Admission Criteria - Gates of Care
- Medical Instability:
- Weight < 75% IBW or rapid, persistent loss.
- Vitals: HR < 40 bpm, BP < 80/60 mmHg, Temp < 35.5°C.
- Labs: K+ < 3 mmol/L, PO4 < 0.65 mmol/L (critical for refeeding), ECG changes.
- Psychiatric Instability:
- Acute suicidal risk (intent/plan).
- Severe comorbid conditions (e.g., psychosis, major depression).
- Treatment Context:
- Failure of less intensive treatment levels.
- Need for structured refeeding & medical monitoring.

⭐ Hypophosphatemia is a hallmark of refeeding syndrome, a critical risk during initial inpatient nutritional rehabilitation.
Initial Assessment - Patient Profiling
- History:
- Psychiatric: Co-morbidities (depression, anxiety), suicide risk.
- Medical/Dietary: Weight hx, amenorrhea, intake patterns, purging (frequency, methods).
- Social: Support system, stressors, family dynamics.
- Examination:
- MSE: Body image distortion, insight, mood, suicidality.
- Physical: BMI, vitals (bradycardia, hypotension, hypothermia), signs of malnutrition (lanugo, hair loss), purging (Russell's sign, dental erosion).
- Key Risks: Suicidality, medical instability, refeeding syndrome (e.g., BMI <16 kg/m², rapid weight loss).
- Baseline Investigations: CBC, electrolytes (K, PO4, Mg), LFTs, RFTs, glucose, ECG.
⭐ SCOFF Questionnaire (Sick, Control, One stone, Fat, Food): Score ≥2 indicates a likely case of Anorexia Nervosa or Bulimia Nervosa. Useful for quick screening.
Nutritional Rehab - Refuel & Rebuild
- Goal: Restore weight, normalize eating, correct deficiencies.
- Initial Calories: Start low: 1200-1800 kcal/day (or 30-40 kcal/kg/day).
- Increase: Gradually by 300-400 kcal every 3-4 days, based on tolerance.
- Weight Gain Target (Inpatient): 1-1.5 kg/week. (Outpatient: 0.5-1 kg/week).
- ⚠️ Refeeding Syndrome: High risk in severely malnourished. Key sign: hypophosphatemia (e.g., serum P $<0.65$ mmol/L).
- Monitor: Serum Phosphate, Potassium (K), Magnesium (Mg).
- Thiamine: Prophylactic 100-300mg IV/IM daily before feeds & for 3-5 days.
- Correct electrolyte imbalances pre-feed.
⭐ The primary biochemical hallmark of refeeding syndrome is hypophosphatemia, often seen within the first 72 hours.
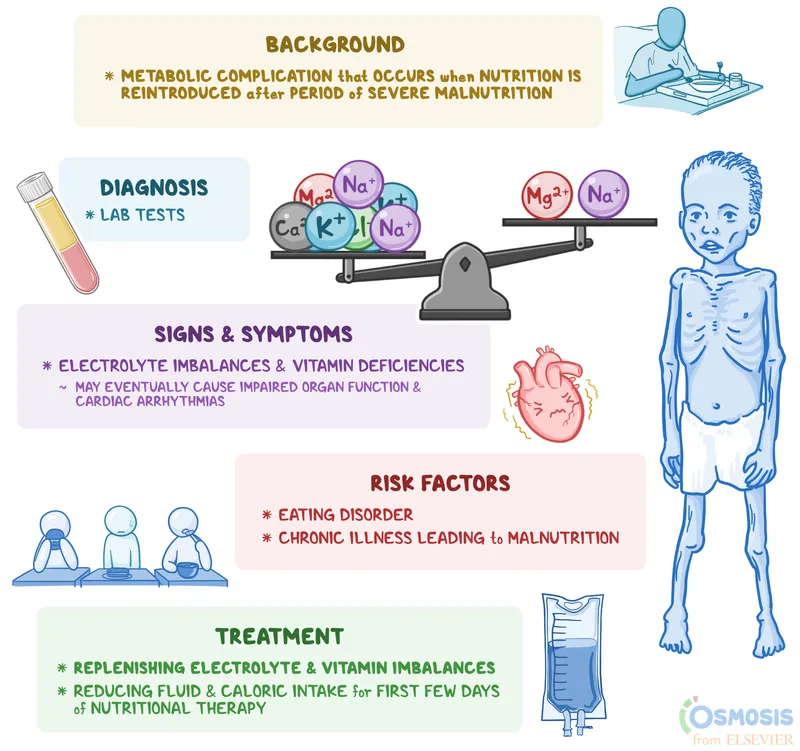
Medical Complications - Code Red Alerts
