Pancreatectomy Basics - Pancreas Prep & Plan
- Key Indications:
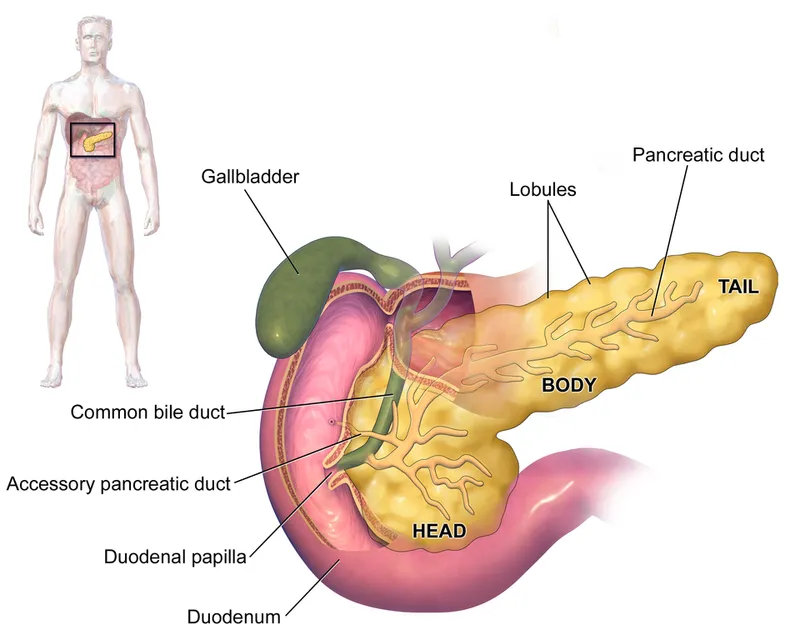
- Malignant: Pancreatic Ductal Adenocarcinoma (PDAC), ampullary Ca, distal Common Bile Duct (CBD) Ca, duodenal Ca.
- Benign/Premalignant: Intraductal Papillary Mucinous Neoplasm (IPMN) (high-risk features), Mucinous Cystic Neoplasm (MCN), Serous Cystadenoma (SCN) (symptomatic/large), Neuroendocrine Tumors (NETs), chronic pancreatitis (selected cases, e.g., intractable pain, mass).
- Trauma: Severe pancreatic ductal injury.
- Essential Pre-operative Workup:
- Imaging (Staging & Resectability): High-resolution pancreatic protocol CT or MRI (evaluates tumor extent, vascular involvement: SMV/Portal Vein, SMA, celiac axis).
- Tissue Diagnosis: Endoscopic Ultrasound (EUS) + Fine Needle Aspiration (FNA) for suspicious lesions.
- Laboratory: CA 19-9 (baseline, prognostic), Liver Function Tests (LFTs), coagulation profile, nutritional status (e.g., albumin).
- Optimization: Nutritional support (oral/enteral/parenteral), smoking cessation, manage comorbidities.
- Biliary Drainage (ERCP/PTBD): Indicated for cholangitis, symptomatic jaundice, or if total bilirubin >10-15 mg/dL with anticipated significant surgical delay.
- Broad Classification of Pancreatectomies:
- Resections of Head: Pancreaticoduodenectomy (Whipple procedure), Pylorus-Preserving Pancreaticoduodenectomy (PPPD).
- Resections of Body/Tail: Distal Pancreatectomy (often with splenectomy for oncologic indications).
- Total Pancreatectomy: For diffuse disease or multifocal tumors.
- Parenchyma-Sparing: Enucleation (for small, benign, superficial tumors like insulinomas), Central Pancreatectomy (for lesions in pancreatic neck/proximal body).
⭐ Pancreaticoduodenectomy (Whipple procedure) is the standard operation for resectable cancer of the head of the pancreas.
Major Resections - Whipple & Distal Showdown
-
Whipple Procedure (Pancreaticoduodenectomy)
- Resection: Pancreatic head, duodenum, prox. jejunum, gallbladder, distal CBD, +/- antrum.
- Reconstruction (📌 P-H-G): Pancreaticojejunostomy (PJ) (critical), Hepaticojejunostomy (HJ), Gastrojejunostomy/Duodenojejunostomy (GJ/DJ).
- Variants: Classic vs. Pylorus-Preserving (PPPD).

