Principles of Oncologic Surveillance - Watching the Horizon
- Core Goals: Early detection of cancer recurrence (local, regional, distant), new primary malignancies, & management of treatment-related complications.
- Benefits: Aims to improve overall survival & quality of life (QoL); provides patient reassurance.
- Methods Include:
- Regular history & physical examination (H&P).
- Scheduled imaging (e.g., CT, MRI, PET scans).
- Tumor markers (e.g., CEA, PSA).
- Endoscopic procedures (site-specific).
- Frequency: Tailored to cancer type, stage, & individual risk. Typically more intensive initially (e.g., every 3-6 months for 2-3 years), then decreases.
- Key Principle: Individualized surveillance strategy is paramount.
⭐ Surveillance is most effective when it detects asymptomatic, treatable recurrences or second primary cancers.
Surveillance Tools & Techniques - The Detective's Kit
- Clinical Assessment: Cornerstone; regular history & physical exam (H&P).
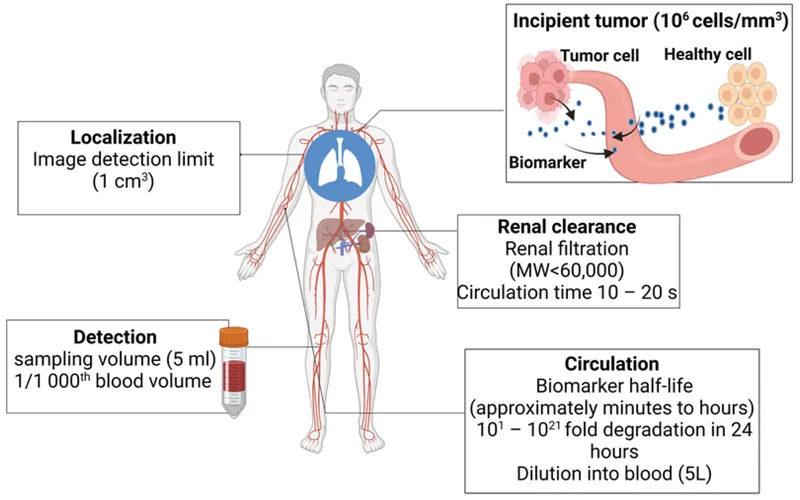
- Tumor Markers (Blood Tests): Monitor trends, not just absolute values.
- CEA: Colorectal, medullary thyroid.
- AFP: Hepatocellular Carcinoma (HCC), non-seminomatous germ cell tumors.
- CA 19-9: Pancreatic, cholangiocarcinoma.
- CA-125: Ovarian cancer.
- PSA: Prostate cancer.
- hCG: Germ cell tumors.
- Imaging Studies: Tailored to cancer type & risk.
- Ultrasound (USG): Initial, accessible (e.g., liver, nodes, thyroid).
- Contrast-Enhanced CT (CECT): Chest/Abdomen/Pelvis (CAP) - standard for metastases.
- MRI: Superior for specific sites (e.g., brain, liver, rectal cancer restaging).
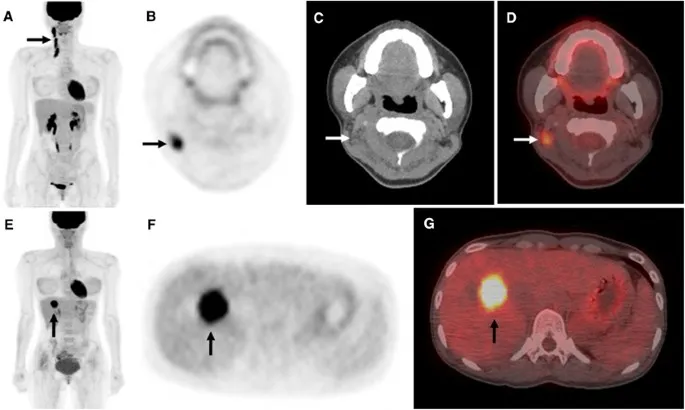
- PET-CT (FDG): Detects metabolic activity, occult recurrence, treatment response.
- Endoscopic Procedures: Direct visualization & biopsy capability.
- Colonoscopy (Colorectal), Upper GI Endoscopy (Gastric/Esophageal), Bronchoscopy (Lung).
- Pathology: Biopsy/FNAC of suspicious lesions confirms recurrence.
⭐ PET-CT can identify occult metastases or unsuspected recurrence, changing management in approximately 15-30% of patients being re-evaluated for various cancers after primary treatment.
Site-Specific Surveillance Snippets - Cancer Case Files
- Breast Cancer (Post-Tx):
- H&P: q3-6mo for 2yrs, q6-12mo for 3yrs, then annually.
