Extravasation of Contrast Media - Uh Oh, It Leaked!
- Leakage of IV contrast into surrounding soft tissues.
- Incidence: 0.1-0.9%; ↑ with high-osmolar contrast media (HOCM), power injectors, fragile veins.
- Symptoms: Pain, swelling, erythema at site. Severe: Compartment syndrome, tissue necrosis.
- Management:
- STOP injection immediately.
- Elevate affected limb.
- Apply warm or cold compresses (local policy).
- Observe; surgical consult if severe (e.g., large volume, skin changes).
- Prevention: Secure IV access, test flush with saline, monitor injection site.
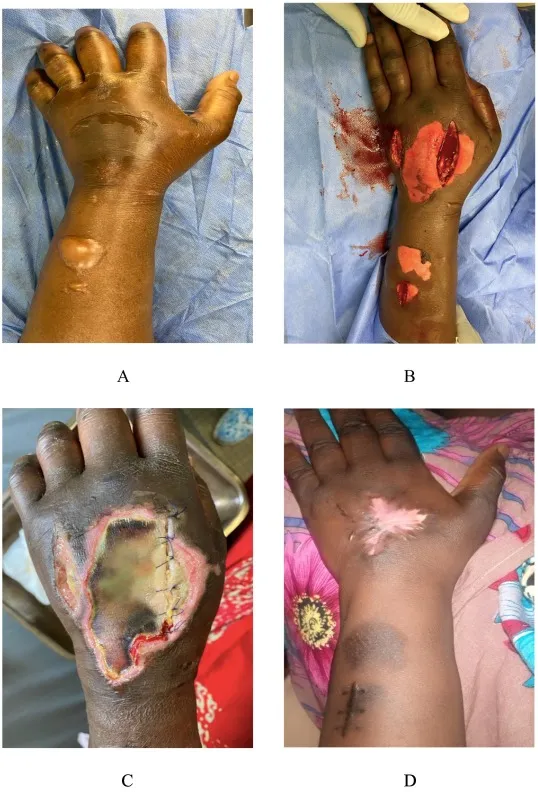
⭐ Most extravasations are minor; however, volumes >30ml (ionic contrast) or >100ml (non-ionic contrast) may warrant urgent surgical consultation, especially if skin blistering or altered tissue perfusion occurs.
Extravasation of Contrast Media - Vulnerability Scan
- Patient Factors:
- Age extremes (pediatric, geriatric)
- Impaired communication/sensation (e.g., neuropathy, altered sensorium)
- Fragile/compromised veins (e.g., chemotherapy, previous IV attempts, steroids)
- Peripheral vascular disease, diabetes
- Obesity, lymphedema
- Procedural Factors:
- Site: Hand, wrist, foot, ankle (↑ risk vs. antecubital fossa)
- Mismatched cannula/vein size; insecure cannula
- High injection rates/pressure (especially with power injector)
- Unattended injection; multiple puncture attempts
- Contrast Factors:
- Large volume
- High viscosity/osmolality
⭐ Patients unable to report pain (e.g., sedated, neuropathy, infants) have ↑ risk of severe extravasation due to delayed detection and larger volumes extravasated.
Extravasation of Contrast Media - Symptom Spotlight

- Immediate Symptoms (minutes to hours):
- Pain or burning sensation at injection site
- Swelling, erythema, tenderness
- Blistering (less common)
- ↓ skin temperature locally
- Delayed Symptoms (hours to days):
- Persistent pain, induration
- Skin ulceration or necrosis (rare, with large volumes or certain agents)
- Compartment syndrome (severe cases)
- Pathophysiology: Direct toxicity of contrast, osmotic effects, inflammatory response.
- Severity Assessment:
- Volume extravasated (small < 10 mL, moderate 10-50 mL, large > 50 mL for iodinated; < 30 mL vs > 30 mL for gadolinium)
- Type of contrast (ionic > non-ionic for severity)
- Patient factors (e.g., impaired circulation)
⭐ Most extravasations are minor and resolve with conservative management (elevation, cold/warm compresses). However, large volume extravasations (>30-50 mL of iodinated contrast, or >10 mL of vesicant contrast) can lead to severe complications like compartment syndrome or skin necrosis.
Extravasation of Contrast Media - Damage Control Mode
- Immediate Actions:
- Stop injection.
- Elevate limb.
- Cold compress (15-20 min, 3-4x/day, 24-48h).
- Attempt gentle aspiration, then remove IV.
- Notify physician, document (volume, type, site, symptoms).
- Monitor Closely:
- Neurovascular status (pulses, capillary refill, sensation).
- Skin: swelling, blistering, necrosis.
- ⚠️ Surgical Consult If:
- Volume >50-100 mL (agent dependent).
- Severe/progressive pain or swelling.
- Skin necrosis, ulceration, blistering.
- Signs of compartment syndrome (5 P's: Pain, Pallor, Paresthesia, Pulselessness, Paralysis - 📌 remember late signs).
- ↓ Tissue perfusion.
⭐ Compartment syndrome is a rare but limb-threatening emergency post-extravasation; characterized by pain out of proportion to injury. Fasciotomy may be required.
Extravasation of Contrast Media - Stop It Before It Starts
- Prevention is Key:
- Assess risk: prior reactions, eGFR, IV quality.
- Use 18-20G cannula; antecubital vein preferred.
- Warm contrast; test patency with saline.
- Monitor site; ensure patient reports discomfort.
⭐ Confirm IV patency with saline flush before power injection to significantly reduce extravasation risk.
High‑Yield Points - ⚡ Biggest Takeaways
- Extravasation is the leakage of IV contrast into surrounding soft tissues.
- Key risk factors: fragile veins (elderly/children), high injection pressure/rate, previous IV attempts.
- Clinical signs: pain, swelling, erythema at site; severe cases cause ulceration, necrosis.
- Compartment syndrome is a rare but serious complication requiring urgent fasciotomy.
- Initial management: Stop injection immediately, elevate affected limb, apply compresses (warm/cold).
- Prevention is key: secure IV access, use appropriate cannula, monitor injection.
- Non-ionic LOCM generally cause less tissue damage than HOCM.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

