Biofilm Basics - Slime Shields Up!
- Structured microbial communities, adherent to surfaces, encased in a self-produced Extracellular Polymeric Substance (EPS).
- EPS: Protective "slime layer" of polysaccharides, proteins, eDNA, and lipids. Shields embedded cells.
- Readily attach to biotic (e.g., tissues) and abiotic surfaces (e.g., catheters, implants).
- Key features:
- Significantly ↑ antimicrobial resistance (often 100-1000x).
- Effective evasion of host immune responses (e.g., phagocytosis).
- Major cause of persistent, chronic infections.
- Quorum Sensing (QS): Bacterial cell-to-cell communication; regulates biofilm architecture, development, and virulence.
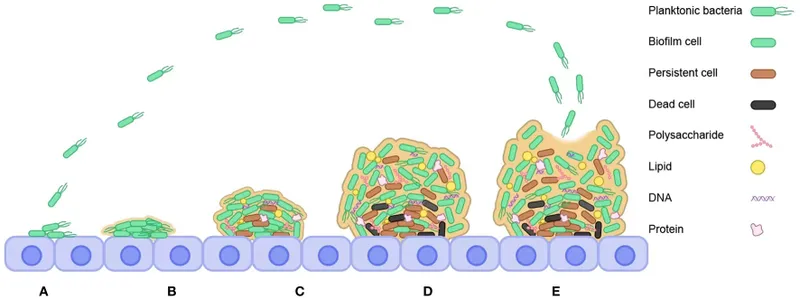
⭐ Biofilms are implicated in approximately 65% of all microbial infections and up to 80% of chronic infections treated by physicians in the developed world.
Implants & Infections - Unwanted Guests
- Implants: Foreign bodies, non-vascularized, susceptible to microbial colonization.
- Biofilm Formation: Key to persistent implant infections.
- Attachment: Initial microbial adhesion ("Race to the surface").
- Proliferation & Matrix Production: Slimy glycocalyx (EPS - extracellular polymeric substance) protects bacteria.
- Quorum Sensing: Bacterial communication, coordinates biofilm development.
- Detachment: Dispersal of bacteria, potential for systemic spread.
- Common Culprits: Staphylococcus epidermidis (most common), Staphylococcus aureus.
- Challenges: ↑ Antibiotic resistance within biofilms, difficult to eradicate without implant removal.
⭐ Biofilms can make bacteria up to 1000x more resistant to antibiotics compared to their planktonic (free-floating) counterparts.
- Prevention: Sterile technique, antibiotic-coated implants, perioperative antibiotics.
- Diagnosis: Clinical signs, imaging, cultures (sonication of implant).
Clinical Clues & Diagnosis - Spotting the Stealth
- Presentation: Often insidious & delayed (weeks to years).
- Persistent pain, erythema, warmth, swelling at implant site.
- Low-grade fever (may be absent).
- Chronic draining sinus tract: highly suggestive.
- Implant loosening, instability, or mechanical failure.
- Recurrent infection despite prior antibiotic courses.
- Challenges:
- Routine cultures frequently negative (bacteria within biofilm).
- Inflammatory markers (ESR, CRP) can be normal or mildly elevated.
- Diagnostic Pathway:
⭐ Sonication of explanted prosthetic material significantly increases diagnostic yield in prosthetic joint infections (PJIs) by disrupting biofilm and releasing bacteria for culture.
- Key Samples:
- Aspirated fluid (joint, bursa).
- Multiple (≥3, ideally 5-6) intraoperative tissue samples from implant interface.
- Explanted implant itself (for sonication).
- 📌 MSIS Criteria for PJI: Often used for diagnosis (Major/Minor criteria).
Tackling Biofilms - Breaking Barriers
- Prevention:
- Strict aseptic technique.
- Antimicrobial-coated implants (silver, antibiotics).
- Implant surface modification.
- Disruption/Eradication: 📌 Mnemonic: Surgical Debridement, Chemicals, Antibiotics, Removal (SCAR)
- Mechanical: Debridement, sonication, lavage.
- Chemical: Dispersants (DNase), chelators (EDTA), quorum sensing inhibitors (QSIs).
- Antibiotics: High local dose, combination therapy (rifampicin crucial for Staph).
- Implant Management:
- DAIR: Early infection (<4 wks post-op / <3 wks symptoms), stable implant.
- Exchange:
- One-stage: Single surgery.
- Two-stage: Gold standard for chronic PJI; spacer + antibiotics (6-8 wks) then reimplantation.
- Implant removal.
⭐ Rifampicin is key against staphylococcal biofilms; never use as monotherapy due to rapid resistance. Combine with another agent.
High‑Yield Points - ⚡ Biggest Takeaways
- Biofilms: Structured microbial communities in self-produced EPS matrix on implants, highly resistant to antibiotics.
- Resistance due to EPS barrier, slow bacterial growth, and presence of persister cells within the biofilm.
- Quorum sensing coordinates biofilm formation and the expression of virulence factors.
- Staphylococcus epidermidis and S. aureus are primary pathogens in implant-related infections.
- Diagnosis: Sonication of explanted device for culture is the most sensitive method for detecting biofilm bacteria.
- Treatment: Often requires complete implant removal combined with prolonged, high-dose systemic antibiotics.
- Prevention: Strict aseptic techniques during surgery and use of antimicrobial-coated implants are crucial measures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