- Cardiovascular:
- Bradycardia (HR <40 bpm)
- Hypotension (SBP <80 mmHg)
- QTc prolongation (>500ms)
- Arrhythmias
- Electrolyte Imbalance (⚠️ Refeeding Syndrome):
- Hypokalemia <3.0 mmol/L
- Hypophosphatemia <0.65 mmol/L
- Hypomagnesemia <0.6 mmol/L
- Hematological:
- Severe neutropenia (<1.0 x 10⁹/L)
- Other Critical Signs:
- BMI <13 kg/m² or rapid weight loss (>1kg/wk for 2 wks)
- Hypothermia (<35°C)
- Seizures, delirium
- Persistent food/fluid refusal
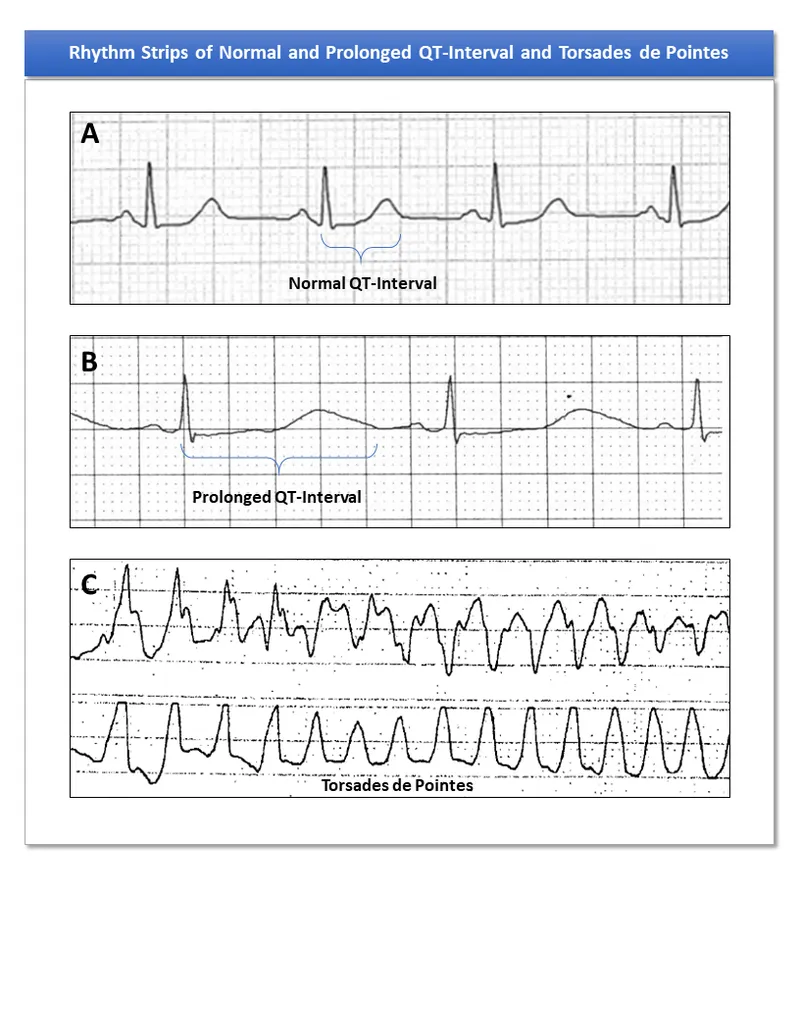
⭐ Hypophosphatemia is a hallmark of refeeding syndrome and can precipitate cardiac failure and arrhythmias.
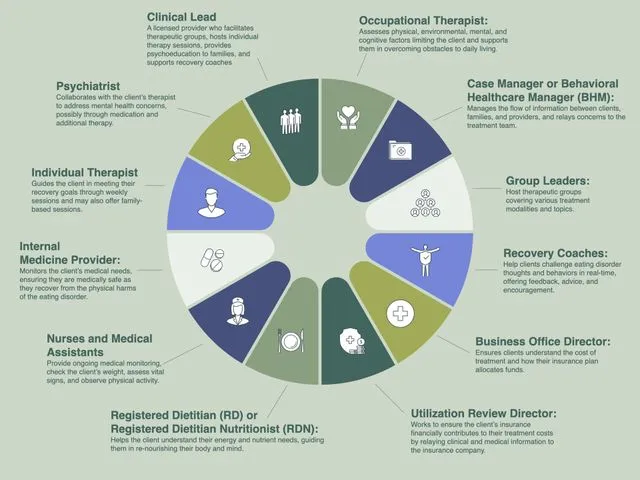
Psycho-Social Support & Discharge - Mind Matters Most
- Multidisciplinary Team (MDT) Approach: Psychiatrist, psychologist, dietitian, social worker, occupational therapist.
- Therapies:
- Individual: CBT-ED, IPT, psychodynamic therapy.
- Family: Essential, especially for adolescents (e.g., Maudsley Method/FBT).
- Group therapy: Peer support, psychoeducation.
- Psychoeducation: For patient and family about illness, nutrition, relapse prevention.
- Discharge Planning:
- Gradual transition: Day-care, halfway homes.
- Relapse prevention plan: Identify triggers, coping strategies.
- Regular follow-up: Monitor weight, mental state, adherence.
- Support groups: e.g., EDA (Eating Disorders Anonymous).
⭐ Family-Based Therapy (FBT), particularly the Maudsley approach, has the strongest evidence base for adolescents with Anorexia Nervosa, often leading to better outcomes than individual therapy alone during inpatient and post-discharge phases.
- 📌 MDT CARE: Motivation, Diet, Therapy, Coping, Aftercare, Relapse prevention, Education.
High‑Yield Points - ⚡ Biggest Takeaways
- Admit for severe malnutrition (BMI < 15), physiological instability (HR < 40, Temp < 35°C, electrolyte imbalance), or suicidality.
- Critical risk: Refeeding syndrome. Monitor electrolytes (K, PO4, Mg); refeed slowly.
- Goals: medical stabilization, nutritional rehabilitation via structured, supervised meals.
- Target weight gain: 0.5-1 kg/week once stable.
- Multidisciplinary team (medical, psychiatric, dietitian) is crucial.
- Manage co-morbidities and initiate psychotherapy (e.g., CBT-E).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

