Definition, Etiology & Epidemiology - Pancreas Under Siege
- Definition: Chronic, progressive, irreversible inflammatory disease of the pancreas, characterized by parenchymal fibrosis, ductal changes, and loss of exocrine/endocrine function.
- Etiology:
- Alcohol abuse: Predominant cause (India: ~60-70%).
- Tropical pancreatitis: Significant in specific Indian regions.
- 📌 TIGAR-O classification guides etiological assessment (Toxic-metabolic, Idiopathic, Genetic, Autoimmune, Recurrent/severe AP, Obstructive).
- Epidemiology: Indian prevalence: ~120-140 per 100,000 population. Marked male predominance.

⭐ Alcohol and tropical pancreatitis are the leading causes of chronic pancreatitis in the Indian subcontinent.
Pathophysiology & Clinical Features - Scarred & Sore
-
Pathophysiology:
- Recurrent inflammation & ductal obstruction (stones, strictures) → ↑ intraductal pressure.
- Progressive pancreatic fibrosis, acinar atrophy, calcification.
- Neural hypertrophy & perineural inflammation cause chronic pain.
- Islet cell destruction → endocrine insufficiency (diabetes).
-
Clinical Features:
- Pain: Dominant; severe, persistent epigastric, radiates to back. Postprandial, relieved by leaning forward. 📌
- Malabsorption: Steatorrhea (bulky, foul stools), weight loss, fat-soluble vitamin (A,D,E,K) deficiency.
- Diabetes Mellitus (Type 3c): Pancreatogenic; often brittle, late feature.
- Nausea, vomiting.

⭐ Pain in chronic pancreatitis is often relentless and multifactorial, significantly impacting quality of life and being notoriously difficult to manage effectively.
Diagnosis & Staging - Spotting the Damage
- Imaging First:
- CT: Calcifications, ductal dilatation, atrophy.
- MRCP: Ductal map (strictures, stones).
- EUS: Most sensitive for early changes (parenchymal/ductal).
- Function Tests:
- Direct: Secretin test (gold standard).
- Indirect: Fecal elastase-1 (< 200 µg/g indicates insufficiency), serum trypsinogen.
- Severity Staging:
- Cambridge classification (ERCP/MRCP based).
- M-ANNHEIM score (multifactorial).
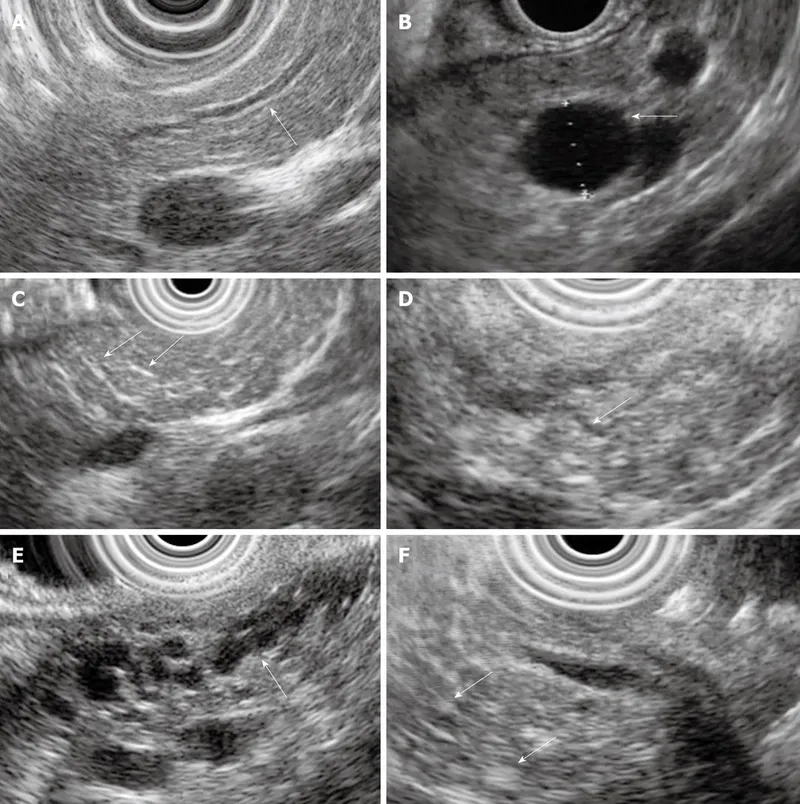
⭐ EUS is the most sensitive imaging modality for detecting early changes of chronic pancreatitis.
Complications of Chronic Pancreatitis - When It Gets Worse
- Pseudocysts: Fluid collections; risk of pain, infection, rupture.
- Biliary obstruction: Jaundice, pruritus, cholangitis.
- Duodenal stenosis/obstruction: Gastric outlet obstruction symptoms.
- Vascular complications:
- Pseudoaneurysms (e.g., splenic artery).
- Venous thrombosis (splenic, portal) → sinistral portal hypertension.
- Pancreatic ascites/pleural effusion (due to ductal disruption/fistula).
- Exocrine insufficiency: Steatorrhea, maldigestion, weight loss.
- Endocrine insufficiency: Pancreatogenic diabetes (Type 3c DM).
- Chronic pain: Often severe, debilitating.
- Pancreatic cancer: Risk significantly ↑.

⭐ Splenic vein thrombosis, a known complication, can cause isolated gastric varices (due to sinistral portal hypertension) leading to upper GI bleeding without esophageal varices typically seen in generalized portal hypertension.
Management (Medical, Endo, Surgical) - Taming the Flame
- Medical Management:
- Pain: Analgesia (WHO ladder), adjuncts (pregabalin).
- Exocrine: PERT (25,000-40,000 U lipase/meal). Low-fat diet.
- Lifestyle: Alcohol/smoking cessation.
- Endoscopic Therapy (ET):
- Indications: MPD stones, dominant strictures.
- Procedures: ERCP (sphincterotomy, stone removal, stenting).
- Pain: Celiac Plexus Neurolysis (CPN).
- Surgical Therapy:
- Indications: Intractable pain, complications (obstruction, malignancy suspicion), failed med/endo.
- Drainage (MPD >6-7mm): Puestow (LPJ), Frey (LPJ + head coring).
- Resection (head mass, non-dilated duct): Whipple, Beger, Distal Pancreatectomy.
⭐ Frey procedure combines pancreatic head excavation with lateral pancreaticojejunostomy, ideal for painful chronic pancreatitis with inflammatory head mass & dilated MPD.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common cause: Alcohol abuse; tropical pancreatitis also significant in India.
- Hallmark symptom: Chronic epigastric pain radiating to the back, often postprandial.
- Classic triad: Pancreatic calcification (pathognomonic), steatorrhea, and diabetes mellitus (late).
- Diagnosis: CT scan is gold standard (calcifications, ductal changes); MRCP for ductal anatomy.
- Key complications: Pseudocysts, biliary/duodenal obstruction, splenic vein thrombosis, pancreatic cancer risk ↑.
- Surgical indications: Intractable pain, failed medical/endoscopic therapy, or complications. Frey's procedure is common.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

