DL Fundamentals - Brainy Basics
- Deep Learning (DL): Subfield of Machine Learning (ML) using Artificial Neural Networks (ANNs) with multiple layers ("deep architectures").
- Inspired by human brain structure and function.
- Neurons (Nodes): Core processing units.
- Weights & Biases: Learnable parameters, adjusted during training.
- Activation Functions: Introduce non-linearity (e.g., ReLU, Sigmoid, Tanh). $f(x)$
- Training Process:
- Forward Propagation: Input data flows through network to generate prediction.
- Backpropagation: Algorithm to calculate gradients & update weights to minimize error (loss function).
- Requires large labeled datasets for optimal performance.

⭐ Exam Favourite: Backpropagation is key for DL training; it adjusts network weights to minimize prediction errors. DL excels at automatic feature extraction from raw data, unlike traditional ML.
Key Architectures - Image Interpreters
- Convolutional Neural Networks (CNNs): Workhorse for radiological image analysis.
- Automatically learn hierarchical features (edges → patterns → objects).
- Key Layers:
- Convolutional: Feature extraction using filters.
- Pooling (e.g., Max Pooling): Downsampling, reduces dimensionality.
- Fully Connected: Classification/regression based on features.
- Activation (e.g., ReLU) for non-linearity.

- U-Net: Specialized CNN architecture for precise biomedical image segmentation.
- Encoder-decoder structure with skip connections to preserve spatial info.
⭐ Convolutional layers are the core of CNNs, responsible for automatically detecting and learning features like edges, textures, and patterns directly from pixel data.
Clinical Applications - Digital Diagnostic Dynamos
- Detection & Localization:
- Identifies pathologies: lung nodules, fractures, intracranial bleeds.
- Aids in Computer-Aided Detection (CADe).
- Segmentation:
- Delineates organs or lesions (e.g., tumor volume for radiotherapy).
- Classification:
- Categorizes findings (e.g., benign vs. malignant, BI-RADS scores).
- Quantification:
- Automates measurements: lesion size, bone density, ejection fraction.
- Image Enhancement & Reconstruction:
- Improves image quality from low-dose CT or accelerated MRI.
- Reduces noise, enhances resolution.
- Workflow Optimization:
- Prioritizes critical studies (e.g., stroke, pneumothorax).
- Automates preliminary report generation.
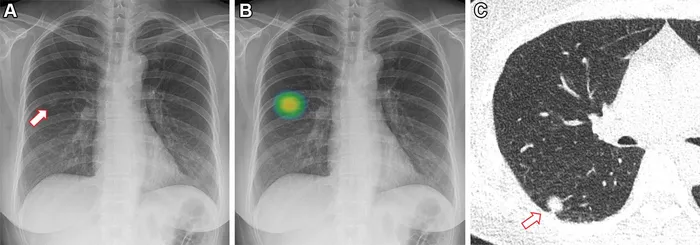
⭐ Exam Favourite: DL excels in mammography for early breast cancer detection, often matching or exceeding human performance in identifying subtle lesions, potentially improving screening efficacy.
Challenges & Future - AI's Ascent & Agonies
- Challenges (Agonies):
- Data Hurdles:
⭐ Critical need: Large, diverse, high-quality, annotated datasets for robust, unbiased AI.
- Privacy (DICOM de-identification), security, & ethical data handling.
- Heterogeneity (scanners, protocols); class imbalance (rare diseases).
- Model Limitations:
- "Black box" issue: Poor interpretability & explainability of AI decisions.
- Generalizability to new data/settings; overfitting; adversarial attack vulnerability.
- Implementation & Societal:
- Workflow integration; regulatory approval (CDSCO); high costs.
- Algorithmic bias; medicolegal clarity; user trust.
- India: Infrastructure, digital literacy, equitable access.
- Data Hurdles:
- Future (Ascent):
- Smarter AI Development:
- Explainable AI (XAI) for transparency & trust.
- Federated learning: privacy-preserving collaborative training.
- Expanding Clinical Utility:
- Personalized radiology; population screening; quantitative biomarkers.
- AI-augmented diagnostics & reporting efficiency.
- Indian Healthcare Focus:
- Indigenous, affordable, accessible AI tools.
- AI-enhanced teleradiology for wider reach.
- Smarter AI Development:
High‑Yield Points - ⚡ Biggest Takeaways
- Convolutional Neural Networks (CNNs) are key for radiological image analysis.
- Supervised learning with large annotated datasets is most common.
- Main applications: image segmentation, lesion detection, and classification.
- Overfitting is a major challenge; addressed by data augmentation.
- Transfer learning helps with limited medical data by using pre-trained models.
- Explainability (XAI) issues ("black box") hinder clinical adoption.
- Regulatory approval (e.g., FDA) is vital for clinical use of AI tools.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