- Mammogram: Annually. Routine tumor markers (CEA, CA15-3) NOT recommended for asymptomatic surveillance.
- Bone density scan: Consider if on Aromatase Inhibitors (AIs).
- Colorectal Cancer (CRC) (Post-Resection Stage II/III):
- H&P, CEA: q3-6mo for 2yrs, then q6mo for 3yrs (total 5yrs).
- CT C/A/P: Annually for 3-5 years (high-risk Stage II and Stage III).
- Colonoscopy: 1yr post-op. If normal, then in 3yrs. If normal, then q5yrs.
⭐ Lynch syndrome: Annual colonoscopy from age 20-25 or 2-5 yrs prior to earliest family CRC diagnosis.
- Oral Cavity Cancer (Post-Tx):
- H&P, oral exam: q1-3mo (yr1); q2-6mo (yr2); q4-8mo (yrs3-5); annually (after 5yr).
- Imaging (CT/MRI/PET): Baseline post-Tx scan, then clinically indicated. Regular dental eval (e.g., q6mo).
- Cervical Cancer (Post-Tx):
- H&P, pelvic exam: q3-6mo for 2yrs, q6-12mo for 3yrs, then annually.
- Pap smear (if cervix present) or vault smear (post-hysterectomy): Follow pelvic exam schedule.
Recurrence & Survivorship Care - The Next Chapter
- Recurrence: Cancer reappearance after initial treatment-induced remission.
- Types: Local (at primary site), Regional (lymph nodes), Distant (metastasis).
- Detection: Vigilant follow-up (history, physical exam, imaging like PET-CT, tumor markers e.g., CEA, CA-125).
- Management: Individualized; may involve re-surgery, salvage chemotherapy/radiotherapy, or palliative care.
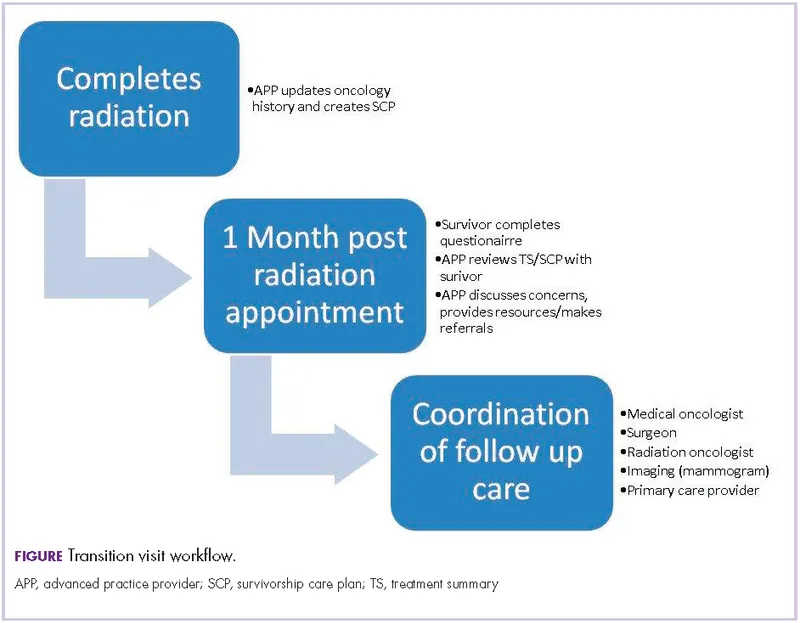
- Survivorship Care Plan (SCP): Comprehensive approach for post-treatment well-being.
- Surveillance: For recurrence, second primary malignancies.
- Late Effects Management: Chronic pain, fatigue, lymphedema, cardiotoxicity, neurocognitive issues, psychosocial distress.
- Health Promotion: Diet, exercise, smoking cessation.
- Care Coordination: Oncologists, PCP, specialists.
- Emphasis on Quality of Life (QoL) and functional recovery.
⭐ Most solid tumor recurrences manifest within the first 2-5 years after primary treatment completion.
High‑Yield Points - ⚡ Biggest Takeaways
- Goals: Detect recurrence (local/distant), manage sequelae, screen for second primaries.
- Frequency: Intense early (q3-6mo, 2-3 yrs), then less (annually post 5 yrs), varies by cancer.
- Methods: Clinical exam, tumor markers (CEA, PSA, CA-125), imaging (CT, PET).
- Tumor Markers: Monitor response/recurrence; rising trend often precedes clinical signs.
- Imaging: For symptoms, ↑ markers, or protocol-based surveillance in high-risk cases.
- Second Primaries: Survivors at increased risk; requires specific, ongoing screening.
- Adherence: Crucial for early detection, impacting prognosis and survivorship care.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

