Neck Anatomy Essentials - Anatomy Unveiled
- Fascial Layers: Define surgical planes, limit infection spread.
- Superficial: Platysma, cutaneous nerves, vessels.
- Deep cervical fascia:
- Investing: Encases Sternocleidomastoid (SCM) & trapezius.
- Pretracheal (middle): Visceral compartment (thyroid, trachea, esophagus).
- Prevertebral (deep): Surrounds vertebral column, deep neck muscles.
- Carotid sheath: Contains Common/Internal Carotid Artery (CCA/ICA), Internal Jugular Vein (IJV), Vagus n. (CN X).
- Triangles: Key surgical landmarks.
- Anterior: Bounded by SCM, mandible, midline. Contents: Thyroid, larynx, carotid system.
- Posterior: Bounded by SCM, trapezius, clavicle. Contents: Cranial Nerve XI (Accessory n.), brachial plexus trunks, subclavian artery.
- Danger Spaces:
- Prevertebral & Retropharyngeal: Potential for infection spread to mediastinum.
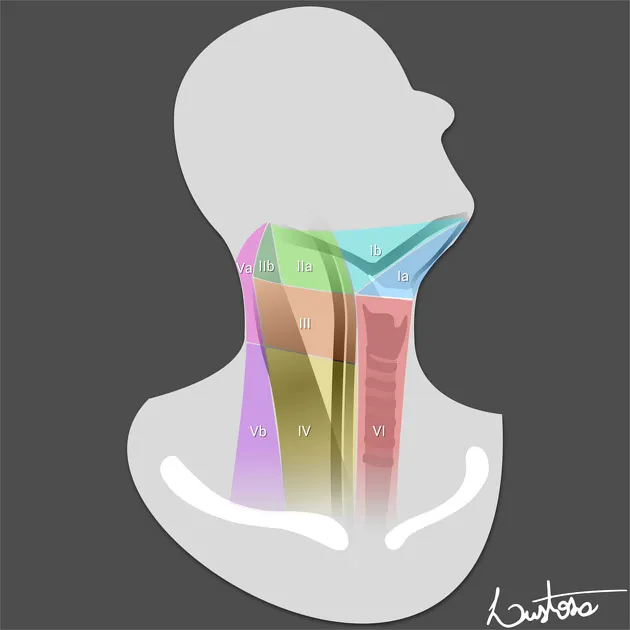
- Lymph Node Levels (I-VII): Crucial for oncologic staging & guiding neck dissection.
⭐ The Spinal Accessory Nerve (CN XI) is particularly vulnerable during posterior triangle dissections; its injury causes trapezius muscle weakness (shoulder droop, impaired arm abduction >90°).
 oka
oka
Neck Dissections Demystified - Lymph Node Lowdown
-
Goal: Remove cervical lymph nodes (LNs) for cancer staging/treatment. Classified by structures removed/preserved.
-
Key Structures: Sternocleidomastoid (SCM), Internal Jugular Vein (IJV), Spinal Accessory Nerve (SAN).
-
Types of Neck Dissection:
- Radical (RND): Removes LNs (Levels I-V), SCM, IJV, SAN.
- Modified Radical (MRND): Preserves ≥1 of SCM, IJV, SAN.
- Type I: SAN preserved.
- Type II: SAN, IJV preserved.
- Type III (Functional): SAN, IJV, SCM preserved.
- Selective (SND): Preserves SCM, IJV, SAN. Removes specific LN levels (e.g., Supraomohyoid: Levels I-III).
- Extended: RND + additional structures/LNs.

⭐ The Spinal Accessory Nerve (SAN) is the most commonly injured nerve during neck dissection, leading to trapezius muscle dysfunction and shoulder droop. Its preservation is a key goal in MRND and SND.
- Common LN Levels Targeted:
- I: Submental/Submandibular
- II: Upper Jugular
- III: Middle Jugular
- IV: Lower Jugular
- V: Posterior Triangle
Incision Insights - Cutting Edge Cuts
- Guiding Principles:
- Align with Langer's lines (RSTL) for best cosmesis & healing.
- Aim for adequate exposure, minimal tissue trauma.
- Protect vital neurovascular structures.
- Common Neck Incisions & Uses:
- Kocher (Collar): Transverse, ~2 fingerbreadths above clavicle; thyroid, parathyroid.

- Transverse Cervical: Single/double (MacFee for bilateral); neck dissections.
- Utility (Apron/Hockey-stick): Extensive resections, laryngectomy, RND.
- Frey's (Lazy S): Parotidectomy.
- Schobinger: Flap for RND; better cosmesis than Y-incisions.
- Kocher (Collar): Transverse, ~2 fingerbreadths above clavicle; thyroid, parathyroid.
- ⭐ High-Yield Fact:
MacFee incision consists of two parallel transverse incisions, preferred for bilateral neck dissections to improve cosmesis and reduce flap necrosis risk compared to a single large apron flap.
Post-Op Pitfalls - Healing Hurdles
- Hematoma/Seroma: Early: neck swelling, ↑ drain output. Mgmt: Small - observe; Large/Expanding - OR for evacuation.
- Surgical Site Infection (SSI): Signs: fever, erythema, pus. Mgmt: Antibiotics, drainage. Prophylaxis is key.
- Nerve Injury:
- Recurrent Laryngeal (RLN): Hoarseness (unilat), stridor (bilat).
- Superior Laryngeal (SLN): Voice fatigue, ↓ pitch.
- Marginal Mandibular: Drooping mouth corner.
- Spinal Accessory: Shoulder droop, weak abduction.
- Chyle Leak: Milky drain output (Triglycerides > 110 mg/dL). Mgmt: Conservative (low-fat diet, octreotide), pressure dressing; surgical if persistent (> 500-600 mL/day).
⭐ Chyle leaks are more common on the left side due to thoracic duct anatomy.
- Wound Dehiscence/Fistula: Risks: radiation, poor nutrition. Mgmt: Local care, nutritional support, possible flap.

📌 Mnemonic for common nerve injuries: "MARS" - Marginal mandibular, Accessory (Spinal), Recurrent laryngeal, Superior laryngeal.
High‑Yield Points - ⚡ Biggest Takeaways
- Kocher's incision: Transverse, for thyroid/parathyroid surgery; good cosmesis.
- Crile (Hockey-stick) incision: Along SCM anterior border; for Radical Neck Dissection (RND).
- MacFee incision: Parallel transverse incisions for bilateral RND; skin bridge sparing.
- Utility (Apron/H) incision: Wide exposure for laryngectomy with neck dissection.
- Minimally invasive: TORS/TLM for select H&N tumors; no external scars.
- Nerve injury risks: Marginal mandibular, spinal accessory, hypoglossal.
- Incision choice: Based on pathology, neck dissection, cosmesis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

