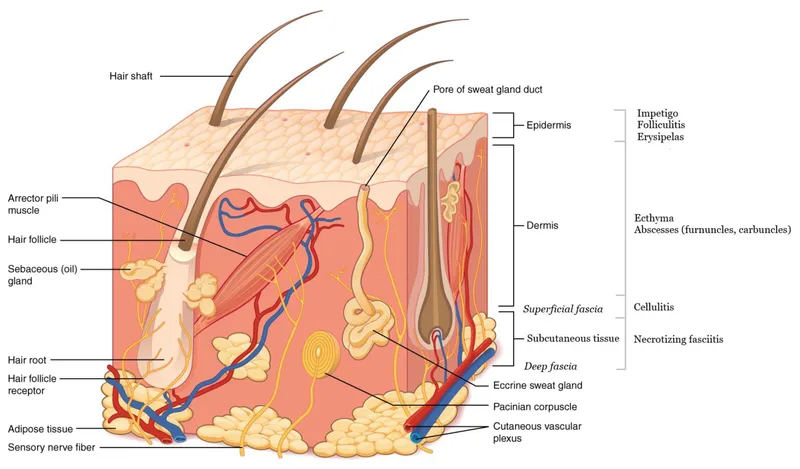
- Superficial Infections (Epidermis/Dermis):
- Impetigo: Epidermal infection, honey-colored crusts.
- Erysipelas: Dermal, superficial lymphatics; well-demarcated, raised, erythematous.
- Cellulitis: Deeper dermis, subcutaneous tissue; ill-defined borders, spreading.
- Deeper Infections (Subcutaneous/Fascia/Muscle):
- Cutaneous Abscess: Localized pus in dermis/subcutaneous tissue.
- Necrotizing Fasciitis: Rapidly progressive, involves fascia; surgical emergency!
- Myositis/Pyomyositis: Muscle inflammation/abscess.
⭐ Fournier's gangrene is a type of necrotizing fasciitis affecting the perineal, genital, or perianal regions, often polymicrobial.
Microbiology & Risks - The Nasty Crew
- Causative Agents:
- Staphylococcus aureus (MSSA/MRSA): Most common.
- Streptococcus pyogenes (GAS): Cellulitis, erysipelas, necrotizing fasciitis.
- Gram-negatives (Pseudomonas, E. coli): Immunocompromised, burns, diabetic foot infections.
- Anaerobes (Clostridium, Bacteroides): Gas gangrene, deep abscesses.
- Polymicrobial infections are frequent.
- Patient Vulnerabilities:
- Skin barrier disruption: Trauma, surgery, bites, IV catheters.
- Impaired immunity: Diabetes Mellitus (DM), PVD, steroids, HIV.
- Systemic factors: Obesity, malnutrition, lymphedema, extremes of age.
⭐ Clostridium perfringens is notorious for causing gas gangrene, characterized by crepitus and rapid tissue destruction.
Diagnosis & Scoring - Red Alert Signs
- Clinical: History, exam (local signs: erythema, warmth, tenderness, fluctuance).
- LRINEC Score (Lab Risk Indicator for Necrotizing Fasciitis):
- Parameters: CRP >150, WBC >15, Hb <13.5, Na <135, Creatinine >1.6, Glucose >180.
- Interpretation: <6 (low risk), 6-7 (intermediate), ≥8 (high risk NF).