-
Distal Pancreatectomy
- Indications: Body/tail lesions (tumors, cysts).
- Spleen Management:
- Preservation (benign/low-grade): Kimura (splenic vessels preserved), Warshaw (relies on short gastrics).
- Splenectomy: For malignant tumors or direct splenic/vascular involvement.

⭐ The order of anastomosis in Whipple's procedure typically starts with the pancreaticojejunostomy, considered the most critical and prone to leakage.
- Comparative Overview: Whipple vs. Distal
| Feature | Whipple Procedure | Distal Pancreatectomy |
|---|---|---|
| Key Indications | Pancreatic head/periampullary tumors | Pancreatic body/tail lesions |
| Resected Structures | Pancreatic head, duodenum, GB, distal CBD, prox. jejunum | Pancreatic body/tail, +/- spleen |
| Major Anastomoses | PJ, HJ, GJ/DJ (typically 3) | Pancreaticojejunostomy (if duct transected) |
| Specific Complications | Delayed Gastric Emptying (DGE), Pancreatic Fistula (POPF), Biliary Leak | POPF, Splenic issues (if preserved), Abscess |
Other Techniques & Complications - Niche Slices & Fallouts
- Central Pancreatectomy:
- Indications: Benign/low-grade tumors in neck/body.
- Goal: Preserve pancreatic function.
- Reconstruction: Pancreaticojejunostomy/-gastrostomy to distal remnant.
- Total Pancreatectomy:
- Indications: Diffuse disease (multifocal IPMN, extensive PDAC).
- Consequences: Brittle diabetes (insulin), exocrine insufficiency (enzymes).
- Enucleation:
- Indications: Small (<2-3 cm) benign, superficial tumors (insulinoma) distant from main duct.
- Surgical Approaches:
- Open: Standard.
- Laparoscopic: Minimally invasive, ↓recovery; learning curve.
- Robotic: Enhanced vision/dexterity; ↑cost, learning curve.
- Key Complications: 📌
- Pancreatic Fistula (POPF): Drain amylase >3x serum ULN on/after POD3.

Grade Definition (ISGPS) Clinical Impact A Biochemical leak, no impact No change B Needs management change, <50% organ failure Abx, NPO, TPN, drains, intervention C Major change, >50% organ failure ICU, re-op, sepsis, mortality risk - Delayed Gastric Emptying (DGE): ISGPS Grades A,B,C.
- Post-Pancreatectomy Hemorrhage (PPH): ISGPS Grades A,B,C (early <24h, late >24h).
- Infections: Abscess, cholangitis.
- Chyle Leak: Lymphatic collection.
- Long-term: Endocrine & exocrine insufficiency.
- Pancreatic Fistula (POPF): Drain amylase >3x serum ULN on/after POD3.
⭐ Clinically relevant pancreatic fistula (ISGPS Grade B/C) is the most common and feared complication after pancreatectomy, significantly impacting morbidity.
High‑Yield Points - ⚡ Biggest Takeaways
- Whipple procedure (PD): Standard for pancreatic head/periampullary cancers; major resection.
- Pylorus-Preserving PD (PPPD): Modifies Whipple to preserve pylorus, potentially reducing dumping syndrome.
- Distal pancreatectomy: For body/tail tumors; often includes splenectomy.
- Central pancreatectomy: For neck/proximal body benign/low-grade tumors; preserves pancreatic function.
- Total pancreatectomy: For extensive disease; causes insulin-dependent diabetes and malabsorption.
- Pancreatic fistula (POPF): Most common and serious complication after pancreatectomy.
- Reconstruction (Whipple): Involves pancreaticojejunostomy, hepaticojejunostomy, and gastro/duodenojejunostomy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

