Defining Resistance - Stubborn Stressors
- Treatment-Resistant Anxiety (TRA): Persistent anxiety symptoms despite ≥2 adequate, distinct treatment courses.
- Criteria for Defining TRA:
- Failed Trials: Minimum of two separate trials of first-line treatments.
- Examples: Two different SSRIs/SNRIs, or one SSRI/SNRI and one course of CBT.
- Adequate Trial: Each trial must ensure:
- Dose: Optimal therapeutic level.
- Duration: Typically 8-12 weeks at this dose.
- Adherence: Good patient compliance.
- Failed Trials: Minimum of two separate trials of first-line treatments.
- "Stubborn Stressors" (Factors contributing to resistance):
- High illness severity or chronicity.
- Psychiatric comorbidities (e.g., depression, personality disorder).
- Prominent psychosocial stressors.
⭐ Approximately 20-30% of patients with anxiety disorders may not respond adequately to initial standard treatments, meeting criteria for TRA.
Investigating Resistance - Unmasking Mimics
- 1. Verify Diagnosis: Is it truly anxiety, or a mimic?
- Rule out other psychiatric disorders (e.g., MDD with anxious distress).
- 2. Assess Prior Treatment Adequacy (📌 "ADD"):
- Adherence: Was medication taken as prescribed?
- Dose: Was it optimal? (e.g., SSRIs at therapeutic levels)
- Duration: Sufficient trial length? (e.g., 8-12 weeks for SSRIs/SNRIs)
- 3. Screen for Comorbidities:
- Medical: Thyroid dysfunction (TSH, T3, T4), cardiac issues (ECG), pheochromocytoma, anemia.
- Psychiatric: Depression, OCD, PTSD, personality disorders.
- 4. Evaluate Substance Use:
- Caffeine, nicotine, alcohol, illicit drugs (stimulants, cannabis).
- Withdrawal syndromes.
- 5. Psychosocial Factors:
- Ongoing stressors, trauma, poor social support, family dynamics.
⭐ Exam Favourite: Inadequate trial duration (e.g., < 8 weeks for an SSRI at a therapeutic dose) is a common reason for apparent treatment resistance in anxiety disorders.
Pharmacotherapy - Pill Power-Ups
- Core Strategy: Maximize current Rx before escalating.
- Optimize: Max tolerated dose (e.g., Escitalopram 20-30 mg), duration (8-12 wks), adherence for current SSRI/SNRI.
- Switch: Another SSRI/SNRI, Venlafaxine XR, Duloxetine. TCAs (e.g., Clomipramine) or MAOIs (specialist, last resort).
- Augment/Combine: For partial/no response.
- Augmentation Options:
| Agent | Dose (mg/day) | Notes |
|---|---|---|
| Quetiapine XR | 50-300 | GAD, SAD. Metabolic SEs. |
| Risperidone | 0.5-2 | Anxiety. EPS, prolactin. |
| Pregabalin | 150-600 | GAD, SAD. Rapid. ⚠️ Misuse. |
| Gabapentin | 900-3600 | GAD, SAD. Sedation. |
| Buspirone | 15-60 | GAD. Slow onset. No dependence. Augments SSRIs. |
| BZDs (short-term) | e.g., Clonaz 0.5-2 | Severe anxiety. ⚠️ Dependence. |
Beyond Pills - Mind & Machine
-
Intensive Psychotherapies:
- CBT: ↑ dose/frequency (e.g., >16-20 sessions), therapist-assisted exposure.
- MBCT: Integrates CBT & mindfulness; prevents relapse in recurrent anxiety.
- ACT: Promotes psychological flexibility via acceptance, mindfulness, values.
-
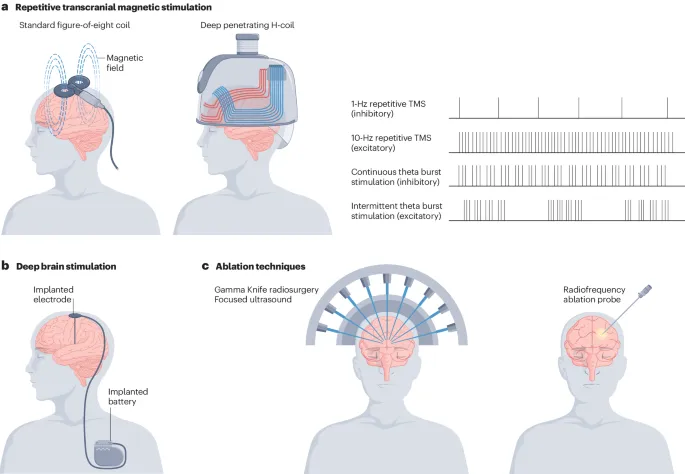
Neuromodulation (For severe, refractory TRA):
⭐ rTMS targeting the right dorsolateral prefrontal cortex (DLPFC) is an emerging option for GAD.
Neuromodulation Comparison:
Technique Invasiveness Key Feature (Anxiety) rTMS Non-invasive Magnetic pulses (R-DLPFC) tDCS Non-invasive Weak current (DLPFC) VNS Invasive Vagal nerve stim (implant) DBS Invasive Deep brain stim (implant, VC/VS)
High‑Yield Points - ⚡ Biggest Takeaways
- Treatment-Resistant Anxiety (TRA): Defined by failure to respond to ≥2 adequate trials of different first-line treatments (e.g., SSRI/SNRI, CBT).
- Crucial initial step: Exclude non-adherence, misdiagnosis, and comorbid medical or substance use disorders.
- Common augmentation strategies include buspirone, low-dose atypical antipsychotics (e.g., quetiapine, risperidone), and pregabalin/gabapentin.
- For severe, refractory TRA: Consider MAOIs (e.g., phenelzine) or TCAs (e.g., clomipramine), monitoring closely for side effects.
- Intensive or specialized CBT (e.g., exposure-based) and robust psychosocial support remain cornerstone adjunctive treatments.
- Emerging options (largely investigational): Ketamine infusions, D-cycloserine (DCS) augmentation for CBT.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