- Red Alerts (Suspect NF):
- Pain out of proportion
- Tense edema, bullae, skin necrosis
- Crepitus (gas)
- Systemic toxicity (fever, ↑HR, ↓BP)
- Wooden-hard induration
- Rapid progression despite antibiotics
- Serum lactate >2 mmol/L
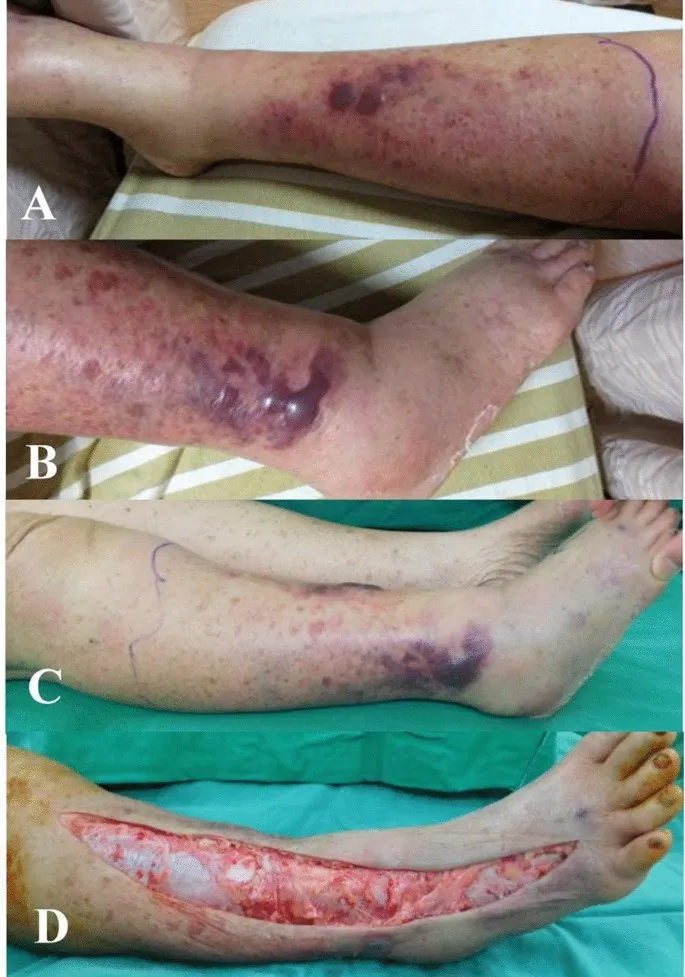
⭐ Pain out of proportion to clinical findings is a key early indicator of necrotizing fasciitis.
Treatment Strategies - Slash & Dose
Primary goals: control infection, prevent spread, preserve function.
- Slash (Surgery):
- I&D: For abscesses.
- Debridement: Aggressive removal of ALL non-viable tissue; crucial for necrotizing infections. Re-look PRN.
- Fasciotomy: If compartment syndrome.
- Dose (Antibiotics):
- Empirical: Broad-spectrum IV (e.g., Vancomycin + Piperacillin-Tazobactam). Add Clindamycin for toxin suppression (📌).
- Definitive: Tailor to C&S.
- Supportive: Fluids, nutrition, tetanus toxoid. HBO for clostridial myonecrosis/severe NF.
⭐ Early, aggressive surgical debridement is the single most important determinant of outcome in necrotizing soft tissue infections.
Key STIs - Deadly Details
- Necrotizing Fasciitis (NF):
- "Flesh-eating"; rapid fascial spread.
- Type I (polymicrobial), Type II (GAS).
- Severe pain out of proportion, crepitus, bullae. LRINEC >6.
- Tx: Aggressive surgical debridement, broad-spectrum Abx.
- Gas Gangrene (Clostridial Myonecrosis):
- C. perfringens (alpha-toxin); muscle necrosis, gas.
- Bronze skin, foul odor, crepitus.
- Tx: Debridement, Penicillin + Clindamycin, HBO.
- Fournier's Gangrene:
- NF of perineum/genitalia; polymicrobial.
- Rapid onset, pain, swelling, crepitus, necrosis.
- Tx: Urgent debridement, broad-spectrum Abx.
⭐ > Fournier's gangrene carries high mortality (20-40%) despite aggressive therapy, often linked to diabetes.

High‑Yield Points - ⚡ Biggest Takeaways
- Cellulitis: common S. pyogenes; erysipelas is superficial with sharply demarcated borders.
- Skin abscesses: typically S. aureus (MRSA), require incision and drainage (I&D).
- Necrotizing fasciitis: surgical emergency needing urgent, wide debridement. Fournier's gangrene affects the perineum.
- Gas gangrene (C. perfringens): presents with crepitus, muscle necrosis; requires surgery & antibiotics.
- Diabetic foot infections: often polymicrobial, need aggressive debridement, broad-spectrum antibiotics.
- Bite wounds (Pasteurella, Eikenella) often warrant prophylactic amoxicillin-clavulanate.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

